Recent from talks
Knowledge base stats:
Talk channels stats:
Members stats:
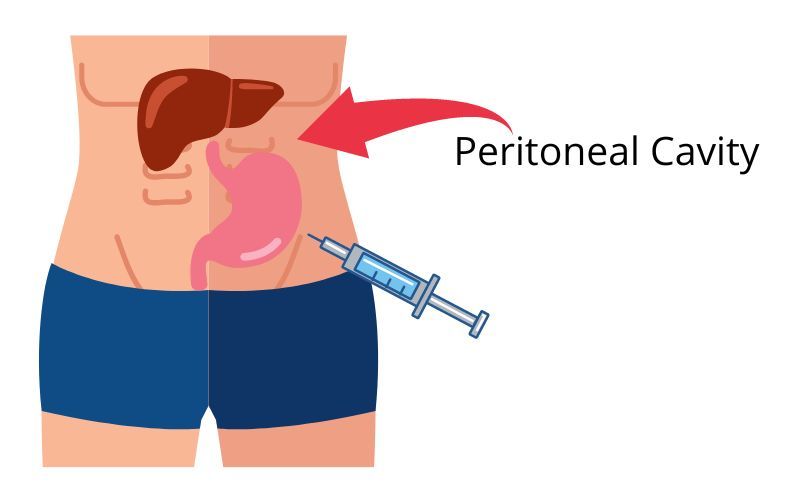
Intraperitoneal injection
Intraperitoneal injection or IP injection is the injection of a substance into the peritoneum (body cavity). It is more often applied to non-human animals than to humans. In general, it is preferred when large amounts of blood replacement fluids are needed or when low blood pressure or other problems prevent the use of a suitable blood vessel for intravenous injection.[citation needed]
In humans, the method is widely used to administer chemotherapy drugs to treat some cancers, particularly ovarian cancer. Although controversial, intraperitoneal use in ovarian cancer has been recommended as a standard of care. Fluids are injected intraperitoneally in infants, also used for peritoneal dialysis.[citation needed]
Intraperitoneal injections are a way to administer therapeutics and drugs through a peritoneal route (body cavity). They are one of the few ways drugs can be administered through injection, and have uses in research involving animals, drug administration to treat ovarian cancers, and much more. Understanding when intraperitoneal injections can be utilized and in what applications is beneficial to advance current drug delivery methods and provide avenues for further research. The benefit of administering drugs intraperitoneally is the ability for the peritoneal cavity to absorb large amounts of a drug quickly. A disadvantage of using intraperitoneal injections is that they can have a large variability in effectiveness and misinjection. Intraperitoneal injections can be similar to oral administration in that hepatic metabolism could occur in both.
There are few accounts of the use of intraperitoneal injections prior to 1970. One of the earliest recorded uses of IP injections involved the insemination of a guinea-pig in 1957. The study however did not find an increase in conception rate when compared to mating. In that same year, a study injected egg whites intraperitoneally into rats to study changes in "droplet" fractions in kidney cells. The study showed that the number of small droplets decreased after administration of the egg whites, indicating that they have been changed to large droplets. In 1964, a study delivered chemical agents such as acetic acid, bradykinin, and kaolin to mice intraperitoneally in order to study a "squirming" response. In 1967, the production of amnesia was studied through an injection of physostigmine. In 1968, melatonin was delivered to rats intraperitoneally in order to study how brain serotonin would be affected in the midbrain. In 1969, errors depending on a variety of techniques of administering IP injections were analyzed, and a 12% error in placement was found when using a one-man procedure versus a 1.2% error when using a two-man procedure.
A good example of how intraperitoneal injections work is depicted through "The distribution of salicylate in mouse tissues after intraperitoneal injection" because it includes information on how a drug can travel to the blood, liver, brain, kidney, heart, spleen, diaphragm, and skeletal muscle once it has been injected intraperitoneally.
These early uses of Intraperitoneal injections provide good examples of how the delivery method can be used, and provides a base for future studies on how to properly inject mice for research.
Currently, there are a handful of drugs that are delivered through intraperitoneal injection for chemotherapy. They are mitomycin C, cisplatin, carboplatin, oxaliplatin, irinotecan, 5-fluorouracil, gemcitabine, paclitaxel, docetaxel, doxorubicin, premetrexed, and melphalan. There needs to be more research done to determine appropriate dosing and combinations of these drugs to advance intraperitoneal drug delivery.
There are few examples of the use of intraperitoneal injections in humans cited in literature because it is mainly used to study the effects of drugs in mice. The few examples that do exist pertain to the treatment of pancreatic/ovarian cancers and injections of other drugs in clinical trials. One study utilized IP injections to study pain in the abdomen after a hysterectomy when administering anesthetic continuously vs patient-controlled. The results depicted that ketobemidone consumption was significantly lower when patients controlled anesthetic through IP. This led to the patients being able to be discharged earlier than when anesthesia was administered continuously. These findings could be advanced by studying how the route of injection affects the organs in the peritoneal cavity.
Hub AI
Intraperitoneal injection AI simulator
(@Intraperitoneal injection_simulator)
Intraperitoneal injection
Intraperitoneal injection or IP injection is the injection of a substance into the peritoneum (body cavity). It is more often applied to non-human animals than to humans. In general, it is preferred when large amounts of blood replacement fluids are needed or when low blood pressure or other problems prevent the use of a suitable blood vessel for intravenous injection.[citation needed]
In humans, the method is widely used to administer chemotherapy drugs to treat some cancers, particularly ovarian cancer. Although controversial, intraperitoneal use in ovarian cancer has been recommended as a standard of care. Fluids are injected intraperitoneally in infants, also used for peritoneal dialysis.[citation needed]
Intraperitoneal injections are a way to administer therapeutics and drugs through a peritoneal route (body cavity). They are one of the few ways drugs can be administered through injection, and have uses in research involving animals, drug administration to treat ovarian cancers, and much more. Understanding when intraperitoneal injections can be utilized and in what applications is beneficial to advance current drug delivery methods and provide avenues for further research. The benefit of administering drugs intraperitoneally is the ability for the peritoneal cavity to absorb large amounts of a drug quickly. A disadvantage of using intraperitoneal injections is that they can have a large variability in effectiveness and misinjection. Intraperitoneal injections can be similar to oral administration in that hepatic metabolism could occur in both.
There are few accounts of the use of intraperitoneal injections prior to 1970. One of the earliest recorded uses of IP injections involved the insemination of a guinea-pig in 1957. The study however did not find an increase in conception rate when compared to mating. In that same year, a study injected egg whites intraperitoneally into rats to study changes in "droplet" fractions in kidney cells. The study showed that the number of small droplets decreased after administration of the egg whites, indicating that they have been changed to large droplets. In 1964, a study delivered chemical agents such as acetic acid, bradykinin, and kaolin to mice intraperitoneally in order to study a "squirming" response. In 1967, the production of amnesia was studied through an injection of physostigmine. In 1968, melatonin was delivered to rats intraperitoneally in order to study how brain serotonin would be affected in the midbrain. In 1969, errors depending on a variety of techniques of administering IP injections were analyzed, and a 12% error in placement was found when using a one-man procedure versus a 1.2% error when using a two-man procedure.
A good example of how intraperitoneal injections work is depicted through "The distribution of salicylate in mouse tissues after intraperitoneal injection" because it includes information on how a drug can travel to the blood, liver, brain, kidney, heart, spleen, diaphragm, and skeletal muscle once it has been injected intraperitoneally.
These early uses of Intraperitoneal injections provide good examples of how the delivery method can be used, and provides a base for future studies on how to properly inject mice for research.
Currently, there are a handful of drugs that are delivered through intraperitoneal injection for chemotherapy. They are mitomycin C, cisplatin, carboplatin, oxaliplatin, irinotecan, 5-fluorouracil, gemcitabine, paclitaxel, docetaxel, doxorubicin, premetrexed, and melphalan. There needs to be more research done to determine appropriate dosing and combinations of these drugs to advance intraperitoneal drug delivery.
There are few examples of the use of intraperitoneal injections in humans cited in literature because it is mainly used to study the effects of drugs in mice. The few examples that do exist pertain to the treatment of pancreatic/ovarian cancers and injections of other drugs in clinical trials. One study utilized IP injections to study pain in the abdomen after a hysterectomy when administering anesthetic continuously vs patient-controlled. The results depicted that ketobemidone consumption was significantly lower when patients controlled anesthetic through IP. This led to the patients being able to be discharged earlier than when anesthesia was administered continuously. These findings could be advanced by studying how the route of injection affects the organs in the peritoneal cavity.