Recent from talks
Nothing was collected or created yet.
Permanent teeth
View on Wikipedia| Adult teeth | |
|---|---|
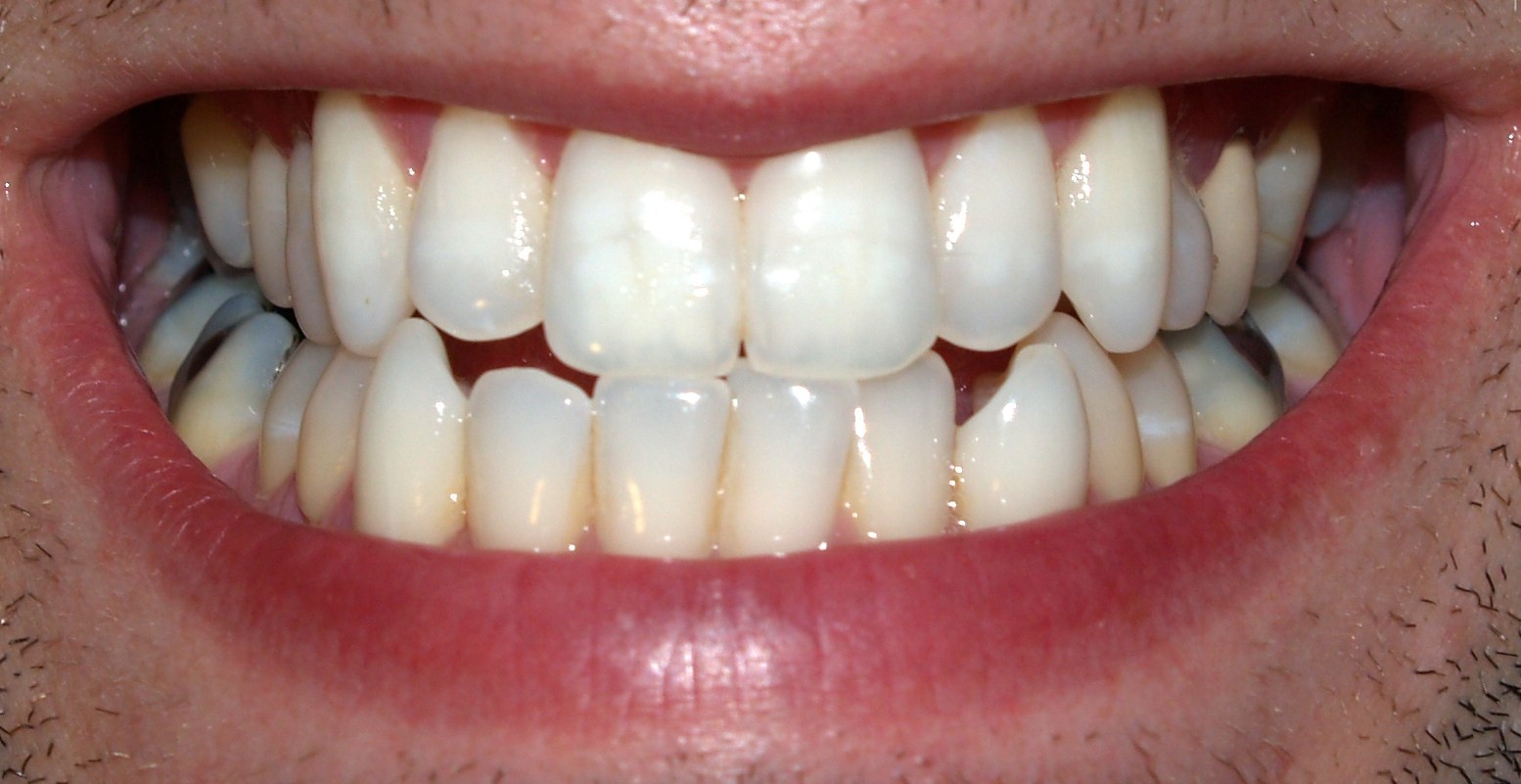
 Adult mouth showing full set of permanent teeth | |
| Details | |
| Identifiers | |
| Latin | dentes permanentes |
| TA98 | A05.1.03.077 |
| TA2 | 913 |
| FMA | 75152 |
| Anatomical terminology | |
Permanent teeth or adult teeth are the second set of teeth formed in diphyodont mammals. In humans and old world simians, there are thirty-two permanent teeth, consisting of six maxillary and six mandibular molars, four maxillary and four mandibular premolars, two maxillary and two mandibular canines, four maxillary and four mandibular incisors.[1]
Timeline
[edit]The first permanent tooth usually appears in the mouth at around 5-6 years of age, and the mouth will then be in a transition time with both primary (or deciduous dentition) teeth and permanent teeth during the mixed dentition period until the last primary tooth is lost or shed.[2]
The first of the permanent teeth to erupt are the permanent first molars, right behind the last 'milk' molars of the primary dentition. These first permanent molars are important for the correct development of a permanent dentition. Up to thirteen years of age, 28 of the 32 permanent teeth will appear.
The full permanent dentition is completed much later during the permanent dentition period.[3] The four last permanent teeth, the third molars, usually appear between the ages of 17 and 21 years; they are considered wisdom teeth.[4]
Pathology
[edit]It is possible to have extra, or "supernumerary", teeth. This phenomenon is called hyperdontia and is often erroneously referred to as "a third set of teeth." These teeth may erupt into the mouth or remain impacted in the bone. Hyperdontia is often associated with syndromes such as cleft lip and cleft palate, tricho-rhino-phalangeal syndrome, cleidocranial dysplasia, and Gardner's syndrome.[5]
See also
[edit]- Animal tooth development – Process by which teeth form and grow into the mouth
- Deciduous dentition – First set of teeth in diphyodonts
- Dentition – Development and arrangement of teeth
- Teething – Infants gaining their first teeth
- Tooth eruption – Process in tooth development
References
[edit]- ^ "Tooth eruption: The permanent teeth". American Dental Association. Archived from the original (PDF) on July 15, 2016.
- ^ "Permanent tooth eruption chart". American Dental Association.
- ^ Fehrenbach; Popowics (2026). lllustrated Dental Embryology, Histology, and Anatomy. Elsevier. pp. 217–219.
- ^ "Tooth eruption: The permanent teeth" (PDF). American Dental Association. Archived from the original (PDF) on June 27, 2012.
- ^ Jordan, Joseph A. Regezi & James J. Sciubba; Richard C. K. (2003). Oral pathology : clinical pathologic correlations (4th ed.). St. Louis: Saunders. ISBN 978-0721698052.
{{cite book}}: CS1 maint: multiple names: authors list (link)
- Ash, Major M. and Stanley J. Nelson, 2003. Wheeler’s Dental Anatomy, Physiology, and Occlusion. 8th edition.
![]() This article incorporates text in the public domain from the 20th edition of Gray's Anatomy (1918)
This article incorporates text in the public domain from the 20th edition of Gray's Anatomy (1918)
External links
[edit]Permanent teeth
View on GrokipediaAnatomy
Types and Arrangement
Permanent teeth in humans are classified into four main types based on their morphology and function: incisors, canines, premolars, and molars. There are 32 permanent teeth in a complete adult dentition, comprising 8 incisors (4 maxillary and 4 mandibular), 4 canines (2 maxillary and 2 mandibular), 8 premolars (4 maxillary and 4 mandibular), and 12 molars (6 maxillary and 6 mandibular, including 4 third molars or wisdom teeth).[1][4] These teeth are arranged in two dental arches: the maxillary (upper) arch and the mandibular (lower) arch, each divided into four quadrants—upper right, upper left, lower right, and lower left—for systematic organization. The universal numbering system, widely used in the United States, assigns numbers 1 through 32 to permanent teeth, beginning with the maxillary right third molar as tooth 1 and proceeding clockwise around the arches: teeth 1–8 in the upper right quadrant, 9–16 in the upper left, 17–24 in the lower left, and 25–32 in the lower right. This system facilitates precise identification in clinical and radiographic contexts.[5][6] Each tooth type is adapted for specific mechanical roles in food processing. Incisors, located at the anterior of each arch, feature thin, chisel-like edges for cutting and biting food into smaller pieces. Canines, positioned lateral to the incisors, have pointed cusps suited for tearing tougher foods. Premolars, situated between canines and molars, possess broader surfaces with two cusps each for crushing and initial grinding. Molars, at the posterior of the arches, have multiple cusps and large occlusal surfaces optimized for thorough grinding and pulverizing of food.[1][7] Variations in permanent dentition include agenesis, or congenital absence of teeth, and supernumerary teeth, or extra teeth beyond the normal complement. Agenesis is prevalent, affecting approximately 3–10% of the population excluding third molars, with third molars being absent in approximately 23% of individuals due to their distal position and evolutionary trends.[1][8] Supernumerary teeth occur rarely, with a prevalence of 1–3% in the permanent dentition, often as mesiodens (extra incisors) or supplemental forms in other regions. These anomalies can influence occlusion and require orthodontic or surgical intervention.[9]Microscopic Structure
The microscopic structure of permanent teeth consists of several distinct layers, each with unique histological and material properties that contribute to the tooth's durability and functionality. The outermost layer is enamel, a highly mineralized, acellular tissue primarily composed of hydroxyapatite crystals arranged in rod-like prisms with interrod spaces, providing a protective covering over the coronal dentin.[10] Beneath the enamel lies dentin, the bulk of the tooth, which forms a tubular matrix produced by odontoblasts and containing approximately 70% mineral content (hydroxyapatite), 20% organic material, and 10% water, with dentinal tubules housing odontoblastic processes that transmit sensory stimuli.[10] The innermost core is the dental pulp, a soft, vascularized connective tissue rich in fibroblasts, blood vessels, and nerves, divided into zones including an odontoblastic layer and a central core, which nourishes the surrounding dentin and provides sensory innervation.[10] Covering the root surface is cementum, a mineralized tissue akin to bone in composition, containing cementocytes within lacunae and Sharpey's fibers that integrate with the periodontal ligament; it anchors the tooth to the surrounding structures.[10] The periodontal ligament, a fibrous connective tissue composed mainly of type I collagen and fibroblasts, connects the cementum to the alveolar bone, facilitating tooth support, proprioception, and limited remodeling during orthodontic movement.[11] Permanent tooth roots exhibit varied morphologies depending on tooth type, with incisors and canines typically featuring a single root, while premolars often have one or two roots and molars possess two to three roots, each containing a root canal system that converges at the apical foramen—an opening at the root apex through which nerves and blood vessels enter to supply the pulp.[12] This apical foramen is usually singular per root but can vary, with configurations ranging from one to multiple foramina in some cases, ensuring vital tissue continuity.[12] In terms of material properties, enamel exhibits a Mohs hardness of approximately 5, making it the hardest substance in the human body and comparable to steel in durability, while dentin has a lower Mohs hardness of about 3, providing elasticity to absorb occlusal forces.[13] Enamel lacks regenerative capacity due to the absence of ameloblasts after tooth eruption, rendering it non-vital and irreparable once damaged, whereas dentin demonstrates limited regeneration through odontoblast-mediated formation of secondary dentin in response to irritation, though this process diminishes with age.[14] The vascular supply to permanent teeth derives from the superior and inferior alveolar arteries, branches of the maxillary artery, which enter via the apical foramen to perfuse the pulp and surrounding periodontium.[15] Innervation is provided by the superior alveolar nerves (from the maxillary division of the trigeminal nerve, CN V2) for maxillary teeth and the inferior alveolar nerve (from the mandibular division, CN V3) for mandibular teeth, forming dental plexuses that supply sensory fibers to the pulp, dentin, and periodontal ligament.[15]Development
Formation Process
The formation of permanent teeth, known as odontogenesis, is a complex process that begins during fetal development and continues postnatally, involving reciprocal interactions between epithelial and mesenchymal tissues derived from the oral ectoderm and neural crest cells, respectively.[16] This process establishes the 32 permanent teeth, which develop lingual to the primary tooth buds around the 20th week of gestation.[2] The dental lamina, formed at 6-7 weeks of gestation, gives rise to both primary and permanent tooth buds, but permanent tooth development initiates later with the bud stage at approximately 20 weeks, where epithelial swellings emerge; followed by the cap stage, marked by the formation of the enamel organ and early crown shaping; the bell stage, during which cells differentiate into ameloblasts (for enamel) and odontoblasts (for dentin); the apposition stage, involving calcification and matrix deposition, which begins at birth for the first permanent molars and continues postnatally for others; and the maturation stage, where roots complete formation after crown development, often extending into childhood.[16] These stages differ from primary tooth development, as permanent tooth buds form later and lingually to the primary ones, with calcification initiating at birth for first molars, 3-4 months for central incisors and mandibular lateral incisors, 4-5 months for canines, 10-12 months for maxillary lateral incisors, 1.5-2.5 years for premolars, and 2.5-3 years for second molars, allowing for a sequential replacement of the deciduous dentition.[17] Genetic and molecular factors play a critical role in regulating these stages through epithelial-mesenchymal interactions, where signaling pathways such as BMP, FGF, SHH, and WNT mediate induction and patterning.[16] Genes like PAX9 and MSX1, which encode transcription factors, are essential for tooth initiation and agenesis prevention; mutations in these genes lead to hypodontia or oligodontia, particularly affecting permanent molars and premolars.[18] For instance, PAX9 mutations disrupt posterior tooth formation by impairing mesenchymal condensation, while MSX1 influences early bud stage proliferation.[19] Environmental influences can modulate odontogenesis, particularly during calcification. Adequate nutrition, including vitamin D, supports enamel and dentin mineralization; deficiencies during gestation or early infancy may result in hypoplastic defects in permanent incisors and molars.[20] Similarly, fluoride exposure during the apposition and maturation stages enhances remineralization but excessive levels can cause dental fluorosis, mottling the enamel of developing permanent teeth.[21]Eruption Timeline
The eruption of permanent teeth follows a predictable sequence and timeline, beginning around age 6 and typically completing by the early 20s, though individual variations exist. The process starts with the first permanent molars, which emerge before the central incisors, followed by other incisors, premolars, and canines, with second and third molars appearing later; this order ensures proper alignment in the dental arch.[17] In the mandible, the sequence often begins with the first molars (6-7 years), central incisors (6-7 years), lateral incisors (7-8 years), first premolars (10-12 years), second premolars (11-12 years), canines (9-10 years), second molars (11-13 years), and third molars (17-21 years or later). The maxillary sequence is similar but slightly delayed: first molars (6-7 years), central incisors (7-8 years), lateral incisors (8-9 years), first premolars (10-11 years), second premolars (10-12 years), canines (11-12 years), second molars (12-13 years), and third molars (17-21 years or later).[22]| Tooth Type | Mandibular Eruption Age (years) | Maxillary Eruption Age (years) |
|---|---|---|
| First Molar | 6-7 | 6-7 |
| Central Incisor | 6-7 | 7-8 |
| Lateral Incisor | 7-8 | 8-9 |
| First Premolar | 10-12 | 10-11 |
| Canine | 9-10 | 11-12 |
| Second Premolar | 11-12 | 10-12 |
| Second Molar | 11-13 | 12-13 |
| Third Molar | 17-21 or later | 17-21 or later |