Recent from talks
Nothing was collected or created yet.
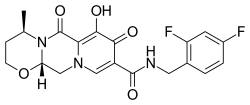
Dolutegravir
View on Wikipedia
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Tivicay, Tivicay PD, Instgra |
| Other names | GSK572, S-349572 |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a613043 |
| License data |
|
| Pregnancy category |
|
| Routes of administration | By mouth |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | n/a[4] |
| Protein binding | ≥98.9% |
| Metabolism | UGT1A1 and CYP3A |
| Elimination half-life | ~14 hours |
| Excretion | Feces (53%) and urine (18.9%) |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| PDB ligand | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.237.735 |
| Chemical and physical data | |
| Formula | C20H19F2N3O5 |
| Molar mass | 419.385 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| | |
Dolutegravir (DTG), sold under the brand name Tivicay or Instgra, is an antiretroviral medication used, together with other medication, to treat HIV/AIDS.[6] It may also be used, as part of post exposure prophylaxis, to prevent HIV infection following potential exposure.[7] It is taken by mouth.[6]
Common side effects include trouble sleeping, feeling tired, diarrhea, high blood sugar, and headache.[7] Severe side effects may include allergic reactions and liver problems.[7] Concerns that usage during pregnancy can result in harm to the baby have been refuted by further studies that show there is no statistical difference in neural tube defects from the usage of dolutegravir compared to other antiretrovirals.[8] It is unclear if use during breastfeeding is safe.[7] Dolutegravir is an HIV integrase strand transfer inhibitor which blocks the functioning of HIV integrase which is needed for viral replication.[7]
Dolutegravir was approved for medical use in the United States in 2013.[7] It is on the World Health Organization's List of Essential Medicines.[9] Abacavir/dolutegravir/lamivudine, a combination with abacavir and lamivudine is also available.[7][10][11] As of 2019, the World Health Organization (WHO) recommends DTG as the first- and second-line treatment for all persons with HIV.[12]
Medical use
[edit]Dolutegravir is approved for use in a broad population of HIV-infected patients. It can be used to treat HIV-infected adults who have never taken HIV therapy (treatment-naïve) and HIV-infected adults who have previously taken HIV therapy (treatment-experienced), including those who have been treated with other integrase strand transfer inhibitors. Tivicay is also approved for children ages 12 years and older weighing at least 40 kilograms (kg) who are treatment-naïve or treatment-experienced but have not previously taken other integrase strand transfer inhibitors.[13]
In the European Union it is indicated, in combination with other anti-retroviral medicinal products, for the treatment of Human Immunodeficiency Virus (HIV) infected adults, adolescents and children above six years of age.[5]
In June 2020, the indication for dolutegravir in the US was updated to include children at least four weeks old and weighing at least 3 kg (6.61 pounds).[14]
Adverse effects
[edit]Common side effects of dolutegravir in clinical trials included insomnia and headache. Serious side effects included allergic reactions and abnormal liver function in patients who were also infected with hepatitis B or C.[15] The package insert warns against a mean rise in serum creatinine of 0.11 mg/dL due to inhibition of tubular secretion of creatinine and does not affect GFR.[4]
Pregnancy
[edit]In 2019 there were tentative concerns[16] that usage during pregnancy can result in the increased risk of neural tube defects however further studies have refuted that claim finding no statistical difference between dolutegravir and other antiretrovirals.[8] As of 31 January 2024[17] dolutegravir is the NIH preferred antiretroviral drug for pregnant or nonpregnant people trying to conceive.[18]
History
[edit]In February 2013, the U.S. Food and Drug Administration (FDA) announced that it would fast track dolutegravir's approval process.[19] On 13 August 2013, dolutegravir was approved for medical use in the United States.[20] On 4 November 2013, dolutegravir was approved by Health Canada.[21] On 16 January 2014, it was approved by the European Commission for use throughout the European Union.[5]
In 2019, a triple-combination therapy, with dolutegravir replacing efavirenz, was introduced as the first-line treatment for all people (pregnant excluded) with HIV by the South African Government (public) sector.[medical citation needed]
In June 2020, dolutegravir was approved in the US with an indication to treat HIV-1 infection in children at least four weeks old and weighing at least 3 kg (6.61 pounds) in combination with other antiretroviral treatments.[14] It is intended to treat children at least 4 weeks old and 3 kg who have never been treated for HIV or who have been treated, but not with an integrase strand transferase inhibitor (INSTI) class drug.[14][22]
The U.S. Food and Drug Administration (FDA) granted the approval of Tivicay and Tivicay PD to ViiV Healthcare.[14]
Access
[edit]In April 2024, the government of Colombia issued its first ever compulsory license to invalidate the patent of Dolutegravir.[23][24] Access to dolutegravir was enabled by a license to the Medicines Patent Pool however Colombia was not a listed territory.[25] UNAIDS supported the move to enable a compulsory license decision.[26] ViiV Healthcare disagreed with the decision on the use of the compulsory license by the government of Colombia.[27] A separate agreement with the Medicines Patent Pool permits the distribution of generic versions of the medicine in Colombia, but this is restricted to children only.[28]
Climate change
[edit]Dolutegravir, used by 24 million people in low- and middle-income countries, has significantly reduced carbon emissions compared to the previous standard of care, efavirenz.[29] This is the first report to analyze the environmental impact of a widely used medicine compared to its alternative. According to Unitaid, this transition will prevent over 26 million tons of CO2 from entering the atmosphere between 2017 and 2027, equivalent to eliminating 10 years of carbon emissions from Geneva, Switzerland.[30]
References
[edit]- ^ "Dolutegravir (Tivicay) Use During Pregnancy". Drugs.com. 16 October 2018. Retrieved 13 February 2020.
- ^ "Prescription medicines: registration of new chemical entities in Australia, 2014". Therapeutic Goods Administration (TGA). 21 June 2022. Retrieved 10 April 2023.
- ^ "Drug and medical device highlights 2018: Helping you maintain and improve your health". Health Canada. 14 October 2020. Retrieved 17 April 2024.
- ^ a b c "Tivicay- dolutegravir sodium tablet, film coated". DailyMed. 24 October 2019. Retrieved 13 February 2020.
- ^ a b c "Tivicay EPAR". European Medicines Agency (EMA). 17 September 2018. Retrieved 13 February 2020.
- ^ a b British national formulary: BNF 69 (69 ed.). British Medical Association. 2015. p. 429. ISBN 978-0-85711-156-2.
- ^ a b c d e f g "Dolutegravir Sodium Monograph for Professionals". Drugs.com. Retrieved 20 April 2019.
- ^ a b Gill MM, Khumalo P, Chouraya C, Kunene M, Dlamini F, Hoffman HJ, et al. (2023). "Strengthening the Evidence: Similar Rates of Neural Tube Defects Among Deliveries Regardless of Maternal HIV Status and Dolutegravir Exposure in Hospital Birth Surveillance in Eswatini". Open Forum Infect Dis. 10 (9) ofad441. doi:10.1093/ofid/ofad441. PMC 10502921. PMID 37720700.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ World Health Organization (2019). World Health Organization model list of essential medicines: 21st list 2019. Geneva: World Health Organization. hdl:10665/325771. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- ^ Ciccullo A, Baldin G, Borghetti A, Di Giambenedetto S (April 2020). "Dolutegravir plus lamivudine for the treatment of HIV-1 infection". Expert Review of Anti-infective Therapy. 18 (4): 279–292. doi:10.1080/14787210.2020.1729742. PMID 32067525. S2CID 211160876.
- ^ Patel R, Evitt L, Mariolis I, Di Giambenedetto S, d'Arminio Monforte A, Casado J, et al. (August 2021). "HIV Treatment with the Two-Drug Regimen Dolutegravir Plus Lamivudine in Real-world Clinical Practice: A Systematic Literature Review". Infectious Diseases and Therapy. 10 (4): 2051–2070. doi:10.1007/s40121-021-00522-7. PMC 8572911. PMID 34426899.
{{cite journal}}: CS1 maint: overridden setting (link) - ^ "WHO recommends dolutegravir as preferred HIV treatment option in all populations". World Health Organization (Press release). Retrieved 22 July 2019.
- ^ "FDA approves new drug to treat HIV infection". Food and Drug Administration. 12 August 2013. Archived from the original on 8 February 2014.
- ^ a b c d "FDA Approves Drug to Treat Infants and Children with HIV". U.S. Food and Drug Administration (FDA) (Press release). 12 June 2020. Archived from the original on 12 June 2020. Retrieved 12 June 2020.
- ^ "U.S. FDA approves GlaxoSmithKline's HIV drug Tivicay". Reuters. 12 August 2013. Retrieved 13 February 2020.
- ^ "Consolidated Guidelines on HIV Prevention, Testing, Treatment, Service Delivery and Monitoring: Recommendations for a Public Health Approach". World Health Organization. 29 October 2020. Retrieved 15 July 2024.
- ^ "What to Start: Initial Antiretroviral Regimens During Pregnancy for People Who Are Antiretroviral-Naïve". Clinicalinfo. 31 January 2024. Retrieved 15 July 2024.
- ^ "Case-Specific Use of Antiretroviral Drugs in Pregnant and Nonpregnant People Trying to Conceive". Clinicalinfo. Retrieved 15 July 2024.
- ^ "GSK wins priority status for new HIV drug in U.S". Reuters. 16 February 2013. Archived from the original on 19 February 2013. Retrieved 18 February 2013.
- ^ "Drug Approval Package: Tivicay (dolutegravir) Tablets NDA #204790". U.S. Food and Drug Administration (FDA). 13 September 2013. Archived from the original on 15 February 2016. Retrieved 12 June 2020.
- ^ "ViiV Healthcare receives approval for Tivicay (dolutegravir) in Canada for the treatment of HIV" (PDF). Archived from the original (PDF) on 12 November 2013. Retrieved 11 November 2013.
- ^ "ViiV Healthcare announces US FDA approval of the first-ever dispersible tablet formulation of dolutegravir, Tivicay PD, a once-daily treatment for children living with HIV". GSK (Press release). Retrieved 12 June 2020.
- ^ Silverman E (25 April 2024). "Colombia issues a compulsory license for an HIV medicine and 'plants a flag for global health equity'". STAT. Retrieved 28 July 2024.
- ^ "Colombia Issues Compulsory License To Enable It To Access Generic HIV Drug, Dolutegravir - Health Policy Watch". 25 April 2024. Retrieved 28 July 2024.
- ^ "More than 100 low- and middle-income countries have now received the WHO-recommended treatment for HIV thanks to access-oriented voluntary licensing agreements - MPP". Retrieved 28 July 2024.
- ^ "UNAIDS welcomes new decision in Colombia allowing more affordable access to quality HIV medicines". UNAIDS. 4 October 2023. Retrieved 28 July 2024.
- ^ "ViiV Healthcare statement on compulsory licence for dolutegravir in Colombia". viivhealthcare.com. Retrieved 28 July 2024.
- ^ "DOLUTEGRAVIR - PAEDIATRICS (DTG) - MPP". Retrieved 28 July 2024.
- ^ Shetty D (15 July 2024). "World's Leading HIV Drug Reduces Carbon Emissions by 26 Million Tons In Comparison to Predecessor". Health Policy Watch.
- ^ "New Unitaid report: World's leading HIV drug proven to have reduced global CO2 emissions by 26 million tons". UNITAID. 15 July 2024.
Dolutegravir
View on GrokipediaDolutegravir is an antiretroviral medication classified as an integrase strand transfer inhibitor (INSTI) used in combination therapy for the treatment and prevention of HIV-1 infection.[1][2] It functions by binding to the active site of the HIV integrase enzyme, thereby blocking the strand transfer step of retroviral DNA integration into the host cell genome, which is essential for viral replication.[3][1] Developed through a collaboration between Shionogi and ViiV Healthcare—a joint venture involving GlaxoSmithKline—dolutegravir received initial U.S. FDA approval in 2013 for treatment-naïve adults, with subsequent expansions to broader populations including children and treatment-experienced patients based on phase III trials demonstrating superior viral suppression compared to alternatives like efavirenz-based regimens.[4][5] Its high genetic barrier to resistance, unboosted once-daily oral dosing, and favorable pharmacokinetic profile have positioned it as a preferred first-line component in global HIV guidelines, contributing to improved outcomes in resource-limited settings.[2][6] While generally well-tolerated, with common adverse effects including insomnia and headache, dolutegravir has been associated with benign elevations in serum creatinine due to tubular secretion inhibition and initial concerns over neural tube defects in infants exposed during conception—stemming from observational data in Botswana—but subsequent large-scale studies and meta-analyses have not confirmed a causal increase in such risks, leading to its endorsement by the WHO and others for use in pregnancy with counseling.[7][8][9]
Pharmacology
Mechanism of action
Dolutegravir functions as a second-generation integrase strand transfer inhibitor (INSTI), specifically targeting the HIV-1 integrase enzyme to block the strand transfer step of viral DNA integration into the host cell genome. By binding to the integrase active site, dolutegravir chelates the Mg²⁺ ions essential for catalysis, forming a stable complex that prevents the 3'-processing and subsequent strand transfer of proviral DNA. This inhibition occurs post-reverse transcription, halting the viral replication cycle at the integration phase without affecting host cellular processes.[10][11] In comparison to first-generation INSTIs like raltegravir, dolutegravir exhibits markedly slower dissociation kinetics from integrase-DNA complexes, with dissociation half-lives exceeding 5 hours for both wild-type and mutant enzymes harboring substitutions at residues E92, Y143, Q148, or N155. This prolonged binding affinity enhances its potency, as demonstrated in biochemical assays where dolutegravir maintained inhibitory activity against integrase variants resistant to raltegravir, due to its ability to accommodate conformational changes in the binding pocket.[12][13] In vitro studies confirm dolutegravir's efficacy against wild-type HIV-1 integrase, with IC₅₀ values in the nanomolar range for strand transfer inhibition, and retained activity against clinically relevant mutants that confer resistance to earlier INSTIs through reduced binding affinity. These findings underscore dolutegravir's targeted disruption of the intasome complex, the nucleoprotein assembly critical for viral DNA integration.[12][10]Pharmacokinetics
Dolutegravir is rapidly absorbed after oral administration, achieving median peak plasma concentrations (T_max) of 2 to 3 hours post-dose in the fasted state. Although absolute bioavailability has not been established due to lack of intravenous data, its pharmacokinetic profile indicates efficient oral absorption. Administration with food enhances exposure, increasing the area under the plasma concentration-time curve (AUC) by 33% to 66% and maximum concentration (C_max) by 46% to 67%, while delaying T_max to 3 to 5 hours; these changes do not alter the recommended dosing, allowing administration with or without meals.[14] The drug exhibits high plasma protein binding of at least 98.9%, primarily to albumin and alpha-1 acid glycoprotein, with an apparent volume of distribution of 17.4 L following a 50 mg dose. Dolutegravir is primarily metabolized in the liver via uridine diphosphate glucuronosyltransferase (UGT)1A1-mediated glucuronidation, with a minor role for cytochrome P450 (CYP)3A; the principal inactive metabolite is the ether glucuronide.[14] Elimination occurs mainly through feces, with approximately 53% of a radiolabeled dose recovered unchanged and 31% in urine (predominantly as metabolites, with <1% as unchanged drug), reflecting both biliary secretion and unabsorbed drug. The terminal elimination half-life is about 14 hours in healthy subjects (11 to 12 hours in HIV-infected individuals), and apparent oral clearance is 1.0 L/h, supporting once-daily dosing.[14] In special populations, no dose adjustments are required for mild to moderate hepatic impairment (Child-Pugh A or B), where exposures are comparable to healthy subjects, though severe impairment (Child-Pugh C) has not been studied. For renal impairment, pharmacokinetics remain unchanged in mild to moderate cases (creatinine clearance ≥30 mL/min); in severe impairment or end-stage renal disease, AUC and C_max are reduced by about 40% and 23%, respectively, but no adjustment is recommended given the minimal renal excretion of unchanged drug (<1%).[14] Population pharmacokinetic analyses in adults show no clinically significant influences from age, sex, race, or body weight.[14]Medical uses
Indications and regimens
Dolutegravir is indicated by the U.S. Food and Drug Administration (FDA) for the treatment of human immunodeficiency virus type 1 (HIV-1) infection in adults and pediatric patients aged at least 4 weeks and weighing at least 3 kg, either treatment-naïve or treatment-experienced, always in combination with other antiretroviral agents.[3][15] The European Medicines Agency (EMA) similarly approves dolutegravir in combination with other antiretrovirals for HIV-1-infected adults and adolescents aged 12 years and older weighing at least 40 kg, with extensions to younger children via dispersible formulations for those weighing at least 3 kg from 4 weeks of age.[16][17] The World Health Organization (WHO) has recommended dolutegravir-based regimens as the preferred first-line option for HIV treatment in adults since its 2016 guidelines, with the 2019 update extending this preference to all populations, including children, adolescents, and pregnant or breastfeeding women, following reviews of safety and programmatic data.[18][19] Approved combination regimens include dolutegravir with lamivudine (Dovato), a two-drug option for virologically suppressed adults and adolescents aged 12 years and older, as well as dolutegravir with abacavir and lamivudine (Triumeq) for broader pediatric and adult use.[20][3] Dolutegravir is utilized in patients with multi-class resistance due to its high genetic barrier to resistance, particularly in integrase strand transfer inhibitor-naïve or experienced individuals without documented resistance to dolutegravir or raltegravir with sufficient dolutegravir dose adjustment.[3] It is not indicated for HIV-2 infection, for which specific antiretroviral options differ due to inherent virologic distinctions, nor for acute HIV infection, as approvals focus on established chronic treatment.[21][22]Dosage and administration
Dolutegravir is available as 50 mg film-coated tablets for adults and older children, and as 5 mg or 10 mg scored dispersible tablets for oral suspension in younger pediatric patients.[23] The dispersible tablets must be dispersed in a small volume of room-temperature water (typically 15-20 mL depending on the number of tablets) and administered immediately, with any remaining suspension discarded; they are not chewed, cut, or swallowed whole.[15] No intravenous formulation exists, and administration is exclusively oral.[23] For adults and adolescents weighing at least 40 kg who are antiretroviral-naïve or integrase strand transfer inhibitor (INSTI)-experienced without resistance, the recommended dose is 50 mg once daily, administered with or without food.[23] In patients coadministered potent cytochrome P450 3A or UGT1A1 inducers such as efavirenz, fosamprenavir/ritonavir, tipranavir/ritonavir, or rifampin, the dose increases to 50 mg twice daily, with doses separated by approximately 12 hours.[21] For INSTI-experienced patients with certain resistance mutations (e.g., Q148 with additional substitutions), a 50 mg twice-daily regimen may restore activity in optimized combination therapy, per U.S. Department of Health and Human Services guidelines. Pediatric dosing is weight-based and uses dispersible tablets for children under 40 kg:| Body Weight (kg) | Recommended Dose |
|---|---|
| 3 to <6 | 5 mg once daily (one 5-mg dispersible tablet) |
| 6 to <10 | 15 mg once daily (three 5-mg dispersible tablets) |
| 10 to <14 | 20 mg once daily (two 10-mg dispersible tablets) |
| 14 to <20 | 25 mg once daily (either two 10-mg and one 5-mg dispersible tablets or one 25-mg film-coated tablet if available) |
| 20 to <40 | 35 mg once daily (one 10-mg and three 5-mg dispersible tablets, or adjusted film-coated equivalents) |
| ≥40 | 50 mg once daily (one 50-mg film-coated tablet) |

