Recent from talks
Nothing was collected or created yet.
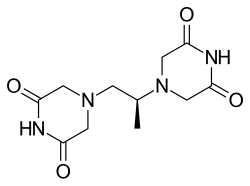
Dexrazoxane
View on Wikipedia
 | |
| Clinical data | |
|---|---|
| Trade names | Zinecard, others |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a609010 |
| License data |
|
| Routes of administration | Intravenous |
| ATC code | |
| Legal status | |
| Legal status | |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.163.459 |
| Chemical and physical data | |
| Formula | C11H16N4O4 |
| Molar mass | 268.273 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| (verify) | |
Dexrazoxane hydrochloride, sold under the brand name Zinecard among others, is a cardioprotective agent. It was discovered in 1972. The IV administration of dexrazoxane is in acidic condition with HCl adjusting the pH.[3]
Medical uses
[edit]Dexrazoxane has been used to protect the heart against the cardiotoxic side effects of chemotherapeutic drugs such as anthracyclines,[4] such as daunorubicin or doxorubicin or other chemotherapeutic agents.[5] However, in July 2011 the European Medicines Agency (EMA) released a statement restricting use only in adult patients with cancer who have received > 300 mg/m2 doxorubicin or > 540 mg/m2 epirubicin and general approval for use for cardioprotection.[6][7] That showed a possibly higher rate of secondary malignancies and acute myelogenous leukemia in pediatric patients treated for different cancers with both dexrazoxane and other chemotherapeutic agents that are associated with secondary malignancies.[8] On 19 July 2017, based on evaluation of the currently available data the European Commission issued an EU-wide legally binding decision to implement the recommendations of the Committee for Medicinal Products for Human Use (CHMP) on dexrazoxane and lifted its 2011-contraindication for primary prevention of anthracycline-induced cardiotoxicity with dexrazoxane in children and adolescents where high doses (≥ 300 mg/m3) of anthracyclines are anticipated.
Dexrazoxane was designated by the US FDA as an orphan drug for "prevention of cardiomyopathy for children and adults 0 through 16 years of age treated with anthracyclines".[9] This decision allows virtually all children to receive dexrazoxane starting with the first dose of anthracycline at the discretion of the treating provider. The label change by the agency announcing dexrazoxane as an approved cardio-oncology protectant has been followed by a review by the agency.[10] Currently, the only FDA and EMA approved cardioprotective treatment for anthracycline cardioprotection is dexrazoxane, which provides effective primary cardioprotection against anthracycline-induced cardiotoxicity without reducing anthracycline activity and without enhancing secondary malignancies.[11]
The United States Food and Drug Administration has also approved a dexrazoxane for use as a treatment of extravasation resulting from IV anthracycline chemotherapy.[12][13] Extravasation is an adverse event in which chemotherapies containing anthracylines leak out of the blood vessel and necrotize the surrounding tissue.
Mechanism
[edit]As a derivative of EDTA, dexrazoxane chelates iron and thus reduces the number of metal ions complexed with anthracycline and, consequently, decrease the formation of superoxide radicals.[14] The exact chelation mechanism is unknown, but it has been postulated that dexrazoxane can be converted into ring-opened form intracellularly and interfere with iron-mediated free radical generation that is in part thought to be responsible for anthracycline induced cardiomyopathy.[15] It was speculated that dexrazoxane could be used for further investigation to synthesize new antimalarial drugs.[16]
References
[edit]- ^ "Dexrazoxane-Reach (Reach Pharmaceuticals Pty Ltd)". Therapeutic Goods Administration (TGA). 16 April 2025. Retrieved 3 May 2025.
- ^ "Savene EPAR". European Medicines Agency (EMA). 19 September 2001. Retrieved 7 September 2024.
- ^ "Zinecard (Dexrazoxane): Side Effects, Interactions, Warning, Dosage & Uses".
- ^ Lipshultz SE, Rifai N, Dalton VM, Levy DE, Silverman LB, Lipsitz SR, et al. (July 2004). "The effect of dexrazoxane on myocardial injury in doxorubicin-treated children with acute lymphoblastic leukemia". The New England Journal of Medicine. 351 (2): 145–53. doi:10.1056/NEJMoa035153. PMID 15247354.
{{cite journal}}: CS1 maint: overridden setting (link) - ^ Bjelogrlic SK, Radic J, Radulovic S, Jokanovic M, Jovic V (December 2007). "Effects of dexrazoxane and amifostine on evolution of Doxorubicin cardiomyopathy in vivo". Experimental Biology and Medicine. 232 (11): 1414–24. doi:10.3181/0705-RM-138. PMID 18040065. S2CID 20119026.
- ^ Tebbi CK, London WB, Friedman D, Villaluna D, De Alarcon PA, Constine LS, et al. (February 2007). "Dexrazoxane-associated risk for acute myeloid leukemia/myelodysplastic syndrome and other secondary malignancies in pediatric Hodgkin's disease". Journal of Clinical Oncology. 25 (5): 493–500. doi:10.1200/JCO.2005.02.3879. PMID 17290056.
{{cite journal}}: CS1 maint: overridden setting (link) - ^ Salzer WL, Devidas M, Carroll WL, Winick N, Pullen J, Hunger SP, et al. (February 2010). "Long-term results of the pediatric oncology group studies for childhood acute lymphoblastic leukemia 1984-2001: a report from the children's oncology group". Leukemia. 24 (2): 355–70. doi:10.1038/leu.2009.261. PMC 4300959. PMID 20016527.
- ^ "FDA Statement on Dexrazoxane". Food and Drug Administration. Archived by the Wayback Machine. 20 July 2011. Archived from the original on 18 August 2011. Retrieved 29 October 2023.
- ^ "Orphan drug designations and approvals". Retrieved 7 June 2019.
- ^ "Cardioxane". 17 September 2018.
- ^ Reichardt P, Tabone MD, Mora J, Morland B, Jones RL (October 2018). "Risk-benefit of dexrazoxane for preventing anthracycline-related cardiotoxicity: re-evaluating the European labeling". Future Oncology. 14 (25): 2663–2676. doi:10.2217/fon-2018-0210. PMID 29747541.
- ^ "NDA 22-025 TOTECT™ (DEXRAZOXANE) FOR INJECTION | Totect™ Package Insert" (PDF). FDA. Archived by the Wayback Machine. Archived from the original (PDF) on 25 March 2009. Retrieved 29 October 2023.
- ^ Kane RC, McGuinn WD, Dagher R, Justice R, Pazdur R (April 2008). "Dexrazoxane (Totect): FDA review and approval for the treatment of accidental extravasation following intravenous anthracycline chemotherapy". The Oncologist. 13 (4): 445–50. doi:10.1634/theoncologist.2007-0247. PMID 18448560. S2CID 7753443.
- ^ Jones RL (November 2008). "Utility of dexrazoxane for the reduction of anthracycline-induced cardiotoxicity". Expert Review of Cardiovascular Therapy. 6 (10): 1311–7. doi:10.1586/14779072.6.10.1311. PMID 19018683. S2CID 25950994.
- ^ "ZINECARD- dexrazoxane hydrochloride injection, powder, lyophilized, for solution". Pharmacia and Upjohn Company LLC.
- ^ Loyevsky M, Sacci JB, Boehme P, Weglicki W, John C, Gordeuk VR (February 1999). "Plasmodium falciparum and Plasmodium yoelii: effect of the iron chelation prodrug dexrazoxane on in vitro cultures". Experimental Parasitology. 91 (2): 105–14. doi:10.1006/expr.1998.4371. PMID 9990337.

