Recent from talks
Knowledge base stats:
Talk channels stats:
Members stats:
Neonatal nursing
Neonatal nursing is a sub-specialty of nursing care for newborn infants up to 28 days after birth. The term neonatal comes from neo, "new", and natal, "pertaining to birth or origin". Neonatal nursing requires a high degree of skill, dedication and emotional strength as they care for newborn infants with a range of problems. These problems vary between prematurity, birth defects, infection, cardiac malformations and surgical issues. Neonatal nurses are a vital part of the neonatal care team and are required to know basic newborn resuscitation, be able to control the newborn's temperature and know how to initiate cardiopulmonary and pulse oximetry monitoring. Most neonatal nurses care for infants from the time of birth until they are discharged from the hospital.
There are four different levels of nurseries where a neonatal nurse might work. The updated classification of neonatal levels by the American Academy of Pediatrics (AAP) includes a Level IV.
Over many years, research and evidence-based practice regimes have been incorporated into everyday nursing protocols to eliminate human error. Due to neonatal nurses' long shifts and busy schedules, nurse tiredness is the number one reason leading to a lack of attention, causing human errors. To prevent this from continuously happening, safety checks and measures are put into place so nurses can provide the most optimal care. Some of these practices include extensive interviews to confirm that those being hired are qualified and willing to continue to learn throughout their careers so they can be the best nurses possible. Strong communication skills are key in any nursing practice; notifying your team members of changes in your patients' status will save their lives. One nurse cannot be at the hospital at all times, so every healthcare member must use teamwork and collaboration to keep each other up to date and to keep their patients alive. Some other key measures include following old protocols and adapting to and utilizing new protocols, checking labels frequently and multiple times before administering a drug, the need for a high attention span, and completing rounds regularly every shift. These are just a few of the safety measures that neonatal nurses must follow to provide the best care.
Neonatal care became a specialty in the United States in 1960 and in that same year, the first NICU was established in the United States. There have been some major changes in Neonatal Care over the past 120 years. Some of these changes include the invention of the incubator, changes in respiratory care and the development of surfactants.
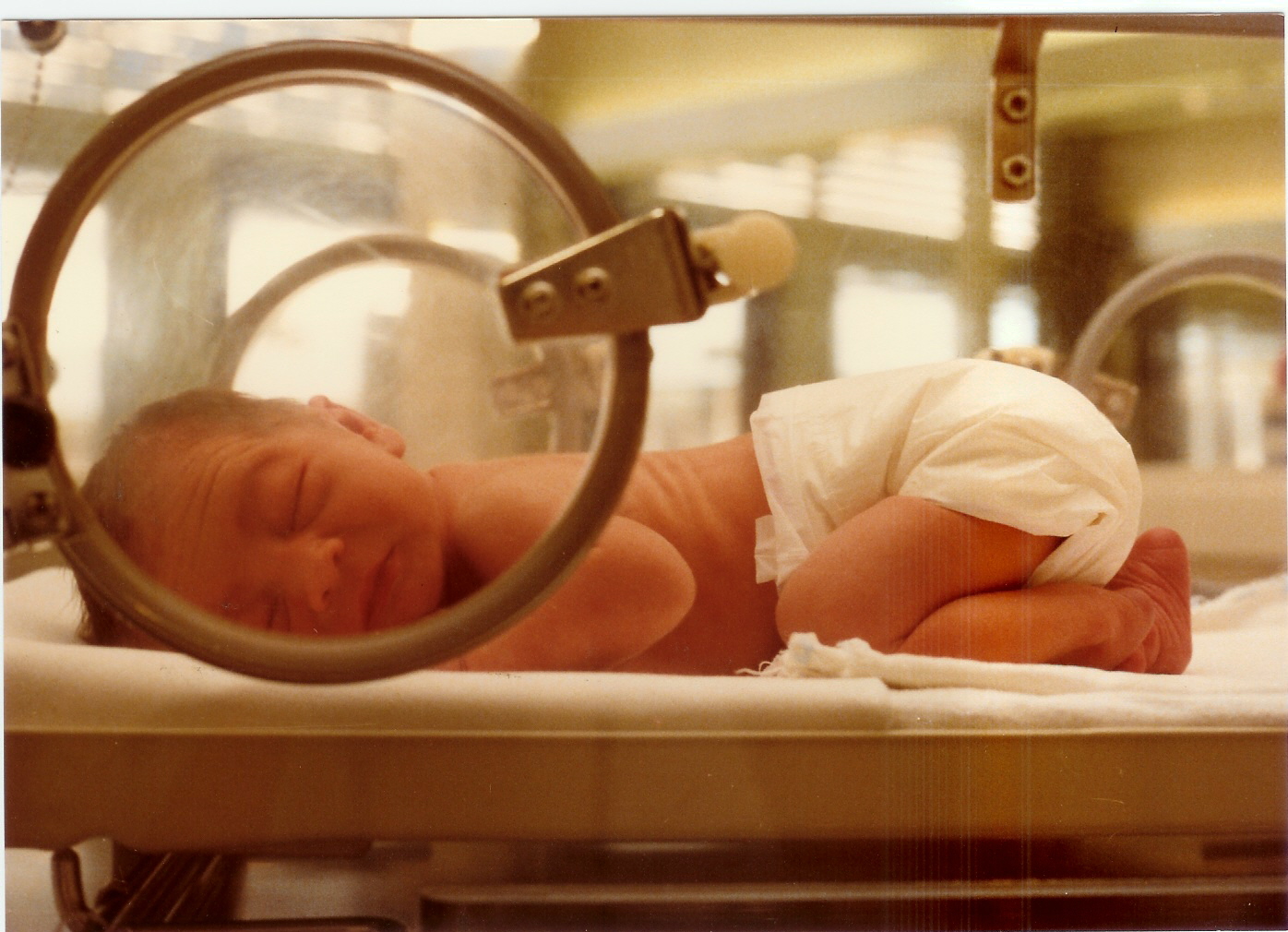
An incubator is a plastic dome-shaped machine designed as a crib that regulates a newborn infant's body temperature. The incubator is designed to allow the temperature to be adjusted according to the state of the baby's current body heat. A range of five types of incubators all serve different purposes in the neonatal intensive care unit. The closed-box incubator is used to prevent infection that could be contracted the outside of the box; it filtrates the air and keeps the moisture fresh. The double-walled incubator keeps heat inside the box. Servo-controlled incubators are controlled by skin detectors which are designed to recognize the loss or gain of body heat and make adjustments to maintain the correct temperature. The open box incubator produces heat from beneath the baby to keep it warm. Portable incubators transport the newborn to and from different parts of the hospital. In 1880, Dr. Tarnier was convinced that the maintenance of internal temperature was key to the premature infant's survival. This led him to introduce the first human incubator. Inspired by chicken eggs hatching in an incubator, he asked a zoo keeper to design a similar incubator for premature infants. Dr. Delee expanded the use and function of the incubator by incorporating an oxygen chamber and an electric controlled thermostat which allowed the incubator to be transported in ambulances.
Administration of oxygen assists and generates oxygen intake for neonates. Oxygen administration began with a metal forked device in the nostrils, and it is now administered through thin plastic tubes in the nostrils, also known as nasal cannula. The first ventilation of an infant was in 1961 in a positive pressure situation, and mechanical ventilation was improved in 1971. Mechanical ventilation is the process in which a machine, attached to the patient, regulates breathing by pumping air in and out of the lungs. Another type of breathing mechanism used is the continuous positive airway pressure (CPAP) mask which attaches to the face to help with breathing. These masks were first used in 1973 as an alternate less invasive form of support.
A surfactant allows a substance to get "wet" to help another substance dissolve. In 1910, the first study of the use of surfactants on infants took place in Japan. Surfactant therapy since has improved the infant mortality rate by 50%. Surfactants combined with the least invasive respiratory therapy (bubble CPAP or nasal CPAP) has greatly improved the infant mortality rate in the US.[citation needed]
In the later 70s, family involvement in treatment became a major addition to patient treatment plans. This decade allowed for upgrades in visiting hours. Hours were expanded and siblings and fathers were encouraged to assist the mother in physical treatment. Many studies showed that with the higher frequency of family interaction such as bottle feeding, skin-to-skin contact, and overall baby holding, and support allowed for patients to have overall major health improvements which eventually lead to a decreasing need for ventilators and quicker discharge rates.
Hub AI
Neonatal nursing AI simulator
(@Neonatal nursing_simulator)
Neonatal nursing
Neonatal nursing is a sub-specialty of nursing care for newborn infants up to 28 days after birth. The term neonatal comes from neo, "new", and natal, "pertaining to birth or origin". Neonatal nursing requires a high degree of skill, dedication and emotional strength as they care for newborn infants with a range of problems. These problems vary between prematurity, birth defects, infection, cardiac malformations and surgical issues. Neonatal nurses are a vital part of the neonatal care team and are required to know basic newborn resuscitation, be able to control the newborn's temperature and know how to initiate cardiopulmonary and pulse oximetry monitoring. Most neonatal nurses care for infants from the time of birth until they are discharged from the hospital.
There are four different levels of nurseries where a neonatal nurse might work. The updated classification of neonatal levels by the American Academy of Pediatrics (AAP) includes a Level IV.
Over many years, research and evidence-based practice regimes have been incorporated into everyday nursing protocols to eliminate human error. Due to neonatal nurses' long shifts and busy schedules, nurse tiredness is the number one reason leading to a lack of attention, causing human errors. To prevent this from continuously happening, safety checks and measures are put into place so nurses can provide the most optimal care. Some of these practices include extensive interviews to confirm that those being hired are qualified and willing to continue to learn throughout their careers so they can be the best nurses possible. Strong communication skills are key in any nursing practice; notifying your team members of changes in your patients' status will save their lives. One nurse cannot be at the hospital at all times, so every healthcare member must use teamwork and collaboration to keep each other up to date and to keep their patients alive. Some other key measures include following old protocols and adapting to and utilizing new protocols, checking labels frequently and multiple times before administering a drug, the need for a high attention span, and completing rounds regularly every shift. These are just a few of the safety measures that neonatal nurses must follow to provide the best care.
Neonatal care became a specialty in the United States in 1960 and in that same year, the first NICU was established in the United States. There have been some major changes in Neonatal Care over the past 120 years. Some of these changes include the invention of the incubator, changes in respiratory care and the development of surfactants.
An incubator is a plastic dome-shaped machine designed as a crib that regulates a newborn infant's body temperature. The incubator is designed to allow the temperature to be adjusted according to the state of the baby's current body heat. A range of five types of incubators all serve different purposes in the neonatal intensive care unit. The closed-box incubator is used to prevent infection that could be contracted the outside of the box; it filtrates the air and keeps the moisture fresh. The double-walled incubator keeps heat inside the box. Servo-controlled incubators are controlled by skin detectors which are designed to recognize the loss or gain of body heat and make adjustments to maintain the correct temperature. The open box incubator produces heat from beneath the baby to keep it warm. Portable incubators transport the newborn to and from different parts of the hospital. In 1880, Dr. Tarnier was convinced that the maintenance of internal temperature was key to the premature infant's survival. This led him to introduce the first human incubator. Inspired by chicken eggs hatching in an incubator, he asked a zoo keeper to design a similar incubator for premature infants. Dr. Delee expanded the use and function of the incubator by incorporating an oxygen chamber and an electric controlled thermostat which allowed the incubator to be transported in ambulances.
Administration of oxygen assists and generates oxygen intake for neonates. Oxygen administration began with a metal forked device in the nostrils, and it is now administered through thin plastic tubes in the nostrils, also known as nasal cannula. The first ventilation of an infant was in 1961 in a positive pressure situation, and mechanical ventilation was improved in 1971. Mechanical ventilation is the process in which a machine, attached to the patient, regulates breathing by pumping air in and out of the lungs. Another type of breathing mechanism used is the continuous positive airway pressure (CPAP) mask which attaches to the face to help with breathing. These masks were first used in 1973 as an alternate less invasive form of support.
A surfactant allows a substance to get "wet" to help another substance dissolve. In 1910, the first study of the use of surfactants on infants took place in Japan. Surfactant therapy since has improved the infant mortality rate by 50%. Surfactants combined with the least invasive respiratory therapy (bubble CPAP or nasal CPAP) has greatly improved the infant mortality rate in the US.[citation needed]
In the later 70s, family involvement in treatment became a major addition to patient treatment plans. This decade allowed for upgrades in visiting hours. Hours were expanded and siblings and fathers were encouraged to assist the mother in physical treatment. Many studies showed that with the higher frequency of family interaction such as bottle feeding, skin-to-skin contact, and overall baby holding, and support allowed for patients to have overall major health improvements which eventually lead to a decreasing need for ventilators and quicker discharge rates.