Recent from talks
All channels
Be the first to start a discussion here.
Be the first to start a discussion here.
Be the first to start a discussion here.
Be the first to start a discussion here.
Welcome to the community hub built to collect knowledge and have discussions related to Anterior segment of eyeball.
Nothing was collected or created yet.
Anterior segment of eyeball
View on Wikipediafrom Wikipedia
| Anterior segment of eyeball | |
|---|---|
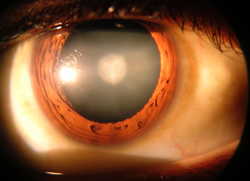
 Human eye Anterior Segment - Magnified view seen on examination with a slit lamp under diffuse illumination showing conjunctiva overlying the white sclera, transparent cornea, pharmacologically dilated pupil and cataract | |
| Details | |
| Identifiers | |
| Latin | segmentum anterius bulbi oculi |
| MeSH | D000869 |
| Anatomical terminology | |

1. Lens, 2. Zonule of Zinn or ciliary zonule, 3. Posterior chamber and 4. Anterior chamber with 5. Aqueous humour flow; 6. Pupil, 7. Corneosclera with 8. Cornea, 9. Trabecular meshwork and Schlemm's canal. 10. Corneal limbus and 11. Sclera; 12. Conjunctiva, 13. Uvea with 14. Iris, 15. Ciliary body.
The anterior segment or anterior cavity[1] is the front third of the eye that includes the structures in front of the vitreous humour: the cornea, iris, ciliary body, and lens.[2][3][4]
Within the anterior segment are two fluid-filled spaces:
- the anterior chamber between the posterior surface of the cornea (i.e. the corneal endothelium) and the iris.
- the posterior chamber between the iris and the front face of the vitreous.[2]
Aqueous humour fills these spaces within the anterior segment and provides nutrients to the surrounding structures.
Some ophthalmologists and optometrists specialize in the treatment and management of anterior segment disorders and diseases.[3]
See also
[edit]References
[edit]- ^ "Medical gallery of Blausen Medical 2014". WikiJournal of Medicine. 1 (2). 29 August 2014. doi:10.15347/WJM/2014.010.
- ^ a b Cassin, B. and Solomon, S. Dictionary of Eye Terminology. Gainesville, Florida: Triad Publishing Company, 1990.
- ^ a b "Departments. Anterior segment." Archived September 27, 2006, at the Wayback Machine Cantabrian Institute of Ophthalmology.
- ^ Fraser, AS; Ang, M; Bellchambers, A; Chu, CJ; Denniston, AK; Downie, LE; Evans, T; Hau, S; Huang, AS; Keane, PA; Liu, X; Mehta, JS; Ometto, G; Petzold, A; Tsui, E; Fraser, TS; Xu, B; Thaung, C; Solebo, AL (14 August 2025). "Proposed Nomenclature for Landmarks in Anterior-Segment OCT: The APOSTEL-AS Panel Consensus". JAMA Ophthalmology. 143 (9): 749–757. doi:10.1001/jamaophthalmol.2025.2414. PMC 12355391. PMID 40810988.
External links
[edit]- Anterior+Eye+Segment at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
Anterior segment of eyeball
View on Grokipediafrom Grokipedia
Anatomy
Cornea
The cornea is the transparent, avascular dome-shaped anterior portion of the outer fibrous layer of the eye, serving as the primary refractive surface of the anterior segment. It consists of five main layers, each contributing to its structural integrity, transparency, and optical function. The outermost layer is the epithelium, a non-keratinized stratified squamous epithelium approximately 50 μm thick, composed of 5–7 layers of basal, wing, and superficial cells that provide a protective barrier and regenerate rapidly from stem cells in the limbus. Beneath it lies Bowman's layer, an acellular sheet of type I and V collagen about 12 μm thick, which interfaces the epithelium and stroma but does not regenerate if damaged, potentially leading to scarring. The stroma forms the bulk of the cornea, comprising 80–85% of its thickness with regularly arranged collagen lamellae that ensure transparency through precise fibril organization and minimal light scattering. Descemet's membrane, a thin elastic basement membrane of type IV collagen secreted by the endothelium, measures about 7 μm and thickens with age to 10 μm, providing structural support. The innermost endothelium is a single layer of hexagonal cells, approximately 5 μm thick, responsible for pumping ions and fluid to maintain corneal dehydration and clarity, though it lacks regenerative capacity in adults.[7][8] In terms of dimensions, the human cornea has a horizontal diameter of 11–12 mm and a vertical diameter of 9–11 mm, with central thickness ranging from 551–565 μm and peripheral thickness from 612–640 μm, making it thinnest at the center to optimize refraction. Optically, the cornea provides the majority of the eye's refractive power, contributing approximately 40–44 diopters and accounting for 65–75% of total focusing ability due to its high refractive index of 1.376 and anterior surface curvature radius of about 7.8 mm. Its transparency is maintained by the uniform diameter and spacing of stromal collagen fibrils (around 300–400 molecules per fibril), which minimize light scattering, while avascularity prevents vascular interference with light transmission; nourishment occurs primarily via diffusion from the aqueous humor, with minor contributions from the tear film and limbal vessels. The cornea is densely innervated by branches of the long ciliary and nasociliary nerves from the ophthalmic division of the trigeminal nerve (CN V1), forming a sub-basal nerve plexus with 300–600 times the density of skin nociceptors, conferring high sensitivity to touch, temperature, and chemicals for protective reflexes.[7][8] Endothelial cell density is notably high at birth, approximately 4,000 cells/mm², decreasing progressively with age to about 3,000 cells/mm² in young adults and further to around 2,500 cells/mm² by age 60 in healthy individuals, reflecting gradual attrition without replacement and underscoring the layer's vulnerability to stressors.[9]Iris and pupil
The iris is a thin, circular diaphragm composed of connective tissue and smooth muscle that forms the colored portion of the eye, positioned anterior to the lens and posterior to the cornea. It consists of several layers, including the anterior stroma—a loose connective tissue network featuring crypts (diamond-shaped openings) and furrows (radial folds) that contribute to its textured surface—and a posterior pigmented epithelium derived from the neuroectoderm of the optic cup.[10][11] The iris root, or periphery, attaches directly to the ciliary body, while its central unbound margin defines the pupil, which separates the anterior and posterior chambers of the eye.[10] The musculature of the iris includes two primary smooth muscle components, both originating from the neuroectoderm of the optic cup: the sphincter pupillae, a circular band of muscle fibers located near the pupillary margin that contracts to constrict the pupil (miosis), and the dilator pupillae, radially oriented fibers extending from the iris root that contract to dilate the pupil (mydriasis).[10][12] These muscles enable precise regulation of light entry into the eye, with the sphincter pupillae innervated by parasympathetic fibers from the oculomotor nerve (cranial nerve III) via the ciliary ganglion, and the dilator pupillae supplied by sympathetic fibers from the superior cervical ganglion.[10][13] The pupil serves as a dynamic aperture, typically ranging from 2 to 8 mm in diameter depending on lighting conditions, with an average resting size of 3 to 4 mm in bright light to optimize retinal illumination while minimizing optical aberrations.[14][15] Its size is modulated by the pupillary light reflex, where afferent signals travel via the optic nerve (cranial nerve II) from retinal ganglion cells to the pretectal nucleus in the midbrain, then efferent signals via the oculomotor nerve to the iris sphincter, resulting in bilateral constriction to protect the retina from excessive light.[16] Variations in iris color arise primarily from the concentration and distribution of melanin in the anterior border layer and stroma, with higher melanin levels producing brown eyes through light absorption, while lower levels allow structural scattering of shorter blue wavelengths for lighter colors like blue or green.[17][18] The crypts and furrows in the anterior stroma enhance this effect by influencing light scattering and reflection, with deeper crypts in lighter irises promoting greater diffusion of light to create the appearance of blue hues.[11]Ciliary body
The ciliary body represents the anterior continuation of the choroid as part of the uveal tract, forming a ring-shaped structure that encircles the lens and extends from the ora serrata posteriorly to just behind the corneoscleral junction anteriorly.[19] It measures approximately 6 mm in width and consists of two main components: the ciliary muscle and the ciliary processes.[19] The ciliary processes, numbering 70 to 80 radially oriented folds, are located in the anterior pars plicata portion, which is pigmented and highly secretory, while the posterior pars plana is relatively avascular and non-secretory, serving primarily as a structural zone suitable for surgical access.[19] These processes are lined by a double-layered epithelium—pigmented and non-pigmented—that facilitates the production of aqueous humor through mechanisms including ultrafiltration driven by hydrostatic pressure and diffusion across the blood-aqueous barrier.[20] The ciliary muscle, a smooth muscle component, is organized into three meridians of fibers: longitudinal (meridional or Brücke's), radial (oblique), and circular (Müller's).[19] The longitudinal fibers insert into the scleral spur and trabecular meshwork, contributing to the regulation of aqueous outflow, while the circular fibers encircle the lens equator to modulate zonular tension.[19] Innervated primarily by parasympathetic fibers from the oculomotor nerve (cranial nerve III) via the ciliary ganglion and short ciliary nerves, contraction of these muscles alters the shape of the lens for focusing.[19] The ciliary body receives its vascular supply from the anterior ciliary arteries, branches of the ophthalmic artery, which anastomose with posterior ciliary arteries to nourish the processes and muscle.[19] Functionally, the ciliary body is responsible for secreting the aqueous humor at a rate of 2 to 3 μl per minute, essential for maintaining intraocular pressure and providing nutrients to avascular structures like the lens and cornea.[19][20] This secretion occurs via active ion transport in the non-pigmented epithelium, supported by numerous mitochondria and aquaporin channels for water movement, with the processes' capillary networks supplying plasma ultrafiltrate.[20] The ciliary body attaches at its anterior margin to the iris root and connects posteriorly to the zonular ligaments that suspend the lens.[19]Lens
The crystalline lens is a biconvex, transparent, and avascular structure positioned behind the iris and suspended by zonular fibers from the ciliary body, serving as the primary adjustable refractive element in the anterior segment of the eye.[21] It consists of three main layers: an elastic capsule, a single layer of anterior epithelium, and elongated lens fibers that form the bulk of its mass.[22] The capsule is a thin, basement membrane-like structure composed primarily of type IV collagen and laminin, providing structural support and facilitating interaction with zonular fibers.[21] The anterior epithelium comprises a monolayer of cuboidal, hexagonal cells that are mitotically active at the equator, where they differentiate into lens fibers.[22] These fibers are highly elongated, anucleated cells lacking organelles, organized into concentric layers: the outer cortex of newer, softer fibers and the inner nucleus of older, compacted fibers, ensuring optical clarity through minimal extracellular space and tight packing.[21] The lens's composition is optimized for transparency and refraction, with approximately 65-70% water content and the remainder primarily soluble proteins, including alpha-, beta-, and gamma-crystallins, which constitute up to 90% of the soluble protein fraction.[23] These crystallins create a gradient refractive index, increasing from about 1.38 in the cortex to 1.42 in the nucleus, which minimizes spherical aberration and enables efficient light focusing.[21] Being avascular, the lens relies on anaerobic glycolysis for metabolism, with glucose and nutrients diffusing from the aqueous and vitreous humors via gap junctions between fibers.[22] Lens growth occurs lifelong through the continuous addition of new fibers at the equator, resulting in a biphasic pattern: rapid prenatal growth forming a fixed nuclear core, followed by linear postnatal expansion of the cortex.[24] In adults, the lens reaches a diameter of approximately 10 mm and a thickness of about 4 mm, with an annual increase in thickness of roughly 0.012 mm.[24] This growth contributes to the lens providing 15-20 diopters of refractive power in the non-accommodated state, accounting for about 20% of the eye's total focusing ability.[25] With age, progressive hardening due to nuclear compaction and protein aggregation reduces flexibility, leading to presbyopia typically by the fifth decade of life.[21]Chambers and aqueous humor
The anterior chamber is the fluid-filled space bounded anteriorly by the posterior surface of the cornea and posteriorly by the anterior surface of the iris, with the pupil serving as the central communication pathway to the posterior chamber.[26] Its typical depth measures approximately 3 mm in adults, varying slightly with age and ethnicity.[9] The posterior chamber, in contrast, is a narrow cleft-like space located between the posterior surface of the iris and the anterior surface of the lens, including the zonular fibers; it communicates freely with the anterior chamber through the pupillary aperture.[18] Both chambers are filled with aqueous humor, a clear, low-viscosity fluid that constitutes about 99% water and maintains the structural integrity of the anterior segment.[27] This fluid has a pH of approximately 7.4 and is isosmotic to plasma, with a composition featuring electrolytes similar to plasma ultrafiltrate, glucose at about 75% of plasma levels, high concentrations of ascorbate (20-50 times that of plasma for antioxidant protection), and very low protein content (<0.02 g/dL).[28] The total volume of aqueous humor is roughly 0.25 mL, distributed as approximately 0.2 mL in the anterior chamber and 0.05 mL in the posterior chamber.[29] Aqueous humor is primarily produced by the non-pigmented epithelium of the ciliary processes at a rate of 2-3 μL per minute, with minor contributions from diffusion across iris vessels.[30] Its complete turnover occurs approximately every 100 minutes, ensuring dynamic renewal while nourishing avascular structures such as the lens and corneal endothelium, the latter of which relies on the humor for dehydration control via active pumping.[31] This circulation helps maintain normal intraocular pressure between 10 and 21 mmHg, essential for ocular health.[32]Physiology
Aqueous humor dynamics
Aqueous humor is primarily produced by the non-pigmented epithelium of the ciliary processes through active secretion, involving Na⁺/K⁺-ATPase pumps that drive solute transport across the epithelial barrier.[27] This process is supported by carbonic anhydrase, which facilitates bicarbonate (HCO₃⁻) formation essential for maintaining the osmotic gradient that draws water into the humor.[33] An ultrafiltration component also contributes passively, as plasma from ciliary body capillaries filters through the epithelial layers under hydrostatic pressure.[28] The ciliary body serves as the key site for this production, generating approximately 2 mL of aqueous humor daily in adults.[34] Once formed in the posterior chamber, aqueous humor circulates passively by diffusion through the pupil into the anterior chamber, where it nourishes avascular structures before draining.[27] This flow maintains optical clarity by preventing stagnation and ensuring nutrient delivery without direct vascular supply.[35] Drainage occurs via two main pathways to balance production and sustain intraocular pressure (IOP). The conventional pathway handles 80-90% of outflow, with humor passing through the trabecular meshwork—a sieve-like tissue in the anterior chamber angle—into Schlemm's canal, and then into episcleral veins.[27] The uveoscleral pathway accounts for the remaining 10-20%, involving bulk flow through the extracellular matrix of the ciliary muscle and supraciliary space toward the sclera and choroid.[36] Regulation of aqueous humor dynamics ensures IOP homeostasis, typically around 10-21 mmHg, through feedback mechanisms influenced by the autonomic nervous system; for instance, beta-adrenergic stimulation enhances production, while alpha-adrenergic activity suppresses it.[27] The relationship between production, outflow, and IOP is described by the Goldmann equation:where is the aqueous formation rate (μL/min), is the outflow facility (μL/min/mmHg), and EVP is episcleral venous pressure (mmHg).[37] With aging, outflow facility declines due to structural changes in the trabecular meshwork, reducing drainage efficiency and elevating glaucoma risk through sustained IOP increases.[38]