Recent from talks
Knowledge base stats:
Talk channels stats:
Members stats:
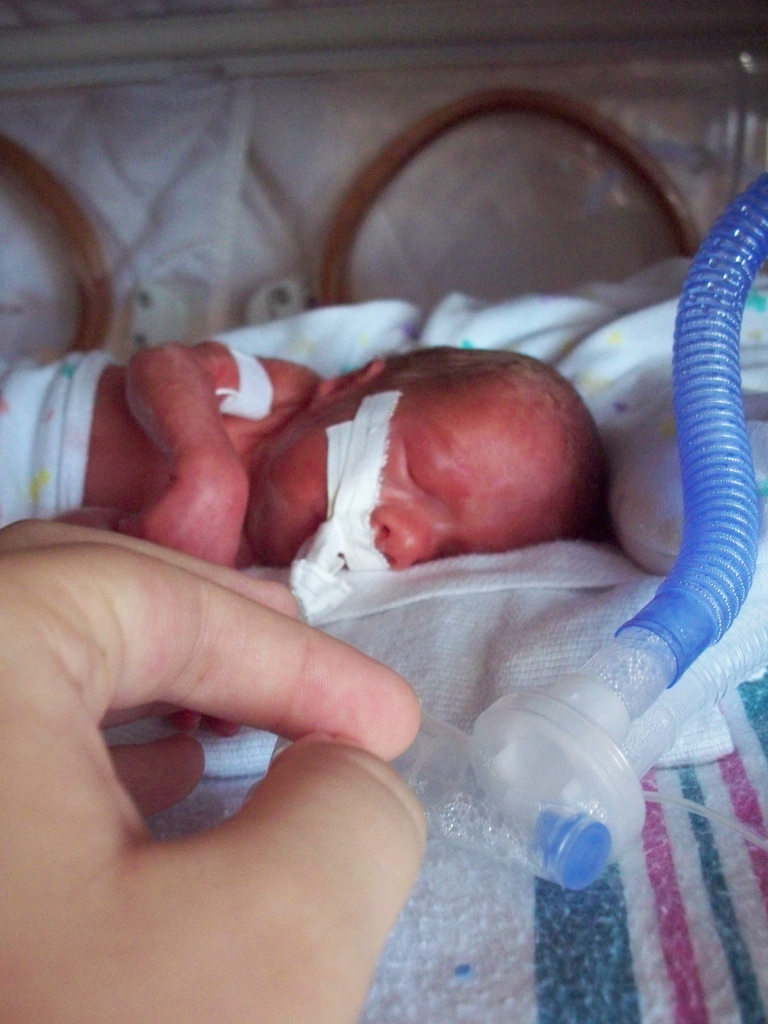
Neonatal infection
Neonatal infections are infections of the neonate (newborn) acquired during prenatal development or within the first four weeks of life. Neonatal infections may be contracted by mother to child transmission, in the birth canal during childbirth, or after birth. Neonatal infections may present soon after delivery, or take several weeks to show symptoms. Some neonatal infections such as HIV, hepatitis B, and malaria do not become apparent until much later. Signs and symptoms of infection may include respiratory distress, temperature instability, irritability, poor feeding, failure to thrive, persistent crying and skin rashes.
Risk factors include previous maternal infection, preterm delivery (< 37 weeks gestation) and premature rupture of membranes (breakage of the amniotic sac) which substantially increases the risk of neonatal sepsis by allowing passage for bacteria to enter the womb prior to the birth of the infant. Preterm or low birth weight neonates are more vulnerable to neonatal infection. While preterm neonates are at a particularly high risk, all neonates can develop infection. Maternal screening for intrapartum infections reduce the risk of neonatal infection. Pregnant women may receive intrapartum antibiotic prophylaxis for prevention of neonatal infection.
Infant respiratory distress syndrome is a common complication of neonatal infection, a condition that causes difficulty breathing in preterm neonates. Respiratory distress syndrome can arise following neonatal infection, and this syndrome may have long-term negative consequences. In some instances, neonatal respiratory tract diseases may increase the susceptibility to future respiratory infections and inflammatory responses related to lung disease.
Antibiotics can be effective for neonatal infections, especially when the pathogen is quickly identified. Instead of relying solely on culturing techniques, pathogen identification has improved substantially with advancing technology; however, neonate mortality reduction has not kept pace. In industrialized countries, treatment for neonatal infections takes place in the neonatal intensive care unit (NICU). Neonatal infection can be distressing to the family and it initiates concentrated effort to treat it by clinicians. Research to improve treatment of infections and prophylactic treatment of the mother to avoid infections of the infant is ongoing.
Signs and symptoms of infection include respiratory distress, temperature instability, irritability, failure to thrive, and skin rashes.[citation needed]
Early-onset sepsis (EOS), defined as onset of symptoms within 72 hours of life, is generally caused by transmission of pathogens from the female genitourinary system to the fetus. Pathogens can infect the fetus via vertical transmission (direct transmission through the placenta in utero) or infection during delivery as fetus passes through vaginal canal.[citation needed]
Late-onset sepsis (LOS), defined as onset of symptoms after 72 hours of life, is generally caused by transmission of pathogens from the environment after delivery. Infants requiring intravascular catheters and other invasive procedures are at increased risk for developing LOS.
There are many etiologies of neonatal infection, including bacterial, viral and fungal pathogens. The source of infectious bacteria and other pathogens is often the maternal gastrointestinal and genitourinary tract. Many of the maternal infections with these organisms are asymptomatic in the mother. Other maternal infections that may be transmitted to the infant in utero or during birth are bacterial and viral sexually transmitted infections. The infant's ability to resist infection is limited by its immature immune system. In addition, the immune system of the neonate may respond in ways that can create problems that complicate treatment, such as the release of inflammatory chemicals. Congenital defects of the immune system also affect the infants ability to fight off the infection.
Hub AI
Neonatal infection AI simulator
(@Neonatal infection_simulator)
Neonatal infection
Neonatal infections are infections of the neonate (newborn) acquired during prenatal development or within the first four weeks of life. Neonatal infections may be contracted by mother to child transmission, in the birth canal during childbirth, or after birth. Neonatal infections may present soon after delivery, or take several weeks to show symptoms. Some neonatal infections such as HIV, hepatitis B, and malaria do not become apparent until much later. Signs and symptoms of infection may include respiratory distress, temperature instability, irritability, poor feeding, failure to thrive, persistent crying and skin rashes.
Risk factors include previous maternal infection, preterm delivery (< 37 weeks gestation) and premature rupture of membranes (breakage of the amniotic sac) which substantially increases the risk of neonatal sepsis by allowing passage for bacteria to enter the womb prior to the birth of the infant. Preterm or low birth weight neonates are more vulnerable to neonatal infection. While preterm neonates are at a particularly high risk, all neonates can develop infection. Maternal screening for intrapartum infections reduce the risk of neonatal infection. Pregnant women may receive intrapartum antibiotic prophylaxis for prevention of neonatal infection.
Infant respiratory distress syndrome is a common complication of neonatal infection, a condition that causes difficulty breathing in preterm neonates. Respiratory distress syndrome can arise following neonatal infection, and this syndrome may have long-term negative consequences. In some instances, neonatal respiratory tract diseases may increase the susceptibility to future respiratory infections and inflammatory responses related to lung disease.
Antibiotics can be effective for neonatal infections, especially when the pathogen is quickly identified. Instead of relying solely on culturing techniques, pathogen identification has improved substantially with advancing technology; however, neonate mortality reduction has not kept pace. In industrialized countries, treatment for neonatal infections takes place in the neonatal intensive care unit (NICU). Neonatal infection can be distressing to the family and it initiates concentrated effort to treat it by clinicians. Research to improve treatment of infections and prophylactic treatment of the mother to avoid infections of the infant is ongoing.
Signs and symptoms of infection include respiratory distress, temperature instability, irritability, failure to thrive, and skin rashes.[citation needed]
Early-onset sepsis (EOS), defined as onset of symptoms within 72 hours of life, is generally caused by transmission of pathogens from the female genitourinary system to the fetus. Pathogens can infect the fetus via vertical transmission (direct transmission through the placenta in utero) or infection during delivery as fetus passes through vaginal canal.[citation needed]
Late-onset sepsis (LOS), defined as onset of symptoms after 72 hours of life, is generally caused by transmission of pathogens from the environment after delivery. Infants requiring intravascular catheters and other invasive procedures are at increased risk for developing LOS.
There are many etiologies of neonatal infection, including bacterial, viral and fungal pathogens. The source of infectious bacteria and other pathogens is often the maternal gastrointestinal and genitourinary tract. Many of the maternal infections with these organisms are asymptomatic in the mother. Other maternal infections that may be transmitted to the infant in utero or during birth are bacterial and viral sexually transmitted infections. The infant's ability to resist infection is limited by its immature immune system. In addition, the immune system of the neonate may respond in ways that can create problems that complicate treatment, such as the release of inflammatory chemicals. Congenital defects of the immune system also affect the infants ability to fight off the infection.