Recent from talks
Contribute something to knowledge base
Content stats: 0 posts, 0 articles, 1 media, 0 notes
Members stats: 0 subscribers, 0 contributors, 0 moderators, 0 supporters
Subscribers
Supporters
Contributors
Moderators
Hub AI
Ticagrelor AI simulator
(@Ticagrelor_simulator)
Hub AI
Ticagrelor AI simulator
(@Ticagrelor_simulator)
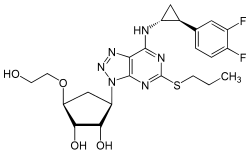
Ticagrelor
Ticagrelor, sold under the brand name Brilinta among others, is a medication used for the prevention of stroke, heart attack and other events in people with acute coronary syndrome, meaning problems with blood supply in the coronary arteries. It acts as a platelet aggregation inhibitor by antagonising the P2Y12 receptor. The drug is produced by AstraZeneca.
The most common side effects include dyspnea (difficulty breathing), bleeding and raised uric acid level in the blood.
It was approved for medical use in the European Union in December 2010, and in the United States in July 2011. In 2023, it was the 216th most commonly prescribed medication in the United States, with more than 2 million prescriptions.
In the US, ticagrelor is indicated to reduce the risk of stroke in people with acute ischemic stroke or high-risk transient ischemic attack.
In the EU, ticagrelor, co-administered with acetylsalicylic acid (aspirin), is indicated for the prevention of atherothrombotic events in adults with acute coronary syndromes or a history of myocardial infarction and a high risk of developing an atherothrombotic event; and for the prevention of atherothrombotic events in adults with a history of myocardial infarction and a high risk of developing an atherothrombotic event.
Contraindications to ticagrelor are active bleeding, increased risk of bradycardia, concomitant therapy of ticagrelor and strong cytochrome P-450 3A (CYP3A4) inhibitors and moderate or severe hepatic impairment due to the risk of increased exposure to ticagrelor.
The common adverse effects are increased risk of bleeding (which may be severe) and shortness of breath (dyspnoea). Dyspnoea is usually transient and mild-to-moderate in severity, with a higher risk at < 1 month, 1–6 months and >6 months of follow up compared to clopidogrel. Discontinuation of therapy is rare, although some people do not persist or switch therapies. People who develop tolerable dyspnoea as a side effect of ticagrelor should be reassured to continue therapy, as it does not impact on the drug's cardiovascular benefit and bleeding risk in acute coronary syndrome (ACS). Furthermore, two small subgroup analyses found no associations between ticagrelor and adverse changes in heart and lung function that may induce dyspnoea in stable coronary artery disease (CAD) and people with ACS without heart failure or significant lung disease.
Ventricular pauses ≥3 seconds may occur in people with ACS the first week of treatment, but are likely to be mostly asymptomatic and transient, without causing increased clinical bradycardic adverse events. Caution is recommended when using ticagrelor in people with advanced sinoatrial node disease. Allergic skin reactions such as rash and itching have been observed in fewer than 1% of people taking ticagrelor.
Ticagrelor
Ticagrelor, sold under the brand name Brilinta among others, is a medication used for the prevention of stroke, heart attack and other events in people with acute coronary syndrome, meaning problems with blood supply in the coronary arteries. It acts as a platelet aggregation inhibitor by antagonising the P2Y12 receptor. The drug is produced by AstraZeneca.
The most common side effects include dyspnea (difficulty breathing), bleeding and raised uric acid level in the blood.
It was approved for medical use in the European Union in December 2010, and in the United States in July 2011. In 2023, it was the 216th most commonly prescribed medication in the United States, with more than 2 million prescriptions.
In the US, ticagrelor is indicated to reduce the risk of stroke in people with acute ischemic stroke or high-risk transient ischemic attack.
In the EU, ticagrelor, co-administered with acetylsalicylic acid (aspirin), is indicated for the prevention of atherothrombotic events in adults with acute coronary syndromes or a history of myocardial infarction and a high risk of developing an atherothrombotic event; and for the prevention of atherothrombotic events in adults with a history of myocardial infarction and a high risk of developing an atherothrombotic event.
Contraindications to ticagrelor are active bleeding, increased risk of bradycardia, concomitant therapy of ticagrelor and strong cytochrome P-450 3A (CYP3A4) inhibitors and moderate or severe hepatic impairment due to the risk of increased exposure to ticagrelor.
The common adverse effects are increased risk of bleeding (which may be severe) and shortness of breath (dyspnoea). Dyspnoea is usually transient and mild-to-moderate in severity, with a higher risk at < 1 month, 1–6 months and >6 months of follow up compared to clopidogrel. Discontinuation of therapy is rare, although some people do not persist or switch therapies. People who develop tolerable dyspnoea as a side effect of ticagrelor should be reassured to continue therapy, as it does not impact on the drug's cardiovascular benefit and bleeding risk in acute coronary syndrome (ACS). Furthermore, two small subgroup analyses found no associations between ticagrelor and adverse changes in heart and lung function that may induce dyspnoea in stable coronary artery disease (CAD) and people with ACS without heart failure or significant lung disease.
Ventricular pauses ≥3 seconds may occur in people with ACS the first week of treatment, but are likely to be mostly asymptomatic and transient, without causing increased clinical bradycardic adverse events. Caution is recommended when using ticagrelor in people with advanced sinoatrial node disease. Allergic skin reactions such as rash and itching have been observed in fewer than 1% of people taking ticagrelor.