Methaqualone
View on Wikipedia
 | |
| Clinical data | |
|---|---|
| Pronunciation | /mɛθəˈkweɪloʊn/ |
| Trade names | Quaalude, Sopor, Mandrax |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Protein binding | 70–80% |
| Elimination half-life | Biphasic (10–40; 20–60 hours) |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.000.710 |
| Chemical and physical data | |
| Formula | C16H14N2O |
| Molar mass | 250.301 g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 113 °C (235 °F) |
| |
| |
| (verify) | |
Methaqualone is a sedative-hypnotic medication that was widely prescribed during the mid-20th century. It was marketed under various brand names, including Quaalude (/ˈkweɪluːd/ KWAY-lood) and Sopor, typically containing 300 mg of methaqualone per tablet. A combination drug known as Mandrax was sold primarily in Europe, containing 250 mg of methaqualone and 20 mg of diphenhydramine in a single tablet.
Methaqualone belongs to the quinazolinone class of compounds. Its commercial production was discontinued in many countries during the mid-1980s due to widespread misuse, addiction, and associated public health concerns.
Medical use
[edit]Methaqualone's sedative-hypnotic properties were first identified in 1955. It gained popularity during the 1960s and 1970s for the treatment of insomnia, and as a general sedative and muscle relaxant. However, due to its abuse potential, it was eventually withdrawn from medical use.
The drug was classified as pregnancy category D, meaning there was evidence of risk to the human fetus, and it was not recommended during pregnancy.[2]
Like other GABAergic substances, prolonged use of methaqualone can lead to drug tolerance, physical dependence, and withdrawal symptoms upon cessation.[3]
Overdose
[edit]An overdose of methaqualone can lead to coma and death.[4] Additional effects are delirium, convulsions, hypertonia, hyperreflexia, vomiting, kidney failure, and death through cardiac or respiratory arrest. Methaqualone overdose resembles barbiturate poisoning, but with increased motor difficulties and a lower incidence of cardiac or respiratory depression. The standard single tablet adult dose of Quaalude brand of methaqualone was 300 mg when made by Lemmon. A dose of 8000 mg is lethal and a dose as little as 2000 mg could induce a coma if taken with an alcoholic beverage.[5]
Pharmacology
[edit]Pharmacodynamics
[edit]Methaqualone acts primarily as a sedative, reducing anxiety and inducing sleep. It binds to GABAA receptors, where it functions as a positive allosteric modulator at many receptor subtypes, enhancing the inhibitory effects of the neurotransmitter GABA. It shows negligible affinity for a wide array of other potential targets, including other receptors and neurotransmitter transporters.[6] This action is similar to that of benzodiazepines like diazepam.
Unlike most benzodiazepines, however, methaqualone may also act as a negative allosteric modulator at certain GABAA receptor subtypes, producing excitatory effects in neurons expressing those receptors. As such, methaqualone is considered a mixed GABAA receptor modulator.[6]
The binding site for methaqualone on the GABAA receptor complex is distinct from those of benzodiazepines, barbiturates, and neurosteroids, though it may partially overlap with the etomidate binding site.[6]
Pharmacokinetics
[edit]Methaqualone reaches peak plasma concentrations within a few hours of administration. Its elimination half-life ranges between 20 and 60 hours, contributing to its sedative effects and potential for accumulation with repeated dosing.
History
[edit]Methaqualone was first synthesized in India in 1951 by Indra Kishore Kacker and Syed Husain Zaheer, who were conducting research on finding new antimalarial medications.[5][7][8] In 1962, methaqualone was patented in the United States by Wallace and Tiernan.[9] By 1965, it was the most commonly prescribed sedative in Britain, where it has been sold legally under the names Malsed, Malsedin, and Renoval. In 1965, a methaqualone/antihistamine combination was sold as the sedative drug Mandrax in Europe, by Roussel Laboratories (now part of Sanofi S.A.). In 1972, it was the sixth-bestselling sedative in the US,[10] where it was legal under the brand name Quaalude.
Quaalude in the United States was originally manufactured in 1965 by the pharmaceutical firm William H. Rorer, Inc., based in Fort Washington, Pennsylvania. The drug name "Quaalude" is a portmanteau, combining the words "quiet interlude" and shared a stylistic reference to another drug marketed by the firm, Maalox.[11]
In 1978, Rorer sold the rights to manufacture Quaalude to the Lemmon Company of Sellersville, Pennsylvania. At that time, Rorer chairman John Eckman commented on Quaalude's bad reputation stemming from illegal manufacture and use of methaqualone, and illegal sale and use of legally prescribed Quaalude: "Quaalude accounted for less than 2% of our sales, but created 98% of our headaches."[5]
Both companies still regarded Quaalude as an excellent sleeping drug. Lemmon, well aware of Quaalude's public image problems, used advertisements in medical journals to urge physicians "not to permit the abuses of illegal users to deprive a legitimate patient of the drug". Lemmon also marketed a small quantity under another name, Mequin, so doctors could prescribe the drug without the negative connotations.[5]
The rights to Quaalude were held by the JB Roerig & Company division of Pfizer, before the drug was discontinued in the United States in 1985, mainly due to its psychological addictiveness, widespread abuse, and illegal recreational use.[12]
A 2024 Hungarian investigative documentary reported on large-scale production and sales of the drug by the Hungarian People's Republic to the United States in the 1970s and 1980s. It asserts that a Hungarian state-owned company utilized connections to Colombian drug cartels to facilitate the sale of extraordinary amounts to the United States.[13][14]
Society and culture
[edit]Methaqualone became increasingly popular as a recreational drug and club drug in the late 1960s and 1970s, known variously as "ludes" or "disco biscuits"[15] due to its widespread use during the popularity of disco in the 1970s, or "sopers" (also "soaps") in the United States and Canada, and "mandrakes" and "mandies" in the United Kingdom, Australia and New Zealand. The substance was sold both as a free base and as a salt (hydrochloride).
Brand names
[edit]Methaqualone was sold under the brand name Quaalude (sometimes stylized "Quāālude" in the United States and Canada),[16] and Mandrax in the UK, South Africa, and Australia.
Regulation
[edit]Methaqualone was initially placed in Schedule I as defined by the UN Convention on Psychotropic Substances, but was moved to Schedule II in 1979.[17]
In Canada, methaqualone is listed in Schedule III of the Controlled Drugs and Substances Act and requires a prescription, but it is no longer manufactured. Methaqualone is banned in India.[18]
In the United States it was withdrawn from the market in 1983 and made a Schedule I drug in 1984.[19]
Recreational
[edit]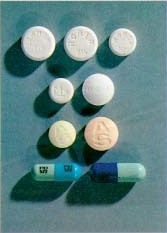
Methaqualone became increasingly popular as a recreational drug in the late 1960s and 1970s, known variously as "ludes" or "sopers" and "soaps" (sopor is a Latin word for sleep) in the United States and "mandrakes" and "mandies" in the UK, Australia and New Zealand.
The drug was more tightly regulated in Britain under the Misuse of Drugs Act 1971 and in the U.S. from 1973. It was withdrawn from many developed markets in the early 1980s. In the United States it was withdrawn in 1983 and made a Schedule I drug in 1984. It has a DEA ACSCN of 2565 and in 2022 the aggregate annual manufacturing quota for the United States was 60[20] grams.
Mention of its possible use in some types of cancer and AIDS treatments has periodically appeared in the literature since the late 1980s. Research does not appear to have reached an advanced stage. The DEA has also added the methaqualone analogue mecloqualone (also a result of some incomplete clandestine syntheses) to Schedule I as ACSCN 2572, with a manufacturing quota of 30 g.[20]
Gene Haislip, the former head of the Chemical Control Division of the Drug Enforcement Administration (DEA), told the PBS documentary program Frontline, "We beat 'em." By working with governments and manufacturers around the world, the DEA was able to halt production and, Haislip said, "eliminated the problem".[21][22] Methaqualone was manufactured in the United States under the name Quaalude by the pharmaceutical firms Rorer and Lemmon with the numbers 714 stamped on the tablet, so people often referred to Quaalude as 714's, "Lemmons", or "Lemmon 7's".
Methaqualone was also manufactured in the US under the trade names Sopor and Parest. After the legal manufacture of the drug ended in the United States in 1982, underground laboratories in Mexico continued the illegal manufacture of methaqualone throughout the 1980s, continuing the use of the "714" stamp, until their popularity waned in the early 1990s. Drugs purported to be methaqualone are in a significant majority of cases found to be inert, or contain diphenhydramine or benzodiazepines.
Illicit methaqualone is one of the most commonly used recreational drugs in South Africa. Manufactured clandestinely, often in India, it comes in tablet form, but is smoked with marijuana. This method of ingestion is known as "white pipe".[23][24] It is popular elsewhere in Africa and in India.[24]
Chemical weapon – Project Coast
[edit]Illegal efforts to weaponize methaqualone have occurred. During the 1980s, the apartheid regime in South Africa ordered the covert manufacture of a large amount of methaqualone at the front company Delta G Scientific Company, as part of a secret chemical weapons program known as Project Coast.[25] Methaqualone was given the codename MosRefCat (Mossgas Refinery Catalyst). Details of this activity came to light during the 1998 hearings of the post-apartheid Truth and Reconciliation Commission.
Sexual assault
[edit]Actor Bill Cosby admitted in a 2015 civil deposition to giving methaqualone to women before allegedly sexually assaulting them.[26][27] Film director Roman Polanski was convicted in 1977 of sexually assaulting a 13-year-old girl after giving her alcohol and methaqualone.[28]
Popular culture
[edit]Quaaludes are mentioned in the 1983 film Scarface, when Al Pacino's character Tony Montana says, "Another quaalude... she'll love me again." The little white pills, referred to as "ludes," get a cameo along with several other illicit drugs in the 1983 comedy-drama The Big Chill.[29] Quaaludes are also referenced extensively in the 2013 film The Wolf of Wall Street.[30] They are briefly mentioned in the movie Dinner in America as the reason behind the behavior of one of the characters. Almost Famous is another movie where the drug appears, as "Penny Lane", played by Kate Hudson, is shown to have taken quaaludes during a scene in which she is drugged.[31][32]
Parody glam rocker "Quay Lewd", one of the costumed performance personae used by Tubes singer Fee Waybill, was named after the drug. Many songs also refer to quaaludes, including the following: David Bowie's "Time" ("Time, in quaaludes and red wine"), "Rebel Rebel" ("You got your cue line/And a handful of 'ludes"), when signing "All The Young Dudes" on stage Bowie would often use the line ("All The Young Dudes, carry the ludes"); Lou Reed's song "The Last Shot" ("Shot a vein in my neck and I coughed up a Quaalude"); "Cosmic Doo Doo" by the American country music singer-songwriter Blaze Foley ("Got some quaaludes in their purse"); "That Smell" by Lynyrd Skynyrd ("Can't speak a word when you're full of 'ludes"); "Flakes" by Frank Zappa ("Wanna buy some mandies, Bob?"); "Straight Edge" by Minor Threat ("Laugh at the thought of eating ludes"); "Kind of Girl" by French Montana ("That high got me feelin' like the Quaaludes from Wolf of Wall Street"); and "Nights" by Frank Ocean ("This feel like a Quaalude")
Season 18 of Law & Order: Special Victims Unit addresses Quaalude administration as a date rape drug in episode 9, "Decline and Fall", which aired January 18, 2017.[33][34] In True Detective season 1, Rust Cohle's use of Quaaludes is briefly mentioned in several episodes.[35]
It is also used by Patrick Melrose in Edward St Aubyn's 1992 novel Bad News.[citation needed]
In the 2024 film Maria, Maria Callas, played by Angelina Jolie, stuffs Mandrax into the pockets of her coats and bags so that she'll be able to escape detection by her butler/guardian Ferruccio (Pierfrancesco Favino).
Further reading
[edit]- Hammer H, Bader BM, Ehnert C, Bundgaard C, Bunch L, Hoestgaard-Jensen K, et al. (August 2015). "A Multifaceted GABAA Receptor Modulator: Functional Properties and Mechanism of Action of the Sedative-Hypnotic and Recreational Drug Methaqualone (Quaalude)". Molecular Pharmacology. 88 (2): 401–420. doi:10.1124/mol.115.099291. PMC 4518083. PMID 26056160.
References
[edit]- ^ Anvisa (2023-07-24). "RDC Nº 804 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 804 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 2023-07-25). Archived from the original on 2023-08-27. Retrieved 2023-08-27.
- ^ "Methaqualone in Pregnancy and Breastfeeding". TheDrugSafety.com. Archived from the original on 2012-10-02. Retrieved 15 August 2012.
- ^ Suzuki T, Koike Y, Chida Y, Misawa M (April 1988). "Cross-physical dependence of several drugs in methaqualone-dependent rats". Japanese Journal of Pharmacology. 46 (4): 403–410. doi:10.1254/jjp.46.403. PMID 3404770.
- ^ "Recreational drugs tranquilizers". Drug Library EU. Archived from the original on 2013-03-02.
- ^ a b c d Linder L (28 May 1981). Simons Jr DC, Mayer B, Nordyke R, Torrey A (eds.). "Quaalude manufacturer: Image hurt by street use". Lawrence Journal-World. Vol. 123, no. 148. Lawrence, Kansas, United States of America. Associated Press. p. 6. Retrieved 16 August 2013 – via Google Newspapers.
Eckman/Fisher
- ^ a b c Hammer H, Bader BM, Ehnert C, Bundgaard C, Bunch L, Hoestgaard-Jensen K, et al. (August 2015). "A Multifaceted GABAA Receptor Modulator: Functional Properties and Mechanism of Action of the Sedative-Hypnotic and Recreational Drug Methaqualone (Quaalude)". Molecular Pharmacology. 88 (2): 401–420. doi:10.1124/mol.115.099291. PMC 4518083. PMID 26056160.
- ^ van Zyl EF (November 2001). "A survey of reported synthesis of methaqualone and some positional and structural isomers". Forensic Science International. 122 (2–3): 142–9. doi:10.1016/S0379-0738(01)00484-4. PMID 11672968.
- ^ Kacker IK, Zaheer SH (1951). "Potential Analgesics. Part I. Synthesis of substituted 4-quinazolones". J. Ind. Chem. Soc. 28: 344–346.
- ^ U.S. patent 3,135,659
- ^ Foltz RL, Fentiman AF, Foltz RB (August 1980). "GC/MS assays for abused drugs in body fluids" (PDF). NIDA Research Monograph. 32. Washington, D.C.: United States Department of Health and Human Services: 1–198. PMID 6261132. Archived from the original (PDF) on 2004-10-22.
- ^ "Dividends: Dropping the Last 'Lude". Time. 28 November 1983. Archived from the original on December 22, 2008. Retrieved 16 August 2013.
- ^ Silverstein S. "Quaaludes Again". Captain Wayne's Mad Music.com.
- ^ "A nagy titkosszolgálati drogjátszma – amikor a magyar Chinoin látta el kábítószerrel Amerikát | Válasz Online" (in Hungarian). Retrieved 2024-09-08.
- ^ Jamrik L, Csók I, Dezsö A, Ficzere B (2024-01-08), Vörös narkó (Documentary), X-Trame, retrieved 2024-09-08
- ^ Bekiempis V (August 2, 2015). "Do People Still Take Quaaludes?". Newsweek. NEWSWEEK DIGITAL LLC. Retrieved 22 July 2023.
- ^ Rile K (1983). Winter Music (First ed.). Boston and Toronto: Little, Brown and Company. pp. 41, 59. ISBN 978-0-316-74657-1.
- ^ Sandouk L. "green-lists". www.incb.org. Archived from the original on 2017-09-18. Retrieved 2017-09-06.
- ^ "Drugs banned in India". Central Drugs Standard Control Organization, Dte.GHS, Ministry of Health and Family Welfare, Government of India. Archived from the original on 2015-02-21. Retrieved 2013-09-17.
- ^ "Methaqualone". PubChem. U.S. National Library of Medicine. Retrieved 2021-05-19.
- ^ a b Drug Enforcement Administration (2 December 2021). "Established Aggregate Production Quotas for Schedule I and II Controlled Substances and Assessment of Annual Needs for the List I Chemicals Ephedrine, Pseudoephedrine, and Phenylpropanolamine for 2022". Federal Register, the Daily Register of the United States Government.
- ^ Ferns S (25 October 2007). "Lecture: Gene Haislip: The Chemical Connection: A Historical Perspective on Chemical Control" (PDF). Drug Enforcement Administration Museum Lecture Series. Arlington, Virginia. Archived from the original (PDF) on 31 March 2014.
- ^ Piccini S (Spring 2010). "Drug Warrior: The DEA's Gene Haislip '60, B.C.L. '63 Battled Worldwide Against the Illegal Drug Trade – and Scored a Rare Victory" (PDF). William & Mary Alumni Magazine. College of William & Mary.
- ^ "Mandrax". DrugAware. Reality Media. 2003. Retrieved 2009-08-13.
- ^ a b McCarthy G, Myers B, Siegfried N (April 2005). "Treatment for methaqualone dependence in adults". The Cochrane Database of Systematic Reviews (2) CD004146. doi:10.1002/14651858.CD004146.pub2. PMID 15846700.
- ^ "Project Coast: Apartheid's Chemical and Biological Warfare Program" (PDF). Geneva, Switzerland: United Nations Institute for Disarmament Research (UNIDIR).
- ^ Bowley G, Ember S (2015-07-19). "Bill Cosby, in Deposition, Said Drugs and Fame Helped Him Seduce Women". The New York Times. ISSN 0362-4331. Retrieved 2023-01-24.
- ^ Bowley G, Somaiya R (2015-07-07). "Bill Cosby Admission About Quaaludes Offers Accusers Vindication". The New York Times. ISSN 0362-4331. Retrieved 2023-01-24.
- ^ Freeman H (2018-01-30). "What does Hollywood's reverence for child rapist Roman Polanski tell us?". the Guardian. Retrieved 2023-01-24.
- ^ The Big Chill: When Boomers Stumble on the Truth about Their Own Failings, National Review, Kyle Smith, April 7, 2021
- ^ Loughrey C (18 September 2017). "Jordan Belfort had to teach Leonardo DiCaprio how to look like he was on drugs for Wolf of Wall Street". The Independent. Retrieved 24 January 2023.
- ^ "Kate Hudson thinks Hollywood's too sensitive". Yahoo News. July 6, 2020.
- ^ Colyar B (September 11, 2020). "The Real Penny Lane Has a Few Things Left to Say About Almost Famous". Vulture.
- ^ Janna Dela Cruz (January 15, 2017). "'Law & Order: SVU' season 18 episode 9 spoilers: Bob Gunton guest stars as billionaire rapist". The Christian Times. Retrieved February 19, 2023.
- ^ Jack Ori (January 18, 2017). "Law & Order: SVU Season 18 Episode 9 Review: Decline and Fall". TV Fanatic. Retrieved February 19, 2023.
- ^ "True Detective" The Long Bright Dark (TV Episode 2014) - IMDb. Retrieved 2024-09-09 – via www.imdb.com.
External links
[edit]Methaqualone
View on GrokipediaChemistry and Pharmacology
Chemical Properties and Synthesis
Methaqualone, chemically known as 2-methyl-3-(2-methylphenyl)-3,4-dihydroquinazolin-4-one, possesses the molecular formula CHNO and a molar mass of 250.30 g/mol.[1] It belongs to the quinazolinone class of heterocyclic compounds.[1] The compound was first synthesized in 1951 by Indian chemists Indra Kishore Kacker and Syed Husain Zaheer as part of research into potential therapeutic agents.[4] In its pure form, methaqualone free base manifests as white crystals with little to no odor and a bitter taste.[1] The melting point of the free base ranges from 113 °C to 116 °C, while the hydrochloride salt melts at 255–265 °C.[5] Methaqualone exhibits low solubility in water but dissolves readily in organic solvents, including 1 part in 12 parts ethanol, 1 part in 1 part chloroform, and 1 part in 50 parts ether.[1][5]| Property | Free Base Value | Hydrochloride Salt Value |
|---|---|---|
| Appearance | White crystals | Crystals |
| Melting Point (°C) | 113–116 | 255–265 |
| Solubility in Water | Practically insoluble | Low |
