Recent from talks
Contribute something to knowledge base
Content stats: 0 posts, 0 articles, 1 media, 0 notes
Members stats: 0 subscribers, 0 contributors, 0 moderators, 0 supporters
Subscribers
Supporters
Contributors
Moderators
Hub AI
Chorioamnionitis AI simulator
(@Chorioamnionitis_simulator)
Hub AI
Chorioamnionitis AI simulator
(@Chorioamnionitis_simulator)
Chorioamnionitis
Chorioamnionitis, also known as amnionitis and intra-amniotic infection (IAI), is inflammation of the fetal membranes (amnion and chorion), usually due to bacterial infection. In 2015, a National Institute of Child Health and Human Development Workshop expert panel recommended use of the term "triple I" to address the heterogeneity of this disorder. The term triple I refers to intrauterine infection or inflammation or both and is defined by strict diagnostic criteria, but this terminology has not been commonly adopted although the criteria are used.
Chorioamnionitis results from an infection caused by bacteria ascending from the vagina into the uterus and is associated with premature or prolonged labor. It triggers an inflammatory response to release various inflammatory signaling molecules, leading to increased prostaglandin and metalloproteinase release. These substances promote uterine contractions and cervical ripening, causations of premature birth. The risk of developing chorioamnionitis increases with number of vaginal examinations performed in the final month of pregnancy, including labor. Tobacco and alcohol use also puts mothers at risk for chorioamnionitis development.
Chorioamnionitis is caught early by looking at signs and symptoms such as fever, abdominal pain, or abnormal vaginal excretion. Administration of antibiotics if the amniotic sac bursts prematurely can prevent chorioamnionitis occurrence.
The signs and symptoms of clinical chorioamnionitis include fever, leukocytosis (>15,000 cells/mm3), maternal (>100 bpm) or fetal (>160 bpm) tachycardia, uterine tenderness and preterm rupture of membranes.
Causes of chorioamnionitis stem from bacterial infection as well as obstetric and other related factors.
Bacterial, viral, and even fungal infections can cause chorioamnionitis. Most commonly from Ureaplasma, Fusobacterium, and Streptococcus bacteria species. Less commonly, Gardnerella, Mycoplasma, and Bacteroides bacteria species. Sexually transmitted infections, chlamydia and gonorrhea, can cause development of the condition as well. Studies are continuing to identify other microorganism classes and species as infection sources.
Birthing-related events, lifestyle, and ethnic background have been linked to an increase in the risk of developing chorioamnionitis apart from bacterial causation. Premature deliveries, ruptures of the amniotic sac membranes, prolonged labor, and primigravida childbirth are associated with this condition. At term mothers who experience a combination of pre-labor membrane ruptures and multiple invasive vaginal examinations, prolonged labor, or have meconium appear in the amniotic fluid are at higher risk than at term mothers experiencing just one of those events. In other studies, smoking, alcohol use and drug use are noted as risk factors. Those of African American ethnicity are noted to be at higher risk.
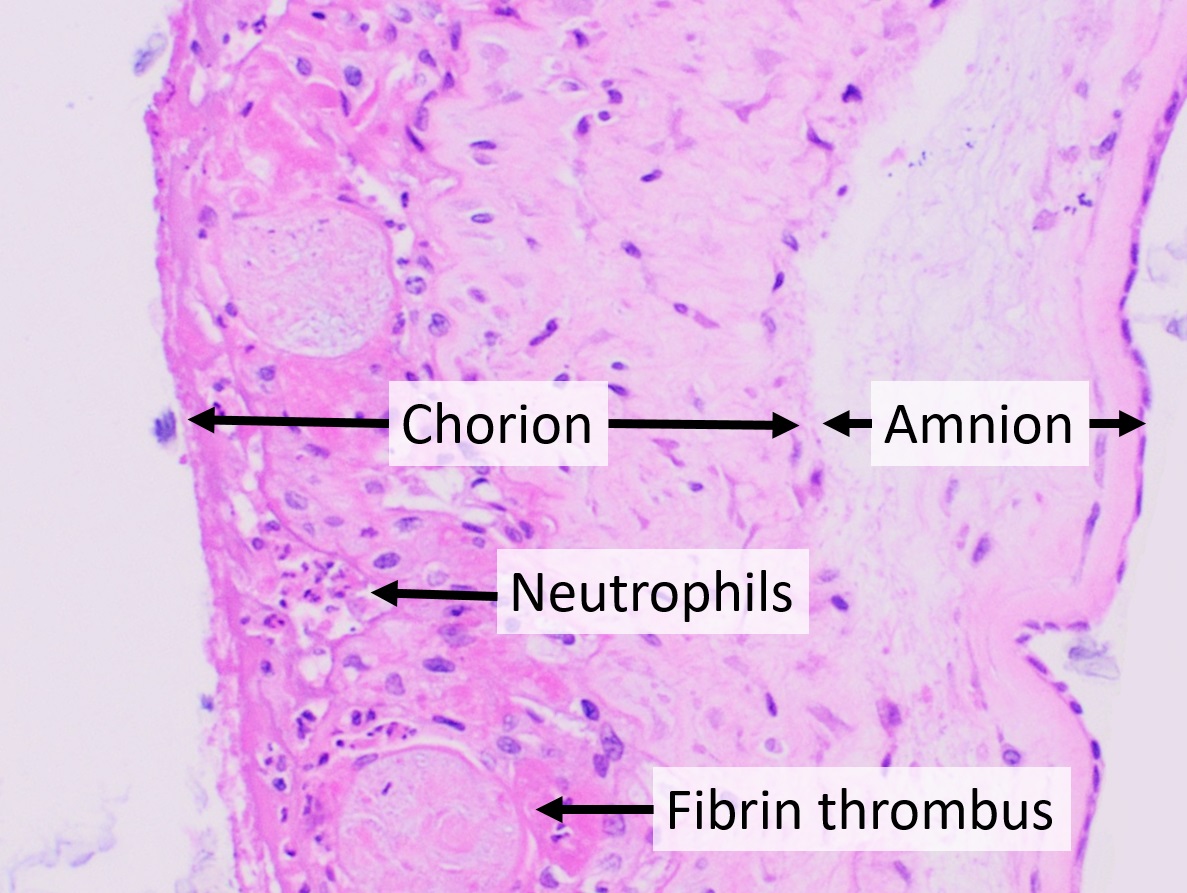
The amniotic sac consists of two parts:
Chorioamnionitis
Chorioamnionitis, also known as amnionitis and intra-amniotic infection (IAI), is inflammation of the fetal membranes (amnion and chorion), usually due to bacterial infection. In 2015, a National Institute of Child Health and Human Development Workshop expert panel recommended use of the term "triple I" to address the heterogeneity of this disorder. The term triple I refers to intrauterine infection or inflammation or both and is defined by strict diagnostic criteria, but this terminology has not been commonly adopted although the criteria are used.
Chorioamnionitis results from an infection caused by bacteria ascending from the vagina into the uterus and is associated with premature or prolonged labor. It triggers an inflammatory response to release various inflammatory signaling molecules, leading to increased prostaglandin and metalloproteinase release. These substances promote uterine contractions and cervical ripening, causations of premature birth. The risk of developing chorioamnionitis increases with number of vaginal examinations performed in the final month of pregnancy, including labor. Tobacco and alcohol use also puts mothers at risk for chorioamnionitis development.
Chorioamnionitis is caught early by looking at signs and symptoms such as fever, abdominal pain, or abnormal vaginal excretion. Administration of antibiotics if the amniotic sac bursts prematurely can prevent chorioamnionitis occurrence.
The signs and symptoms of clinical chorioamnionitis include fever, leukocytosis (>15,000 cells/mm3), maternal (>100 bpm) or fetal (>160 bpm) tachycardia, uterine tenderness and preterm rupture of membranes.
Causes of chorioamnionitis stem from bacterial infection as well as obstetric and other related factors.
Bacterial, viral, and even fungal infections can cause chorioamnionitis. Most commonly from Ureaplasma, Fusobacterium, and Streptococcus bacteria species. Less commonly, Gardnerella, Mycoplasma, and Bacteroides bacteria species. Sexually transmitted infections, chlamydia and gonorrhea, can cause development of the condition as well. Studies are continuing to identify other microorganism classes and species as infection sources.
Birthing-related events, lifestyle, and ethnic background have been linked to an increase in the risk of developing chorioamnionitis apart from bacterial causation. Premature deliveries, ruptures of the amniotic sac membranes, prolonged labor, and primigravida childbirth are associated with this condition. At term mothers who experience a combination of pre-labor membrane ruptures and multiple invasive vaginal examinations, prolonged labor, or have meconium appear in the amniotic fluid are at higher risk than at term mothers experiencing just one of those events. In other studies, smoking, alcohol use and drug use are noted as risk factors. Those of African American ethnicity are noted to be at higher risk.
The amniotic sac consists of two parts: