Recent from talks
Nothing was collected or created yet.
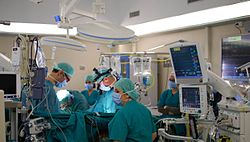
Surgeon
View on WikipediaIn medicine, a surgeon is a medical doctor who performs surgery. Even though there are different traditions in different times and places, a modern surgeon is a licensed physician and received the same medical training as physicians before specializing in surgery.
In some countries and jurisdictions, the title of 'surgeon' is restricted to maintain the integrity of the craft group in the medical profession. A specialist regarded as a legally recognized surgeon includes podiatry, dentistry, and veterinary medicine. It is estimated that surgeons perform over 300 million surgical procedures globally each year.[1][2]
History
[edit]
The first person to document a surgery was the 6th century BC Indian physician-surgeon, Sushruta. He specialized in cosmetic plastic surgery and even documented an open rhinoplasty procedure.[3] His magnum opus Suśruta-saṃhitā is one of the most important surviving ancient treatises on medicine and is considered a foundational text of both Ayurveda and surgery. The treatise addresses all aspects of general medicine, but the translator G. D. Singhal dubbed Sushruta "the father of surgical intervention" on account of the extraordinarily accurate and detailed accounts of surgery to be found in the work.[4]
After the eventual decline of the Sushruta School of Medicine in India, surgery was largely ignored until the Islamic Golden Age surgeon Al-Zahrawi (936–1013) re-established surgery as an effective medical practice. He is considered the greatest medieval surgeon to have appeared from the Islamic World, and has also been described as the father of surgery.[5] His greatest contribution to medicine is the Kitab al-Tasrif, a thirty-volume encyclopedia of medical practices.[6] He was the first physician to describe an ectopic pregnancy, and the first physician to identify the hereditary nature of haemophilia.[7]
His pioneering contributions to the field of surgical procedures and instruments had an enormous impact on surgery but it was not until the 18th century that surgery emerged as a distinct medical discipline in England.[7]
In Europe, surgery was mostly associated with barber-surgeons who also used their hair-cutting tools to undertake surgical procedures, often at the battlefield and also for their employers.[8] With advances in medicine and physiology, the professions of barbers and surgeons diverged; by the 19th century barber-surgeons had virtually disappeared, and surgeons were almost invariably qualified doctors who had specialized in surgery. Surgeon continued, however, to be used as the title for military medical officers until the end of the 19th century, and the title of Surgeon General continues to exist for both senior military medical officers and senior government public health officers.
Titles in the Commonwealth
[edit]In 1950, the Royal College of Surgeons of England (RCS) in London began to offer surgeons a formal status via RCS membership. The title Mister became a badge of honour, and today, in many Commonwealth countries, a qualified doctor who, after at least four years' training, obtains a surgical qualification (formerly Fellow of the Royal College of Surgeons, but now also Member of the Royal College of Surgeons or a number of other diplomas) is given the honour of being allowed to revert to calling themselves Mr, Miss, Mrs or Ms in the course of their professional practice, but this time the meaning is different. It is sometimes assumed that the change of title implies consultant status (and some mistakenly think non-surgical consultants are Mr too), but the length of postgraduate medical training outside North America is such that a qualified surgeon may be years away from obtaining such a post: many doctors previously obtained these qualifications in the senior house officer grade, and remained in that grade when they began sub-speciality training. The distinction of Mr (etc.) is also used by surgeons in the Republic of Ireland, some states of Australia, Barbados, New Zealand, South Africa, Zimbabwe, and some other Commonwealth countries.[9] In August 2021, the Royal Australasian College of Surgeons announced that it was advocating for this practice to be phased out and began encouraging the use of the gender neutral title Dr or appropriate academic titles such as Professor.[10]
The reason for the otherwise undistinguished title of "mister" is historical. In the 18th century only physicians, with an MD degree, were entitled to call themselves "doctor". Most surgeons did not have a degree—in the Middle Ages they were also barbers, expert users of cutting tools—and were considered inferior and subordinate to physicians; "Mr" was initially a lower honorific, but came to be a badge of honour.[11]
Military titles
[edit]In many English-speaking countries the military title of surgeon is applied to any medical practitioner, due to the historical evolution of the term. The US Army Medical Corps retains various surgeon United States military occupation codes in the ranks of officer pay grades, for military personnel dedicated to performing surgery on wounded soldiers.
Specialties
[edit]
- Cardiothoracic surgery
- Colorectal surgery
- Craniofacial surgery
- Dental surgery
- Endocrine surgery
- General surgery
- Neurological surgery
- Obstetrics and gynaecology
- Ophthalmology
- Oral and maxillofacial surgery
- Orthopedic surgery
- Otorhinolaryngology
- Pediatric surgery
- Plastic surgery
- Podiatric surgery
- Surgical oncology
- Thoracic surgery (in the United States considered part of cardiothoracic surgery)
- Transplant surgery
- Trauma surgery
- Upper gastrointestinal surgery
- Urology
- Vascular surgery
Some physicians who are general practitioners or specialists in family medicine or emergency medicine may perform limited ranges of minor, common, or emergency surgery. Anesthesia often accompanies surgery, and anesthesiologists and nurse anesthetists may oversee this aspect of surgery. Surgeon's assistant, surgical nurses, surgical technologists are trained professionals who support surgeons.
In the United States, the Department of Labor description of a surgeon is "a physician who treats diseases, injuries, and deformities by invasive, minimally-invasive, or non-invasive surgical methods, such as using instruments, appliances, or by manual manipulation".[12]
Around the world, the array of 'surgical' pathology that a surgeon manages does not always require surgical methods. For example, surgeons treat diverticulitis conservatively using antibiotics and bowel rest. In some cases of small bowel obstruction, particularly where a patient has had previous abdominal surgery, the surgeon treats the patient with fluid resuscitation, nasogastric decompression of the stomach, which gives rise to resolution of the intestinal obstruction in cases where adhesions are the aetiology of the obstruction. The same is true for other craft groups in surgery.
Pioneer surgeons
[edit]

- Christiaan Barnard (cardiac surgery, first heart transplantation)
- Alfred Blalock (first modern day successful open heart surgery in 1944)
- Nina Starr Braunwald (First female cardiac surgeon)
- Dorothy-Laviania Brown (First female African-American surgeon)
- Victor Chang Australian pioneer of heart transplantation
- Harvey Cushing (pioneer, and often considered the father of, modern neurosurgery)
- Eleanor Davies-Colley (surgeon and founder of the South London Hospital for Women and Children)
- Michael DeBakey (educator and innovator in the field of cardiac surgery)
- René Favaloro (first surgeon to perform bypass surgery)
- Svyatoslav Fyodorov (creator of radial keratotomy)
- Harold Gillies (pioneer of plastic surgery)
- Jesse Gray (First female chief of surgery at Hopkinz Hospital)
- William Stewart Halsted (initiated surgical residency training in U.S., pioneer in many fields)
- Michael R. Harrison (pioneer of fetal surgery)
- Sir Victor Horsley (neurosurgery)
- John Hunter (Scottish, viewed as the father of modern surgery, performed hundreds of dissections, served as the model for Dr. Jekyll.)
- Gavriil Ilizarov, inventor of the Ilizarov apparatus for lengthening limb bones and for the method of surgery named after him, the Ilizarov surgery
- Charles Kelman (Invented phacoemulsification, the technique of modern cataract surgery)
- Lars Leksell (neurosurgery, inventor of radiosurgery)
- C. Walton Lillehei (labeled "Father of modern day open heart surgery")
- Joseph Lister (discoverer of surgical sepsis,[13] Listerine named in his honour[13])
- B. K. Misra – first neurosurgeon in the world to perform image-guided surgery for aneurysms, first in South Asia to perform stereotactic radiosurgery, first in India to perform awake craniotomy and laparoscopic spine surgery.[14]
- Ioannis Pallikaris (Greek surgeon. Performed the first LASIK procedure on a human eye.[15] Developed Epi-LASIK.[16])
- Fidel Pagés (pioneer of epidural anesthesia)
- Wilder Penfield (neurosurgery)
- Gholam A. Peyman (inventor of LASIK,[17])
- Nikolay Pirogov (the founder of field surgery)
- Jennie Simile Robertson (first female surgeon in Canada)
- Valery Shumakov (pioneer of artificial organs implantation)
- Maria Siemionow (pioneer of near-total face transplant surgery)
- Thomas E. Starzl (pioneer of the development of liver transplantations[18])
- Sushruta (the first to document an operation of open rhinoplasty[3])
- Paul Tessier (French surgeon in Craniofacial surgery)
- Mary Edwards Walker (first female surgeon in the United States)
- Gazi Yasargil (Turkish neurosurgeon, founder of microneurosurgery)
- al-Zahrawi, regarded as one of the greatest medieval surgeons and a father of surgery.[19]
Organizations and fellowships
[edit]References
[edit]- ^ Weiser, Thomas G.; Haynes, Alex B.; Molina, George; Lipsitz, Stuart R.; Esquivel, Micaela M.; Uribe-Leitz, Tarsicio; Fu, Rui; Azad, Tej; Chao, Tiffany E.; Berry, William R.; Gawande, Atul A. (2015). "Estimate of the global volume of surgery in 2012: An assessment supporting improved health outcomes". The Lancet. 385: S11. doi:10.1016/S0140-6736(15)60806-6. PMID 26313057. S2CID 24856780.
- ^ Liu, Liang Qin; Mehigan, Sinead (2021). "A Systematic Review of Interventions Used to Enhance Implementation of and Compliance with the World Health Organization Surgical Safety Checklist in Adult Surgery" (PDF). AORN Journal. 114 (2): 159–170. doi:10.1002/aorn.13469. PMID 34314014. S2CID 236452617. Archived (PDF) from the original on 2023-02-28. Retrieved 2023-02-28.
- ^ a b Papel, Ira D. and Frodel, John (2008) Facial Plastic and Reconstructive Surgery. Thieme Medical Pub. ISBN 1588905152
- ^ Singhal, G. D. (1972). Diagnostic considerations in ancient Indian surgery: (based on Nidāna-Sthāna of Suśruta Saṁhitā). Varanasi: Singhal Publications.
- ^ Ahmad, Z. (St Thomas' Hospital) (2007), "Al-Zahrawi – The Father of Surgery", ANZ Journal of Surgery, 77 (Suppl. 1): A83, doi:10.1111/j.1445-2197.2007.04130_8.x, S2CID 57308997
- ^ al-Zahrāwī, Abū al-Qāsim Khalaf ibn ʻAbbās; Studies, Gustave E. von Grunebaum Center for Near Eastern (1973). Albucasis on surgery and instruments. University of California Press. ISBN 978-0-520-01532-6. Retrieved 16 May 2011.
- ^ a b Cosman, Madeleine Pelner; Jones, Linda Gale (2008). Handbook to Life in the Medieval World. Handbook to Life Series. Vol. 2. Infobase Publishing. pp. 528–530. ISBN 978-0-8160-4887-8.
- ^ "Surgeons and Surgical Spaces #The barbers shop". sciencemuseum.org.uk. Archived from the original on 2020-08-07. Retrieved 2020-05-05.
- ^ "Patients: The Surgical Team: Qualifications of a surgeon". Royal College of Surgeons of England. Archived from the original on 2 July 2015. Retrieved 13 June 2015.
- ^ "RACS phases out gendered titles for surgeons". Royal Australasian College of Surgeons. Archived from the original on 31 August 2021. Retrieved 31 August 2021.
- ^ Loudon, I. (23 December 2000). "Why are (male) surgeons still addressed as Mr?". BMJ. 321 (7276): 1589–1591. doi:10.1136/bmj.321.7276.1589. ISSN 0959-8138. PMC 1119265. PMID 11124190.
- ^ "Occupational Employment Statistic: Occupational Employment and Wages, May 2015: 29–1067 Surgeons". bls.gov. Archived from the original on 2016-05-06. Retrieved 2016-04-26.
- ^ a b "Joseph Lister's antisepsis system | Science Museum". www.sciencemuseum.org.uk. Retrieved 2024-04-28.
- ^ Basant Kumar Misra, President NSI 2008. Neurological Society of India
- ^ Stuart, Annie (1 June 2009). "A Look at LASIK Past, Present and Future". American Academy of Ophthalmology. Archived from the original on 10 July 2016. Retrieved 2 July 2016.
- ^ "When Cornea Transplants Fail. What Next?" Harvard University. Archived 2006-09-09 at the Wayback Machine
- ^ Peyman, Gholam A. (1989) U.S. patent 4,840,175 "Method for modifying corneal curvature".
- ^ "The Transplanted Organs: The Liver". www.starzl.pitt.edu.
- ^ Martín-Araguz, A.; Bustamante-Martínez, C.; Fernández-Armayor Ajo, V.; Moreno-Martínez, J. M. (2002). "Neuroscience in al Andalus and its influence on medieval scholastic medicine". Revista de Neurología. 34 (9): 877–892. doi:10.33588/rn.3409.2001382. PMID 12134355.