Recent from talks
Nothing was collected or created yet.
Apical foramen
View on Wikipedia| Apical foramen | |
|---|---|
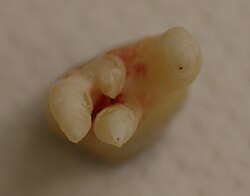
 Apical foramina on a wisdom tooth | |
| Details | |
| Identifiers | |
| Latin | foramen apicis dentis |
| TA98 | A05.1.03.050 |
| TA2 | 933 |
| FMA | 57159 |
| Anatomical terminology | |

17. Periodontium
:18. Gingiva: ::19. free or interdental ::20. marginal ::21. alveolar :22. Periodontal ligament :23. Alveolar bone 24. Vessels and nerves: :25. dental :26. periodontal :27. alveolar through channel
In dental anatomy, the apical foramen, literally translated "small opening of the apex," is the tooth's natural opening, found at the root's very tip—that is, the root apex — whereby an artery, vein, and nerve enter the tooth and commingle with the tooth's internal soft tissue, called pulp. Additionally, the apical foramen is the point where the pulp meets the periodontal tissues, the connective tissues that surround and support the tooth. The foramen is located 0.5mm to 1.5mm from the apex of the tooth. Each tooth has an apical foramen.[1]
Characteristics
[edit]The average size of the orifice is 0.3 to 0.4 mm in diameter. There can be two or more foramina separated by a portion of dentin and cementum or by cementum only. If more than one foramen is present on each root, the largest one is designated as the apical foramen and the rest are considered accessory foramina.[1][2]
Apical delta
[edit]Apical delta refers to the branching pattern of small accessory canals and minor foramina seen at the tip or apex of some tooth roots. The pattern is said to be reminiscent of a river delta when sectioned and viewed using a microscope. Because the anatomy of this area is very small and complex with several portals of entry to the root canal i.e. more than one apical foramen.[1]
Endodontic treatment
[edit]It is a point of interest in endodontics, as it is considered necessary to thoroughly chemomechanically debride the pulp space to remove all necrotic tissue and minimise bacterial load in the pulp space. Ideally, this debridement would terminate exactly at the apical foramen. In reality, determining the exact position of the apical foramen is problematic, requiring radiography and/or use of an electronic apex locator to produce a refined estimate. A tooth may have multiple small accessory canals in the root apex area forming an apical delta which can complicate the endodontic problem.[1]
The presence of an apical delta may make successful endodontic treatment less likely. The root tip is removed during apicoectomy to eliminate the apical delta and maximise the chance of successful healing.[1]
An apical constriction is often present. In immature teeth the root is not fully formed, leading to an open apex. This is also seen in some pathological teeth.[1]
References
[edit]- ^ a b c d e f Color Atlas and Textbook of Oral Anatomy, Histology, and Embryology by B. K. Berkovitz, G. R. Holland, B. J. Moxham Hardcover, Mosby, ISBN 0-8151-0697-1 (0-8151-0697-1)
- ^ Elmar Hellwig, Joachim Klimek, Thomas Attin (2013). Einführung in die Zahnerhaltung. Deutscher Ärzte-Verlag GmbH. p. 366. ISBN 978-3-7691-3448-3.
{{cite book}}: CS1 maint: multiple names: authors list (link)