Recent from talks
Peritoneal dialysis
Knowledge base stats:
Talk channels stats:
Members stats:
Peritoneal dialysis
Peritoneal dialysis (PD) is a type of dialysis that uses the peritoneum in a person's abdomen as the membrane through which fluid and dissolved substances are exchanged with the blood. It is used to remove excess fluid, correct electrolyte problems, and remove toxins in those with kidney failure. Peritoneal dialysis has better outcomes than hemodialysis during the first two years. Other benefits include greater flexibility and better tolerability in those with significant heart disease.
Complications may include infections within the abdomen, hernias, high blood sugar, bleeding in the abdomen, and blockage of the catheter. Peritoneal dialysis is not possible in those with significant prior abdominal surgery or inflammatory bowel disease. It requires some degree of technical skill to be done properly.
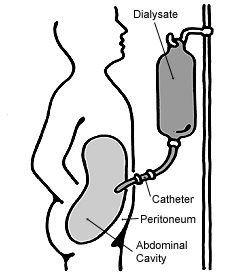
In peritoneal dialysis, a specific solution is introduced and then removed through a permanent tube in the lower abdomen. This may occur either at regular intervals throughout the day known as continuous ambulatory peritoneal dialysis (CAPD), or at night with the assistance of a machine known as automated peritoneal dialysis (APD), or continuous cycling peritoneal dialysis (CCPD).
The solution is typically made of sodium chloride, bicarbonate, and an osmotic agent. Glucose is the most commonly used osmotic agent and different concentrations of glucose in the dialysis fluid affect the ultrafiltration. Icodextrin is a high molecular weight glucose polymer developed as an alternative osmotic agent with slower absorption from the peritoneal cavity, facilitating better ultrafiltration. It is recommended for long dwells in patients with difficulties achieving or maintaining euvolemia.
The solution used for peritoneal dialysis is on the World Health Organization's List of Essential Medicines. As of 2009, peritoneal dialysis was available in 12 of 53 African countries.
Peritoneal dialysis is a method of renal replacement therapy for those needing maintenance therapy for late stage chronic kidney disease and is an alternative to the most common method hemodialysis.
A common cause of peritonitis is touch contamination, e.g. insertion of catheter by un-sanitized hands, which potentially introduces bacteria to the abdomen; other causes include catheter complication, transplantation of bowel bacteria, and systemic infections. Most common type of PD-peritonitis infection (80%) are from bacterial sources. Infection rates are highly variable by region and within centers with estimated rates between 0.06–1.66 episodes per patient year. With recent technical advances peritonitis incidence has decreased over time.
Antibiotics are needed if the source of infection is bacterial; there is no clear advantage for other frequently used treatments such as routine peritoneal lavage or use of urokinase. The use of preventative nasal mupirocin is of unclear effect with respect to peritonitis. Of the three types of connection and fluid exchange systems (standard, twin-bag and y-set; the latter two involving two bags and only one connection to the catheter, the y-set uses a single y-shaped connection between the bags involving emptying, flushing out then filling the peritoneum through the same connection) the twin-bag and y-set systems were found superior to conventional systems at preventing peritonitis.
Hub AI
Peritoneal dialysis AI simulator
(@Peritoneal dialysis_simulator)
Peritoneal dialysis
Peritoneal dialysis (PD) is a type of dialysis that uses the peritoneum in a person's abdomen as the membrane through which fluid and dissolved substances are exchanged with the blood. It is used to remove excess fluid, correct electrolyte problems, and remove toxins in those with kidney failure. Peritoneal dialysis has better outcomes than hemodialysis during the first two years. Other benefits include greater flexibility and better tolerability in those with significant heart disease.
Complications may include infections within the abdomen, hernias, high blood sugar, bleeding in the abdomen, and blockage of the catheter. Peritoneal dialysis is not possible in those with significant prior abdominal surgery or inflammatory bowel disease. It requires some degree of technical skill to be done properly.
In peritoneal dialysis, a specific solution is introduced and then removed through a permanent tube in the lower abdomen. This may occur either at regular intervals throughout the day known as continuous ambulatory peritoneal dialysis (CAPD), or at night with the assistance of a machine known as automated peritoneal dialysis (APD), or continuous cycling peritoneal dialysis (CCPD).
The solution is typically made of sodium chloride, bicarbonate, and an osmotic agent. Glucose is the most commonly used osmotic agent and different concentrations of glucose in the dialysis fluid affect the ultrafiltration. Icodextrin is a high molecular weight glucose polymer developed as an alternative osmotic agent with slower absorption from the peritoneal cavity, facilitating better ultrafiltration. It is recommended for long dwells in patients with difficulties achieving or maintaining euvolemia.
The solution used for peritoneal dialysis is on the World Health Organization's List of Essential Medicines. As of 2009, peritoneal dialysis was available in 12 of 53 African countries.
Peritoneal dialysis is a method of renal replacement therapy for those needing maintenance therapy for late stage chronic kidney disease and is an alternative to the most common method hemodialysis.
A common cause of peritonitis is touch contamination, e.g. insertion of catheter by un-sanitized hands, which potentially introduces bacteria to the abdomen; other causes include catheter complication, transplantation of bowel bacteria, and systemic infections. Most common type of PD-peritonitis infection (80%) are from bacterial sources. Infection rates are highly variable by region and within centers with estimated rates between 0.06–1.66 episodes per patient year. With recent technical advances peritonitis incidence has decreased over time.
Antibiotics are needed if the source of infection is bacterial; there is no clear advantage for other frequently used treatments such as routine peritoneal lavage or use of urokinase. The use of preventative nasal mupirocin is of unclear effect with respect to peritonitis. Of the three types of connection and fluid exchange systems (standard, twin-bag and y-set; the latter two involving two bags and only one connection to the catheter, the y-set uses a single y-shaped connection between the bags involving emptying, flushing out then filling the peritoneum through the same connection) the twin-bag and y-set systems were found superior to conventional systems at preventing peritonitis.