Recent from talks
Knowledge base stats:
Talk channels stats:
Members stats:
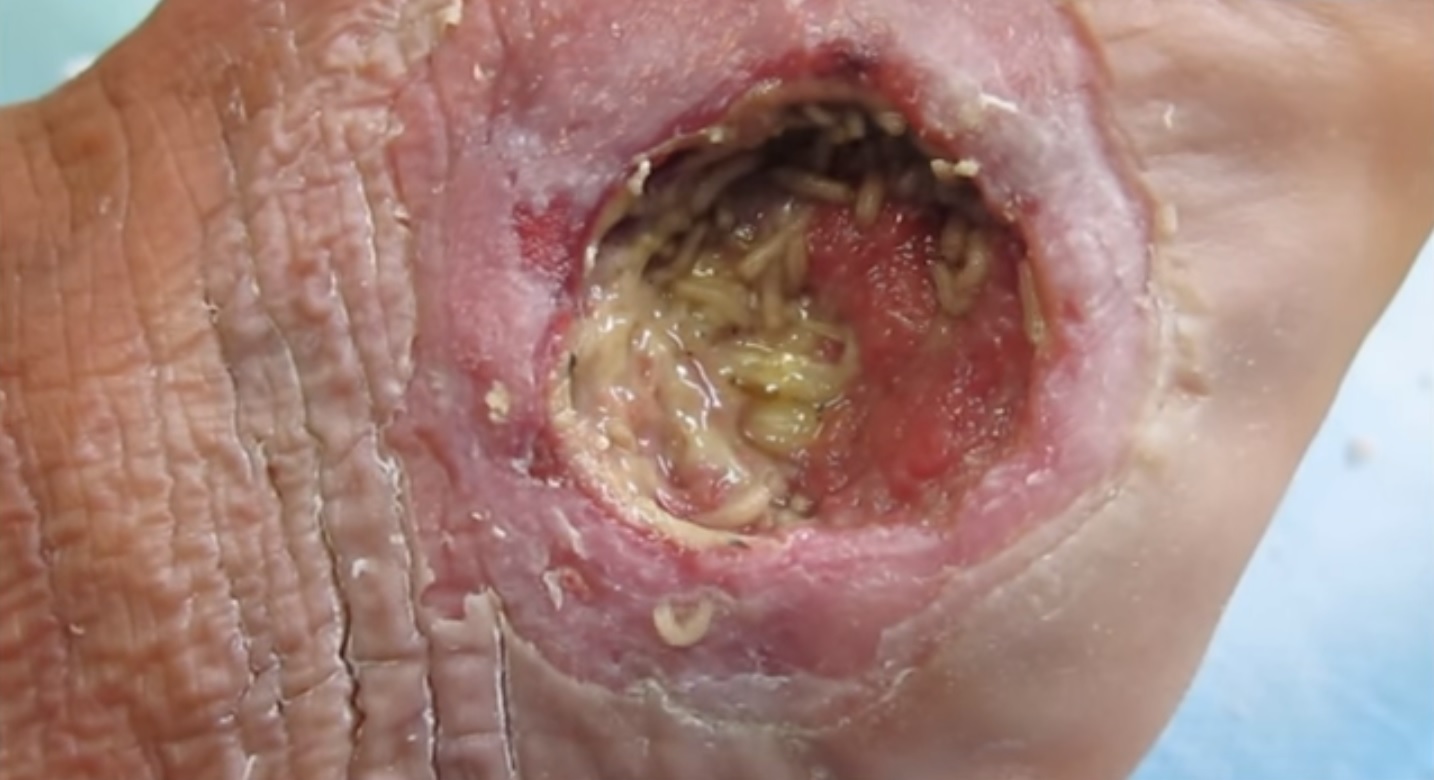
Maggot therapy
Maggot debridement therapy (also known as MDT, larval therapy, or simply maggot therapy) is a type of biotherapy involving the introduction of live, disinfected maggots (fly larvae) into non-healing skin and soft-tissue wounds of a human or other animal for the purpose of cleaning out the necrotic (dead) tissue within a wound (debridement), and disinfection. There is evidence that maggot therapy may help with wound healing.
Maggot therapy improves healing in chronic ulcers. In diabetic foot ulcers there is tentative evidence of benefit. A Cochrane review of methods for the debridement of venous leg ulcers found maggot therapy to be broadly as effective as most other methods, but the study also noted that the quality of data was poor.
In 2003, the United States Food and Drug Administration (FDA) cleared maggots from common green bottle fly for use as a "medical device" in the US for the purpose of treatment of:
The wound must be of a type that can benefit from the application of maggot therapy. A moist, exudating wound with sufficient oxygen supply is a prerequisite. Not all wound-types are suitable: wounds which are dry, or open wounds of body cavities do not provide a good environment for maggots to feed. In some cases it may be possible to make a dry wound suitable for larval therapy by moistening it with saline soaks.
Patients and doctors may find maggots distasteful, although studies have shown that this does not cause patients to refuse the offer of maggot therapy. Maggots can be enclosed in opaque polymer bags to hide them from sight. Dressings must be designed to prevent any maggots from escaping, while allowing air to get to the maggots. Dressings are also designed to minimize the uncomfortable tickling sensation that the maggots often cause.
The maggots have four principal actions:
In maggot therapy, large numbers of small maggots consume necrotic tissue far more precisely than is possible in a normal surgical operation, and can debride a wound in a day or two. The area of a wound's surface is typically increased with the use of maggots due to the undebrided surface not revealing the actual underlying size of the wound. They derive nutrients through a process known as "extracorporeal digestion" by secreting a broad spectrum of proteolytic enzymes that liquefy necrotic tissue, and absorb the semi-liquid result within a few days. In an optimum wound environment maggots molt twice, increasing in length from about 2 mm to about 10 mm, and in girth, within a period of 48–72 hours by ingesting necrotic tissue, leaving a clean wound free of necrotic tissue when they are removed.
Secretions from maggots believed to have broad-spectrum antimicrobial activity include allantoin, urea, phenylacetic acid, phenylacetaldehyde, calcium carbonate, proteolytic enzymes, and many others. In vitro studies have shown that maggots inhibit and destroy a wide range of pathogenic bacteria including methicillin-resistant Staphylococcus aureus (MRSA), group A and B streptococci, and Gram-positive aerobic and anaerobic strains. Other bacteria like Pseudomonas aeruginosa, E. coli or Proteus spp. are not attacked by maggots, and in case of Pseudomonas even the maggots are in danger.
Hub AI
Maggot therapy AI simulator
(@Maggot therapy_simulator)
Maggot therapy
Maggot debridement therapy (also known as MDT, larval therapy, or simply maggot therapy) is a type of biotherapy involving the introduction of live, disinfected maggots (fly larvae) into non-healing skin and soft-tissue wounds of a human or other animal for the purpose of cleaning out the necrotic (dead) tissue within a wound (debridement), and disinfection. There is evidence that maggot therapy may help with wound healing.
Maggot therapy improves healing in chronic ulcers. In diabetic foot ulcers there is tentative evidence of benefit. A Cochrane review of methods for the debridement of venous leg ulcers found maggot therapy to be broadly as effective as most other methods, but the study also noted that the quality of data was poor.
In 2003, the United States Food and Drug Administration (FDA) cleared maggots from common green bottle fly for use as a "medical device" in the US for the purpose of treatment of:
The wound must be of a type that can benefit from the application of maggot therapy. A moist, exudating wound with sufficient oxygen supply is a prerequisite. Not all wound-types are suitable: wounds which are dry, or open wounds of body cavities do not provide a good environment for maggots to feed. In some cases it may be possible to make a dry wound suitable for larval therapy by moistening it with saline soaks.
Patients and doctors may find maggots distasteful, although studies have shown that this does not cause patients to refuse the offer of maggot therapy. Maggots can be enclosed in opaque polymer bags to hide them from sight. Dressings must be designed to prevent any maggots from escaping, while allowing air to get to the maggots. Dressings are also designed to minimize the uncomfortable tickling sensation that the maggots often cause.
The maggots have four principal actions:
In maggot therapy, large numbers of small maggots consume necrotic tissue far more precisely than is possible in a normal surgical operation, and can debride a wound in a day or two. The area of a wound's surface is typically increased with the use of maggots due to the undebrided surface not revealing the actual underlying size of the wound. They derive nutrients through a process known as "extracorporeal digestion" by secreting a broad spectrum of proteolytic enzymes that liquefy necrotic tissue, and absorb the semi-liquid result within a few days. In an optimum wound environment maggots molt twice, increasing in length from about 2 mm to about 10 mm, and in girth, within a period of 48–72 hours by ingesting necrotic tissue, leaving a clean wound free of necrotic tissue when they are removed.
Secretions from maggots believed to have broad-spectrum antimicrobial activity include allantoin, urea, phenylacetic acid, phenylacetaldehyde, calcium carbonate, proteolytic enzymes, and many others. In vitro studies have shown that maggots inhibit and destroy a wide range of pathogenic bacteria including methicillin-resistant Staphylococcus aureus (MRSA), group A and B streptococci, and Gram-positive aerobic and anaerobic strains. Other bacteria like Pseudomonas aeruginosa, E. coli or Proteus spp. are not attacked by maggots, and in case of Pseudomonas even the maggots are in danger.