Recent from talks
Nothing was collected or created yet.
Seborrhoeic dermatitis
View on Wikipedia
| Seborrhoeic dermatitis | |
|---|---|
| Other names | Sebopsoriasis, seborrhoeic eczema, pityriasis capitis[1] |
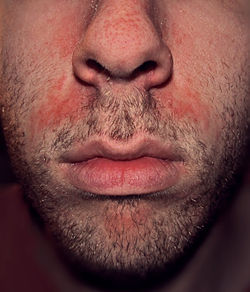 | |
| Seborrhoeic dermatitis of the face | |
| Specialty | Dermatology |
| Symptoms | Flaking, dry or greasy, red, itchy, and inflamed skin[2][3] |
| Duration | Several weeks to lifelong[4] |
| Causes | Multiple factors[4] |
| Risk factors | Stress, dry skin or excessive sebum, winter, poor immune function, Parkinson disease[4], genetics |
| Diagnostic method | Based on symptoms[4] |
| Differential diagnosis | Psoriasis, atopic dermatitis, tinea capitis, rosacea, systemic lupus erythematosus[4] |
| Treatment | Humidifier |
| Medication | Antifungal cream, anti-inflammatory agents, coal tar, phototherapy[3] |
| Frequency | ~5% (adults),[4] ~10% (babies)[5] |

Seborrhoeic dermatitis (also spelled seborrheic dermatitis in American English) is a long-term skin disorder.[4] Symptoms include flaky, scaly, greasy, and occasionally itchy and inflamed skin.[2][3] Areas of the skin rich in oil-producing glands are often affected including the scalp, face, and chest.[4] It can result in social or self-esteem problems.[4] In babies, when the scalp is primarily involved, it is called cradle cap.[2] Mild seborrhoeic dermatitis of the scalp may be described in lay terms as dandruff due to the dry, flaky character of the skin.[6] However, as dandruff may refer to any dryness or scaling of the scalp, not all dandruff is seborrhoeic dermatitis.[6] Seborrhoeic dermatitis is sometimes inaccurately referred to as seborrhoea.[4]
The cause is unclear but believed to involve a number of genetic and environmental factors.[2][4] Risk factors for seborrhoeic dermatitis include poor immune function, Parkinson's disease, and alcoholic pancreatitis.[4][6] The condition may worsen with stress or during the winter.[4] Malassezia yeast is believed to play a role.[6] It is not a result of poor hygiene.[7] Diagnosis is typically clinical and based on the symptoms present.[4][8] The condition is not contagious.[9]
The typical treatment is topical antifungal cream and anti-inflammatory agents.[3] Specifically, ketoconazole or ciclopirox are effective.[10] Seborrhoeic dermatitis of the scalp is often treated with shampoo preparations of ketoconazole, zinc pyrithione, and selenium.[11]
The condition is common in infants within the first three months of age or adults aged 30 to 70 years.[2][4][5] It tends to affect more males.[12] Seborrhoeic dermatitis is more common in African Americans, among immune-compromised individuals, such as those with HIV, and individuals with Parkinson's disease.[11][12]
Signs and symptoms
[edit]



Seborrhoeic dermatitis typically appears as oily, yellowish, flaky skin. Although commonly associated with oily skin, it can also appear on dry scalps or skin, where the flaking may look similar to dandruff. The flakes can be fine, loose, and diffuse or thick and adherent.[11][8] In addition to flaky skin, seborrhoeic dermatitis can have areas of red, rashy, inflamed, and itchy skin that coincide with the area of skin flaking, but not all individuals have this symptom.[8]
Seborrhoeic dermatitis of the scalp can appear similarly to dandruff.[11] When the scalp is affected, there can be associated temporary hair loss.[11] Such hair loss varies in appearance from diffuse thinning to patchy areas of hair loss.[11] On close inspection, the locations where hair has thinned may have broken stubs of hair and pustules around the hair follicles.[11] Individuals with more pigmented skin tones may experience increased or decreased skin pigmentation in affected areas.[12]
Various locations can be affected by seborrhoeic dermatitis. Commonly affected areas include the face, ears, scalp, and across the body. It is less common in intertriginous areas, which are areas where the skin folds and comes into contact with itself, such as the groin or the underarms.[11]
Seborrhoeic dermatitis' symptoms are typically mild and appear gradually but are often persistent, lasting weeks to years.[8][11][13] Individuals with seborrhoeic dermatitis are subject to recurrent bouts and it may be a lifelong condition.[8] Seborrhoeic dermatitis can also occur quickly and severely in patients with Human Immunodeficiency Virus (HIV). This is sometimes the first indication of HIV.[12]
Causes
[edit]The cause of seborrhoeic dermatitis has not been fully clarified as of 2019.[14][15]
In addition to the presence of Malassezia, genetic, environmental, hormonal, and immune-system factors are necessary for and/or modulate the expression of seborrhoeic dermatitis.[16][17] The condition may be aggravated by illness, psychological stress, fatigue, sleep deprivation, change of season, and reduced general health.[18]
Fungi
[edit]The condition is thought to be due to a local inflammatory response to overgrowth by Malassezia fungi species in sebum-producing skin areas including the scalp, face, chest, back, underarms, and groin.[3][15] This is based on observations of high counts of Malassezia species in skin affected by seborrhoeic dermatitis and on the effectiveness of antifungals in treating the condition.[15] Species of Malassezia implicated in Seborrhoeic dermatitis include M. furfur (formerly Pityrosporum ovale), M. globosa, M. restricta, M. sympodialis, and M. slooffiae.[3]
Malassezia appears to be a significant factor in seborrhoeic dermatitis, but it is thought that other factors are necessary for the presence of Malassezia to result in seborrhoeic dermatitis.[15] For example, summer growth of Malassezia in the skin alone does not result in seborrhoeic dermatitis.[15] Besides antifungals, the effectiveness of anti-inflammatory drugs, which reduce inflammation, and antiandrogens, which reduce sebum production, provide further insights into the pathophysiology of seborrhoeic dermatitis.[3][19][20]
Bacteria
[edit]Several bacteria, including Propionibacterium species and Staphylococcus aureus, have been shown to have some level of interaction with seborrhoeic dermatitis, though their exact impact is not known.[21][12]
Nutrition
[edit]Seborrhoeic dermatitis-like eruptions are also associated with pyridoxine (vitamin B6) and riboflavin (vitamin B2) deficiency.[22][8] In children and babies, issues with Δ6-desaturase enzymes[18] have been correlated with increased risk.
Immune dysfunction
[edit]Those with immunodeficiency (especially infection with HIV) and with neurological disorders that may impact immune system function such as Parkinson's disease (for which the condition is an autonomic sign) and stroke are particularly prone to it.[23][unreliable medical source?]
Climate
[edit]Climate can affect seborrheic dermatitis, but there is a lack of consensus about which climates tend to exacerbate seborrheic dermatitis the most. Some studies show low humidity and low temperature are responsible for the high frequency of seborrheic dermatitis.[24] Others suggest hot environments may also worsen seborrhoeic dermatitis.[12] Yet another described that high humidity and low UV exposure are culpable.[25] Dry skin and an impaired skin barrier contribute to the condition.[12][21] It is likely that climate and weather variations affect the water and lipid content of skin.[21]
Mechanism
[edit]Seborrhoeic dermatitis is a complex condition with many interacting factors that are not yet fully explained.[15] In general, the major factors that influence the development and severity include Malassezia yeast present on and in the skin, skin production of oily sebum, and a subsequent inflammatory response against Malassezia and their byproducts.[12] Additional factors involved in the condition are a compromised skin barrier, the makeup and amount of sebum produced, the character of the immune response and inflammation, and the presence of other microbe species inhabiting the skin.[15][12]
A suggested series of events leading to seborrhoeic dermatitis is an initially damaged skin barrier and abnormal sebum production, which leads to a change in the microbiome of the skin that in turn elicits an immune response.[15] An alternative explanation is an increase in sebum production feeding an increase in the Malassezia population that instigates inflammation; the inflammation then causes cellular changes that damage the skin barrier. This barrier disruption then encourages additional Malassezia growth and inflammation and again worsens skin barrier function.[12]
Diagnosis
[edit]Typically, seborrhoeic dermatitis is a clinical diagnosis based on a physician's expertise in identifying and differentiating skin conditions based on the history of the individual and the appearance of the skin.[8] However, seborrhoeic dermatitis may also be diagnosed with additional testing. The least invasive test is a visual inspection in the clinic using a Wood's Lamp.[11] A KOH test can also be used, where skin scraping of the affected skin may also be taken and prepared with potassium hydroxide (KOH) and visualized under a microscope to look for Malassezia or other microbiological cells. Additionally, a fungal culture of the affected skin may be taken to attempt to grow and identify the causative organism.[11]
Differential diagnosis
[edit]Seborrhoeic dermatitis can look similar to other skin conditions that share its characteristic dry, flaky, scaly, and inflamed appearance, but have different causes and treatments. Physicians use the history of the individual with the skin condition as well as other tests to identify which disorder is present. Other conditions that may be confused with seborrhoeic dermatitis based on appearance are listed below.[8][11]
Management
[edit]Medications
[edit]A variety of different types of medications can reduce symptoms of seborrhoeic dermatitis.[3] These include certain antifungals, anti-inflammatory agents like corticosteroids and nonsteroidal anti-inflammatory drugs, antiandrogens, and antihistamines, among others.[3][14] Treatments must take into consideration potential side effects, especially with long-term use given the chronic nature of seborrhoeic dermatitis.[neutrality is disputed] Initial therapy is usually a topical preparation with an agreeable side effect profile.[12]
Antifungals
[edit]Regular use of an over-the-counter or prescription antifungal shampoo or cream is a common treatment. The topical antifungal medications ketoconazole and ciclopirox have the best evidence.[10] Ketoconazole should be used twice per week.[8] Shampoo or soap containing zinc pyrithione or selenium disulfide is also used.[8] These options should be used daily but may also be used in conjunction with a ketoconazole shampoo regimen on alternate days.[8] It is unclear if other antifungals are equally effective, as this has not been sufficiently studied.[10] Antifungals that have been studied and found to be effective in the treatment of seborrhoeic dermatitis include ketoconazole, fluconazole, miconazole, bifonazole, sertaconazole, clotrimazole, flutrimazole, ciclopirox, terbinafine, butenafine, selenium disulfide, and lithium salts such as lithium gluconate and lithium succinate.[10][3]
Topical climbazole appears to have little effectiveness in the treatment of seborrhoeic dermatitis.[10] Systemic therapy with oral antifungals including itraconazole, fluconazole, ketoconazole is effective, but adverse side effects have been documented for fluconazole and ketoconazole, with the latter not recommended for use, while itraconazole, with its good safety profile, is the most commonly prescribed.[3] Terbinafine is said to be effective, but with adverse side effects, while other sources state it is not effective and should not be used.[3][11]
Anti-inflammatory treatments
[edit]Topical corticosteroids are effective in short-term treatment of seborrhoeic dermatitis and are as effective or more effective than antifungal treatment with azoles. These are sometimes used for only a few weeks at a time.[11][additional citation(s) needed] There is also evidence for the effectiveness of topical calcineurin inhibitors like tacrolimus and pimecrolimus as well as lithium salt therapy.[26] Calcineurin inhibitors were also effective in reducing the growth of Malassezia, offering two routes by which they may treat seborrhoeic dermatitis.[25] Medications such as calcineurin inhibitors should not be used in individuals with seborrhoeic dermatitis who are immune-compromised because they cause further immune suppression.[11]
Oral immunosuppressive treatment, such as with prednisone, has been used in short courses for seborrhoeic dermatitis, as a last resort due to its potential side effects.[27]
Antihistamines
[edit]Antihistamines are used primarily to reduce itching, if present. However, research studies suggest that some antihistamines have anti-inflammatory properties.[28]
Keratolytics
[edit]Keratolytics help the skin via exfoliation of built-up skin flakes and thereby remove scale. They are applied topically to the affected area. Keratolytics include urea, salicylic acid, coal tar, lactic acid, pyrithione zinc and propylene glycol.[25] Coal tar shampoo formulations can be effective.[8][25] Although no significant increased risk of cancer in human treatment with coal tar shampoos have been found, caution is advised since coal tar is carcinogenic in animals, and heavy human occupational exposures do increase cancer risks.[29]
Other treatments
[edit]- Isotretinoin, a sebosuppressive agent, may be used to reduce sebaceous gland activity as a last resort in refractory disease.[30] However, isotretinoin has potentially serious side effects, and few patients with seborrhoeic dermatitis are appropriate candidates for therapy.[27]
- Topical 0.75% and 1% Metronidazole[10][11]
- Topical 4% nicotinamide[3]
- Topical sulfacetamide[11]
- Tea tree oil[12]
- Cannabidiol shampoo[25]
- Frequent washing to avoid the build-up of scale, especially on the scalp, but while avoiding overly drying the skin[12][11][21]
- Avoiding damaging skin with harsh grooming or chemical irritants[21]
- Bicalutamide, an antiandrogen, has been observed in one patient to have potentially been the cause of seborrheic dermatitis relief. However, even if it were demonstrated that bicalutamide or any other antiandrogen is a treatment, it is not recommended due to side effects and price.[31]
Phototherapy
[edit]Another option is natural and artificial UV radiation since it can inhibit the growth of Malassezia yeast.[32] Some recommend photodynamic therapy using UV-A and UV-B laser or red and blue LED light to inhibit the growth of Malassezia fungus and reduce seborrhoeic inflammation.[32][33][34]
Outcome
[edit]Seborrhoeic dermatitis is generally a chronic and recurring condition. Individuals may have the condition for several weeks to months, but it may also last years or their lifetime. There may be periods of relapse and worsening.[11][8]
Epidemiology
[edit]Seborrhoeic dermatitis affects 1 to 5% of the general population.[14][35][36] It is slightly more common in men, but affected women tend to have more severe symptoms.[36] The condition usually recurs throughout a person's lifetime.[37] Seborrhoeic dermatitis can occur in any age group[37] but often occurs during the first three months of life then again at puberty and peaks in incidence at around 40 years of age.[38][21] It can reportedly affect as many as 31% of older people.[36] Infants may also have this condition, though it is typically milder, and is referred to as cradle cap.[12] Seborrhoeic dermatitis is more common in African-Americans.[12]
Severity is worse in dry climates[37] as well as hot weather, as dry skin can exacerbate the condition.[12] COVID-19 related mask usage may also cause or exacerbate facial seborrhoeic dermatitis.[12]
Individuals who are immunocompromised have an increased risk of seborrhoeic dermatitis.[12] Conditions that are associated with increased rates of seborrhoeic dermatitis include individuals with HIV, Hepatitis C, alcoholic pancreatitis, Parkinson's disease, and alcohol abuse.[12] Seborrhoeic dermatitis is common in people with alcoholism, between 7 and 11 percent, which is twice the normal expected occurrence.[39]
References
[edit]- ^ Cite error: The named reference
Des201ca3was invoked but never defined (see the help page). - ^ a b c d e "Seborrheic Dermatitis - Dermatologic Disorders". Merck Manuals Professional Edition. Archived from the original on 26 January 2020. Retrieved 22 November 2019.
- ^ a b c d e f g h i j k l m Borda LJ, Perper M, Keri JE (March 2019). "Treatment of seborrheic dermatitis: a comprehensive review". The Journal of Dermatological Treatment. 30 (2): 158–169. doi:10.1080/09546634.2018.1473554. PMID 29737895. S2CID 13686180.
- ^ a b c d e f g h i j k l m n o Ijaz N, Fitzgerald D (June 2017). "Seborrhoeic dermatitis". British Journal of Hospital Medicine. 78 (6): C88 – C91. doi:10.12968/hmed.2017.78.6.C88. PMID 28614013.
- ^ a b Nobles T, Harberger S, Krishnamurthy K (August 2021). "Cradle Cap". StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. PMID 30285358. Archived from the original on 21 January 2021. Retrieved 26 February 2022.
- ^ a b c d Naldi L, Diphoorn J (May 2015). "Seborrhoeic dermatitis of the scalp". BMJ Clinical Evidence. 2015. PMC 4445675. PMID 26016669.
- ^ "Seborrheic dermatitis". American Academy of Dermatology. Archived from the original on 21 October 2017. Retrieved 20 October 2017.
- ^ a b c d e f g h i j k l m n o p q Papadakis MA, McPhee SJ (2023). "Dermatitis, Seborrheic". Quick Medical Diagnosis & Treatment 2023 (2023 ed.). McGraw-Hill Education. ISBN 978-1-264-68734-3.
- ^ "Seborrheic Dermatitis: What is It, Diagnosis & Treatment". Cleveland, Ohio: Cleveland Clinic. Archived from the original on 17 October 2021. Retrieved 12 October 2021.
- ^ a b c d e f Okokon EO, Verbeek JH, Ruotsalainen JH, Ojo OA, Bakhoya VN (May 2015). Okokon EO (ed.). "Topical antifungals for seborrhoeic dermatitis". The Cochrane Database of Systematic Reviews. 4 (5) CD008138. doi:10.1002/14651858.CD008138.pub3. PMC 4448221. PMID 25933684.
- ^ a b c d e f g h i j k l m n o p q r s t u v Dinulos JG (2021). Habif's Clinical Dermatology, Seventh Edition (7th ed.). Elsevier Inc. ISBN 978-0-323-61269-2.
- ^ a b c d e f g h i j k l m n o p q r s t u v Jackson JM, Alexis A, Zirwas M, Taylor S (December 2022). "Unmet needs for patients with seborrheic dermatitis". Journal of the American Academy of Dermatology. 90 (3): S0190–9622(22)03307–2. doi:10.1016/j.jaad.2022.12.017. PMID 36538948. S2CID 254843412.
- ^ "Dermatitis". Archived from the original on 25 September 2011. Retrieved 11 June 2010.
- ^ a b c Dessinioti C, Katsambas A (July–August 2013). "Seborrheic dermatitis: etiology, risk factors, and treatments: facts and controversies". Clinics in Dermatology. 31 (4): 343–351. doi:10.1016/j.clindermatol.2013.01.001. PMID 23806151.
- ^ a b c d e f g h Wikramanayake TC, Borda LJ, Miteva M, Paus R (September 2019). "Seborrheic dermatitis-Looking beyond Malassezia". Experimental Dermatology. 28 (9): 991–1001. doi:10.1111/exd.14006. PMID 31310695.
- ^ Johnson BA, Nunley JR (May 2000). "Treatment of seborrheic dermatitis". American Family Physician. 61 (9): 2703–10, 2713–4. PMID 10821151. Archived from the original on 6 July 2010.
- ^ Janniger CK, Schwartz RA (July 1995). "Seborrheic dermatitis". American Family Physician. 52 (1): 149–55, 159–60. PMID 7604759.
- ^ a b Schwartz RA, Janusz CA, Janniger CK (July 2006). "Seborrheic dermatitis: an overview". American Family Physician. 74 (1): 125–130. PMID 16848386. Archived from the original on 26 January 2020. Retrieved 15 April 2010.
- ^ Trivedi MK, Shinkai K, Murase JE (March 2017). "A Review of hormone-based therapies to treat adult acne vulgaris in women". International Journal of Women's Dermatology. 3 (1): 44–52. doi:10.1016/j.ijwd.2017.02.018. PMC 5419026. PMID 28492054.
- ^ Paradisi R, Fabbri R, Porcu E, Battaglia C, Seracchioli R, Venturoli S (October 2011). "Retrospective, observational study on the effects and tolerability of flutamide in a large population of patients with acne and seborrhea over a 15-year period". Gynecological Endocrinology. 27 (10): 823–829. doi:10.3109/09513590.2010.526664. PMID 21117864. S2CID 20250916.
- ^ a b c d e f Mangion SE, Mackenzie L, Roberts MS, Holmes AM (April 2023). "Seborrheic dermatitis: topical therapeutics and formulation design". European Journal of Pharmaceutics and Biopharmaceutics. 185: 148–164. doi:10.1016/j.ejpb.2023.01.023. PMID 36842718. S2CID 257214910.
- ^ Alamgir AN (2018). Therapeutic Use of Medicinal Plants and their Extracts: Volume 2: Phytochemistry and Bioactive Compounds. Springer. p. 435. ISBN 978-3-319-92387-1.
- ^ "Seborrhoeic dermatitis and dandruff (seborrheic eczema). DermNet NZ". . DermNet NZ. 20 March 2012. Archived from the original on 15 June 2012. Retrieved 10 June 2012.
- ^ Araya M, Kulthanan K, Jiamton S (September 2015). "Clinical Characteristics and Quality of Life of Seborrheic Dermatitis Patients in a Tropical Country". Indian Journal of Dermatology. 60 (5): 519. doi:10.4103/0019-5154.164410. PMC 4601435. PMID 26538714.
- ^ a b c d e Leroy AK, Cortez de Almeida RF, Obadia DL, Frattini S, Melo DF (June 2023). "Scalp Seborrheic Dermatitis: What We Know So Far". Skin Appendage Disorders. 9 (3): 160–164. doi:10.1159/000529854. PMC 10264915. PMID 37325288.
- ^ Kastarinen H, Oksanen T, Okokon EO, Kiviniemi VV, Airola K, Jyrkkä J, et al. (May 2014). "Topical anti-inflammatory agents for seborrhoeic dermatitis of the face or scalp". The Cochrane Database of Systematic Reviews. 2017 (5) CD009446. doi:10.1002/14651858.CD009446.pub2. PMC 6483543. PMID 24838779.
- ^ a b Gupta AK, Richardson M, Paquet M (January 2014). "Systematic review of oral treatments for seborrheic dermatitis". Journal of the European Academy of Dermatology and Venereology. 28 (1): 16–26. doi:10.1111/jdv.12197. PMID 23802806. S2CID 25441626.
- ^ Grob JJ, Castelain M, Richard MA, Bonniol JP, Béraud V, Adhoute H, et al. (May 1998). "Antiinflammatory properties of cetirizine in a human contact dermatitis model. Clinical evaluation of patch tests is not hampered by antihistamines". Acta Dermato-Venereologica. 78 (3): 194–197. doi:10.1080/000155598441512. PMID 9602225.
- ^ Roelofzen JH, Aben KK, Oldenhof UT, Coenraads PJ, Alkemade HA, van de Kerkhof PC, et al. (April 2010). "No increased risk of cancer after coal tar treatment in patients with psoriasis or eczema". The Journal of Investigative Dermatology. 130 (4): 953–961. doi:10.1038/jid.2009.389. PMID 20016499.
- ^ de Souza Leão Kamamoto C, Sanudo A, Hassun KM, Bagatin E (January 2017). "Low-dose oral isotretinoin for moderate to severe seborrhea and seborrheic dermatitis: a randomized comparative trial". International Journal of Dermatology. 56 (1): 80–85. doi:10.1111/ijd.13408. PMID 27778328. S2CID 13049459.
- ^ Rebora A. "Bicalutamide: A Novel Treatment of Seborrheic Dermatitis?" (PDF). Scientific Research and Community - Open Access Journals. Journal of Dermatology Research. Retrieved 8 June 2024.
- ^ a b Wikler JR, Janssen N, Bruynzeel DP, Nieboer C (1990). "The effect of UV-light on pityrosporum yeasts: ultrastructural changes and inhibition of growth". Acta Dermato-Venereologica. 70 (1): 69–71. PMID 1967880.
- ^ Calzavara-Pinton PG, Venturini M, Sala R (January 2005). "A comprehensive overview of photodynamic therapy in the treatment of superficial fungal infections of the skin". Journal of Photochemistry and Photobiology B: Biology. 78 (1): 1–6. Bibcode:2005JPPB...78....1C. doi:10.1016/j.jphotobiol.2004.06.006. PMID 15629243.
- ^ Maisch T, Szeimies RM, Jori G, Abels C (October 2004). "Antibacterial photodynamic therapy in dermatology". Photochemical & Photobiological Sciences. 3 (10). rsc.org: 907–917. Bibcode:2004PhPhS...3..907M. doi:10.1039/B407622B. PMID 15480480. S2CID 32215045.
- ^ Goldstein MA, Goldstein MC, Credit LP (17 March 2009). Your Best Medicine: From Conventional and Complementary Medicine--Expert-Endorsed Therapeutic Solutions to Relieve Symptoms and Speed Healing. Rodale. pp. 462–. ISBN 978-1-60529-656-2. Archived from the original on 5 November 2017.
- ^ a b c Farage MA, Miller KW, Maibach HI (2 December 2009). Textbook of Aging Skin. Springer Science & Business Media. pp. 534–. ISBN 978-3-540-89655-5. Archived from the original on 5 November 2017.
- ^ a b c Jacknin J (2001). Smart Medicine for Your Skin: A Comprehensive Guide to Understanding Conventional and Alternative Therapies to Heal Common Skin Problems. Penguin. pp. 271–. ISBN 978-1-58333-098-2. Archived from the original on 5 November 2017.
- ^ Ooi ET, Tidman MJ (February 2014). "Improving the management of seborrhoeic dermatitis". The Practitioner. 258 (1768): 23–6, 3. PMID 24689165.
- ^ Kostović K, Lipozencić J (2004). "Skin diseases in alcoholics". Acta Dermatovenerologica Croatica. 12 (3): 181–190. PMID 15369644.
External links
[edit]![]() Media related to Seborrhoeic dermatitis at Wikimedia Commons
Media related to Seborrhoeic dermatitis at Wikimedia Commons
Seborrhoeic dermatitis
View on GrokipediaSymptoms
Symptoms typically include persistent flaking and scaling of the skin, with oily or greasy patches that may appear pink or red on lighter skin tones and purple, pink, or darker on brown or Black skin.[4] Common sites include the scalp (leading to dandruff), eyebrows, beard area, ears, nose creases, and chest, often accompanied by mild to intense itching or soreness.[3] In infants, it presents as thick, crusty scales on the scalp known as cradle cap, which usually resolves without treatment by age one.[1] Severe cases may involve widespread involvement or secondary infections due to scratching.[6]Causes and Risk Factors
The exact etiology remains unclear but involves an interplay of Malassezia yeast overgrowth on the skin, sebum production, and an abnormal immune response, rather than direct infection or allergy.[1] Genetic predisposition, epidermal barrier dysfunction, and microbial dysbiosis contribute to its pathophysiology, with no single cause identified.[1] Risk factors include neurological conditions like Parkinson's disease, immune suppression such as in HIV (where prevalence can reach 35-85%), recovery from stressful illnesses like heart attacks, and certain demographics including men, individuals over 50, and those with oily skin or other dermatoses like psoriasis.[3] Environmental triggers such as cold, dry weather or fatigue can exacerbate flares.[4]Diagnosis and Management
Diagnosis is primarily clinical, based on the characteristic distribution and appearance of lesions, though biopsy may be used to rule out similar conditions like psoriasis or eczema.[1] There is no cure, but management focuses on symptom control through topical antifungals (e.g., ketoconazole shampoo), mild corticosteroids, or calcineurin inhibitors to reduce inflammation and yeast proliferation.[7] For severe or refractory cases, oral antifungals or phototherapy may be considered, with regular maintenance therapy preventing recurrences.[1] Early intervention by a dermatologist can significantly improve quality of life, as the condition is benign but can be persistent and cosmetically distressing.[4]Signs and symptoms
Presentation in adults
Seborrheic dermatitis in adults typically presents as red, inflamed skin with greasy, yellowish scales or plaques that primarily affect seborrheic areas rich in sebaceous glands.[3][1] Common sites include the scalp, where it manifests as dandruff-like flaking; the face, particularly the nasolabial folds, eyebrows, eyelids, sides of the nose, forehead, and central face; the beard and mustache areas in men; the ears and postauricular regions; and the upper trunk, such as the chest and back.[6][3] In more extensive cases, involvement may extend to the armpits, groin, or under the breasts.[6] The skin lesions appear as erythematous to salmon-colored papules and plaques covered with fine, powdery scales or greasy yellowish crusts that adhere to oily skin, often described as yellowish or white in lighter skin tones, while in individuals with darker skin, they may present as pinkish, purplish, hypopigmented, or darker areas with less noticeable redness. Particularly on the face, including the forehead and areas around the nose, small raised papules or bumps may occur, which can appear small, red, salmon-colored, yellow-crusted, or darker depending on skin tone and inflammation level, reflecting the condition's papulosquamous morphology.[1][6] Patients commonly experience mild to moderate itching or a burning sensation, which can be more intense on the scalp and may lead to scratching that exacerbates flaking.[6][8] In severe scalp involvement, temporary hair shedding can occur due to inflammation-induced telogen effluvium, though it is reversible with treatment.[9] Severity varies widely, from mild forms limited to flaky scalp scaling (often indistinguishable from dandruff) to moderate presentations with thin plaques and pruritus, or severe cases featuring extensive erythematous plaques, oozing or crusting in skin folds like the ears, and significant discomfort that disrupts daily activities.[6][3] Dandruff represents the mildest variant, confined to the scalp without facial or body involvement, whereas full seborrheic dermatitis extends beyond this with more inflammatory features.[6] The condition may be more prevalent or severe in adults with underlying disorders such as Parkinson's disease or HIV infection.[8] The recurrent flaky scalp in seborrheic dermatitis, often perceived as "dry scalp" or dandruff, results from overgrowth of Malassezia yeast, excess sebum production, and an immune response leading to inflammation and accelerated epidermal turnover with flaking. The condition characteristically comes and goes, with flares triggered by stress, cold or dry weather, hormonal changes, illness, fatigue, or seasonal factors. This distinguishes it from pure dry scalp (xerosis) due to low humidity or harsh hair products, which may recur seasonally but is less likely to be chronically recurrent without persistent triggers.[3][1]Presentation in infants and children
Seborrhoeic dermatitis in infants, commonly known as cradle cap, typically manifests as thick, yellowish, greasy scales or crusts on the scalp, particularly affecting the vertex and frontal regions. These scales are often adherent and may form a firm, bran-like covering that binds the hair, but the condition is generally asymptomatic, with no associated itching or pain in most cases.[1] The lesions can extend beyond the scalp to involve the forehead, eyebrows, postauricular areas, ears, and occasionally the neck or face in a T-shaped distribution along the nasolabial folds.[10] Onset usually occurs between the second and third week of life, peaking in prevalence around 3 months of age, and the condition is self-limiting, resolving spontaneously in the majority of infants by 8 to 12 months without scarring or complications.[11] In rare instances, infantile seborrhoeic dermatitis may present with involvement of intertriginous areas, such as the diaper region, axillae, or navel, where erythematous plaques with finer scaling predominate over thick crusts, sometimes leading to confusion with irritant diaper dermatitis.[1] The disseminated form can affect the trunk or extremities minimally, but scalp involvement remains the hallmark. Four clinical subtypes have been described in infants: cephalic (limited to scalp), facial, diaper-type (genital and perineal), and disseminated, though the cephalic variant, or cradle cap, is by far the most common.[11] Despite its greasy appearance, the scales are non-inflammatory and do not typically cause discomfort to the infant, though they may provoke parental concern due to cosmetic issues.[10] In older children beyond infancy, seborrhoeic dermatitis tends to be milder and less prevalent, affecting approximately 7% in the second year of life and becoming rare after age 4. Presentation often mirrors a subtler version of the adult form, featuring fine, powdery scaling or flaking on the scalp, eyebrows, or behind the ears, with occasional mild erythema or subtle itching that rarely disrupts daily activities.[10] Facial involvement may include the nasolabial folds or glabella, but widespread or severe scaling is uncommon, and the condition remains self-resolving in most pediatric cases without progression to chronicity.[1] Persistent symptoms beyond 12 months warrant evaluation to exclude alternative diagnoses, as true seborrhoeic dermatitis in this age group is typically transient and tied to the maturation of sebaceous glands.[11]Diagnosis
Clinical diagnosis
The diagnosis of seborrhoeic dermatitis is primarily clinical, relying on a thorough visual examination of the skin and a detailed patient history, without the need for laboratory tests in typical cases.[1][12] Clinicians identify characteristic lesions as erythematous patches or plaques covered with greasy, yellowish scales, often presenting in areas rich in sebaceous glands such as the scalp, face (including nasolabial folds and eyebrows), ears, and upper trunk.[13][14] These findings are corroborated by a history of chronic, relapsing symptoms that align with common presentations like flaky scalp or facial scaling, typically occurring in otherwise healthy individuals without systemic involvement.[15][1] Specific laboratory investigations, such as skin scrapings for fungal culture or skin biopsy, are rarely required and are reserved for atypical presentations where other conditions must be excluded.[12][13] If a fungal etiology is suspected due to unusual features, adjunctive tools like dermoscopy may be employed to assess for dotted vessels or fine scaling patterns that support the diagnosis, while a Wood's lamp can help rule out fluorescence indicative of other dermatoses.[12] Key diagnostic criteria include the symmetrical distribution of lesions in sebaceous gland-dense regions and the absence of systemic symptoms, such as fever or lymphadenopathy, which further affirm the clinical impression.[1][15] This approach ensures accurate identification based on the disease's hallmark localization and morphology.[13]Differential diagnosis
Seborrhoeic dermatitis must be differentiated from other conditions that can present with recurrent flaky scalp, scaling, erythema, or pruritus in seborrhoeic areas such as the scalp, face, and upper trunk.[1] Distinguishing features include the distribution in oil-rich areas, greasy yellow scales, and mild pruritus, contrasting with more inflammatory or infectious mimics.[13] Psoriasis typically features sharply demarcated erythematous plaques with thick, silvery-white scales, often involving the nails with pitting and lacking the greasy quality of seborrhoeic scales; it commonly affects extensor surfaces beyond seborrhoeic regions and can cause recurrent flaky scalp.[16][1] In contrast to seborrhoeic dermatitis, psoriatic lesions show a positive Auspitz sign upon scale removal.[15] Atopic dermatitis presents with more intense pruritus, dry and lichenified patches rather than oily scales, and a predilection for flexural areas like the antecubital and popliteal fossae, often with a personal or family history of atopy.[13][16] Unlike seborrhoeic dermatitis, it may involve weeping or crusting and spares the typical seborrhoeic distribution in many cases.[1] Tinea capitis, a fungal infection, is characterized by patchy alopecia, scaling with broken "black dot" hairs, and a scaly, elevated leading edge; diagnosis is confirmed by positive potassium hydroxide (KOH) preparation or fungal culture showing dermatophytes.[13][15] It differs from seborrhoeic dermatitis by its association with hair loss and lack of diffuse greasy scaling, being more common in children than adults.[1] Contact dermatitis often has an acute onset linked to exposure to irritants or allergens, such as shampoos or hair dyes, resulting in localized vesicular or eczematous reactions that resolve upon avoidance; it typically follows the pattern of contact rather than seborrhoeic areas and can cause recurrent flaky scalp if exposure is repeated.[16][1] Eyelid involvement or sharp demarcation from exposure sites further distinguishes it from the more chronic, symmetric distribution of seborrhoeic dermatitis.[15] Simple dry scalp (xerosis) is characterized by fine, dry, white flakes on the scalp, often due to low humidity, harsh hair products, or excessive washing. It is non-inflammatory, lacking the erythema, greasy scales, and significant pruritus of seborrheic dermatitis. The flaking can recur seasonally with dry weather or due to triggers like harsh products, but is less likely to be chronically recurrent without persistent triggers. It differs from seborrheic dermatitis by the absence of inflammation and greasy quality, and usually improves with moisturizing and gentle hair care.[17][18] Rosacea manifests as central facial erythema, telangiectasias, and papules or pustules without significant scaling or scalp involvement, often accompanied by flushing or ocular symptoms like meibomianitis.[13][16] Acne, similarly, features comedones, inflammatory papules, and pustules primarily on the face, chest, or back, lacking the diffuse greasy crusts and seborrhoeic distribution seen in seborrhoeic dermatitis.[1][15]Etiology
Microbial causes
Seborrhoeic dermatitis is closely linked to the genus Malassezia, a group of lipophilic yeasts that form part of the normal cutaneous microbiome and preferentially colonize sebaceous gland-rich areas such as the scalp, face, and upper trunk.[19] Among the 18 identified Malassezia species, M. globosa and M. restricta are the most frequently implicated in the condition, comprising the majority of isolates from lesional skin.[19] These yeasts thrive in lipid-rich environments, with overgrowth often triggered by increased sebum production during puberty or other physiological changes that alter sebum composition, such as elevated levels of triglycerides and cholesterol alongside reduced squalene and free fatty acids.[19] Malassezia species produce lipases that metabolize sebum lipids into irritant free fatty acids, such as oleic acid, which can disrupt the skin barrier and contribute to the initiation of dermatitis.[19] Studies have demonstrated higher densities of Malassezia in lesional compared to non-lesional or healthy skin, with quantitative cultures showing significantly elevated yeast counts in affected scalp areas of patients with seborrhoeic dermatitis.[19] This overgrowth is supported by the clinical response to topical antifungals, such as ketoconazole, which reduce Malassezia populations and lead to rapid symptom improvement, thereby establishing a causal association.[19] Despite this role, seborrhoeic dermatitis is not contagious, as Malassezia represents normal skin flora present from early infancy in both healthy individuals and those susceptible to the condition.[19] Bacterial components of the skin microbiome also play a contributory role, with dysbiosis characterized by shifts in populations of Propionibacterium (now classified as Cutibacterium) and Staphylococcus species.[20] Staphylococcus aureus is isolated more frequently from lesional skin of patients (49%) than from healthy controls (20%), potentially exacerbating the condition through secondary colonization and promotion of inflammation.[21] Coagulase-negative staphylococci, such as S. epidermidis, are predominant in seborrhoeic dermatitis lesions and decrease with effective treatment, suggesting involvement in microbial imbalance.[20] Cutibacterium acnes appears underrepresented in affected skin and may indirectly support pathogenesis by hydrolyzing sebum to provide substrates for Malassezia growth, though its density is often reduced compared to controls.[21] Evidence of biofilm formation by these bacteria remains limited, but their altered abundance supports a model of secondary microbial contributions to disease initiation in susceptible individuals.[20]Individual susceptibility factors
Seborrheic dermatitis is associated with immune dysfunction, particularly impaired T-cell responses and altered complement activation, which may contribute to an inadequate reaction against skin commensals. Recent genomic studies (as of 2025) have identified a unique immune profile in SD, characterized by elevated Th17 and Th22 cytokines and mutations in barrier function genes, further supporting immune dysregulation as a key susceptibility factor.[22] In individuals with HIV, the prevalence ranges from 20% to 83%, linked to immune dysregulation that disrupts the skin's microbial balance.[23] Similarly, patients with Parkinson's disease exhibit a strong association, potentially due to central nervous system influences on peripheral immune function, including reduced T-cell activity.[24] Organ transplant recipients on immunosuppressive therapy also show increased susceptibility, with studies reporting higher incidence rates attributed to diminished cellular immunity.[1] Genetic predisposition to seborrheic dermatitis involves familial clustering and mutations in immune-related genes, though no single gene has been definitively established as causative. Hereditary deficiencies in the complement component C5, such as nonsense mutations in exons 1 and 36, have been identified in affected families, leading to SD-like phenotypes through impaired innate immunity.[25] Polymorphisms in genes involved in inflammatory pathways, including those regulating IL-1 and TNF signaling, may heighten susceptibility by altering cytokine responses in the skin.[26] Animal models, such as mice with seb gene mutations, further support a genetic basis, demonstrating inherited traits like sebaceous gland hyperactivity and epidermal changes.[25] Nutritional deficiencies have been linked to seborrheic dermatitis in some cases, with evidence suggesting roles for zinc, pyridoxine (vitamin B6), and essential fatty acids, although causal relationships remain mixed. Zinc deficiency can manifest as periorificial dermatitis resembling seborrheic dermatitis, due to impaired epidermal barrier function and immune modulation.[27] Pyridoxine deficiency commonly presents with seborrheic-like eruptions on the scalp, face, and trunk, often in the context of malabsorption or dietary inadequacy.[28] Deficiencies in essential fatty acids may exacerbate symptoms through disrupted skin lipid composition, leading to increased transepidermal water loss and inflammation, though supplementation trials show variable efficacy.[29] Hormonal influences, particularly androgens, contribute to susceptibility by stimulating sebaceous gland activity and sebum production, which is prominent during puberty. Elevated androgen levels, such as dihydrotestosterone, enhance lipid secretion on the skin surface, creating an environment conducive to dermatitis flares.[30] Stress-induced hormonal shifts, including cortisol and androgen surges, can similarly trigger exacerbations by altering sebum composition and immune responses in sebaceous areas.[31]Environmental factors
Seborrheic dermatitis tends to exacerbate in cold, dry climates, where low temperatures and reduced humidity impair the skin barrier and increase symptom frequency.[32] Studies in temperate regions demonstrate an inverse correlation between ambient temperature and disease prevalence, with flares peaking during winter months when conditions are harshest on the skin.[32] Conversely, symptoms often improve in warm, humid environments, particularly with higher ultraviolet exposure during summer, which may suppress inflammatory responses.[33] Seasonal variations are pronounced in temperate zones, with the highest incidence reported in autumn and winter—up to 35% of cases—compared to only 13-14% in summer.[32] Changes in season, such as the transition to drier air, commonly trigger outbreaks by altering skin hydration and microbial balance.[3] These patterns highlight how environmental humidity and UV index inversely influence disease activity, with low levels of both correlating to increased risk.[32] Psychological stress frequently precedes flares of seborrheic dermatitis, with patients often identifying it as a primary trigger in a study of 82 individuals, where it was linked to poorer prognosis.[34] Elevated cortisol from stress can stimulate sebum production, creating conditions favorable for symptom worsening, and is linked to higher recurrence rates and poorer prognosis.[34] Lifestyle factors, including poor hygiene or use of occlusive hair products and detergents, may further aggravate the condition by trapping moisture and irritants on affected skin.[35] Occupational exposures rarely cause seborrheic dermatitis but can exacerbate it through irritants or prolonged occlusion from personal protective equipment in hot environments.[36] For instance, workers in metalworking or similar industries wearing flame-retardant gear for extended periods may experience relapsing facial and scalp eruptions mimicking or worsening the disease.[36] Such cases are often underreported and may be misdiagnosed as irritant contact dermatitis due to overlapping presentations.[36]Pathophysiology
Initiating factors
Seborrheic dermatitis often initiates through the interaction between excess sebum production and Malassezia yeast proliferation on the skin surface. Malassezia species, lipophilic fungi resident in sebaceous areas, metabolize sebum triglycerides via lipase activity, releasing irritant free fatty acids such as oleic acid and arachidonic acid.[8] These metabolites penetrate the stratum corneum, altering epidermal lipid composition and initiating early pathological changes.[37] The microbial byproducts from this sebum-Malassezia interaction contribute to initial barrier disruption by inducing aberrant keratinocyte differentiation and stratum corneum abnormalities, such as parakeratosis and lipid droplet accumulation. This weakens the skin's protective barrier, allowing further penetration of irritants and setting the stage for disease onset without invoking a primary infectious process.[8] Oleic acid, in particular, has been shown to disrupt the lamellar structure of epidermal lipids, exacerbating susceptibility in seborrheic regions.[37] Onset of seborrheic dermatitis frequently occurs post-puberty, coinciding with hormonally driven increases in sebaceous gland activity and sebum output, which provide an enriched substrate for Malassezia growth.[8] Trigger events such as psychological stress, acute illness, or immune compromise can precipitate initial flares, often in an idiopathic manner without a clear precipitant.[8] For instance, stress elevates cortisol levels that may indirectly promote sebum alterations, while conditions like HIV infection heighten risk through subtle immune shifts.[8] The disease follows a multifactorial model of initiation, where no single factor predominates; instead, convergence of heightened sebaceous secretions, microbial colonization by Malassezia, and host susceptibility—such as genetic predispositions affecting sebum composition—collectively drive the early events.[8] This interplay underscores the idiopathic nature of many cases, with environmental modulators like seasonal changes amplifying the process.[37]Inflammatory and epidermal response
In seborrheic dermatitis, immune activation is primarily driven by antigens from Malassezia species, which stimulate T helper 1 (Th1) and Th17 cells, leading to the release of proinflammatory cytokines such as interleukin-1 (IL-1), IL-6, and tumor necrosis factor-alpha (TNF-α).[38] These cytokines promote local inflammation and activate the complement system, exacerbating the immune response in sebaceous gland-rich areas. Th17 cells further contribute by producing IL-17 and IL-22, which amplify keratinocyte responses and sustain chronic inflammation.[39] This immune cascade induces epidermal hyperproliferation, characterized by abnormal keratinization that results in parakeratosis and the formation of adherent scales.[40] In acute phases, spongiosis—intercellular edema within the epidermis—predominates, contributing to the erythematous and pruritic lesions.[37] Chronic lesions exhibit psoriasiform hyperplasia, with thickened stratum corneum and reduced spongiosis, reflecting ongoing dysregulated epidermal turnover.[40] Vascular changes accompany these processes, with cytokine-mediated dilation of superficial dermal vessels causing the hallmark erythema observed in affected sites.[40] The inflammatory and epidermal responses typically resolve with diminution of precipitating factors, such as reduced microbial burden or environmental stressors, allowing normalization of immune and barrier functions.[1] However, relapses are frequent due to underlying individual susceptibility, including genetic predispositions to aberrant immune signaling and barrier defects.[39]Management
Seborrhoeic dermatitis in adults is highly manageable with consistent treatment, which can achieve dramatic and lasting improvement, with many patients experiencing near-total clearance of symptoms. Although no treatment eradicates the condition permanently, therapies including topical antifungals (e.g., ketoconazole, selenium sulfide) and newer options such as roflumilast foam render it controllable for most individuals, allowing symptom-free periods much of the time with suitable maintenance routines. Persistent flares may necessitate dermatologist consultation for personalized plans or assessment of related conditions.[7]Antifungal treatments
Antifungal treatments for seborrhoeic dermatitis primarily target the overgrowth of Malassezia yeast species, which play a key role in the condition's pathogenesis.[12] These agents, particularly azoles, are considered first-line therapy for mild to moderate cases, reducing fungal load and alleviating symptoms such as erythema, scaling, and pruritus.[13] There is no single "best" shampoo for seborrheic dermatitis universally agreed upon in 2025, as effectiveness varies by individual. However, medicated shampoos with ketoconazole (e.g., Nizoral) are widely recommended as highly effective against the Malassezia yeast causing the condition. Other strong options include those with selenium sulfide, zinc pyrithione, or salicylic acid. In 2025 reviews, Nizoral, CeraVe Anti-Dandruff Hydrating Shampoo, and Jupiter Balancing Shampoo were highlighted for dandruff and seborrheic dermatitis relief.[41][42] Topical azoles, such as ketoconazole 2% shampoo or cream, are commonly prescribed and applied 2-3 times weekly after initial daily use for 2-4 weeks, with the shampoo left on the scalp for 3-5 minutes before rinsing.[13][43] In Sweden, ketoconazole 2% shampoo is available over-the-counter at pharmacies, with Fungoral 20 mg/ml being a widely recommended option. It treats both dandruff and seborrheic dermatitis by targeting the Malassezia fungus and is approved for adults and children over 12 years. The recommended usage is to apply it twice weekly for 2-4 weeks, leaving it on for 3-5 minutes before rinsing. If symptoms do not improve within one month or are severe, consult a physician for further assessment and possible complementary treatment, such as a corticosteroid solution.[44] Ketoconazole effectively decreases Malassezia colonization and improves clinical symptoms, with studies showing significant reduction in scaling, itching, and flakes (approximately 70-80% improvement in trials).[12] Ciclopirox olamine serves as an effective alternative, available as 1% shampoo applied 2-3 times weekly or 0.77% gel twice daily, demonstrating superior tolerability and symptom relief in moderate to severe cases without notable differences between concentrations.[13] Zinc pyrithione shampoos, with antifungal properties, are effective for mild to moderate cases, providing good long-term control of symptoms based on clinical evidence.[45] Selenium sulfide shampoos (1-2.5%) offer another antifungal option, particularly for oily and scaly presentations, with studies indicating significant reduction in flaking and scaling.[46] These antifungal shampoos are also applicable to facial and beard areas affected by seborrheic dermatitis, where the condition commonly manifests as beard dandruff with associated itch and flaking. Over-the-counter 1% ketoconazole shampoo (e.g., Nizoral A-D) can be applied to the damp beard and surrounding skin, lathered thoroughly, left on for several minutes (typically 3–5 minutes), and then rinsed off. For faster relief from flakes and itch, it is often used daily initially until symptoms improve, followed by maintenance use 2–3 times weekly or as directed. Similarly, anti-dandruff shampoos containing pyrithione zinc (e.g., Head & Shoulders) or selenium sulfide can be applied in the same manner for milder cases. Consultation with a physician is recommended if symptoms persist or do not improve.[14][47][48] Overall, topical antifungals clear symptoms in approximately 70-90% of patients within 4 weeks, though maintenance therapy (e.g., twice-weekly applications) is recommended to prevent relapse.[12] For severe or recalcitrant cases, oral antifungals like fluconazole or itraconazole may be used under medical supervision, with regular monitoring for hepatic effects due to potential systemic absorption.[49] Fluconazole, typically dosed at 200-300 mg weekly for 2-4 weeks, has shown clinical efficacy in reducing symptoms, though results vary across studies.[50] Itraconazole, administered as 200 mg daily for 1 week followed by intermittent dosing (e.g., 200 mg twice daily for 2 days monthly), achieves marked improvement in about 67-83% of patients by 3 months.[51] Common side effects of topical antifungals include mild irritation, pruritus, or contact dermatitis, which are generally well-tolerated with low incidence.[13] Oral agents carry risks of nausea, headache, abdominal pain, and rare hepatotoxicity, necessitating liver function tests during treatment.[52]Anti-inflammatory treatments
Anti-inflammatory treatments for seborrhoeic dermatitis primarily target the reduction of erythema, pruritus, and scaling through suppression of inflammatory pathways in the skin. These agents are often used for short durations to manage acute flares, particularly in sensitive areas like the face and scalp, where they provide symptomatic relief without addressing underlying microbial factors.[53] Topical corticosteroids, such as hydrocortisone 1% cream or fluocinolone acetonide 0.01% oil-based solution, are commonly prescribed for initial control of inflammation in seborrhoeic dermatitis. Hydrocortisone 1% is available over-the-counter and suitable for mild cases on the face and body, including beard areas affected by seborrhoeic dermatitis, where it provides quick relief from itch; it is applied sparingly to affected skin once or twice daily. Fluocinolone is particularly effective for scalp involvement, where it can be applied as a shampoo or oil and left on for several minutes before rinsing. These agents are recommended for short-term use, typically 1-2 weeks, to minimize risks such as skin atrophy, telangiectasia, or tachyphylaxis, which can occur with prolonged application. Consult a doctor if symptoms persist.[33][54][7][14] Calcineurin inhibitors, including tacrolimus 0.1% ointment and pimecrolimus 1% cream, serve as steroid-sparing alternatives, especially for facial seborrhoeic dermatitis where long-term steroid use is undesirable. Tacrolimus and pimecrolimus inhibit T-cell activation, reducing inflammation without the atrophogenic effects of corticosteroids. They are applied twice daily to affected areas and have shown efficacy in clearing symptoms within 2 weeks, with maintenance therapy possible for recurrent cases. These agents are particularly beneficial for periorificial regions, offering a safer profile for extended use in sensitive skin.[14][55][56] Phosphodiesterase-4 (PDE4) inhibitors represent a newer non-steroidal class, with roflumilast 0.3% foam (Zoryve) approved by the FDA in December 2023 for treating seborrhoeic dermatitis in patients aged 9 years and older. Applied once daily to the scalp and body, roflumilast foam targets cyclic AMP elevation to dampen inflammatory cytokine release, providing broad coverage without the need for frequent dosing. Clinical trials demonstrated that 73.8% of patients achieved treatment success (Investigator Global Assessment score of 0 or 1 with at least a 2-grade improvement from baseline) after 8 weeks, compared to 40.9% with vehicle.[57][58] Overall, anti-inflammatory treatments offer rapid symptom relief, with improvement rates ranging from 70-80% in responsive cases across classes, though long-term use requires monitoring for potential tolerance or side effects like tachyphylaxis in corticosteroids. Selection depends on lesion location, severity, and patient factors, with non-steroidal options preferred for maintenance to avoid cutaneous thinning.[53][58][54]Adjunctive therapies
Adjunctive therapies for seborrhoeic dermatitis aim to alleviate symptoms such as scaling and itching through supportive measures that complement primary treatments. These include keratolytics to facilitate scale removal, antimicrobial agents like selenium sulfide for mild cases, and symptomatic relief options for pruritus. Keratolytics, such as shampoos containing 2% salicylic acid or 5% coal tar, are used to loosen and remove adherent scales from the scalp and other affected areas, particularly in cases of thick, white, scaly, oily dandruff. These agents work by softening the hyperkeratotic stratum corneum, allowing easier desquamation, exfoliating the skin, and helping to control excess oil production; they are often combined with antifungal treatments for enhanced efficacy. Salicylic acid shampoos are typically applied 2-3 times weekly, left on for 5-10 minutes before rinsing. Clinical guidelines recommend their incorporation into maintenance regimens for moderate scaling, with evidence from randomized trials supporting their efficacy in reducing flaking without significant adverse effects.[13][1][15][46] Selenium sulfide shampoos (0.5-2.5%) serve as an over-the-counter option for mild seborrhoeic dermatitis, particularly on the scalp, by reducing yeast overgrowth and scaling. Applied twice weekly, they provide antipruritic and keratolytic benefits, though they are generally less effective than antifungal alternatives and may cause mild irritation in sensitive skin. Systematic reviews indicate level C evidence for their role in symptom control and relapse prevention in adult patients.[13][12][1] For severe pruritus, oral antihistamines such as loratadine (10 mg daily) may be prescribed as an adjunct, especially when itching disrupts sleep or is histamine-mediated, as scalp histamine levels are elevated in affected individuals. These are rarely used as primary therapy but offer symptomatic relief in refractory cases, with studies showing partial efficacy in dermatitic pruritus.[59][60][61] Emollients, including fragrance-free creams or lotions like sorbolene, help hydrate dry, irritated skin and prevent barrier disruption in seborrhoeic dermatitis. Applied daily after cleansing, they reduce scaling and discomfort, particularly in facial or body involvement, and are supported by expert consensus for maintaining skin integrity.[1][62] Lifestyle measures play a key role in management, emphasizing gentle daily cleansing with mild, non-irritating shampoos and soaps to remove excess sebum and scales without exacerbating inflammation. During active flares of seborrhoeic dermatitis, particularly affecting the scalp, it is generally recommended to stop or minimize the use of many hair products to avoid further irritation. Patients should avoid styling products such as hair sprays, gels, pomades, and those containing alcohol, fragrances, or other irritants, as these can worsen symptoms. Instead, switch to gentle, fragrance-free, eczema-friendly shampoos or medicated antifungal shampoos (e.g., with ketoconazole or zinc pyrithione) as advised by a doctor, and avoid conditioners or other non-essential hair products during flares. Patients should also avoid other triggers like harsh detergents, alcohol-based products, and excessive heat, which can worsen symptoms. In cases of documented zinc deficiency—associated with lower serum levels in seborrhoeic dermatitis patients—supplementation (e.g., 15-30 mg elemental zinc daily) may improve outcomes, though routine use is not recommended without testing.[14][48][1][15][63][64] Patients are advised to consult a dermatologist if there is no improvement after one month of treatment. This information is not personalized medical advice.Phototherapy and other modalities
Phototherapy, particularly narrowband ultraviolet B (NB-UVB), serves as a non-pharmacological option for managing severe or refractory seborrhoeic dermatitis, typically administered 2-3 times per week in clinical settings.[65] This modality targets widespread inflammatory lesions by delivering controlled doses of UVB light, starting at 50-70% of the minimal erythema dose and incrementally increasing based on skin response, often over 8-12 weeks to achieve clearance.[65] In a study of 10 patients with severe disease, NB-UVB treatment resulted in a median clinical score reduction from 7.5 to 0.5 after 8 weeks, indicating near-complete resolution in most cases, with no serious adverse events reported during the course.[65] The mechanism involves suppression of inflammatory responses in the skin, including induction of apoptosis in activated T-cells, which contributes to decreased erythema and scaling in affected areas.[66] Efficacy is particularly notable in resistant patients, with response rates exceeding 70% in small cohorts when used for severe scalp and facial involvement, though relapse often occurs within months post-treatment.[67] Combining NB-UVB with topical antifungals or keratolytics can enhance outcomes by addressing microbial and hyperkeratotic components simultaneously, leading to faster symptom control.[68] Other procedural modalities include targeted laser therapies for localized plaques, though evidence is limited; excimer laser (308 nm), which delivers focused UVB to small areas, has shown promise in analogous inflammatory conditions but requires further validation for seborrhoeic dermatitis.[69] For hyperkeratotic variants, low-dose oral retinoids such as isotretinoin (e.g., 10-20 mg daily) offer an alternative in refractory cases, reducing sebum production and scaling with moderate efficacy and tolerability in clinical trials.[70] One randomized trial demonstrated significant improvement in moderate-to-severe seborrhoeic dermatitis symptoms after 3 months of low-dose isotretinoin compared to placebo, with sustained benefits in adherent patients.[71] These approaches are reserved for cases unresponsive to first-line topicals due to risks including short-term erythema or pruritus from phototherapy and potential long-term effects like premature skin aging or increased non-melanoma skin cancer risk with cumulative UVB exposure.[72] Oral retinoids carry risks of mucocutaneous dryness, hyperlipidemia, and teratogenicity, necessitating careful monitoring.[70] Overall, phototherapy and retinoids are not first-line but provide valuable options for severe, treatment-resistant disease.[73]Maintenance therapy
Seborrhoeic dermatitis is a chronic condition requiring ongoing maintenance therapy to prevent relapses. No dedicated new international guidelines for maintenance therapy were issued specifically in 2024 or 2025. However, recent narrative reviews (2025) and updated resources (e.g., NICE CKS revised November 2024, AAFP 2025) emphasize its chronic nature and the need for maintenance to sustain remission.[74][75][76] Maintenance typically involves reduced frequency of application after 2-4 weeks of initial daily or every-other-day treatment. Common recommendations include:- Topical antifungals (e.g., ketoconazole 2% shampoo or cream): once weekly or every 1-2 weeks after initial treatment.[76]
- Topical calcineurin inhibitors (e.g., tacrolimus 0.1% or pimecrolimus 1%): twice weekly for facial areas.[76]
- OTC shampoos (e.g., selenium disulfide, zinc pyrithione): once weekly or every other week.[76]
- Topical corticosteroids: limited twice-weekly use due to side effects.[76]

