Recent from talks
Nothing was collected or created yet.
Cementoenamel junction
View on Wikipedia| Cementoenamel junction | |
|---|---|
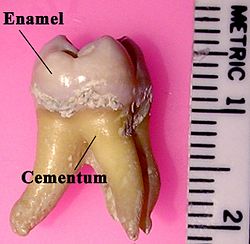
 Labeled molar | |
 The CEJ is the more or less horizontal demarcation line that distinguishes the crown (A) of the tooth from root (B) of the tooth. | |
| Identifiers | |
| MeSH | D019237 |
| TA2 | 926 |
| FMA | 55627 |
| Anatomical terminology | |
In dental anatomy, the cementoenamel junction (CEJ) is the location where the enamel, which covers the anatomical crown of a tooth, and the cementum, which covers the anatomical root of a tooth, meet. Informally it is known as the neck of the tooth.[1] The border created by these two dental tissues has much significance as it is usually the location where the gingiva (gums) attaches to a healthy tooth by fibers called the gingival fibers.[2]
Active recession of the gingiva reveals the cementoenamel junction in the mouth and is usually a sign of an unhealthy condition. The loss of attachment is considered a more reliable indicator of periodontal disease. The CEJ is the site of major tooth resorption. A significant proportion of tooth loss is caused by tooth resorption, which occurs in 5 to 10 percent of the population. The clinical location of CEJ which is a static landmark, serves as a crucial anatomical site for the measurement of probing pocket depth (PPD) and clinical attachment level (CAL). The CEJ varies between subjects, but also between teeth from the same person.[1]
There exists a normal variation in the relationship of the cementum and the enamel at the cementoenamel junction. In about 60–65% of teeth, the cementum overlaps the enamel at the CEJ, while in about 30% of teeth, the cementum and enamel abut each other with no overlap. In only 5–10% of teeth, there is a space between the enamel and the cementum at which the underlying dentin is exposed.[3]
Formation
[edit]In the tooth bud, regions where enamel formation is completed, the enamel organ gives rise to Hertwig's epithelial root sheath, composed of two epithelial layers derived from the external and internal epithelia. The sheath is irregularly fragmented in time and space as it promotes cementum deposition on the newly formed dentin. After this fragmentation, Hertwig's epithelial root sheath also participates in cementogenesis and formation of the periodontal ligament, giving rise to the epithelial rests of Malassez. This irregular fragmentation of Hertwig's epithelial root sheath yields an equally irregular limit of cervical enamel and an irregular onset of formation and deposition of cementum. Consequently, the relationship between cementum and enamel at the CEJ presents an irregular contour, as observed during scanning electron microscope (SEM) analysis of the primary teeth.
Fragmentation of Hertwig's epithelial root sheath and exposure of dentin covered by a thin layer of intermediate cementum are fundamental for the onset of cementogenesis. If Hertwig's epithelial root sheath is not fragmented, there will be enamel deposition and it will be transformed into reduced epithelium, thus preventing cementum deposition on its surface.[4]
Types
[edit]- Coronal cementum - where the enamel overlaps the cement.
- Abutment - It is also known as vis a vis relation, where the cement and enamel meet at the butt joint, occurring in 30% of sections, and the least common, occurring in 10% of sections.
- Gap between cementum and enamel exposing the dentin.[5]
Curvature
[edit]
The shape and location of the cementoenamel junction (CEJ) on each tooth surface should be considered. CEJs differ from tooth to tooth in terms of their anatomy. The curvature of the CEJ is greatest on anterior teeth due to the narrow profile of these teeth.[6] On the anteriors, the distal aspect's curvature is usually one mm lower than the mesial aspect. Posterior teeth have flatter CEJ curvatures on the inter-proximal surfaces in comparison to the anteriors.[7]
Teeth resorption
[edit]Root resorption often starts at cementoenamel junction (CEJ) in teeth. Types of tooth resorption include internal resorption and external resorption.[8]
Internal
[edit]There are two types of internal resorption - root canal (internal) replacement resorption and internal inflammatory resorption.

External
[edit]External resorption can be classified into four categories by its clinical and histologic manifestations: external surface resorption, external inflammatory root resorption, replacement resorption, and ankylosis. External inflammatory root resorption can be further categorized into cervical resorption with or without a vital pulp (invasive cervical root resorption) and external apical root resorption.[8]
References
[edit]- ^ a b Vandana KL, Haneet RK (September 2014). "Cementoenamel junction: An insight". Journal of Indian Society of Periodontology. 18 (5): 549–554. doi:10.4103/0972-124X.142437. PMC 4239741. PMID 25425813.
- ^ Clemente CD (1987). Anatomy, a regional atlas of the human body. Internet Archive. Baltimore : Urban & Schwarzenberg. ISBN 978-0-8067-0323-7.
- ^ Carranza FA, Bernard GW (2002). "The Tooth-Supporting Structures". In Newman MG, Takei HH, Carranza FA (eds.). Carranza's Clinical Periodontology (9th ed.). Philadelphia: W. B. Saunders. p. 43. ISBN 978-0-7216-8331-7.
- ^ Scheid RC (2012). Woelfel's Dental Anatomy (7th ed.). Lippincott Williams & Wilkins. ISBN 978-1-60831-746-2.
- ^ Metwally S, Stachewicz U (October 2020). "Teeth resorption at cement - enamel junction (CEJ) - Microscopy analysis". Micron. 137 102913. doi:10.1016/j.micron.2020.102913. PMID 32590194. S2CID 220120744.
- ^ "Remembering Your Roots". Dimensions of Dental Hygiene | Magazine. 2021-09-22. Retrieved 2023-08-07.
- ^ Nelson SJ, Ash MM (2010). Wheeler's dental anatomy, physiology, and occlusion (9th ed.). Philadelphia, Pa., London: Saunders. ISBN 978-1-4160-6209-7.
- ^ a b Ne RF, Witherspoon DE, Gutmann JL (January 1999). "Tooth resorption". Quintessence International. 30 (1): 9–25. PMID 10323155.
External links
[edit]- Biology-Online Archived 2008-10-08 at the Wayback Machine