Recent from talks
Nothing was collected or created yet.
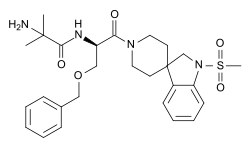
Ibutamoren
View on Wikipedia
 | |
| Clinical data | |
|---|---|
| Other names | MK-677; MK-0677; L-163,191; Oratrope |
| Routes of administration | By mouth |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Elimination half-life | 4–6 hours (in beagles);[1] IGF-1 levels remain elevated in humans with a single oral dose for up to 24 hours[2] |
| Identifiers | |
| |
| CAS Number |
|
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.236.734 |
| Chemical and physical data | |
| Formula | C27H36N4O5S |
| Molar mass | 528.67 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| (verify) | |
Ibutamoren (INN; developmental code MK-677, MK-0677, LUM-201, L-163,191; former tentative brand name Oratrope) is a potent, long-acting, orally-active, selective, and non-peptide agonist of the ghrelin receptor and a growth hormone secretagogue, mimicking the growth hormone (GH)-stimulating action of the endogenous hormone ghrelin.[3][4][5][6][7] It has been shown to increase the secretion of several hormones including GH and insulin-like growth factor 1 (IGF-1) and produces sustained increases in the plasma levels of these hormones while also raising cortisol levels.[8]
Effect on lean mass
[edit]Ibutamoren has been shown to sustain activation of the GH–IGF-1 axis, increasing growth hormone secretion by up to 97%,[9] and to increase lean body mass with no change in total fat mass or visceral fat. It is under investigation as a potential treatment for reduced levels of these hormones, such as in children or elderly adults with growth hormone deficiency,[3][10][11][12] and human studies have shown it to increase both muscle mass and bone mineral density,[13][14] making it a promising potential therapy for the treatment of frailty in the elderly.[15][16] As of June 2017, ibutamoren is in the preclinical stage of development for growth hormone deficiency.[3]
Effect on sleep architecture
[edit]In a small study of 14 subjects, ibutamoren dosed at 25 mg/day at bedtime was shown to increase rapid eye movement sleep by 20% and 50% in young and older subjects respectively.[17] Treatment with ibutamoren also resulted in an approximate 50% increase in slow-wave sleep in young subjects.[17]
Growth hormone deficiency
[edit]In a study of children with growth hormone deficiency, ibutamoren performed better than other growth hormone secretagogues at improving growth hormone levels.[18] An ongoing study compares ibutamoren directly to injectable hGH in terms of height velocity in this population.[19] Topline data from Phase 2 OraGrowtH210 and OraGrowtH212 Trials of LUM-201 in PGHD met all primary and secondary endpoints.
Non-research use
[edit]Since ibutamoren is still an Investigational New Drug, it has not yet been approved to be marketed for consumption by humans in the United States.[3] However, it has been used experimentally by some in the bodybuilding community. The use of ibutamoren is banned in most sports.[20]
See also
[edit]References
[edit]- ^ Smith RG, Thorner MO (28 January 2000). Human Growth Hormone: Research and Clinical Practice. Springer Science & Business Media. pp. 45–. ISBN 978-1-59259-015-5.
- ^ Smith RG, Van der Ploeg LH, Howard AD, Feighner SD, Cheng K, Hickey GJ, et al. (October 1997). "Peptidomimetic regulation of growth hormone secretion". Endocrine Reviews. 18 (5). The Endocrine Society: 621–645. doi:10.1210/edrv.18.5.0316. PMID 9331545.
- ^ a b c d "Ibutamoren - Lumos Pharma/Merck". AdisInsight. Archived from the original on 2018-09-27. Retrieved 2017-12-14.
- ^ Patchett AA, Nargund RP, Tata JR, Chen MH, Barakat KJ, Johnston DB, et al. (July 1995). "Design and biological activities of L-163,191 (MK-0677): a potent, orally active growth hormone secretagogue". Proceedings of the National Academy of Sciences of the United States of America. 92 (15): 7001–7005. Bibcode:1995PNAS...92.7001P. doi:10.1073/pnas.92.15.7001. PMC 41459. PMID 7624358.
- ^ Pong SS, Chaung LY, Dean DC, Nargund RP, Patchett AA, Smith RG (January 1996). "Identification of a new G-protein-linked receptor for growth hormone secretagogues". Molecular Endocrinology. 10 (1): 57–61. doi:10.1210/mend.10.1.8838145. PMID 8838145.
- ^ Cassoni P, Papotti M, Ghè C, Catapano F, Sapino A, Graziani A, et al. (April 2001). "Identification, characterization, and biological activity of specific receptors for natural (ghrelin) and synthetic growth hormone secretagogues and analogs in human breast carcinomas and cell lines". The Journal of Clinical Endocrinology and Metabolism. 86 (4): 1738–1745. doi:10.1210/jcem.86.4.7402. PMID 11297611.
- ^ Holst B, Frimurer TM, Mokrosinski J, Halkjaer T, Cullberg KB, Underwood CR, Schwartz TW (January 2009). "Overlapping binding site for the endogenous agonist, small-molecule agonists, and ago-allosteric modulators on the ghrelin receptor". Molecular Pharmacology. 75 (1): 44–59. doi:10.1124/mol.108.049189. PMID 18923064. S2CID 2218638.
- ^ Nass R, Pezzoli SS, Oliveri MC, Patrie JT, Harrell FE Jr, Clasey JL, et al. (November 2008). "Effects of an oral ghrelin mimetic on body composition and clinical outcomes in healthy older adults: a randomized trial". Annals of Internal Medicine. 149 (9): 601–611. doi:10.7326/0003-4819-149-9-200811040-00003. PMC 2757071. PMID 18981485.
- ^ Chapman IM (1996). "Stimulation of the growth hormone (gh)-insulin-like growth factor I axis by Daily Oral Administration of a GH secretogogue (MK-677) in healthy elderly subjects". Journal of Clinical Endocrinology & Metabolism. 81 (12): 4249–4257. doi:10.1210/jcem.81.12.8954023. PMID 8954023.
- ^ Chapman IM, Bach MA, Van Cauter E, Farmer M, Krupa D, Taylor AM, et al. (December 1996). "Stimulation of the growth hormone (GH)-insulin-like growth factor I axis by daily oral administration of a GH secretogogue (MK-677) in healthy elderly subjects". The Journal of Clinical Endocrinology and Metabolism. 81 (12): 4249–4257. doi:10.1210/jcem.81.12.8954023. PMID 8954023.
- ^ Thorner MO, Chapman IM, Gaylinn BD, Pezzoli SS, Hartman ML (1997). "Growth hormone-releasing hormone and growth hormone-releasing peptide as therapeutic agents to enhance growth hormone secretion in disease and aging". Recent Progress in Hormone Research. 52: 215–44, discussion 244–6. PMID 9238854.
- ^ Chapman IM, Pescovitz OH, Murphy G, Treep T, Cerchio KA, Krupa D, et al. (October 1997). "Oral administration of growth hormone (GH) releasing peptide-mimetic MK-677 stimulates the GH/insulin-like growth factor-I axis in selected GH-deficient adults". The Journal of Clinical Endocrinology and Metabolism. 82 (10): 3455–3463. doi:10.1210/jcem.82.10.4297. PMID 9329386.
- ^ Murphy MG, Bach MA, Plotkin D, Bolognese J, Ng J, Krupa D, et al. (July 1999). "Oral administration of the growth hormone secretagogue MK-677 increases markers of bone turnover in healthy and functionally impaired elderly adults. The MK-677 Study Group". Journal of Bone and Mineral Research. 14 (7): 1182–1188. doi:10.1359/jbmr.1999.14.7.1182. PMID 10404019.
- ^ Murphy MG, Weiss S, McClung M, Schnitzer T, Cerchio K, Connor J, et al. (March 2001). "Effect of alendronate and MK-677 (a growth hormone secretagogue), individually and in combination, on markers of bone turnover and bone mineral density in postmenopausal osteoporotic women". The Journal of Clinical Endocrinology and Metabolism. 86 (3): 1116–1125. doi:10.1210/jcem.86.3.7294. PMID 11238495.
- ^ Smith RG, Sun Y, Jiang H, Albarran-Zeckler R, Timchenko N (November 2007). "Ghrelin receptor (GHS-R1A) agonists show potential as interventive agents during aging". Annals of the New York Academy of Sciences. 1119 (1): 147–164. Bibcode:2007NYASA1119..147S. doi:10.1196/annals.1404.023. PMID 18056963. S2CID 3220799.
- ^ "An Anti-frailty Pill For Seniors? New Drug Increases Muscle Mass In Arms And Legs Of Older Adults". ScienceDaily. 5 November 2008. Archived from the original on 7 November 2017. Retrieved 28 February 2018.
- ^ a b Copinschi G, Leproult R, Van Onderbergen A, Caufriez A, Cole KY, Schilling LM, et al. (October 1997). "Prolonged oral treatment with MK-677, a novel growth hormone secretagogue, improves sleep quality in man". Neuroendocrinology. 66 (4): 278–286. doi:10.1159/000127249. PMID 9349662.
- ^ Bright GM, Thorner MO (30 March 2022). "A GH Secretagogue Receptor Agonist (LUM-201) Elicits Greater GH Responses than Standard GH Secretagogues in Subjects of a Pediatric GH Deficiency Trial". Hormone Research in Paediatrics. 95 (1): 76–81. doi:10.1159/000524244. PMC 9227666. PMID 35354138.
- ^ "Phase 2 Study of LUM-201 in Children With Growth Hormone Deficiency (OraGrowtH210 Trial) - Full Text View". clinicaltrials.gov. Archived from the original on 4 September 2023. Retrieved 4 September 2023.
- ^ "Ibutamoren (MK 677) not OK - Don't be fooled by marketing!". Integrity Blog. Sport Integrity Australia. 23 May 2022. Archived from the original on 9 April 2024. Retrieved 9 April 2024.

