Recent from talks
Knowledge base stats:
Talk channels stats:
Members stats:
Allergic rhinitis
Allergic rhinitis, of which the seasonal type is called hay fever, is a type of inflammation in the nose that occurs when the immune system overreacts to allergens in the air. It is classified as a type I hypersensitivity reaction. Signs and symptoms include a runny or stuffy nose, sneezing, red, itchy, and watery eyes, and swelling around the eyes. The fluid from the nose is usually clear. Symptom onset is often within minutes following allergen exposure, and can affect sleep and the ability to work or study. Some people may develop symptoms only during specific times of the year, often as a result of pollen exposure. Many people with allergic rhinitis also have asthma, allergic conjunctivitis, or atopic dermatitis.
Allergic rhinitis is typically triggered by environmental allergens such as pollen, pet hair, dust mites, or mold. Inherited genetics and environmental exposures contribute to the development of allergies. Growing up on a farm and having multiple older siblings are associated with a reduction of this risk. The underlying mechanism involves IgE antibodies that attach to an allergen, and subsequently result in the release of inflammatory chemicals such as histamine from mast cells. It causes mucous membranes in the nose, eyes and throat to become inflamed and itchy as they work to eject the allergen. Diagnosis is typically based on a combination of symptoms and a skin prick test or blood tests for allergen-specific IgE antibodies. These tests, however, can give false positives. The symptoms of allergies resemble those of the common cold; however, they often last for more than two weeks and, despite the common name, typically do not include a fever.
Exposure to animals early in life might reduce the risk of developing these specific allergies. Several different types of medications reduce allergic symptoms, including nasal steroids, intranasal antihistamines such as olopatadine or azelastine, 2nd generation oral antihistamines such as loratadine, desloratadine, cetirizine, or fexofenadine; the mast cell stabilizer cromolyn sodium, and leukotriene receptor antagonists such as montelukast. Oftentimes, medications do not completely control symptoms, and they may also have side effects. Exposing people to larger and larger amounts of allergen, known as allergen immunotherapy, is often effective and is used when first line treatments fail to control symptoms. The allergen can be given as an injection under the skin or as a tablet under the tongue. Treatment typically lasts three to five years, after which benefits may be prolonged.
Allergic rhinitis is the type of allergy that affects the greatest number of people. In Western countries, between 10 and 30% of people are affected in a given year. It is most common between the ages of twenty and forty. The first accurate description is from the 10th-century physician Abu Bakr al-Razi. In 1859, Charles Blackley identified pollen as the cause. In 1906, the mechanism was determined by Clemens von Pirquet. The link with hay came about due to an early (and incorrect) theory that the symptoms were brought about by the smell of new hay.
The characteristic symptoms of allergic rhinitis are: rhinorrhea (excess nasal secretion), itching, sneezing fits, and nasal congestion/obstruction. Characteristic physical findings include conjunctival swelling and erythema, eyelid swelling with Dennie–Morgan folds, lower eyelid venous stasis (rings under the eyes known as "allergic shiners"), swollen nasal turbinates, and middle ear effusion. Nasal endoscopy may show findings such as pale and boggy inferior turbinates from mucosal edema, stringy mucus throughout the nasal cavities, and cobblestoning.
There can also be behavioral signs; in order to relieve the irritation or flow of mucus, people may wipe or rub their nose with the palm of their hand in an upward motion: an action known as the "nasal salute" or the "allergic salute". This may result in a crease running across the nose (or above each nostril if only one side of the nose is wiped at a time), commonly referred to as the "transverse nasal crease", and can lead to permanent physical deformity if repeated enough.
People might also find that cross-reactivity occurs. For example, people allergic to birch pollen may also find that they have an allergic reaction to the skin of apples or potatoes. A clear sign of this is the occurrence of an itchy throat after eating an apple or sneezing when peeling potatoes or apples. This occurs because of similarities in the proteins of the pollen and the food. There are many cross-reacting substances. Hay fever is not a true fever, meaning it does not cause a core body temperature in the fever over 37.5–38.3 °C (99.5–100.9 °F).[citation needed]
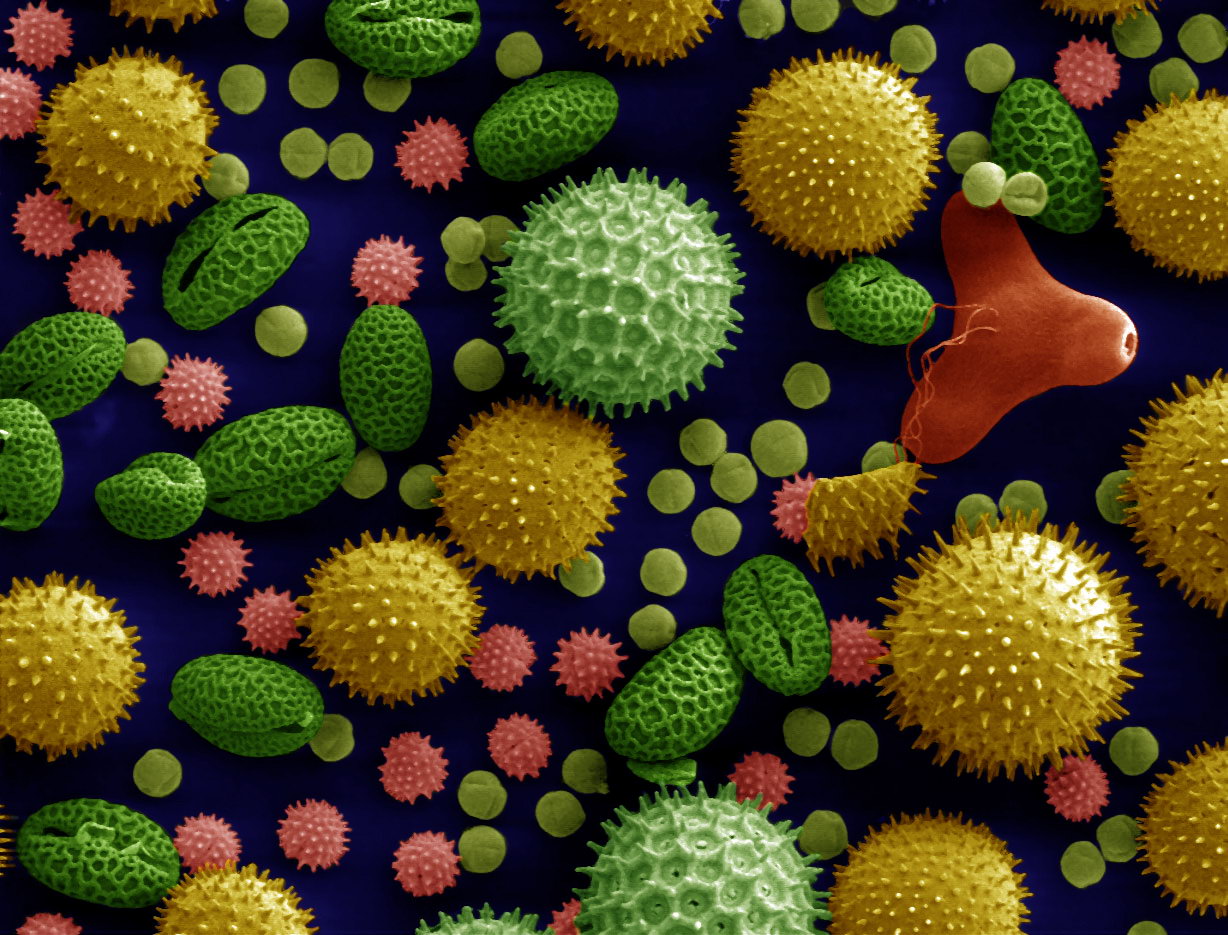
Pollen is often considered as a cause of allergic rhinitis, hence called hay fever (See sub-section below).[citation needed]
Hub AI
Allergic rhinitis AI simulator
(@Allergic rhinitis_simulator)
Allergic rhinitis
Allergic rhinitis, of which the seasonal type is called hay fever, is a type of inflammation in the nose that occurs when the immune system overreacts to allergens in the air. It is classified as a type I hypersensitivity reaction. Signs and symptoms include a runny or stuffy nose, sneezing, red, itchy, and watery eyes, and swelling around the eyes. The fluid from the nose is usually clear. Symptom onset is often within minutes following allergen exposure, and can affect sleep and the ability to work or study. Some people may develop symptoms only during specific times of the year, often as a result of pollen exposure. Many people with allergic rhinitis also have asthma, allergic conjunctivitis, or atopic dermatitis.
Allergic rhinitis is typically triggered by environmental allergens such as pollen, pet hair, dust mites, or mold. Inherited genetics and environmental exposures contribute to the development of allergies. Growing up on a farm and having multiple older siblings are associated with a reduction of this risk. The underlying mechanism involves IgE antibodies that attach to an allergen, and subsequently result in the release of inflammatory chemicals such as histamine from mast cells. It causes mucous membranes in the nose, eyes and throat to become inflamed and itchy as they work to eject the allergen. Diagnosis is typically based on a combination of symptoms and a skin prick test or blood tests for allergen-specific IgE antibodies. These tests, however, can give false positives. The symptoms of allergies resemble those of the common cold; however, they often last for more than two weeks and, despite the common name, typically do not include a fever.
Exposure to animals early in life might reduce the risk of developing these specific allergies. Several different types of medications reduce allergic symptoms, including nasal steroids, intranasal antihistamines such as olopatadine or azelastine, 2nd generation oral antihistamines such as loratadine, desloratadine, cetirizine, or fexofenadine; the mast cell stabilizer cromolyn sodium, and leukotriene receptor antagonists such as montelukast. Oftentimes, medications do not completely control symptoms, and they may also have side effects. Exposing people to larger and larger amounts of allergen, known as allergen immunotherapy, is often effective and is used when first line treatments fail to control symptoms. The allergen can be given as an injection under the skin or as a tablet under the tongue. Treatment typically lasts three to five years, after which benefits may be prolonged.
Allergic rhinitis is the type of allergy that affects the greatest number of people. In Western countries, between 10 and 30% of people are affected in a given year. It is most common between the ages of twenty and forty. The first accurate description is from the 10th-century physician Abu Bakr al-Razi. In 1859, Charles Blackley identified pollen as the cause. In 1906, the mechanism was determined by Clemens von Pirquet. The link with hay came about due to an early (and incorrect) theory that the symptoms were brought about by the smell of new hay.
The characteristic symptoms of allergic rhinitis are: rhinorrhea (excess nasal secretion), itching, sneezing fits, and nasal congestion/obstruction. Characteristic physical findings include conjunctival swelling and erythema, eyelid swelling with Dennie–Morgan folds, lower eyelid venous stasis (rings under the eyes known as "allergic shiners"), swollen nasal turbinates, and middle ear effusion. Nasal endoscopy may show findings such as pale and boggy inferior turbinates from mucosal edema, stringy mucus throughout the nasal cavities, and cobblestoning.
There can also be behavioral signs; in order to relieve the irritation or flow of mucus, people may wipe or rub their nose with the palm of their hand in an upward motion: an action known as the "nasal salute" or the "allergic salute". This may result in a crease running across the nose (or above each nostril if only one side of the nose is wiped at a time), commonly referred to as the "transverse nasal crease", and can lead to permanent physical deformity if repeated enough.
People might also find that cross-reactivity occurs. For example, people allergic to birch pollen may also find that they have an allergic reaction to the skin of apples or potatoes. A clear sign of this is the occurrence of an itchy throat after eating an apple or sneezing when peeling potatoes or apples. This occurs because of similarities in the proteins of the pollen and the food. There are many cross-reacting substances. Hay fever is not a true fever, meaning it does not cause a core body temperature in the fever over 37.5–38.3 °C (99.5–100.9 °F).[citation needed]
Pollen is often considered as a cause of allergic rhinitis, hence called hay fever (See sub-section below).[citation needed]