Recent from talks
Knowledge base stats:
Talk channels stats:
Members stats:
Hypospadias
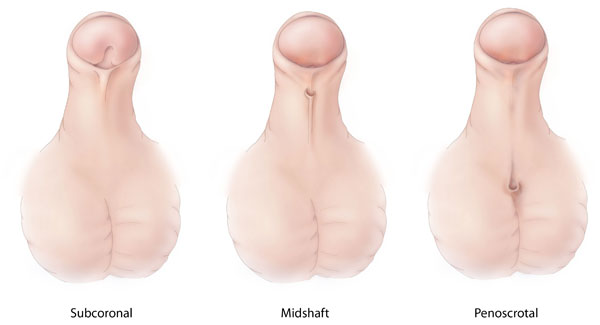
Hypospadias is a common malformation in fetal development of the penis in which the urethra does not open from its usual location on the head of the penis. It is the second-most common birth defect of the male reproductive system, affecting about one of every 250 males at birth, although when including milder cases, is found in up to 4% of newborn males. Roughly 90% of cases are the less serious distal hypospadias, in which the urethral opening (the meatus) is on or near the head of the penis (glans). The remainder have proximal hypospadias, in which the meatus is all the way back on the shaft of the penis, near or within the scrotum. Shiny tissue or anything that typically forms the urethra instead extends from the meatus to the tip of the glans; this tissue is called the urethral plate.
In most cases, the foreskin is less developed and does not wrap completely around the penis, leaving the underside of the glans uncovered. Also, a downward bending of the penis, commonly referred to as chordee, may occur. Chordee is found in 10% of distal hypospadias and 50% of proximal hypospadias cases at the time of surgery. Also, the scrotum may be higher than usual on either side of the penis (called penoscrotal transposition).
The cause of hypospadias is unknown; scientists have investigated both genetic and environmental mechanisms, such as prenatal hormones. Another model suggests hypospadias arises as a result of unerased epigenetic markers which canalize sexual development. It most often occurs by itself, without other variations, although in about 10% of cases it may be part of disorder of sex development condition or a medical syndrome with multiple abnormalities.
The most common associated difference is an undescended testicle, which has been reported in around 3% of infants with distal hypospadias and 10% with proximal hypospadias. The combination of hypospadias and an undescended testicle sometimes indicates a child has a difference of sex development condition, so additional testing may be recommended to make sure the child does not have congenital adrenal hyperplasia with salt wasting[clarify] or a similar condition where immediate medical intervention is needed. Otherwise no blood tests or X-rays are routinely needed in newborns with hypospadias.
Hypospadias can also occur in females. Female hypospadias is defined as a female urethral opening on the anterior vaginal wall proximal to the hymenal ring. The urethra is obviously shorter than usual. This condition usually co-exists with other genitourinary conditions like ectopic ureter, renal anomalies, septate vagina and bicornuate uterus.
Hypospadias is a mild difference in sex development, but some consider that the presence of hypospadias alone is not enough to classify someone as a person as intersex. In most cases, hypospadias is not associated with any other condition. Hypospadias is considered as an intersex condition by several intersex rights activist groups, who consider the repositioning of a working urethra on a child too young to consent to be a human rights violation.
A penis with hypospadias usually has a characteristic appearance. Not only is the meatus (urinary opening) lower than usual, but the foreskin is also often only partially developed, lacking the usual amount that would cover the glans on the underside, causing the glans to have a hooded appearance. However, newborns with partial foreskin development do not necessarily have hypospadias, as some have a meatus in the usual place with a hooded foreskin, called "chordee without hypospadias".
In other cases, the foreskin (prepuce) is typical and the hypospadias is concealed. This is called "megameatus with intact prepuce". The condition is discovered during newborn circumcision or later in childhood when the foreskin begins to retract. A newborn with typical-appearing foreskin and a straight penis who is discovered to have hypospadias after the start of circumcision can have circumcision completed without concern for jeopardizing hypospadias repair.
Hub AI
Hypospadias AI simulator
(@Hypospadias_simulator)
Hypospadias
Hypospadias is a common malformation in fetal development of the penis in which the urethra does not open from its usual location on the head of the penis. It is the second-most common birth defect of the male reproductive system, affecting about one of every 250 males at birth, although when including milder cases, is found in up to 4% of newborn males. Roughly 90% of cases are the less serious distal hypospadias, in which the urethral opening (the meatus) is on or near the head of the penis (glans). The remainder have proximal hypospadias, in which the meatus is all the way back on the shaft of the penis, near or within the scrotum. Shiny tissue or anything that typically forms the urethra instead extends from the meatus to the tip of the glans; this tissue is called the urethral plate.
In most cases, the foreskin is less developed and does not wrap completely around the penis, leaving the underside of the glans uncovered. Also, a downward bending of the penis, commonly referred to as chordee, may occur. Chordee is found in 10% of distal hypospadias and 50% of proximal hypospadias cases at the time of surgery. Also, the scrotum may be higher than usual on either side of the penis (called penoscrotal transposition).
The cause of hypospadias is unknown; scientists have investigated both genetic and environmental mechanisms, such as prenatal hormones. Another model suggests hypospadias arises as a result of unerased epigenetic markers which canalize sexual development. It most often occurs by itself, without other variations, although in about 10% of cases it may be part of disorder of sex development condition or a medical syndrome with multiple abnormalities.
The most common associated difference is an undescended testicle, which has been reported in around 3% of infants with distal hypospadias and 10% with proximal hypospadias. The combination of hypospadias and an undescended testicle sometimes indicates a child has a difference of sex development condition, so additional testing may be recommended to make sure the child does not have congenital adrenal hyperplasia with salt wasting[clarify] or a similar condition where immediate medical intervention is needed. Otherwise no blood tests or X-rays are routinely needed in newborns with hypospadias.
Hypospadias can also occur in females. Female hypospadias is defined as a female urethral opening on the anterior vaginal wall proximal to the hymenal ring. The urethra is obviously shorter than usual. This condition usually co-exists with other genitourinary conditions like ectopic ureter, renal anomalies, septate vagina and bicornuate uterus.
Hypospadias is a mild difference in sex development, but some consider that the presence of hypospadias alone is not enough to classify someone as a person as intersex. In most cases, hypospadias is not associated with any other condition. Hypospadias is considered as an intersex condition by several intersex rights activist groups, who consider the repositioning of a working urethra on a child too young to consent to be a human rights violation.
A penis with hypospadias usually has a characteristic appearance. Not only is the meatus (urinary opening) lower than usual, but the foreskin is also often only partially developed, lacking the usual amount that would cover the glans on the underside, causing the glans to have a hooded appearance. However, newborns with partial foreskin development do not necessarily have hypospadias, as some have a meatus in the usual place with a hooded foreskin, called "chordee without hypospadias".
In other cases, the foreskin (prepuce) is typical and the hypospadias is concealed. This is called "megameatus with intact prepuce". The condition is discovered during newborn circumcision or later in childhood when the foreskin begins to retract. A newborn with typical-appearing foreskin and a straight penis who is discovered to have hypospadias after the start of circumcision can have circumcision completed without concern for jeopardizing hypospadias repair.