Recent from talks
Nothing was collected or created yet.
Norethisterone
View on Wikipedia
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Norlutin, others |
| Other names | NET; Norethindrone; NSC-9564; LG-202; Ethinylnortestosterone; Norpregneninolone; Anhydrohydroxy-norprogesterone; Ethinylestrenolone; 17α-Ethynyl-19-nortestosterone; 17α-Ethynylestra-4-en-17β-ol-3-one; 17α-Hydroxy-19-norpregn-4-en-20-yn-3-one |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a604034 |
| License data | |
| Routes of administration | By mouth |
| Drug class | Progestin |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 47–73% (mean 64%)[9][10] |
| Protein binding | 97%:[11] Albumin: 61%;[11] SHBG: 36%[11] |
| Metabolism | Mainly CYP3A4 (liver);[12] also 5α-/5β-reductase, 3α-/3β-HSD, and aromatase |
| Elimination half-life | 5.2–12.8 hours (mean 8.0 hours)[9] |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.000.619 |
| Chemical and physical data | |
| Formula | C20H26O2 |
| Molar mass | 298.426 g·mol−1 |
| 3D model (JSmol) | |
| Melting point | 203 to 204 °C (397 to 399 °F) |
| |
| |
| (verify) | |
Norethisterone, also known as norethindrone and sold under the brand name Norlutin among others, is a progestin medication used in birth control pills, menopausal hormone therapy, and for the treatment of gynecological disorders.[11][13] The medication is available in both low-dose and high-dose formulations and both alone and in combination with an estrogen.[13][14] It is used by mouth or, as norethisterone enanthate, by injection into muscle.[11][13][15]
Side effects of norethisterone include menstrual irregularities, headaches, nausea, breast tenderness, mood changes, acne, increased hair growth.[16][17] Norethisterone is a progestin, or a synthetic progestogen, and hence is an agonist of the progesterone receptor, the biological target of progestogens like progesterone.[11][13] It has weak androgenic and estrogenic activity, mostly at high dosages, and no other important hormonal activity.[11][18]
Norethisterone was discovered in 1951 and was one of the first progestins to be developed.[19][20][21] It was first introduced for medical use on its own in 1957 and was introduced in combination with an estrogen for use as a birth control pill in 1963.[21][22] It is sometimes referred to as a "first-generation" progestin.[23][24] Like desogestrel and Norgestrel, Norethisterone is available as a progestogen-only "mini pill" for birth control.[25][26][27] Norethisterone is marketed widely throughout the world.[28] It is available as a generic medication.[29] In 2023, it was the 136th most commonly prescribed medication in the United States, with more than 4 million prescriptions.[30][31] It is on the World Health Organization's List of Essential Medicines.[32]
Medical uses
[edit]Norethisterone is used as a hormonal contraceptive in combination with an estrogen – usually ethinylestradiol (EE) – in combined oral contraceptive pills and alone in progestogen-only pills.
Another medical use of norethisterone is to alleviate endometriosis related pain. In fact, 50% of patients who received medical or surgical treatment for endometriosis-related pelvic pain have benefited from progestin therapy. This could be due to the fact that norethisterone induces endometrial proliferation during secretory phase, which has been shown to alleviate endometrial pain complaints. Another way in which norethisterone may be acting to reduce endometrial pain is via inhibition of ovulation. Endometriosis pain and discomfort is worse during ovulation.[33]
| Composition | Dose | Brand names | Use |
|---|---|---|---|
| NET only | Low (e.g., 0.35 mg) | Multiple[a] | Progestogen-only oral contraceptive |
| NET or NETA only | High (e.g., 5 mg, 10 mg) | Multiple[b] | Gynecological disorders and other uses |
| NETE only | Injection (e.g., 200 mg) | Multiple[c] | Progestogen-only injectable contraceptive |
| NET or NETA with ethinylestradiol | Low (e.g., 0.4 mg, 0.5 mg, 0.75 mg, 1 mg, 1.5 mg) | Multiple[d] | Combined oral contraceptive |
| NET with mestranol | Low (e.g., 1 mg, 2 mg) | Multiple[e] | Combined oral contraceptive |
| NETA with estradiol | Low (e.g., 0.1 mg, 0.5 mg) | Multiple[f] | Combined menopausal hormone therapy |
| NETE with estradiol valerate | Injection (e.g., 50 mg) | Multiple[g] | Combined injectable contraceptive |
| Abbreviations: NET = Norethisterone. NETA = Norethisterone acetate. NETE = Norethisterone enanthate. Sources: [34][35] [36][37] Notes:
| |||
Contraindications
[edit]High-dose (10 mg/day) norethisterone has been associated with hepatic veno-occlusive disease, and because of this adverse effect, norethisterone should not be given to patients undergoing allogeneic bone marrow transplantation, as it has been associated with substantially lower one-year survival post-transplantation.[38][39]
Side effects
[edit]At contraceptive and hormone replacement dosages (0.35 to 1 mg/day), norethisterone has essentially progestogenic side effects only. In most clinical studies of norethisterone for contraception or menopausal hormone therapy, the drug has been combined with an estrogen, and for this reason, it is difficult to determine which of the side effects were caused by norethisterone and which of them were caused by estrogen in such research. However, norethisterone enanthate, an intramuscularly administered prodrug of norethisterone which is used as a long-acting contraceptive, is used without an estrogen, and hence can be employed as a surrogate for norethisterone in terms of understanding its effects and tolerability. In clinical studies, the most common side effect with norethisterone enanthate has been menstrual disturbances, including prolonged bleeding or spotting and amenorrhea.[38]: 253 Other side effects have included periodic abdominal bloating and breast tenderness, both of which are thought to be due to water retention and can be relieved with diuretics.[38]: 253 There has been no association with weight gain, and blood pressure, blood clotting, and glucose tolerance have all remained normal.[38]: 253 However, a decrease in HDL cholesterol has been observed.[38]: 253
At high doses (5 to 60 mg/day), for instance those used in the treatment of gynecological disorders, norethisterone can cause hypogonadism due to its antigonadotropic effects and can have estrogenic and weak androgenic side effects.
High doses of norethisterone acetate (10 mg/day) have been associated with abnormal liver function tests, including significant elevations in liver enzymes.[40][41][42] These liver enzymes included lactate dehydrogenase and glutamate pyruvate transaminase.[42] Although they were described as having no clinical relevance,[42] the elevated liver enzymes associated with norethisterone acetate may have precluded its further development for male hormonal contraception.[40][41]
Androgenic
[edit]Due to its weak androgenic activity, norethisterone can produce androgenic side effects such as acne, hirsutism, and voice changes of slight severity in some women at high dosages (e.g., 10 to 40 mg/day).[17] This is notably not the case with combined oral contraceptives that contain norethisterone and EE, however.[18] Such formulations contain low dosages of norethisterone (0.35 to 1 mg/day)[18] in combination with estrogen and are actually associated with improvement in acne symptoms.[43][44] In accordance, they are in fact approved by the FDA for the treatment of acne in women in the United States.[43][44] The improvement in acne symptoms is believed to be due to a 2- to 3-fold increase in sex hormone-binding globulin (SHBG) levels and a consequent decrease in free testosterone levels caused by EE, which results in an overall decrease in androgenic signaling in the body.[45]
The sebaceous glands are highly androgen-sensitive and their size and activity are potential markers of androgenic effect.[46] A high dosage of 20 mg/day norethisterone or norethisterone acetate has been found to significantly stimulate the sebaceous glands, whereas lower dosages of 5 mg/day and 2.5 mg/day norethisterone and norethisterone acetate, respectively, did not significantly stimulate sebum production and were consequently regarded as devoid of significant androgenicity.[46] Conversely, dosages of norethisterone of 0.5 to 3 mg/day have been found to dose-dependently decrease SHBG levels (and hence to suppress hepatic SHBG production), which is another highly sensitive marker of androgenicity.[47]
A large clinical study of high to very high oral dosages of norethisterone (10 to 40 mg/day) administered for prolonged periods of time (4 to 35 weeks) to prevent miscarriage in pregnant women found that 5.5% of the women experienced mild androgenic side effects such as mild voice changes (hoarseness), acne, and hirsutism and that 18.3% of female infants born to the mothers showed, in most cases only slight, virilization of the genitals.[17] Maternal androgenic symptoms occurred most often in women who received a dosage of norethisterone of 30 mg/day or more for a period of 15 weeks or longer.[17] In the female infants who experienced virilization of the genitals, the sole manifestation in 86.7% of the cases was varied but almost always slight enlargement of the clitoris.[17] In the remaining 13.3% of the affected cases, marked clitoral enlargement and partial fusion of the labioscrotal folds occurred.[17] The dosages used in these cases were 20 to 40 mg/day.[17]
In a letter to the editor on the topic of virilization caused by high dosages of norethisterone acetate in women, a physician expressed that they had not observed the "slightest evidence of virilization" and that there had "certainly been no hirsutism nor any voice changes" in 55 women with advanced breast cancer that they had treated with 30 to 60 mg/day norethisterone for up to six months.[48]
High-dosage norethisterone has been used to suppress menstruation in women with severe intellectual disability who were incapable of handling their own menses.[49][50] A study of 118 nulliparous women treated with 5 mg/day norethisterone for a period of 2 to 30 months found that the drug was effective in producing amenorrhea in 86% of the women, with breakthrough bleeding occurring in the remaining 14%.[49] Side effects including weight gain, hirsutism, acne, headache, nausea, and vomiting all did not appear to increase in incidence and no "disturbing side effects" were noted in any of the women.[49][50] Another study of 5 mg/day norethisterone in 132 women also made no mention of androgenic side effects.[51] These findings suggest little to no risk of androgenic side effects with norethisterone at a dosage of 5 mg/day.[49][50] A study of 194 women treated with 5 to 15 mg/day norethisterone acetate for a median duration of 13 months of therapy to suppress symptoms of endometriosis observed no side effects in 55.2% of patients, weight gain in 16.1%, acne in 9.9%, mood lability in 8.9%, hot flashes in 8.3%, and voice deepening in two women (1.0%).[52]
Estrogenic
[edit]Norethisterone is weakly estrogenic (via conversion into its metabolite EE), and for this reason, it has been found at high dosages to be associated with high rates of estrogenic side effects such as breast enlargement in women and gynecomastia in men, but also with improvement of menopausal symptoms in fully menopausal women.[53] It has been suggested that very high dosages (e.g., 40 mg/day, which are sometimes used in clinical practice for various indications) of norethisterone acetate (and by extension norethisterone) may result in an increased risk of venous thromboembolism (VTE) analogously to high dosages (above 50 μg/day) of EE, and that even doses of norethisterone acetate of 10 to 20 mg, which correspond to EE doses of approximately 20 to 30 μg/day, may in certain women be associated with increased risk.[54][55] A study also found that ethinylestradiol and norethisterone had a greater influence on coagulation factors when the dose of norethisterone was 3 or 4 mg than when it was 1 mg.[56] This might have been due to additional ethinylestradiol generated by higher doses of norethisterone.[56]
Overdose
[edit]There have been no reports of serious side effects with overdose of norethisterone, even in small children.[8] As such, overdose usually does not require treatment.[8] High dosages of as much as 60 mg/day norethisterone have been studied for extended treatment durations without serious adverse effects described.[48]
Interactions
[edit]5α-Reductase plays an important role in the metabolism of norethisterone, and 5α-reductase inhibitors such as finasteride and dutasteride can inhibit its metabolism.[citation needed] Norethisterone is partially metabolized via hydroxylation by CYP3A4, and inhibitors and inducers of CYP3A4 can significantly alter circulating levels of norethisterone.[12] For instance, the CYP3A4 inducers rifampicin and bosentan have been found to decrease norethisterone exposure by 42% and 23%, respectively, and the CYP3A4 inducers carbamazepine and St. John's wort have also been found to accelerate norethisterone clearance.[12]
Pharmacology
[edit]Pharmacodynamics
[edit]Norethisterone is a potent progestogen and a weak androgen and estrogen.[11] That is, it is a potent agonist of the progesterone receptor (PR) and a weak agonist of the androgen receptor (AR) and the estrogen receptor (ER).[11] Norethisterone itself has insignificant affinity for the ER; its estrogenic activity is from an active metabolite that is formed in very small amounts, ethinylestradiol (EE), which is a very potent estrogen.[11] Norethisterone and its metabolites have negligible affinity for the glucocorticoid receptor (GR) and mineralocorticoid receptor (MR) and hence have no glucocorticoid, antiglucocorticoid, mineralocorticoid, or antimineralocorticoid activity.[11]
| Compound | Typea | PR | AR | ER | GR | MR | SHBG | CBG |
|---|---|---|---|---|---|---|---|---|
| Norethisterone | – | 67–75 | 15 | 0 | 0–1 | 0–3 | 16 | 0 |
| 5α-Dihydronorethisterone | Metabolite | 25 | 27 | 0 | 0 | ? | ? | ? |
| 3α,5α-Tetrahydronorethisterone | Metabolite | 1 | 0 | 0–1 | 0 | ? | ? | ? |
| 3α,5β-Tetrahydronorethisterone | Metabolite | ? | 0 | 0 | ? | ? | ? | ? |
| 3β,5α-Tetrahydronorethisterone | Metabolite | 1 | 0 | 0–8 | 0 | ? | ? | ? |
| Ethinylestradiol | Metabolite | 15–25 | 1–3 | 112 | 1–3 | 0 | 0.18 | 0 |
| Norethisterone acetate | Prodrug | 20 | 5 | 1 | 0 | 0 | ? | ? |
| Norethisterone enanthate | Prodrug | ? | ? | ? | ? | ? | ? | ? |
| Noretynodrel | Prodrug | 6 | 0 | 2 | 0 | 0 | 0 | 0 |
| Etynodiol | Prodrug | 1 | 0 | 11–18 | 0 | ? | ? | ? |
| Etynodiol diacetate | Prodrug | 1 | 0 | 0 | 0 | 0 | ? | ? |
| Lynestrenol | Prodrug | 1 | 1 | 3 | 0 | 0 | ? | ? |
| Notes: Values are percentages (%). Reference ligands (100%) were promegestone for the PR, metribolone for the AR, estradiol for the ER, dexamethasone for the GR, aldosterone for the MR, dihydrotestosterone for SHBG, and cortisol for CBG. Footnotes: a = Active or inactive metabolite, prodrug, or neither of norethisterone. Sources: See template. | ||||||||
Progestogenic activity
[edit]Norethisterone is a potent progestogen and binds to the PR with approximately 150% of the affinity of progesterone.[11] In contrast, its parent compounds, testosterone, nandrolone (19-nortestosterone), and ethisterone (17α-ethynyltestosterone), have 2%, 22%, and 44% of the relative binding affinity of progesterone for the PR.[57] Unlike norethisterone, its major active metabolite 5α-dihydronorethisterone (5α-DHNET), which is formed by transformation via 5α-reductase, has been found to possess both progestogenic and marked antiprogestogenic activity,[58] although its affinity for the PR is greatly reduced relative to norethisterone at only 25% of that of progesterone.[11] Norethisterone produces similar changes in the endometrium and vagina, such as endometrial transformation, and is similarly antigonadotropic, ovulation-inhibiting, and thermogenic in women compared to progesterone, which is in accordance with its progestogenic activity.[59][57][60]
Androgenic activity
[edit]Norethisterone has approximately 15% of the affinity of the anabolic–androgenic steroid (AAS) metribolone (R-1881) for the AR, and in accordance, is weakly androgenic.[11] In contrast to norethisterone, 5α-DHNET, the major metabolite of norethisterone, shows higher affinity for the AR, with approximately 27% of the affinity of metribolone.[11] However, although 5α-DHNET has higher affinity for the AR than norethisterone, it has significantly diminished and in fact almost abolished androgenic potency in comparison to norethisterone in rodent bioassays.[61][62] Similar findings were observed for ethisterone (17α-ethynyltestosterone) and its 5α-reduced metabolite, whereas 5α-reduction enhanced both the AR affinity and androgenic potency of testosterone and nandrolone (19-nortestosterone) in rodent bioassays.[62] As such, it appears that the ethynyl group of norethisterone at the C17α position is responsible for its loss of androgenicity upon 5α-reduction.[62]
Norethisterone (0.5 to 3 mg/day) has been found to dose-dependently decrease circulating SHBG levels, which is a common property of androgens and is due to AR-mediated suppression of hepatic SHBG production.[47] The drug also has estrogenic activity, and estrogens are known to increase SHBG hepatic production and circulating levels, so it would appear that the androgenic activity of norethisterone overpowers its estrogenic activity in this regard.[47]
Norethisterone is bound to a considerable extent (36%) to SHBG in circulation.[11] Although it has lower affinity for SHBG than endogenous androgens and estrogens,[63] Norethisterone may displace testosterone from SHBG and thereby increase free testosterone levels, and this action may contribute to its weak androgenic effects.[64]
Estrogenic activity
[edit]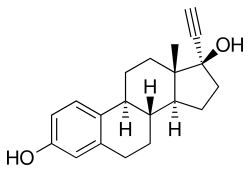
Norethisterone binds to the ERs, the ERα and the ERβ, with 0.07% and 0.01% of the relative binding affinity of estradiol.[65] Due to these very low relative affinities, it is essentially inactive itself as a ligand of the ERs at clinical concentrations.[11] However, norethisterone has been found to be a substrate for aromatase and is converted in the liver to a small extent (0.35%) to the highly potent estrogen ethinylestradiol (EE), and for this reason, unlike most other progestins, norethisterone has some estrogenic activity.[11] However, with typical dosages of norethisterone used in oral contraceptives (0.5 to 1 mg), the levels of EE produced are low, and it has been said that they are probably without clinical relevance.[11] Conversely, doses of 5 and 10 mg of norethisterone, which are used in the treatment of gynecological disorders, are converted at rates of 0.7% and 1.0% and produce levels of EE that correspond to those produced by 30 and 60 μg dosages of EE, respectively.[9][11] The levels of EE formed by 0.5 and 1 mg of norethisterone have been estimated based on higher dosages as corresponding to 2 and 10 μg dosages of EE, respectively.[9] At high doses, norethisterone may increase the risk of venous thromboembolism due to metabolism into EE.[66]
Neurosteroid activity
[edit]Like progesterone and testosterone, norethisterone is metabolized into 3,5-tetrahydro metabolites.[67] Whether these metabolites of norethisterone interact with the GABAA receptor similarly to the 3,5-tetrahydro metabolites of progesterone and testosterone like allopregnanolone and 3α-androstanediol, respectively, is a topic that does not appear to have been studied and hence requires clarification.[67]
Steroidogenesis inhibition
[edit]Norethisterone is a substrate for and is known to be an inhibitor of 5α-reductase, with 4.4% and 20.1% inhibition at 0.1 and 1 μM, respectively.[11] However, therapeutic concentrations of norethisterone are in the low nanomolar range, so this action may not be clinically relevant at typical dosages.[11]
Norethisterone and its major active metabolite 5α-DHNET have been found to act as irreversible aromatase inhibitors (Ki = 1.7 μM and 9.0 μM, respectively).[68] However, like the case of 5α-reductase, the concentrations required are probably too high to be clinically relevant at typical dosages.[11] 5α-DHNET specifically has been assessed and found to be selective in its inhibition of aromatase, and does not affect cholesterol side-chain cleavage enzyme (P450scc), 17α-hydroxylase/17,20-lyase, 21-hydroxylase, or 11β-hydroxylase.[68] Since it is not aromatized (and hence cannot be transformed into an estrogenic metabolite), unlike norethisterone, 5α-DHNET has been proposed as a potential therapeutic agent in the treatment of ER-positive breast cancer.[68]
Other activities
[edit]Norethisterone is a very weak inhibitor of CYP2C9 and CYP3A4 (IC50 = 46 μM and 51 μM, respectively), but these actions require very high concentrations of norethisterone that are far above therapeutic circulating levels (which are in the nanomolar range) and hence are probably not clinically relevant.[11]
Norethisterone and some of its 5α-reduced metabolites have been found to produce vasodilating effects in animals that are independent of sex steroid receptors and hence appear to be non-genomic in mechanism.[69]
Norethisterone stimulates the proliferation of MCF-7 breast cancer cells in vitro, an action that is independent of the classical PRs and is instead mediated via the progesterone receptor membrane component-1 (PGRMC1).[70] Certain other progestins act similarly in this assay, whereas progesterone acts neutrally.[70] It is unclear if these findings may explain the different risks of breast cancer observed with progesterone and progestins in clinical studies.[71]
Antigonadotropic effects
[edit]Due to its progestogenic activity, norethisterone suppresses the hypothalamic–pituitary–gonadal axis (HPG axis) and hence has antigonadotropic effects.[11][57] The estrogenic activity of norethisterone at high doses would also be expected to contribute to its antigonadotropic effects.[72] Due to its antigonadotropic effects, norethisterone suppresses gonadal sex hormone production, inhibits ovulation in women, and suppresses spermatogenesis in men.[11][57][73]
The ovulation-inhibiting dosage of both oral norethisterone and oral norethisterone acetate is about 0.5 mg/day in women.[11][74][75] However, some conflicting data exist, suggesting that higher doses might be necessary for full inhibition of ovulation.[76] An intramuscular injection of 200 mg norethisterone enanthate has been found to prevent ovulation and suppress levels of estradiol, progesterone, luteinizing hormone (LH), and follicle-stimulating hormone (FSH) in women.[77][78][79][80]
Early studies of oral norethisterone in men employing doses of 20 to 50 mg/day observed suppression of 17-ketosteroid excretion, increased estrogen excretion (due to conversion into ethinylestradiol), suppression of spermatogenesis, libido, and erectile function, and incidence of gynecomastia.[81][82][83][53][84] A dosage of oral norethisterone of 25 mg/day for 3 weeks in men has been reported to suppress testosterone levels by about 70%, to 100 to 200 ng/dL, within 4 or 5 days, as well as to suppress sperm count and to have no effect on libido or erectile function over this short time period.[85][86] In healthy young men, norethisterone acetate alone at a dose of 5 to 10 mg/day orally for 2 weeks suppressed testosterone levels from ~527 ng/dL to ~231 ng/dL (–56%).[87]

A single 200 mg intramuscular injection of norethisterone enanthate alone or in combination with 2 mg estradiol valerate has been found to produce a rapid, strong, and sustained decrease in gonadotropin and testosterone levels for up to one month in men.[73][89][90] Intramuscular injections of 200 mg norethisterone enanthate once every 3 weeks have also been found to suppress spermatogenesis in men.[81][91] Similarly, a single intramuscular injection of 50 mg norethisterone enanthate in combination with 5 mg estradiol valerate has been found to strongly suppress testosterone levels in men.[88] Levels of testosterone decreased from ~503 ng/dL at baseline to ~30 ng/dL at the lowest point (–94%) which occurred at day 7 post-injection.[88]
Pharmacokinetics
[edit]The pharmacokinetics of norethisterone have been reviewed.[11][92]
Absorption
[edit]The oral bioavailability of norethisterone is between 47 and 73%, with a mean oral bioavailability of 64%.[9][10] Micronization has been found to significantly improve the oral bioavailability of norethisterone by increasing intestinal absorption and reducing intestinal metabolism.[11][93] A single 2 mg oral dose of norethisterone has been found to result in peak circulating levels of the drug of 12 ng/mL (40 nmol/L), whereas a single 1 mg oral dose of norethisterone in combination with 2 mg estradiol resulted in peak levels of norethisterone of 8.5 ng/mL (29 nmol/L) one-hour post-administration.[11]
-
Norethisterone and ethinylestradiol levels over 24 hours after a single oral dose of 10 mg norethisterone acetate in postmenopausal women.[47]
-
Norethisterone and ethinylestradiol levels over 8 weeks after a single intramuscular injection of 200 mg norethisterone enanthate in premenopausal women.[94]
Distribution
[edit]The plasma protein binding of norethisterone is 97%.[11] It is bound 61% bound to albumin and 36% bound to SHBG.[11]
Metabolism
[edit]Metabolism of norethisterone and its prodrugs in humans
|
Norethisterone has an elimination half-life of 5.2 to 12.8 hours, with a mean elimination half-life of 8.0 hours.[9] The metabolism of norethisterone is very similar to that of testosterone (and nandrolone) and is mainly via reduction of the Δ4 double bond to 5α- and 5β-dihydronorethisterone, which is followed by the reduction of the C3 keto group to the four isomers of 3,5-tetrahydronorethisterone.[11] These transformations are catalyzed by 5α- and 5β-reductase and 3α- and 3β-hydroxysteroid dehydrogenase both in the liver and in extrahepatic tissues such as the pituitary gland, uterus, prostate gland, vagina, and breast.[103] With the exception of 3α,5α- and 3β,5α-tetrahydronorethisterone, which have significant affinity for the ER and are estrogenic to some degree, the 3,5-tetrahydro metabolites of norethisterone are inactive in terms of affinity for sex steroid receptors (specifically, the PR, AR, and ER).[104][105][106] A small amount of norethisterone is also converted by aromatase into EE.[9][11][54] Norethisterone is metabolized in the liver via hydroxylation as well, mainly by CYP3A4.[12] Some conjugation (including glucuronidation and sulfation)[103][107] of norethisterone and its metabolites occurs in spite of steric hindrance by the ethynyl group at C17α.[11] The ethynyl group of norethisterone is preserved in approximately 90% of all of its metabolites.[11]
Norethisterone is used in birth control pills, opposed to progesterone itself, because it is not metabolized as rapidly as progesterone when consumed orally. When progesterone is consumed orally it is rapidly metabolized in the gastrointestinal tract and the liver, and broken down into many different metabolites. Whereas, norethisterone is not as rapidly metabolized allowing norethisterone to be present in higher quantities allowing it to more effectively compete for progesterone receptor binding sites.[11]
Elimination
[edit]Norethisterone is eliminated 33 to 81% in urine and 35 to 43% in feces.[108]
Chemistry
[edit]Norethisterone, also known as 17α-ethynyl-19-nortestosterone or as 17α-ethynylestra-4-en-17β-ol-3-one, is a synthetic estrane steroid and a derivative of testosterone.[109][110] It is specifically a derivative of testosterone in which an ethynyl group has been added at the C17α position and the methyl group at the C19 position has been removed; hence, it is a combined derivative of ethisterone (17α-ethynyltestosterone) and nandrolone (19-nortestosterone).[109][110] These modifications result in increased progestogenic activity and oral bioavailability as well as decreased androgenic/anabolic activity.[111]
Derivatives
[edit]Norethisterone (NET) is the parent compound of a large group of progestins that includes most of the progestins known as the 19-nortestosterone derivatives.[112] This group is divided by chemical structure into the estranes (derivatives of norethisterone) and the gonanes (18-methylgonanes or 13β-ethylestranes; derivatives of levonorgestrel) and includes the following marketed medications:[113]
|
|
Several of these act as prodrugs of norethisterone, including norethisterone acetate, norethisterone enanthate, etynodiol diacetate, lynestrenol, and quingestanol acetate.[114][115][116] Noretynodrel may also be a prodrug of norethisterone.[11][9] Norethisterone acetate is taken by mouth similarly to norethisterone, while norethisterone enanthate is given by injection into muscle.[18]
Non-17α-ethynylated
[edit]19-Nortestosterone (19-NT) progestins which are technically not derivatives of norethisterone (as they do not have a C17α ethynyl group) but are still closely related (with other substitutions at the C17α and/or C16β positions) include the following marketed medications:[109][110]
- The C17α vinyl (ethenyl) derivatives norgesterone (17α-vinyl-δ5(10)-19-NT) and norvinisterone (17α-vinyl-19-NT)
- The C17α allyl derivatives allylestrenol (3-deketo-17α-allyl-19-NT) and altrenogest (17α-allyl-δ9,11-19-NT)
- The C17α alkyl derivative normethandrone (17α-methyl-19-NT)
- The C17α cyanomethyl derivative dienogest (17α-cyanomethyl-δ9-19-NT)
- The C16β ethyl derivative oxendolone (16β-ethyl-19-NT)
Many anabolic steroids of the 19-nortestosterone family, like norethandrolone and ethylestrenol, are also potent progestogens, but were never marketed as such.
Synthesis
[edit]Chemical syntheses of norethisterone have been published.[109][92]
Synthesis 1
[edit]
Estradiol 3-methyl ether (1, EME) is partially reduced to the 1,5-diene (2) as also occurs for the first step in the synthesis of nandrolone. Oppenauer oxidation then transforms the C17β hydroxyl group into a ketone functionality (3). This is then reacted with metal acetylide into the corresponding C17α ethynyl compound (4). Hydrolysis of the enol ether under mild conditions leads directly to (5),[117] which appears to be noretynodrel (although Lednicer states that it is "etynodrel" in his book (which may be a synonym etynodiol); etynodrel is with a chlorine atom attached), an orally active progestin. This is the progestogen component of the first oral contraceptive to be offered for sale (i.e., Enovid). Treatment of the ethynyl enol ether with strong acid leads to norethisterone (6).[19]
In practice, these and all other combined oral contraceptives are mixtures of 1 to 2% EE or mestranol and an oral progestin. It has been speculated that the discovery of the necessity of estrogen in addition to progestin for contraceptive efficacy is due to the presence of a small amount of unreduced EME (1) in early batches of 2. This when subjected to oxidation and ethynylation, would of course lead to mestranol (3). In any event, the need for the presence of estrogen in the mixture is now well established experimentally.
Synthesis 2
[edit]
Norethisterone is made from estr-4-ene-3,17-dione (bolandione), which in turn is synthesized by partial reduction of the aromatic region of the 3-O-methyl ether of estrone with lithium in liquid ammonia, and simultaneously of the keto group at C17α to a hydroxyl group, which is then oxidized back to a keto group by chromium trioxide in acetic acid. The conjugated C4-C5 olefin and the carbonyl group at C3 is then transformed to dienol ethyl ether using ethyl orthoformate. The obtained product is ethynylated by acetylene in the presence of potassium tert-butoxide. After hydrochloride hydrolysis of the formed O-potassium derivative, during which the enol ether is also hydrolyzed, and the remaining double bond is shifted, the desired norethisterone is obtained.
History
[edit]Norethisterone was synthesized for the first time by chemists Luis Miramontes, Carl Djerassi, and George Rosenkranz at Syntex in Mexico City in 1951.[19] It was derived from ethisterone, and was found to possess about 20-fold greater potency as a progestogen in comparison.[citation needed] Norethisterone was the first highly active oral progestogen to be synthesized, and was preceded (as a progestogen) by progesterone (1934), ethisterone (1938), 19-norprogesterone (1944), and 17α-methylprogesterone (1949) as well as by nandrolone (1950), whereas noretynodrel (1952) and norethandrolone (1953) followed the synthesis of norethisterone.[20][21] The drug was introduced as Norlutin in the United States in 1957.[22] Norethisterone was subsequently combined with mestranol and marketed as Ortho-Novum in the United States in 1963. It was the second progestin, after noretynodrel in 1960, to be used in an oral contraceptive.[21] In 1964, additional contraceptive preparations containing norethisterone in combination with mestranol or EE, such as Norlestrin and Norinyl, were marketed in the United States.[21]
Society and culture
[edit]Generic names
[edit]Norethisterone is the INN and BAN of the drug while norethindrone is its USAN.[109][110]
Brand names
[edit]Norethisterone is available in Bangladesh as Menogia (ACI), Normens (Renata) etc. Norethisterone (NET), including as norethisterone acetate and norethisterone enanthate, has been marketed under many brand names throughout the world.[110][28]
Availability
[edit]United States
[edit]Norethisterone was previously available alone in 5 mg tablets under the brand name Norlutin in the United States, but this formulation has since been discontinued.[123] However, norethisterone acetate remains available alone in 5 mg tablets under the brand name Aygestin in the United States.[123] It is one of the only non-contraceptive progestogen-only drug formulations that remains available in the United States.[123] The others include progesterone, medroxyprogesterone acetate, megestrol acetate, and hydroxyprogesterone caproate, as well as the atypical agent danazol.[123]
Both norethisterone and norethisterone acetate are also available in the United States as contraceptives.[123] Norethisterone is available both alone (brand names Camila, Errin, Heather, Micronor, Nor-QD, others) and in combination with EE (Norinyl, Ortho-Novum, others) or mestranol (Norinyl, Ortho-Novum, others), while norethisterone acetate is available only in combination with EE (Norlestrin, others).[123] Norethisterone enanthate is not available in the United States in any form.[123][124][125]
Research
[edit]Norethisterone, as norethisterone acetate and norethisterone enanthate, has been studied for use as a potential male hormonal contraceptive in combination with testosterone in men.[126][127]
Long-acting norethisterone microspheres for intramuscular injection have been studied for potential use in birth control.[128]
References
[edit]- ^ "Product monograph brand safety updates". Health Canada. 6 June 2024. Archived from the original on 29 March 2024. Retrieved 8 June 2024.
- ^ "Camila- norethindrone tablet". DailyMed. 1 April 2024. Retrieved 29 September 2024.
- ^ "Emzahh- norethindrone tablet". DailyMed. 10 April 2023. Retrieved 29 September 2024.
- ^ "Errin- norethindrone tablet". DailyMed. 1 March 2024. Retrieved 29 September 2024.
- ^ "Heather- norethindrone tablet". DailyMed. 31 August 2021. Retrieved 29 September 2024.
- ^ "Incassia- norethindrone tablet". DailyMed. 14 September 2021. Retrieved 29 September 2024.
- ^ "Jencycla- norethindrone tablet". DailyMed. 13 December 2023. Retrieved 29 September 2024.
- ^ a b c "Micronor- norethindrone tablet". DailyMed. 1 April 2011. Retrieved 29 September 2024.
- ^ a b c d e f g h Stanczyk FZ (September 2002). "Pharmacokinetics and potency of progestins used for hormone replacement therapy and contraception". Reviews in Endocrine & Metabolic Disorders. 3 (3): 211–24. doi:10.1023/A:1020072325818. PMID 12215716. S2CID 27018468.
- ^ a b Fotherby K (August 1996). "Bioavailability of orally administered sex steroids used in oral contraception and hormone replacement therapy". Contraception. 54 (2): 59–69. doi:10.1016/0010-7824(96)00136-9. PMID 8842581.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab ac ad ae af ag ah ai aj ak al am an Kuhl H (August 2005). "Pharmacology of estrogens and progestogens: influence of different routes of administration" (PDF). Climacteric. 8 (Suppl 1): 3–63. doi:10.1080/13697130500148875. PMID 16112947. S2CID 24616324. Archived (PDF) from the original on 22 August 2016. Retrieved 6 September 2018.
- ^ a b c d Korhonen T, Turpeinen M, Tolonen A, Laine K, Pelkonen O (May 2008). "Identification of the human cytochrome P450 enzymes involved in the in vitro biotransformation of lynestrenol and norethindrone". The Journal of Steroid Biochemistry and Molecular Biology. 110 (1–2): 56–66. doi:10.1016/j.jsbmb.2007.09.025. PMID 18356043. S2CID 10809537.
- ^ a b c d Taitel HF, Kafrissen ME (1995). "Norethindrone – a review of therapeutic applications". International Journal of Fertility and Menopausal Studies. 40 (4): 207–23. PMID 8520623.
- ^ Alden KR, Lowdermilk DL, Cashion MC, Perry SE (2013). Maternity and Women's Health Care – E-Book. Elsevier Health Sciences. pp. 135–. ISBN 978-0-323-29368-6. Archived from the original on 9 March 2023. Retrieved 8 January 2018.
- ^ a b Kuhl H (September 1990). "Pharmacokinetics of oestrogens and progestogens". Maturitas. 12 (3): 171–97. doi:10.1016/0378-5122(90)90003-o. PMID 2170822.
- ^ "Aygestin (norethindrone acetate tablets, USP)" (PDF). Archived from the original (PDF) on 10 February 2017. Retrieved 11 July 2024.
- ^ a b c d e f g Jacobson BD (October 1962). "Hazards of norethindrone therapy during pregnancy". American Journal of Obstetrics and Gynecology. 84 (7): 962–68. doi:10.1016/0002-9378(62)90075-3. PMID 14450719.
- ^ a b c d IARC Working Group on the Evaluation of Carcinogenic Risks to Humans, World Health Organization, International Agency for Research on Cancer (2007). Combined Estrogen-progestogen Contraceptives and Combined Estrogen-progestogen Menopausal Therapy. World Health Organization. pp. 417–. ISBN 978-92-832-1291-1. Archived from the original on 10 January 2023. Retrieved 12 October 2016.
Norethisterone and its acetate and enanthate esters are progestogens that have weak estrogenic and androgenic properties.
- ^ a b c d Djerassi C, Miramontes L, Rosenkranz G, Sondheimer F, Longo LD (January 2006). "Steroids LIV. Synthesis of 19-nor-17alpha-ethynyltestosterone and 19-nor-17alpha-methyltestosterone. 1954". American Journal of Obstetrics and Gynecology. 194 (1): 289; discussion 290. doi:10.1021/ja01645a010. PMID 16389045.
- ^ a b Shoupe D (2007). The Handbook of Contraception: A Guide for Practical Management. Springer Science & Business Media. pp. 15–. ISBN 978-1-59745-150-5.
- ^ a b c d e Marks L (2010). Sexual Chemistry: A History of the Contraceptive Pill. Yale University Press. pp. 74, 76. ISBN 978-0-300-16791-7.
- ^ a b William Andrew Publishing (2013). Pharmaceutical Manufacturing Encyclopedia (3rd ed.). Elsevier. pp. 2935–. ISBN 978-0-8155-1856-3.
- ^ Hatcher RA, Nelson AL (2007). Contraceptive Technology. Ardent Media. pp. 195–. ISBN 978-1-59708-001-9. Archived from the original on 10 January 2023. Retrieved 8 January 2018.
- ^ Gunasheela S (2011). Practical Management of Gynecological Problems. JP Medical Ltd. pp. 31–. ISBN 978-93-5025-240-6. Archived from the original on 9 March 2023. Retrieved 8 January 2018.
- ^ Grimes DA, Lopez LM, O'Brien PA, Raymond EG (November 2013). "Progestin-only pills for contraception". The Cochrane Database of Systematic Reviews (11) CD007541. doi:10.1002/14651858.CD007541.pub3. PMC 11975192. PMID 24226383.
- ^ Hussain SF (February 2004). "Progestogen-only pills and high blood pressure: is there an association? A literature review". Contraception. 69 (2): 89–97. doi:10.1016/j.contraception.2003.09.002. PMID 14759612.
- ^ "Opill: Package Insert / Prescribing Information". Drugs.com. Retrieved 30 September 2024.
- ^ a b "Norethisterone". Archived from the original on 15 September 2018. Retrieved 8 January 2018.
- ^ "Generic Aygestin Availability". Archived from the original on 24 August 2018. Retrieved 8 January 2018.
- ^ "Top 300 of 2023". ClinCalc. Archived from the original on 12 August 2025. Retrieved 12 August 2025.
- ^ "Norethindrone Drug Usage Statistics, United States, 2013–2023". ClinCalc. Retrieved 18 August 2025.
- ^ World Health Organization (2023). The selection and use of essential medicines 2023: web annex A: World Health Organization model list of essential medicines: 23rd list. Geneva: World Health Organization. hdl:10665/371090. WHO/MHP/HPS/EML/2023.02.
- ^ Kim JJ, Kurita T, Bulun SE (February 2013). "Progesterone action in endometrial cancer, endometriosis, uterine fibroids, and breast cancer". Endocrine Reviews. 34 (1): 130–62. doi:10.1210/er.2012-1043. PMC 3565104. PMID 23303565.
- ^ "Norethisterone". Drugs.com.
- ^ "Drugs@FDA: FDA Approved Drug Products". United States Food and Drug Administration. Archived from the original on 16 November 2016. Retrieved 27 November 2016.
- ^ Index Nominum 2000: International Drug Directory. Taylor & Francis. January 2000. pp. 749–. ISBN 978-3-88763-075-1.
- ^ IARC Working Group on the Evaluation of Carcinogenic Risks to Humans, International Agency for Research on Cancer (1 January 1999). Hormonal Contraception and Post-menopausal Hormonal Therapy (PDF). IARC. p. 65. ISBN 978-92-832-1272-0.
- ^ a b c d e Aronson JK (2009). Meyler's Side Effects of Endocrine and Metabolic Drugs. Elsevier. pp. 217, 253, 275 [217]. ISBN 978-0-08-093292-7.
- ^ Hägglund H, Remberger M, Klaesson S, Lönnqvist B, Ljungman P, Ringdén O (December 1998). "Norethisterone treatment, a major risk-factor for veno-occlusive disease in the liver after allogeneic bone marrow transplantation". Blood. 92 (12): 4568–72. doi:10.1182/blood.V92.12.4568. PMID 9845522.
- ^ a b Cornia PB, Anawalt BD (November 2004). "Male hormonal contraception". Expert Opinion on Emerging Drugs. 9 (2): 335–44. doi:10.1517/14728214.9.2.335. PMID 15571489. S2CID 26886374.
- ^ a b Cornia PB, Anawalt BD (2005). "Male hormonal contraceptives: a potentially patentable and profitable product". Expert Opinion on Therapeutic Patents. 15 (12): 1727–37. doi:10.1517/13543776.15.12.1727. ISSN 1354-3776. S2CID 83941717.
- ^ a b c Kamischke A, Heuermann T, Krüger K, von Eckardstein S, Schellschmidt I, Rübig A, et al. (February 2002). "An effective hormonal male contraceptive using testosterone undecanoate with oral or injectable norethisterone preparations". The Journal of Clinical Endocrinology and Metabolism. 87 (2): 530–39. doi:10.1210/jcem.87.2.8218. PMID 11836281.
- ^ a b Junkins-Hopkins JM (March 2010). "Hormone therapy for acne". Journal of the American Academy of Dermatology. 62 (3): 486–88. doi:10.1016/j.jaad.2009.12.002. PMID 20159314.
- ^ a b Arowojolu AO, Gallo MF, Lopez LM, Grimes DA (July 2012). Arowojolu AO (ed.). "Combined oral contraceptive pills for treatment of acne". The Cochrane Database of Systematic Reviews (7) CD004425. doi:10.1002/14651858.CD004425.pub6. PMC 11437354. PMID 22786490.
- ^ van Vloten WA, Sigurdsson V (2004). "Selecting an oral contraceptive agent for the treatment of acne in women". American Journal of Clinical Dermatology. 5 (6): 435–41. doi:10.2165/00128071-200405060-00008. PMID 15663340. S2CID 9947402.
- ^ a b Pochi PE, Strauss JS (December 1965). "Lack of androgen effect on human sebaceous glands with low-dosage norethindrone". American Journal of Obstetrics and Gynecology. 93 (7): 1002–04. doi:10.1016/0002-9378(65)90162-6. PMID 5843402.
- ^ a b c d Kuhnz W, Heuner A, Hümpel M, Seifert W, Michaelis K (December 1997). "In vivo conversion of norethisterone and norethisterone acetate to ethinyl etradiol in postmenopausal women". Contraception. 56 (6): 379–85. doi:10.1016/s0010-7824(97)00174-1. PMID 9494772.
- ^ a b Curwen S (1962). "Virilization with Norethisterone". BMJ. 1 (5289): 1415. doi:10.1136/bmj.1.5289.1415-a. ISSN 0959-8138. PMC 1958463.
- ^ a b c d Roxburgh DR, West MJ (August 1973). "The use of norethisterone to suppress menstruation in the intellectually severely retarded woman". The Medical Journal of Australia. 2 (7): 310–13. doi:10.5694/j.1326-5377.1973.tb128175.x. PMID 4746398. S2CID 204094551. Archived from the original on 20 December 2016. Retrieved 6 December 2016.
- ^ a b c Roxburgh DR, West MJ (August 1973). "The use of norethisterone to suppress menstruation in the intellectually severely retarded woman". The Medical Journal of Australia. 2 (7): 310–13. doi:10.1097/00006254-197408000-00021. PMID 4746398.
- ^ Board JA (April 1965). "Clinical Evaluation of the Oral Contraceptive Use of Norethindrone 5 Mg. Plus Mestranol 0.075 Mg". Canadian Medical Association Journal. 92 (15): 814–17. PMC 1927985. PMID 14272499.
- ^ Kaser DJ, Missmer SA, Berry KF, Laufer MR (April 2012). "Use of norethindrone acetate alone for postoperative suppression of endometriosis symptoms". Journal of Pediatric and Adolescent Gynecology. 25 (2): 105–08. doi:10.1016/j.jpag.2011.09.013. PMID 22154396.
- ^ a b Paulsen CA, Leach RB, Lanman J, Goldston N, Maddock WO, Heller CG (October 1962). "Inherent estrogenicity of norethindrone and norethynodrel: comparison with other synthetic progestins and progesterone". The Journal of Clinical Endocrinology and Metabolism. 22 (10): 1033–39. doi:10.1210/jcem-22-10-1033. PMID 13942007.
- ^ a b Chu MC, Zhang X, Gentzschein E, Stanczyk FZ, Lobo RA (June 2007). "Formation of ethinyl estradiol in women during treatment with norethindrone acetate". The Journal of Clinical Endocrinology and Metabolism. 92 (6): 2205–07. doi:10.1210/jc.2007-0044. PMID 17341557.
- ^ Connolly A, Britton AG (2017). Women's Health in Primary Care. Cambridge University Press. pp. 153–. ISBN 978-1-108-16595-2.
- ^ a b Farris M, Bastianelli C, Rosato E, Brosens I, Benagiano G (October 2017). "Pharmacodynamics of combined estrogen-progestin oral contraceptives: 2. effects on hemostasis". Expert Review of Clinical Pharmacology. 10 (10): 1129–44. doi:10.1080/17512433.2017.1356718. PMID 28712325. S2CID 205931204.
- ^ a b c d e Kuhl H (2011). "Pharmacology of Progestogens" (PDF). J Reproduktionsmed Endokrinol. 8 (1): 157–77. Archived (PDF) from the original on 11 October 2016. Retrieved 10 October 2016.
- ^ Chu YH, Li QA, Zhao ZF, Zhou YP, Cao DC (June 1985). "[Antiprogestational action of 5 alpha-dihydronorethisterone]". Zhongguo Yao Li Xue Bao = Acta Pharmacologica Sinica (in Chinese). 6 (2): 125–29. PMID 2934946.
- ^ McCuistion LE, Kee JL, Hayes ER (2014). Pharmacology: A Patient-Centered Nursing Process Approach. Elsevier Health Sciences. pp. 846–. ISBN 978-0-323-29348-8.
- ^ Greenblatt RB (July 1956). "The progestational activity of 17-alpha-ethinyl-19-nortestosterone". The Journal of Clinical Endocrinology and Metabolism. 16 (7): 869–75. doi:10.1210/jcem-16-7-869. PMID 13332050.
- ^ Fragkaki AG, Angelis YS, Koupparis M, Tsantili-Kakoulidou A, Kokotos G, Georgakopoulos C (February 2009). "Structural characteristics of anabolic androgenic steroids contributing to binding to the androgen receptor and to their anabolic and androgenic activities. Applied modifications in the steroidal structure". Steroids. 74 (2): 172–97. doi:10.1016/j.steroids.2008.10.016. PMID 19028512. S2CID 41356223.
Many synthetic steroids with high myotrophic activity exhibit myotrophic–androgenic dissociation, since, due to changes introduced in the structure of ring A, they will probably not be substrates for the 5α-reductases [85]. 5α-Reduction does not always amplify the androgenic potency in spite of high RBA of androgens to the AR. This is the case for norethisterone (Fig. 1, 34), a synthetic 19-nor-17α-ethynyl testosterone derivative, which also undergoes enzyme-mediated 5α-reduction and exerts potent androgenic effects in target organs. 5α-Reduced norethisterone displays a higher AR binding but shows a significantly lower androgenic potency than unchanged norethisterone [102, 103].
- ^ a b c Lemus AE, Enríquez J, García GA, Grillasca I, Pérez-Palacios G (January 1997). "5alpha-reduction of norethisterone enhances its binding affinity for androgen receptors but diminishes its androgenic potency". The Journal of Steroid Biochemistry and Molecular Biology. 60 (1–2): 121–29. doi:10.1016/s0960-0760(96)00172-0. PMID 9182866. S2CID 33771349.
- ^ Filshie M, Guillebaud J (2013). Contraception: Science and Practice. Elsevier Science. pp. 26–. ISBN 978-1-4831-6366-6.
Norethisterone binds to SHBG with less affinity than endogenous androgens and oestrogens [...]
- ^ Azziz R (2007). Androgen Excess Disorders in Women. Springer Science & Business Media. pp. 124–. ISBN 978-1-59745-179-6.
- ^ Kuiper GG, Carlsson B, Grandien K, Enmark E, Häggblad J, Nilsson S, et al. (March 1997). "Comparison of the ligand binding specificity and transcript tissue distribution of estrogen receptors alpha and beta". Endocrinology. 138 (3): 863–70. doi:10.1210/endo.138.3.4979. PMID 9048584.
- ^ Wiegratz I, Kuhl H (September 2006). "Metabolic and clinical effects of progestogens". The European Journal of Contraception & Reproductive Health Care. 11 (3): 153–61. doi:10.1080/13625180600772741. PMID 17056444. S2CID 27088428.
- ^ a b Giatti S, Melcangi RC, Pesaresi M (August 2016). "The other side of progestins: effects in the brain". Journal of Molecular Endocrinology. 57 (2): R109–26. doi:10.1530/JME-16-0061. PMID 27339142.
- ^ a b c Yamamoto T, Tamura T, Kitawaki J, Osawa Y, Okada H (June 1994). "Suicide inactivation of aromatase in human placenta and uterine leiomyoma by 5 alpha-dihydronorethindrone, a metabolite of norethindrone, and its effect on steroid-producing enzymes". European Journal of Endocrinology. 130 (6): 634–40. doi:10.1530/eje.0.1300634. PMID 8205267.
- ^ Perusquía M, Villalón CM, Navarrete E, García GA, Pérez-Palacios G, Lemus AE (August 2003). "Vasodilating effect of norethisterone and its 5 alpha metabolites: a novel nongenomic action". European Journal of Pharmacology. 475 (1–3): 161–69. doi:10.1016/s0014-2999(03)02106-x. PMID 12954372.
- ^ a b Neubauer H, Ma Q, Zhou J, Yu Q, Ruan X, Seeger H, et al. (October 2013). "Possible role of PGRMC1 in breast cancer development". Climacteric. 16 (5): 509–13. doi:10.3109/13697137.2013.800038. PMID 23758160. S2CID 29808177.
{{cite journal}}: CS1 maint: overridden setting (link) - ^ Trabert B, Sherman ME, Kannan N, Stanczyk FZ (April 2020). "Progesterone and Breast Cancer". Endocrine Reviews. 41 (2): 320–44. doi:10.1210/endrev/bnz001. PMC 7156851. PMID 31512725.
- ^ Anderson RA, Baird DT (December 2002). "Male contraception" (PDF). Endocrine Reviews. 23 (6): 735–62. doi:10.1210/er.2002-0002. PMID 12466187. Archived (PDF) from the original on 28 August 2021. Retrieved 11 December 2019.
- ^ a b Kamischke A, Nieschlag E (January 2004). "Progress towards hormonal male contraception". Trends in Pharmacological Sciences. 25 (1): 49–57. doi:10.1016/j.tips.2003.11.009. PMID 14723979.
- ^ Rudel HW (September 1968). "Pharmacology of oral contraceptives". Clinical Obstetrics and Gynecology. 11 (3): 632–44. doi:10.1097/00003081-196811030-00002. PMID 4878826.
- ^ Stanczyk FZ (November 2003). "All progestins are not created equal". Steroids. 68 (10–13): 879–90. doi:10.1016/j.steroids.2003.08.003. PMID 14667980. S2CID 44601264.
- ^ Endrikat J, Gerlinger C, Richard S, Rosenbaum P, Düsterberg B (December 2011). "Ovulation inhibition doses of progestins: a systematic review of the available literature and of marketed preparations worldwide". Contraception. 84 (6): 549–57. doi:10.1016/j.contraception.2011.04.009. PMID 22078182.
- ^ Shoupe D (1993). "Injectable Contraceptives and Contraceptive Vaginal Rings". Contraception. Clinical Perspectives in Obstetrics and Gynecology. Springer. pp. 144–57. doi:10.1007/978-1-4612-2730-4_13. ISBN 978-1-4612-7645-6. ISSN 0178-0328.
- ^ Weiner E, Johansson ED (April 1975). "Plasma levels of norethindrone after i.m. injection of 200 mg norethindrone enanthate". Contraception. 11 (4): 419–25. doi:10.1016/0010-7824(75)90004-9. PMID 1122756.
- ^ Fotherby K, Howard G, Shrimanker K, Elder M, Bye PG (December 1977). "Effect of norethisterone oenanthate on serum gonadotrophin levels". Contraception. 16 (6): 591–604. doi:10.1016/0010-7824(77)90060-9. PMID 606499.
- ^ Goebelsmann U, Stanczyk FZ, Brenner PF, Goebelsmann AE, Gentzschein EK, Mishell DR (March 1979). "Serum norethindrone (NET) concentrations following intramuscular NET enanthate injection. Effect upon serum LH, FSH, estradiol and progesterone". Contraception. 19 (3): 283–313. doi:10.1016/0010-7824(79)90022-2. PMID 572279.
- ^ a b Neumann F, Diallo FA, Hasan SH, Schenck B, Traore I (1976). "The influence of pharmaceutical compounds on male fertility". Andrologia. 8 (3): 203–35. doi:10.1111/j.1439-0272.1976.tb02137.x. PMID 793446. S2CID 24859886.
- ^ Heller CG, Laidlaw WM, Harvey HT, Nelson WO (July 1958). "Effects of progestational compounds on the reproductive processes of the human male". Annals of the New York Academy of Sciences. 71 (5): 649–65. doi:10.1111/j.1749-6632.1958.tb54641.x. PMID 13583821. S2CID 32637425.
- ^ Heller CG, Moore DJ, Paulsen CA, Nelson WO, Laidlaw WM (December 1959). "Effects of progesterone and synthetic progestins on the reproductive physiology of normal men". Federation Proceedings. 18: 1057–65. PMID 14400846. Archived from the original on 18 December 2018. Retrieved 11 December 2019.
- ^ Paulsen CA (March 1965). "Progestin Metabolism: Special Reference to Estrogenic Pathways". Metabolism. 14 (3): SUPPL:313–19. doi:10.1016/0026-0495(65)90018-1. PMID 14261416.
- ^ Moudgal NR, Suresh R (1995). "Some thoughts on development of chemically based male contraceptives" (PDF). Current Science (Bangalore). 68 (4): 470–74. ISSN 0011-3891. Archived from the original (PDF) on 11 December 2019. Retrieved 11 December 2019.
- ^ Johonsson ED, Nygren KG (1973). "Depression of plasma testosterone levels in men with norethindrone". Contraception. 8 (3): 219–26. doi:10.1016/0010-7824(73)90032-2. ISSN 0010-7824.
- ^ Zitzmann M, Rohayem J, Raidt J, Kliesch S, Kumar N, Sitruk-Ware R, et al. (May 2017). "Impact of various progestins with or without transdermal testosterone on gonadotropin levels for non-invasive hormonal male contraception: a randomized clinical trial". Andrology. 5 (3): 516–26. doi:10.1111/andr.12328. PMID 28189123. S2CID 41502711.
- ^ a b c d Alvarez BD (11 May 2011). Efecto de una Dosis de 50 mg de Enantato de Noretisterona y 5 mg de Valerato de Estradiol en los Niveles de Testosterona Total en Hombres Mexicanos Sanos [Effect of a Dose of 50 mg of Norethisterone Enanthate and 5 mg of Estradiol Valerate on Total Testosterone Levels in Healthy Mexican Men] (MSc). National Polytechnic Institute of Mexico. Archived from the original on 16 September 2022. Retrieved 12 September 2022.
- ^ Amory JK (2003). "Androgens and Male Contraception". Androgens in Health and Disease. Contemporary Endocrinology. Humana Press. pp. 405–17. doi:10.1007/978-1-59259-388-0_21. ISBN 978-1-61737-314-5.
- ^ Kamischke A, Diebäcker J, Nieschlag E (September 2000). "Potential of norethisterone enanthate for male contraception: pharmacokinetics and suppression of pituitary and gonadal function". Clinical Endocrinology. 53 (3): 351–58. doi:10.1046/j.1365-2265.2000.01097.x. PMID 10971453. S2CID 70515136.
- ^ Petry R, Mauss J, Senge T, Rausch-Stroomann JG (1970). "Über den Einflu#x00DF; von Cyproteronacetat, Norethisteron#x00F6;nanthat und Gestonoroncapronat auf die Hypophysen-Gonadenachse beim Mann". Endokrinologie der Entwicklung und Reifung [Influence of Cyproterone-acetate, Norethisterone-enanthate and Gestonorone-capronate on the Hypophyseal-Gonadal-Axis in the Male]. Symposion der Deutschen Gesellschaft für Endokrinologie in Ulm vom 26–28 Februar 1970. Springer. pp. 428–30. doi:10.1007/978-3-642-80591-2_118. ISBN 978-3-642-80591-2.
- ^ a b Die Gestagene. Springer-Verlag. 2013. pp. 13–14, 283–84. ISBN 978-3-642-99941-3. Archived from the original on 10 January 2023. Retrieved 19 September 2018.
- ^ Saperstein S, Edgren RA, Jung D, Mroszczak EJ, Lee GJ, Dorr A, et al. (December 1989). "Pharmacokinetics of norethindrone: effect of particle size". Contraception. 40 (6): 731–40. doi:10.1016/0010-7824(89)90075-9. PMID 2620531.
- ^ Friedrich C, Berse M, Klein S, Rohde B, Höchel J (June 2018). "In Vivo Formation of Ethinylestradiol After Intramuscular Administration of Norethisterone Enantate". Journal of Clinical Pharmacology. 58 (6): 781–89. doi:10.1002/jcph.1079. PMID 29522253. S2CID 3813229.
- ^ Thijssen JH (1972). "Metabolism of Orally Active Synthetic Progestational Compounds". In Tausk M (ed.). Pharmacology of the Endocrine System and Related Drugs: Progesterone, Progestational Drugs and Antifertility Agents. Vol. II. Pergamon Press. pp. 217–73. ISBN 978-0-08-016812-8. OCLC 278011135.
- ^ Okada H (2010). "Receptors and Mechanism Action of Synthetic Progestogens". Asia-Oceania Journal of Obstetrics and Gynaecology. 7 (1): 15–27. doi:10.1111/j.1447-0756.1981.tb00511.x. ISSN 0389-2328.
- ^ Briggs MH (1980). "Comparative Pharmacodynamics and Pharmacokinetics of Contraceptive Steroids in Animals and Man: A Selective Review". Clinical Pharmacology & Therapeutics. Palgrave Macmillan UK. pp. 493–518. doi:10.1007/978-1-349-05952-2_57. ISBN 978-1-349-05954-6.
- ^ Thomas JA, Keenan EJ (1986). "Progestins and Oral Contraceptives". Principles of Endocrine Pharmacology. Springer. pp. 167–96. doi:10.1007/978-1-4684-5036-1_8. ISBN 978-1-4684-5036-1.
- ^ Orme ML, Back DJ, Breckenridge AM (1983). "Clinical pharmacokinetics of oral contraceptive steroids". Clinical Pharmacokinetics. 8 (2): 95–136. doi:10.2165/00003088-198308020-00001. PMID 6342899. S2CID 43298472.
- ^ Fotherby K (1974). "Metabolism of synthetic steroids by animals and man". Acta Endocrinologica. Supplementum. 185: 119–47. doi:10.1530/acta.0.075s119. PMID 4206183.
- ^ Kuhl H, Wiegratz I (August 2007). "Can 19-nortestosterone derivatives be aromatized in the liver of adult humans? Are there clinical implications?". Climacteric. 10 (4): 344–53. doi:10.1080/13697130701380434. PMID 17653961. S2CID 20759583.
- ^ Stanczyk FZ, Roy S (July 1990). "Metabolism of levonorgestrel, norethindrone, and structurally related contraceptive steroids". Contraception. 42 (1): 67–96. doi:10.1016/0010-7824(90)90093-B. PMID 2143719.
- ^ a b Schoonen WG, Deckers GH, de Gooijer ME, de Ries R, Kloosterboer HJ (November 2000). "Hormonal properties of norethisterone, 7alpha-methyl-norethisterone and their derivatives". The Journal of Steroid Biochemistry and Molecular Biology. 74 (4): 213–22. doi:10.1016/s0960-0760(00)00125-4. PMID 11162927. S2CID 19797254.
[...] several mono- and disulphated as well as mono- and diglucuronidated metabolites of NET have been detected in urine from NET treated women [16,17]. In unconjugated form these NET (or MeNET) metabolites are represented by 5α- and 5β-reduced NET (5α-NET or 5β-NET) and by 3α- and 3β-hydrogenated 5α-NET and 5β-NET, leading to 3α,5α-NET, 3β,5α-NET, 3α,5β-NET and 3β,5β-NET or their corresponding MeNET metabolites (Figs. 1 and 2). These steroid conversions of NET or MeNET may take place in the liver, but also in the pituitary, endometrium, prostate, vagina and breast. The enzymes involved in these metabolic processes are 5α- and 5β-reductase as well as 3α- and 3β-hydroxysteroid dehydrogenase (HSD).
- ^ Chávez BA, Vilchis F, Pérez AE, García GA, Grillasca I, Pérez-Palacios G (January 1985). "Stereospecificity of the intracellular binding of norethisterone and its A-ring reduced metabolites". Journal of Steroid Biochemistry. 22 (1): 121–26. doi:10.1016/0022-4731(85)90151-7. PMID 3871879.
- ^ Garza-Flores J, Vilchis F, García GA, Menjívar M, Pérez-Palacios G (June 1986). "A-ring reduction enhances the antigonadotropic potency of norethisterone". Acta Endocrinologica. 112 (2): 278–83. doi:10.1530/acta.0.1120278. PMID 3090814.
- ^ Lemus AE, Enríquez J, Hernández A, Santillán R, Pérez-Palacios G (February 2009). "Bioconversion of norethisterone, a progesterone receptor agonist into estrogen receptor agonists in osteoblastic cells". The Journal of Endocrinology. 200 (2): 199–206. doi:10.1677/JOE-08-0166. PMID 19008332.
- ^ Scarsi KK, Darin KM, Chappell CA, Nitz SM, Lamorde M (November 2016). "Drug-Drug Interactions, Effectiveness, and Safety of Hormonal Contraceptives in Women Living with HIV". Drug Safety. 39 (11): 1053–72. doi:10.1007/s40264-016-0452-7. PMC 5048570. PMID 27562873.
- ^ DeGroot LJ (2001). Endocrinology. W.B. Saunders Co. p. 2617. ISBN 978-0-7216-7843-6.
- ^ a b c d e Elks J (2014). The Dictionary of Drugs: Chemical Data: Chemical Data, Structures and Bibliographies. Springer. pp. 886–. ISBN 978-1-4757-2085-3. Archived from the original on 10 January 2023. Retrieved 5 October 2016.
- ^ a b c d e Index Nominum 2000: International Drug Directory. Taylor & Francis. 2000. pp. 749–. ISBN 978-3-88763-075-1.
- ^ Chwalisz K, Surrey E, Stanczyk FZ (June 2012). "The hormonal profile of norethindrone acetate: rationale for add-back therapy with gonadotropin-releasing hormone agonists in women with endometriosis". Reproductive Sciences. 19 (6): 563–71. doi:10.1177/1933719112438061. PMID 22457429. S2CID 2882899.
- ^ Shoupe D, Haseltine FP (2012). Contraception. Springer Science & Business Media. pp. 112–. ISBN 978-1-4612-2730-4.
- ^ Ryan KJ (1999). Kistner's Gynecology and Women's Health. Mosby. p. 292. ISBN 978-0-323-00201-1.
- ^ Hammerstein J (December 1990). "Prodrugs: advantage or disadvantage?". American Journal of Obstetrics and Gynecology. 163 (6 Pt 2): 2198–203. doi:10.1016/0002-9378(90)90561-K. PMID 2256526.
- ^ Edelman AB, Cherala G, Stanczyk FZ (October 2010). "Metabolism and pharmacokinetics of contraceptive steroids in obese women: a review". Contraception. 82 (4): 314–23. doi:10.1016/j.contraception.2010.04.016. PMID 20851224.
- ^ Raynaud JP, Ojasoo T (November 1986). "The design and use of sex-steroid antagonists". Journal of Steroid Biochemistry. 25 (5B): 811–33. doi:10.1016/0022-4731(86)90313-4. PMID 3543501.
Similar androgenic potential is inherent to norethisterone and its prodrugs (norethisterone acetate, ethynodiol diacetate, lynestrenol, norethynodrel, quingestanol [acetate]).
- ^ a b Frank B. Colton, U.S. patent 2,655,518 (1952 to Searle & Co).
- ^ Ringold HJ, Rosenkranz G, Sondheimer F (1956). "Steroids. LXXX.11-Methyl-19-nortestosterone and 1-Methyl-17α-ethinyl-19-nortestosterone". Journal of the American Chemical Society. 78 (11): 2477–79. Bibcode:1956JAChS..78.2477R. doi:10.1021/ja01592a037.
- ^ Ueberwasser H, Heusler K, Kalvoda J, Meystre C, Wieland P, Anner G, et al. (1963). "19-Norsteroide II. Ein einfaches Herstellungsverfahren für 19-Norandrostan-Derivate. über Steroide, 193. Mitteilung". Helvetica Chimica Acta. 46: 344–52. doi:10.1002/hlca.19630460135.
- ^ Onken D, Heublein D (January 1970). "[Ethinylated steroids]". Die Pharmazie. 25 (1): 3–9. PMID 4914401.
- ^ U.S. patent 2,744,122
- ^ U.S. patent 2,774,777
- ^ a b c d e f g "Drugs FDA: FDA Approved Drug Products". United States Food and Drug Administration. Archived from the original on 16 November 2016. Retrieved 27 November 2016.
- ^ Bullough VL (2001). Encyclopedia of Birth Control. ABC-CLIO. pp. 145–. ISBN 978-1-57607-181-6. Archived from the original on 10 January 2023. Retrieved 27 November 2016.
- ^ Moskowitz EH, Jennings B (1996). Coerced Contraception?: Moral and Policy Challenges of Long Acting Birth Control. Georgetown University Press. pp. 40–. ISBN 978-1-58901-807-5.
- ^ Nieschlag E (November 2010). "Clinical trials in male hormonal contraception" (PDF). Contraception. 82 (5): 457–70. doi:10.1016/j.contraception.2010.03.020. PMID 20933120. Archived (PDF) from the original on 5 December 2020. Retrieved 28 December 2018.
- ^ Nieschlag E, Behre HM, Nieschlag E, Behre HM, Nieschlag S (2012). Nieschlag E, Behre HM, Nieschlag S (eds.). "The essential role of testosterone in hormonal male contraception". Testosterone: 470–93. doi:10.1017/CBO9781139003353.023. ISBN 978-1-139-00335-3.
- ^ Benagiano G, Primiero FM (June 1983). "Long acting contraceptives. Present status". Drugs. 25 (6): 570–609. doi:10.2165/00003495-198325060-00003. PMID 6223801. S2CID 45898359.
Further reading
[edit]- Brogden RN, Speight TM, Avery GS (1973). "Progestagen-only oral contraceptives: a preliminary report of the action and clinical use of norgestrel and norethisterone". Drugs. 6 (3): 169–81. doi:10.2165/00003495-197306030-00004. PMID 4130566. S2CID 42295736.
- "Norethisterone and norethisterone acetate". IARC Monographs on the Evaluation of the Carcinogenic Risk of Chemicals to Humans. 21: 441–60. December 1979. PMID 120838.
- Stanczyk FZ, Roy S (July 1990). "Metabolism of levonorgestrel, norethindrone, and structurally related contraceptive steroids". Contraception. 42 (1): 67–96. doi:10.1016/0010-7824(90)90093-b. PMID 2143719.
- Wiseman LR, McTavish D (March 1994). "Transdermal estradiol/norethisterone. A review of its pharmacological properties and clinical use in postmenopausal women". Drugs & Aging. 4 (3): 238–56. doi:10.2165/00002512-199404030-00006. PMID 8199397. S2CID 68007924.
- Taitel HF, Kafrissen ME (1995). "Norethindrone – a review of therapeutic applications". International Journal of Fertility and Menopausal Studies. 40 (4): 207–23. PMID 8520623.
- Maier WE, Herman JR (August 2001). "Pharmacology and toxicology of ethinyl estradiol and norethindrone acetate in experimental animals". Regulatory Toxicology and Pharmacology. 34 (1): 53–61. doi:10.1006/rtph.2001.1483. PMID 11502156.
- Riis BJ, Lehmann HJ, Christiansen C (October 2002). "Norethisterone acetate in combination with estrogen: effects on the skeleton and other organs. A review". American Journal of Obstetrics and Gynecology. 187 (4): 1101–16. doi:10.1067/mob.2002.122852. PMID 12389012.
- Draper BH, Morroni C, Hoffman M, Smit J, Beksinska M, Hapgood J, et al. (July 2006). "Depot medroxyprogesterone versus norethisterone oenanthate for long-acting progestogenic contraception". The Cochrane Database of Systematic Reviews. 2012 (3) CD005214. doi:10.1002/14651858.CD005214.pub2. PMC 11491191. PMID 16856087.
- Kuhl H, Wiegratz I (August 2007). "Can 19-nortestosterone derivatives be aromatized in the liver of adult humans? Are there clinical implications?". Climacteric. 10 (4): 344–53. doi:10.1080/13697130701380434. PMID 17653961. S2CID 20759583.
- Casey CL, Murray CA (2008). "HT update: spotlight on estradiol/norethindrone acetate combination therapy". Clinical Interventions in Aging. 3 (1): 9–16. doi:10.2147/cia.s1663. PMC 2544373. PMID 18488874.
- Paulen ME, Curtis KM (October 2009). "When can a woman have repeat progestogen-only injectables--depot medroxyprogesterone acetate or norethisterone enantate?". Contraception. 80 (4): 391–408. doi:10.1016/j.contraception.2009.03.023. PMID 19751863.
- Chwalisz K, Surrey E, Stanczyk FZ (June 2012). "The hormonal profile of norethindrone acetate: rationale for add-back therapy with gonadotropin-releasing hormone agonists in women with endometriosis". Reproductive Sciences. 19 (6): 563–71. doi:10.1177/1933719112438061. PMID 22457429. S2CID 2882899.
Norethisterone
View on GrokipediaMedical Uses
Contraception
Norethisterone, also known as norethindrone, is employed in multiple contraceptive formulations, including progestin-only pills (POPs), combined oral contraceptives (COCs), and injectable preparations. In POPs, it is administered as a daily 0.35 mg tablet, such as in brands like Camila or Micronor, providing contraception without estrogen for women who cannot tolerate estrogen-containing methods, such as those breastfeeding or with certain cardiovascular risks.[6] The primary mechanism involves thickening cervical mucus to block sperm penetration and thinning the endometrial lining to prevent implantation, with ovulation suppressed in approximately 50% of cycles due to the low dose.[7] Contraceptive efficacy for norethisterone POPs is 99% with perfect use (less than 1 pregnancy per 100 women per year) but drops to 91% with typical use (about 9 pregnancies per 100 women per year), largely due to the strict requirement of taking the pill at the same time daily given its short half-life of 5-13 hours.[6][8] In combined oral contraceptives, norethisterone is paired with ethinylestradiol (EE) in various doses, such as 0.5-1 mg norethisterone with 20-35 mcg EE in formulations like Loestrin or Ortho-Novum, taken in 21- or 28-day cycles.[9] This combination primarily inhibits ovulation by suppressing gonadotropin release, while also altering cervical mucus and the endometrium for added protection.[7] Efficacy mirrors other COCs, with perfect-use failure rates of 0.3% and typical-use rates of 9%, supported by extensive clinical data showing high reliability when adherence is maintained. These pills are often first-line options for their established safety profile in preventing pregnancy, though they carry a small risk of venous thromboembolism similar to other estrogen-progestin combinations.[9] Norethisterone enanthate, a long-acting ester, is available as an injectable contraceptive (e.g., Noristerat), administered intramuscularly at 200 mg every 8 weeks.[10] It works mainly by preventing ovulation through sustained progestin levels, with supplementary effects on cervical mucus and endometrium.[11] Clinical studies report a Pearl Index of 0.4 to 1.0 pregnancies per 100 woman-years, indicating high efficacy comparable to depot medroxyprogesterone acetate, with return to fertility typically within 3-4 months after discontinuation.[12] This method suits women seeking long-term, non-daily contraception but may involve irregular bleeding as a common side effect.[11]Menopausal Hormone Therapy
Norethisterone, also known as norethindrone, is a synthetic progestin commonly used in menopausal hormone therapy (MHT) in combination with estrogen to alleviate symptoms of menopause while providing endometrial protection in women with an intact uterus.[7] It opposes the stimulatory effects of estrogen on the endometrium, reducing the risk of hyperplasia and associated endometrial cancer that can occur with unopposed estrogen therapy.[13] This combined approach is recommended for women experiencing vasomotor symptoms such as hot flushes, night sweats, and vulvovaginal atrophy.[14] In continuous combined regimens, norethisterone acetate (NETA) is typically administered daily alongside estrogen to maintain steady hormone levels and minimize withdrawal bleeding. Common oral dosages include 0.5 mg NETA with 1 mg estradiol for treating moderate to severe vasomotor symptoms or 0.5 mg NETA with 0.5 mg estradiol in ultra-low-dose formulations.[15] Transdermal patches deliver, for example, 140 mcg NETA with 50 mcg estradiol twice weekly, offering an alternative route that may reduce gastrointestinal side effects.[16] For sequential regimens, norethisterone is given for at least 10 to 12 days per month (e.g., 5-10 mg daily) to mimic natural cycles and ensure endometrial protection, with studies confirming that shorter durations increase hyperplasia risk.[17][18] Clinical trials demonstrate the efficacy of norethisterone-containing MHT in symptom relief. In a randomized study of postmenopausal women, ultra-low-dose continuous therapy with 0.5 mg estradiol and 0.1 mg NETA reduced vasomotor symptom frequency by 77.1% over 24 weeks, compared to 49.9% with placebo, with significant improvements in severity scores.[19] Low-dose combinations (e.g., 1 mg estradiol/0.5 mg NETA) also enhance quality of life by addressing sleep disturbances and mood changes associated with menopause.[14] Endometrial biopsies in long-term users show minimal hyperplasia rates, affirming its protective role when dosed appropriately.[20] Safety profiles are generally favorable, with adverse event rates comparable to placebo in short-term studies (49.1% vs. 43.3%).[21] Common issues include unscheduled bleeding, particularly in the first months, which often resolves with continued use.[19] While norethisterone provides effective opposition to estrogen, guidelines emphasize individualized dosing to balance benefits against potential risks like venous thromboembolism, with lowest effective doses preferred for women over 60.[14] Monitoring for breakthrough bleeding is advised to ensure ongoing endometrial safety.[22]Treatment of Gynecological Disorders
Norethisterone, a synthetic progestin, is employed in the management of several gynecological disorders by mimicking progesterone's effects on the endometrium and reproductive tract, thereby regulating menstrual cycles and alleviating symptoms associated with hormonal imbalances.[2] It is particularly indicated for conditions such as abnormal uterine bleeding due to hormonal causes, secondary amenorrhea, and endometriosis, where it helps stabilize the endometrium and suppress excessive proliferation.[2] Treatment regimens are tailored to the specific disorder, with dosages typically ranging from 2.5 to 15 mg daily, administered orally for defined periods to induce withdrawal bleeding or maintain suppression.[2] In the treatment of abnormal uterine bleeding (AUB), including heavy menstrual bleeding (HMB) or menorrhagia without organic pathology such as fibroids or malignancy, norethisterone is administered as 5 mg three times daily from days 5 to 26 of the menstrual cycle to reduce blood loss and regulate cycles.[23] This cyclical regimen promotes endometrial stabilization and has been shown to effectively control bleeding in women with ovulatory dysfunction, with withdrawal bleeding occurring 2–4 days after discontinuation.[23] For acute heavy bleeding, higher initial doses up to 10–15 mg daily may be used until hemostasis is achieved, followed by a maintenance taper.[4] Clinical guidelines recommend it as a first-line progestin option for HMB in adolescents and adults intolerant to estrogen-containing therapies, demonstrating significant reduction in menstrual blood loss volumes.[24] For endometriosis, norethisterone is used to suppress lesion growth and relieve associated dysmenorrhea, dyspareunia, and chronic pelvic pain by inhibiting ovulation and endometrial proliferation.[2] Therapy typically begins with 5 mg daily for two weeks, increasing by 2.5 mg increments every two weeks to a maintenance dose of 15 mg daily for 6–9 months or longer, with periodic pauses if breakthrough bleeding occurs.[2] Studies indicate that low-dose norethisterone acetate (5 mg daily) effectively reduces ovarian endometrioma size and pain symptoms, offering a well-tolerated alternative to surgery with good long-term acceptability.[25] It has also shown efficacy in managing colorectal endometriosis symptoms, improving quality of life without significant adverse effects in extended use up to 12 months.[26] Norethisterone addresses secondary amenorrhea by inducing withdrawal bleeding after a course of 2.5–10 mg daily for 5–10 days, confirming the uterus's responsiveness to progestins and aiding diagnosis of underlying anovulation.[2] In endometrial hyperplasia without atypia, it promotes regression through progestogenic effects on atypical cells, with regimens of 10–15 mg daily for 3–6 months showing higher efficacy compared to some alternatives, though hysterectomy rates may remain elevated in non-responders.[27] For adenomyosis, low-dose therapy (5 mg daily) provides symptomatic relief from dysmenorrhea and heavy bleeding, serving as an inexpensive medical option prior to surgical intervention.[28] Across these applications, monitoring for response and side effects is essential, with treatment duration adjusted based on clinical outcomes and patient tolerance.[2]Other Indications
Norethisterone is indicated for the postponement of menstruation, where it is typically administered at a dose of 5 mg three times daily, starting three days before the expected onset of the period, to delay bleeding for as long as treatment continues, with withdrawal bleeding occurring two to three days after discontinuation.[29] In transgender and gender-diverse youth assigned female at birth, norethisterone acetate (5 mg daily) is used off-label for menstrual suppression to alleviate gender dysphoria, achieving amenorrhea rates of 84% after 1-3 months and up to 97% at one year, with significant improvements in bleeding, pain, and mood after three months of use.[30] Similarly, in adolescents with intellectual or physical disabilities, norethisterone facilitates menstrual management by inducing amenorrhea, addressing challenges related to hygiene, behavioral changes, or heavy bleeding, with continuous dosing at 5 mg three times daily recommended for reliable suppression.[31] High-dose norethisterone acetate (up to 40 mg daily) has been employed historically in the palliative treatment of advanced breast cancer, particularly in postmenopausal women, yielding objective response rates of approximately 41% in patients refractory to other therapies.[32] Norethisterone is occasionally used to suppress menstruation in women undergoing hematopoietic stem cell transplantation, though it carries an elevated risk of hepatic veno-occlusive disease compared to alternatives like GnRH agonists.Contraindications and Precautions
Absolute Contraindications
Norethisterone, a synthetic progestin, has several absolute contraindications due to the risk of severe adverse effects, including fetal harm, exacerbation of malignancies, and thromboembolic events. These contraindications are established in official prescribing information to ensure patient safety.[2] Known or suspected pregnancy is an absolute contraindication, as norethisterone may cause fetal abnormalities, including masculinization of female fetuses when used in the first trimester. Several reports suggest an association with congenital anomalies, leading to recommendations against its use during pregnancy or as a diagnostic test for it.[2][33] Undiagnosed abnormal vaginal bleeding contraindicates norethisterone administration, as the drug could mask underlying serious conditions such as endometrial hyperplasia or malignancy, delaying diagnosis and appropriate treatment.[2][33] Known, suspected, or a history of breast cancer represents an absolute contraindication, given the progestin's potential to stimulate hormone-sensitive tumor growth or recurrence. Progestins like norethisterone are contraindicated in patients with active or prior estrogen- or progesterone-dependent neoplasms.[2] Active deep vein thrombosis, pulmonary embolism, or a history of these conditions prohibits norethisterone use, as progestins increase the risk of venous thromboembolism through effects on coagulation factors and vascular endothelium. Similarly, active or recent (within the past year) arterial thromboembolic disease, such as stroke or myocardial infarction, is contraindicated due to heightened cardiovascular risks.[2][34] Impaired liver function, acute liver disease, or benign/malignant liver tumors are absolute contraindications, as norethisterone is metabolized hepatically and can worsen liver pathology or lead to cholestasis and peliosis hepatis. High-dose use has been linked to hepatic veno-occlusive disease.[2][33] Hypersensitivity to norethisterone or any excipients in the formulation is an immediate contraindication to avoid anaphylactic reactions or severe allergic responses.[2][34]Relative Precautions
Norethisterone should be used with caution in patients with a history of venous thromboembolism (VTE), as progestins may increase the risk of thrombotic events, particularly in those with predisposing factors such as obesity or immobilization; regular assessment for symptoms like leg pain, swelling, or shortness of breath is recommended.[29] Caution is advised in all smokers, as cigarette smoking greatly increases the possible effects of norethisterone on the heart and blood vessels. This risk is lower with progestin-only formulations compared to those containing estrogens.[35][36] Patients with conditions exacerbated by fluid retention, such as epilepsy, migraine, asthma, cardiac dysfunction, or renal impairment, require careful monitoring, as norethisterone can cause edema or worsen these states; dose adjustments or discontinuation may be necessary if symptoms intensify.[29] In individuals with diabetes or prediabetes, glucose tolerance may slightly deteriorate, necessitating closer monitoring of blood sugar levels during treatment.[35] Hepatic function should be evaluated prior to initiation and periodically thereafter in patients with mild liver impairment, given rare associations with hepatic adenomas or elevated liver enzymes; treatment should be suspended if jaundice or significant liver function abnormalities occur.[29] Additionally, women with a history of depression or those experiencing new-onset mood changes warrant vigilance, as progestins like norethisterone may exacerbate depressive symptoms in susceptible individuals.[37] Discontinuation is advised 4 to 6 weeks before major elective surgery or periods of prolonged immobilization to mitigate VTE risk.[29]Adverse Effects
Common Side Effects
Norethisterone, a synthetic progestin, commonly causes mild to moderate side effects that are typically self-limiting and resolve with continued use or discontinuation. The most frequently reported adverse effects involve changes in menstrual patterns, including irregular vaginal bleeding, spotting, breakthrough bleeding, and temporary amenorrhea, which occur in a significant proportion of users, particularly in contraceptive regimens.[38] These genitourinary effects are attributed to the drug's progestogenic activity on the endometrium and are noted in clinical studies as affecting up to 20-30% of patients depending on dosage and indication.[39] Gastrointestinal disturbances are also prevalent, with nausea and bloating reported by many users, especially during the initial weeks of therapy.[40] Breast tenderness or enlargement is another common complaint, resulting from the hormone's influence on mammary tissue.[39] Headaches and weight gain or fluid retention further contribute to the profile of routine side effects observed in post-marketing surveillance.[41] Skin and hair-related effects, such as acne, hirsutism (increased facial hair growth), or melasma (brown patches on the face), may occur due to the drug's mild androgenic properties, though these are less universal than menstrual changes.[40] Insomnia or sleep disturbances have been documented in some cases, alongside mood alterations like irritability, but these are generally transient.[42] Overall, the incidence of these effects varies by dose (typically 0.35 mg for contraception versus higher for other uses) and individual factors, with most resolving without intervention.[38] Patients are advised to monitor symptoms and consult healthcare providers if they persist.[40]Androgenic Effects
Norethisterone, a synthetic progestin derived from 19-nortestosterone, exhibits moderate androgenic activity through its ability to bind to the androgen receptor (AR), albeit with lower affinity compared to natural androgens like testosterone. This binding can activate AR-mediated pathways, leading to androgen-like effects in users, particularly women, though the clinical manifestation is generally mild due to the drug's primary progestogenic potency. The androgenic potency of norethisterone is intermediate among progestins, less pronounced than that of second-generation agents like levonorgestrel but sufficient to influence metabolic and dermatological outcomes in susceptible individuals.[5][43] The most commonly reported androgenic adverse effects include acne and hirsutism, which arise from increased sebum production and stimulation of hair follicles, respectively. These dermatological changes typically occur in a minority of users and are dose-dependent, often resolving upon discontinuation. Oily skin and mild weight gain, potentially linked to fluid retention or altered fat distribution, have also been observed, reflecting the drug's impact on androgen-sensitive tissues. In clinical studies, such effects are reported infrequently with standard contraceptive doses (e.g., 0.35–1 mg daily) but may increase with higher therapeutic doses used in conditions like endometriosis (5–10 mg daily).[44][45] Rare but more significant androgenic effects encompass voice deepening and clitoral enlargement, which can be irreversible in prolonged high-dose exposure due to persistent AR activation in laryngeal and genital tissues. Androgenic alopecia, characterized by male-pattern hair thinning, has been noted in case reports, particularly in women predisposed to androgen sensitivity. Additionally, norethisterone's androgenicity contributes to unfavorable lipid profile changes, such as decreased high-density lipoprotein (HDL) cholesterol levels, elevating cardiovascular risk in long-term users. These metabolic effects underscore the need for monitoring in patients with pre-existing lipid disorders.[46][47][5] Overall, the androgenic profile of norethisterone is a key consideration in selecting progestin-based therapies, with lower-androgenicity alternatives preferred for patients at risk of these effects. Clinical guidelines recommend assessing baseline androgen status and educating users on potential changes.[48]Estrogenic Effects
Norethisterone exhibits weak intrinsic estrogenic activity, primarily through bioconversion to A-ring reduced metabolites such as 3β,5α-tetrahydro-norethisterone and 3α,5α-tetrahydro-norethisterone, which bind to and activate estrogen receptors α and β in vitro.[49][50] This estrogenicity is dose-dependent and more pronounced at higher doses, contributing to its mixed hormonal profile alongside dominant progestogenic effects.[51] The estrogenic properties of norethisterone can manifest as adverse effects, particularly including breast tenderness or enlargement, nausea, vomiting, and bloating due to fluid retention.[40] These symptoms mimic those of estrogen exposure and are reported in users of norethisterone-containing therapies, such as oral contraceptives or treatments for gynecological disorders, though they are generally mild and transient. Weight gain associated with fluid retention has also been linked to this activity, occurring in a subset of patients.[41] In postmenopausal hormone therapy combinations, the estrogenic component may exacerbate risks like endometrial changes if not balanced properly, but monotherapy effects remain limited to these common manifestations.[7]Serious Risks
Norethisterone, particularly when used at higher therapeutic doses (e.g., 5–15 mg daily for conditions like menorrhagia or endometriosis), carries an increased risk of venous thromboembolism (VTE), comparable to that of combined oral contraceptives containing 20–30 mcg ethinylestradiol.[53] This risk is estimated at 3–9 additional cases per 10,000 woman-years versus non-users, with higher incidence in women over 35, smokers, or those with obesity, hypertension, or thrombophilic conditions.[54] Arterial thromboembolic events, such as myocardial infarction and ischemic stroke, are also elevated, especially in current users with cardiovascular risk factors.[55] In menopausal hormone therapy combining norethisterone with estrogen, the risk of breast cancer is notably higher than with estrogen alone, with relative risks increasing by approximately 2-fold after 5 years of use and linked to the highest increments among progestogen types.[56] Progestin-only formulations like low-dose norethisterone (0.35 mg) show no significant association with breast cancer, though long-term use may confer a slight elevation.[57] Current or recent use of norethisterone-containing contraceptives is associated with a modest overall breast cancer risk increase (relative risk 1.2–1.5), which diminishes after discontinuation.[58] Hepatic complications represent another serious concern, including cholestatic jaundice, benign liver tumors (hepatic adenomas), and, rarely, hepatocellular carcinoma, particularly with prolonged use; these necessitate immediate discontinuation upon onset of symptoms like jaundice or abdominal pain.[55] Gallbladder disease risk is heightened, manifesting as cholelithiasis or cholecystitis.[59] Other severe risks include sudden vision disturbances or severe headaches suggestive of pseudotumor cerebri, severe hypertension, and psychiatric effects such as major depressive episodes, which may require prompt medical evaluation.[2] Rare but life-threatening allergic reactions, including anaphylaxis, have been reported.[41] In specific contexts, such as post-bone marrow transplantation, norethisterone has been identified as a major risk factor for hepatic veno-occlusive disease.[60]Overdose
Symptoms
Overdose of norethisterone is not associated with serious or life-threatening effects, even in cases of ingestion by children.[7][61] Symptoms of norethisterone overdose typically include nausea and vomiting, which may be significant.[7][62] In females, additional manifestations can involve breast tenderness or enlargement, vaginal bleeding (which may present as spotting or withdrawal bleeding), and abdominal pain.[62][63][61] Less commonly reported symptoms from progestin overdoses, such as those involving norethisterone, may include drowsiness, fatigue, headache, or emotional changes, though these are generally mild and self-limiting.[64][65] There is no specific antidote, and symptoms are managed supportively.[62]Management
Management of norethisterone overdose focuses on supportive care, given the low risk of serious toxicity and absence of a specific antidote. Overdose is not expected to cause dangerous effects, even in children, with no reports of severe ill effects documented in clinical use. Patients should immediately contact a poison control center or seek emergency medical evaluation to assess the situation and receive guidance tailored to the exposure. Supportive measures include monitoring vital signs and providing symptomatic relief for potential effects such as nausea, vomiting, or abdominal pain. In instances of recent oral ingestion, activated charcoal may be administered to reduce drug absorption if deemed appropriate by healthcare providers, though gastric lavage is rarely necessary due to the drug's low toxicity profile. Further treatment is directed toward any observed symptoms, with hospitalization typically unnecessary unless complications arise.Drug Interactions
Pharmacokinetic Interactions
Norethisterone undergoes hepatic metabolism primarily via the cytochrome P450 enzyme CYP3A4, with minor contributions from CYP2C19, CYP1A2, and CYP2A6, making it susceptible to pharmacokinetic interactions with drugs that induce or inhibit these enzymes.[7][66] Inducers of CYP3A4 accelerate the metabolism of norethisterone, leading to reduced plasma concentrations and potentially diminished therapeutic efficacy, such as in contraception or hormone replacement therapy. Conversely, CYP3A4 inhibitors slow metabolism, increasing norethisterone exposure and the risk of adverse effects.[67] CYP3A4 Inducers and Decreased Norethisterone ExposureRifampicin, a potent CYP3A4 inducer, significantly reduces norethisterone bioavailability by enhancing its hepatic clearance; studies in women show a marked decrease in area under the curve (AUC) and peak plasma levels during coadministration, necessitating alternative contraception.[68] Similarly, bosentan induces CYP3A4 and decreases norethisterone AUC by approximately 14% when combined with ethinylestradiol in oral contraceptives, potentially increasing the risk of contraceptive failure.[69] Other inducers like phenobarbital lower plasma norethisterone levels in animal models, with effects persisting after intravenous administration due to enhanced elimination.[70] St. John's wort also induces CYP3A4, potentially reducing norethisterone efficacy through accelerated intestinal and hepatic metabolism, though clinical data are limited to case reports of breakthrough bleeding.[71] CYP3A4 Inhibitors and Increased Norethisterone Exposure
Clarithromycin, a strong CYP3A4 inhibitor, decreases norethisterone metabolism, elevating its serum concentrations and potentially amplifying progestogenic effects.[7] In HIV-positive women treated with ritonavir-boosted regimens, which inhibit CYP3A4 and P-glycoprotein, norethindrone (norethisterone) exposure increased by up to 50%, attributed to reduced gut and liver clearance.[72] Ketoconazole, another potent inhibitor, potently blocks norethisterone formation in vitro (IC50 ≈ 0.1 μM), supporting the potential for elevated levels in vivo.[66] Food intake can also influence pharmacokinetics, with high-fat meals increasing norethisterone AUC by about 27% when administered as part of combined oral contraceptives, likely due to enhanced absorption, but this is not a drug interaction.[73] Overall, patients on norethisterone should avoid strong CYP3A4 modulators or use backup contraception with inducers, as per regulatory guidance.[2]
| Interacting Drug | Enzyme Effect | Impact on Norethisterone | Clinical Implication | Source |
|---|---|---|---|---|
| Rifampicin | CYP3A4 Inducer | Decreased AUC and C_max | Reduced efficacy; use alternative contraception | PubMed 37091 |
| Bosentan | CYP3A4 Inducer | ~14% decrease in AUC | Potential increased contraceptive failure risk | PubMed 16550733 |
| Clarithromycin | CYP3A4 Inhibitor | Increased serum concentrations | Potential for enhanced side effects | DrugBank DB00717 |
| Ritonavir | CYP3A4/P-gp Inhibitor | Up to 50% increase in exposure | Monitor for adverse effects in HIV therapy | PMC4268426 |
Pharmacodynamic Interactions
Norethisterone, a synthetic progestin, exhibits pharmacodynamic interactions primarily through its agonistic effects on progesterone receptors, which can modulate glucose homeostasis, coagulation pathways, and interactions with other hormonal agents. These interactions arise from additive, synergistic, or antagonistic effects at the physiological or receptor level, rather than alterations in drug metabolism. Monitoring is often recommended when norethisterone is coadministered with agents affecting similar systems to mitigate risks such as impaired glycemic control or altered bleeding tendencies.[7] In patients with diabetes, norethisterone can antagonize the therapeutic effects of insulin and other antidiabetic medications by impairing glucose tolerance, potentially leading to elevated blood glucose levels. This occurs due to progestins' influence on insulin sensitivity and hepatic glucose production. For instance, coadministration with various insulin formulations, such as insulin degludec or insulin glulisine, may necessitate dosage adjustments of antidiabetic therapy to maintain glycemic control.[74][7][75] Norethisterone may potentiate the anticoagulant effects of warfarin, increasing the international normalized ratio (INR) and elevating the risk of bleeding, as observed in case reports among adolescent females using it for heavy menstrual bleeding management alongside mechanical heart valves. This interaction likely stems from progestins' modulation of hemostatic factors, including potential effects on vitamin K-dependent clotting factors or fibrinolytic activity. Theoretical risks may apply to direct oral anticoagulants like apixaban due to potential combined impacts on coagulation, though specific data are limited.[76][77][7] Close INR monitoring and dose adjustments are advised. With other hormonal contraceptives or modulators, norethisterone can interact pharmacodynamically; for example, progestogen-only methods containing norethisterone may reduce the efficacy of ulipristal acetate emergency contraception by competing at progesterone receptors, potentially diminishing its ability to delay ovulation. This underscores the need for alternative non-hormonal emergency options in such scenarios. Additionally, when combined with estrogens in hormone replacement therapy, norethisterone exerts synergistic effects on endometrial protection, though this is an intended therapeutic interaction rather than an adverse one.Pharmacology
Pharmacodynamics
Norethisterone, also known as norethindrone, is a synthetic progestin that acts as a potent agonist of the progesterone receptor (PR), the primary biological target for its pharmacodynamic effects. Upon binding to the PR in target tissues such as the uterus, ovaries, and pituitary gland, norethisterone induces conformational changes in the receptor, facilitating its translocation to the nucleus where it modulates gene transcription. This results in downstream alterations in protein synthesis that mediate progestogenic activities, including the promotion of secretory transformation in the endometrium and inhibition of gonadotropin release.[1][78][79] The relative binding affinity (RBA) of norethisterone to the human PR is approximately 150% that of progesterone, indicating higher potency compared to the endogenous hormone.[80][81] This binding suppresses the hypothalamic-pituitary-ovarian axis by negative feedback, reducing the secretion of follicle-stimulating hormone (FSH) and luteinizing hormone (LH), thereby preventing follicular development and ovulation in about 50–80% of cycles depending on dose. Additional local effects include thickening of cervical mucus to impede sperm penetration and thinning of the endometrial lining to reduce receptivity for implantation.[81][82][83] In therapeutic contexts, such as contraception or hormone replacement, norethisterone's PR agonism also contributes to decidualization of the stromal cells in the endometrium, stabilizing it against estrogen-induced proliferation and mitigating risks like endometrial hyperplasia. While norethisterone demonstrates low-affinity binding to other steroid receptors—such as the androgen receptor (AR, RBA ~15–20% relative to dihydrotestosterone) and glucocorticoid receptor (GR, RBA <5% relative to cortisol)—these interactions are secondary to its primary progestogenic profile and are associated with minimal cross-activity at standard doses.[84][85][86]Pharmacokinetics
Norethisterone is rapidly and completely absorbed following oral administration, with peak plasma concentrations typically occurring between 1 and 3 hours post-dose.[29] The oral bioavailability ranges from 47% to 73%, with a mean of approximately 64%, influenced by first-pass metabolism in the liver.[87] Micronization of the drug formulation enhances dissolution and absorption rates.[88] Once absorbed, norethisterone is widely distributed in the body, with plasma levels reaching about 60% of those observed after intravenous administration due to hepatic first-pass effects.[29] It exhibits high protein binding, approximately 97% to plasma proteins, of which 36% to 38% binds to sex hormone-binding globulin (SHBG) and 61% to albumin.[7] The volume of distribution is around 4 L/kg, reflecting its lipophilic nature and tissue penetration.[7] Norethisterone undergoes extensive hepatic metabolism, primarily via cytochrome P450 enzymes, including 3α- and 5α/β-reductions, hydroxylation, and conjugation to form sulfate and glucuronide metabolites.[7] A distinctive feature is its partial biotransformation to ethinylestradiol (EE), an estrogen, which contributes to its mixed progestogenic and estrogenic effects; this conversion occurs to a small extent (about 0.3-0.5% of the dose) but is pharmacologically significant.[89] Many metabolites retain some progestogenic activity, though less potent than the parent compound. Elimination occurs mainly through renal and fecal routes, with approximately 60% of the dose excreted as metabolites in urine and feces over several days.[29] The plasma clearance is estimated at 0.4 L/h/kg, with intrinsic clearance of 73 to 81 L/h.[7] The terminal elimination half-life varies from 5 to 12 hours, with a mean of about 7.6 to 9 hours, supporting once- or twice-daily dosing regimens.[29]Chemistry and Synthesis
Chemical Properties
Norethisterone, also known as norethindrone, is a synthetic steroid hormone belonging to the class of 19-nortestosterones. It features a characteristic steroid backbone with four fused rings: three six-membered cyclohexane rings (A, B, and C) and one five-membered cyclopentane ring (D). The molecule lacks the C19 methyl group typical of testosterone derivatives, incorporates a double bond between C4 and C5, a ketone group at C3, a hydroxyl group at C17β, and an ethynyl group (-C≡CH) at C17α, which enhances its progestogenic potency.[1][7] The molecular formula of norethisterone is C20H26O2, and its molecular weight is 298.42 g/mol. The IUPAC name is (8R,9S,10R,13S,14S,17R)-17-ethynyl-17-hydroxy-13-methyl-1,2,6,7,8,9,10,11,12,13,14,15,16,17-tetradecahydrocyclopentaphenanthren-3-one.[1][7][90] Norethisterone appears as a white to creamy white crystalline powder. It has a melting point of 203–206 °C and an estimated boiling point of approximately 380 °C. The compound is poorly soluble in water (about 0.007 g/L at 25 °C) but soluble in organic solvents such as chloroform, ethanol, and acetone. Its log P (octanol-water partition coefficient) is around 3.0–3.2, indicating moderate lipophilicity, which contributes to its bioavailability in pharmaceutical formulations. The specific rotation is [α]D20 = -31.7° (in chloroform).[1][7][91]Derivatives
Norethisterone, a first-generation 19-nortestosterone-derived progestin, serves as the parent compound for several synthetic derivatives that modify its pharmacokinetic profile, potency, or receptor binding affinity while retaining core progestogenic activity. These derivatives are primarily employed in hormonal contraception, menopausal hormone therapy, and treatment of gynecological disorders, often exhibiting reduced androgenic or estrogenic side effects compared to earlier progestins. Most are metabolized back to norethisterone in vivo, enhancing bioavailability or duration of action.[92] Key derivatives include norethisterone acetate (NETA), the 17β-acetate ester, which is rapidly deacetylated to active norethisterone following oral administration, achieving peak plasma levels within 1-2 hours. NETA binds to the progesterone receptor with high affinity (similar to progesterone) and shows moderate androgenic activity, making it suitable for combined oral contraceptives (e.g., at 0.35-1 mg doses) and endometrial protection in estrogen replacement therapy. It has been widely studied for its role in suppressing ovulation and stabilizing the endometrium without significant mineralocorticoid effects.[93][94] Ethynodiol diacetate, a 3,17-diacetate derivative, acts as a prodrug that undergoes hydrolysis to ethynodiol and subsequently to norethisterone, providing potent progestogenic effects with low androgenicity. Administered at 0.5-1 mg in oral contraceptives, it inhibits gonadotropin release and alters cervical mucus, contributing to contraceptive efficacy rates exceeding 99% with perfect use. Its minimal impact on lipid profiles distinguishes it from more androgenic progestins.[78][92] Norethynodrel, featuring a Δ5(10)-3-keto ene structure, isomerizes to norethisterone during metabolism and was pivotal in the first approved oral contraceptive (Enovid, 1960). It exhibits strong progestogenic activity alongside weak estrogenic properties due to its unsaturated A-ring, used historically at 2.5-5 mg doses for cycle control and fertility suppression, though largely replaced by newer agents with better side-effect profiles.[95] Lynestrenol, the 17α-ethynyl-3-ene derivative lacking the 3-keto group, is converted to norethisterone via hepatic metabolism and displays progestogenic and mild anabolic effects without significant antiestrogenic activity. It is utilized in oral contraceptives (e.g., 0.5 mg with ethinylestradiol) and for treating hypermenorrhea, offering good tolerability and endometrial transformation at lower doses than the parent compound.[92][96] Long-acting esters such as norethisterone enanthate (NET-EN), formed by esterification at the 17β-hydroxyl with heptanoic acid, enable intramuscular depot formulations for extended contraception (up to 8-12 weeks at 200 mg doses). Pharmacokinetic studies show sustained release with antifertility duration not proportionally increased beyond standard doses, but effective ovulation suppression for 2-3 months via progesterone receptor agonism. Other experimental esters, like phenylpropionate variants, have been explored for prolonged action but remain less clinically adopted.[97][98]Synthesis Methods
Norethisterone, also known as 19-nor-17α-ethynyltestosterone, was first synthesized in 1951 by Luis Miramontes under the supervision of Carl Djerassi, George Rosenkranz, and Frank Sondheimer at Syntex in Mexico City. The seminal synthesis began with 3-methoxyestra-1,3,5(10)-trien-17-one (3-O-methylestrone) as the starting material. This compound underwent Birch reduction using sodium in liquid ammonia and ethanol to yield the 1,4-diene intermediate, specifically 3-methoxyestra-1(10),2,4-triene-17-one. Subsequent hydrolysis with aqueous acid cleaved the methyl enol ether, affording estr-4-ene-3,17-dione (19-norandrost-4-ene-3,17-dione). Ethynylation was achieved by reaction with ethynylmagnesium bromide in tetrahydrofuran, yielding 17α-ethynyl-17β-hydroxyestra-4-en-3-one (norethisterone) with an overall yield of approximately 20-30% from the starting estrone derivative.[99] This multi-step process established norethisterone as the first orally active progestin, enabling its use in early contraceptive formulations. The method relied on classical steroid transformations, including partial reduction of the aromatic A-ring, angular methyl group removal at C19 via the Birch procedure, and introduction of the ethynyl group at C17 to enhance progestogenic activity while maintaining oral bioavailability.[99] Subsequent industrial syntheses have optimized efficiency and scalability. A widely adopted approach starts from 19-norandrost-4-ene-3,17-dione and involves ethynylation at C17 using ethynylmagnesium bromide, often in the presence of cerium(III) chloride as a Lewis acid catalyst to improve selectivity and yield. This single-pot reaction proceeds via addition of the acetylide to the 17-keto group, directly affording 17α-ethynyl-17β-hydroxyestra-4-en-3-one (norethisterone) in yields exceeding 80%. The process avoids intermediate isolation, reducing costs and waste in pharmaceutical production.[100] For the acetate derivative, norethisterone acetate, a four-step method from 19-norandrost-4-ene-3,17-dione includes protection of the 3-keto group (e.g., as a ketal), ethynylation at C17, deprotection, and acetylation of the 17-hydroxy group using acetic anhydride. This route achieves high purity suitable for clinical use, with overall yields around 60-70%.[101] Ester derivatives, such as aliphatic and arylcarboxylic esters of norethisterone, have been prepared via a one-step acylation using the corresponding acid chloride or anhydride in pyridine, providing near-quantitative yields (>95%) for prodrug applications. These modifications enhance pharmacokinetics without altering the core synthesis.[102]History and Development
Discovery
Norethisterone, also known as norethindrone or 19-nor-17α-ethynyltestosterone, was first synthesized on October 15, 1951, by Mexican chemist Luis E. Miramontes at the pharmaceutical company Syntex S.A. in Mexico City.[103] This breakthrough occurred under the supervision of Carl Djerassi, a leading steroid chemist, and in collaboration with George Rosenkranz and Franz Sondheimer, as part of Syntex's efforts to develop potent, orally active progestins from plant-derived sterols such as diosgenin obtained from Mexican yams.[104][105] The synthesis built on prior work with ethisterone (17α-ethynyltestosterone), a weakly active oral progestin, by removing the 19-methyl group to enhance progestational activity and bioavailability. The process involved protecting the 4-ene-3-keto functionality as an enol ether, ethynylation at the 17α position using acetylene, and subsequent degradation to remove the 19-methyl group, yielding norethisterone with significantly improved oral progestogenic potency compared to progesterone, enabling effective administration by mouth.[99] This modification addressed the limitations of natural progesterone, which was ineffective when taken orally due to rapid metabolism in the liver.[104] Syntex filed a patent for norethisterone in 1951, recognizing its potential for treating conditions like irregular menstruation and endometriosis, though its contraceptive applications emerged later through clinical studies.[104] The compound's development represented a high-impact contribution to steroid chemistry, paving the way for modern hormonal therapies and earning recognition as one of the first synthetic progestins suitable for oral use.[106]Clinical Introduction
Norethisterone, a synthetic progestin derived from 19-nortestosterone, was first synthesized in 1951 by chemist Luis Miramontes at Syntex S.A. in Mexico City, under the supervision of Carl Djerassi and George Rosenkranz. This breakthrough compound was the first orally active progestogen capable of mimicking the effects of natural progesterone, enabling non-invasive treatment for hormonal imbalances. Initially developed to address gynecological conditions such as irregular menstruation and endometriosis, it represented a major advance over prior progestogens that required injection due to poor oral bioavailability.[105][7][107] The compound was patented shortly after its synthesis and entered clinical practice as a standalone therapeutic agent in 1957, primarily for managing amenorrhea, dysmenorrhea, and abnormal uterine bleeding. Early clinical trials demonstrated its potency in inducing endometrial changes and suppressing ovulation, establishing it as a versatile option for hormone replacement and cycle regulation. By providing reliable oral dosing, norethisterone facilitated broader access to progestin therapy, particularly in regions with limited medical infrastructure, and laid the groundwork for its expanded applications.[108][93] In the early 1960s, norethisterone's role evolved with its incorporation into combined oral contraceptives alongside estrogens like mestranol. Formulations such as Ortho-Novum and Norinyl, containing 2.5 mg or 1 mg of norethisterone, received regulatory approval for contraceptive use starting in 1963, marking the transition from therapeutic to preventive applications. These first-generation pills offered effective ovulation inhibition with typical use failure rates below 5%, revolutionizing family planning while building on norethisterone's established safety profile from non-contraceptive uses.[109][110]Regulatory Milestones
Norethisterone, known as norethindrone in the United States, has a long history of regulatory approvals primarily for use in hormonal therapies and contraception, beginning with its synthesis in 1951 and subsequent marketing in the early 1960s as part of combination oral contraceptives. The compound was first introduced to the American market in formulations containing 10 mg norethindrone and 60 μg mestranol for contraceptive purposes.[45] Specific early approvals include the combination product Ortho-Novum, which received FDA approval in 1963 for prevention of pregnancy, marking one of the initial regulatory milestones for norethisterone-based products following the pioneering Enovid approval in 1960.[109] Subsequent milestones focused on single-agent and low-dose combination formulations. The FDA approved norethindrone acetate tablets (Aygestin, NDA 018405) for the treatment of secondary amenorrhea, endometriosis, and abnormal uterine bleeding due to hormonal imbalance, with the product available prior to generic approvals in 1982. In 1976, the FDA granted approval for Ovcon 35 (0.4 mg norethindrone and 0.035 mg ethinyl estradiol tablets, NDA 17-716) as a 28-day regimen oral contraceptive. Later approvals expanded indications, such as Femhrt (norethindrone acetate and ethinyl estradiol tablets, NDA 21-065) in 1999 for vasomotor symptoms associated with menopause.[111] In recent years, regulatory advancements have emphasized innovative delivery and new indications. The FDA approved Loestrin 24 Fe (norethindrone acetate/ethinyl estradiol and ferrous fumarate) in 2006 as a 24-day active hormone regimen contraceptive. A significant milestone occurred in 2021 with the approval of Myfembree (relugolix, estradiol, and norethisterone acetate) for management of heavy menstrual bleeding associated with uterine fibroids in premenopausal women. Most recently, on July 23, 2024, the FDA approved Femlyv, the first orally disintegrating tablet containing norethindrone acetate and ethinyl estradiol for pregnancy prevention, addressing accessibility for those with swallowing difficulties.[112][113] In Europe, the European Medicines Agency (EMA) has overseen approvals for norethisterone-containing products since the mid-20th century, with Primolut N (norethisterone 5-15 mg/day) approved as monotherapy for menstrual disorders. A 2019 EMA assessment under Article 5(3) of Regulation (EC) No 726/2004 reviewed the benefit-risk profile of norethisterone and ethinylestradiol combinations, recommending continued use with monitoring for cardiovascular risks. In 2021, the EMA approved Ryeqo (relugolix 40 mg, estradiol 1 mg, norethisterone acetate 0.5 mg) for moderate-to-severe symptoms of uterine fibroids, with an extension in 2023 for endometriosis treatment in women of reproductive age.[114][115]Society and Culture
Nomenclature
Norethisterone is the International Nonproprietary Name (INN) and British Approved Name (BAN) for this synthetic progestin, while norethindrone serves as its United States Adopted Name (USAN).[116] These designations reflect regional variations in pharmaceutical nomenclature, with norethisterone being the preferred term in most international contexts, including the Japanese Accepted Name (JAN).[117] Alternative generic names include noréthistérone (French nonproprietary name, DCF) and noretisterone (deleted INN, DCIT).[117] Chemically, norethisterone is classified as a 19-nortestosterone derivative and is systematically named (17α)-17-hydroxy-19-norpregn-4-en-20-yn-3-one.[1] This nomenclature highlights its structure: a pregnane skeleton lacking the 19-methyl group, with a hydroxy group at position 17, an ethynyl group at 17α, and a ketone at position 3.[90] The IUPAC name is (8R,9S,10R,13S,14S,17R)-17-ethynyl-17-hydroxy-13-methyl-1,2,6,7,8,9,10,11,12,14,15,16-dodecahydrocyclopentaphenanthren-3-one.[118] Other synonyms used in scientific literature include ethinylnortestosterone (developmental code name) and norethynodrel (though the latter refers to a closely related but distinct compound).[117] Historical identifiers such as LG-202 have also appeared in early research documentation.[117] The molecular formula is C20H26O2, with a molecular weight of 298.42 g/mol.[1]Brand Names
Norethisterone, a synthetic progestin, is available under numerous brand names globally, often varying by region, formulation (such as tablets for contraception, endometriosis treatment, or hormone replacement), and whether it is used alone or in combination with estrogens.[117] These names reflect local manufacturing and regulatory approvals, with some brands focusing on progestin-only preparations like minipills, while others include acetate esters for specific indications.[7] In the United States, where it is commonly referred to as norethindrone, prominent brands for progestin-only contraceptives include Camila, Errin, Heather, Jencycla, and Nor-QD, all containing 0.35 mg of norethindrone.[119] For higher-dose treatments such as abnormal uterine bleeding or endometriosis, norethindrone acetate is marketed as Aygestin (5 mg tablets).[59] In the United Kingdom and other European countries, key brands include Primolut N (5 mg norethisterone tablets) for menstrual disorders and Noriday (350 micrograms) as a progestogen-only contraceptive.[120] Combination products like Brevinor, Norimin, and Norinyl-1 pair norethisterone with ethinylestradiol for oral contraception.[120] Internationally, Primolut N is widely recognized and available in countries including Australia, Argentina, and the United Arab Emirates for similar indications.[121] Other global examples include Micronor (progestin-only pill in Australia and elsewhere) and Utovlan (5 mg tablets in the UK for heavy menstrual bleeding).[45] In regions like India and Bangladesh, local brands such as Fertinor, Northeal, and Sani-Nor are common for 5 mg or 10 mg formulations.[122]Availability and Regulation
Norethisterone is widely available as a generic medication in numerous countries across the globe, including the United States, United Kingdom, Australia, Canada, India, and many European and Asian nations. It is marketed in various formulations such as tablets, injections, and combinations with estrogens for uses including contraception, treatment of menstrual disorders, endometriosis, and hormone replacement therapy.[117] The drug's broad accessibility is supported by its inclusion of the ester form, norethisterone enanthate, on the World Health Organization's Model List of Essential Medicines, highlighting its role in injectable hormonal contraceptives for basic healthcare systems.[123] In the United States, norethisterone is known as norethindrone or norethindrone acetate and has been regulated by the Food and Drug Administration (FDA) since its initial approval in 1964 for indications such as amenorrhea and endometriosis under the brand name Aygestin. Subsequent approvals expanded its use to contraception, with formulations like Micronor (0.35 mg tablets) receiving FDA approval for preventing pregnancy, though the original drug's status predates modern listing requirements and is considered prior to January 1, 1982. It remains available by prescription, with ongoing generic approvals ensuring supply, such as Aurobindo Pharma's final approval in 2016 for norethindrone tablets.[124][125][126] Within the European Union, norethisterone is authorized through national procedures by the European Medicines Agency (EMA) and member state agencies, with approved doses ranging from 5 to 15 mg daily for monotherapy in treating conditions like heavy menstrual bleeding and premenstrual syndrome. For example, in the United Kingdom, it is regulated by the Medicines and Healthcare products Regulatory Agency (MHRA) and available under brands like Primolut N for prescription-only use in delaying menstruation or managing endometriosis. The EMA has conducted safety assessments, such as the 2019 review of norethisterone with ethinylestradiol combinations, concluding no additional regulatory actions were needed beyond existing labeling.[114][29] In other regions, regulatory oversight varies but generally permits availability under prescription. In Australia, the Therapeutic Goods Administration (TGA) approves norethisterone for similar indications, though periodic shortages have been reported, such as for Norimin tablets (a combination product) from November 5, 2025, to January 30, 2026.[127] As of November 2025, shortages of certain hormone replacement therapy products containing norethisterone, such as transdermal patches, are ongoing and expected to persist until at least July 2026.[128] In India, it is produced by multiple manufacturers and regulated by the Central Drugs Standard Control Organization (CDSCO), with significant export volumes indicating robust supply chains. China and Brazil also list it among approved pharmaceuticals, with no widespread restrictions noted beyond standard prescription requirements. Overall, norethisterone faces no major global bans but is subject to pharmacovigilance monitoring for potential side effects like thromboembolism.[129]Non-Medical Use
Norethisterone has been used off-label to delay menstruation for non-medical reasons, such as vacations, holidays, weddings, or other personal events, where individuals seek to avoid the inconvenience of bleeding during these occasions.[130] This practice gained attention in the late 1990s when analysis of prescribing data in the UK revealed a seasonal peak in July, coinciding with summer holidays, suggesting widespread use for postponing periods rather than treating medical conditions.[130] The drug is taken orally at a dose of 5 mg three times daily starting three days before the expected period, typically delaying bleeding for up to 17 days after discontinuation, though effectiveness varies and side effects like breakthrough bleeding may occur.[131] Debate has arisen over whether this constitutes a "lifestyle drug," defined as a pharmaceutical agent promoting personal wellbeing rather than treating disease, with some viewing the seasonal prescribing pattern as evidence of recreational or convenience-based use.[130] However, health authorities and guidelines increasingly discourage prescribing norethisterone solely for non-medical convenience, emphasizing risks such as hormonal imbalances, mood changes, and potential masking of underlying conditions if used repeatedly.[132] In professional sports, female athletes have reported using norethisterone to suppress periods during competitions for performance and comfort reasons, though this is often framed within therapeutic exemptions rather than purely non-medical intent.[133] Despite its availability over-the-counter in some regions or via online pharmacies, non-medical use is not recommended due to limited long-term safety data for intermittent dosing and the potential for adverse effects including nausea, breast tenderness, and increased thrombosis risk.[131] Regulatory bodies, such as the UK's National Health Service, advise against routine use for lifestyle purposes, prioritizing medical indications like abnormal uterine bleeding.[134]Research Directions
Ongoing Studies
As of 2025, ongoing research on norethisterone emphasizes its integration into combination therapies for managing endometriosis, uterine fibroids, and abnormal uterine bleeding, with a focus on long-term safety profiles, including bone health and cardiovascular risks. Studies are particularly investigating norethisterone acetate in fixed-dose combinations with GnRH antagonists and estrogens, aiming to balance efficacy against hypoestrogenic side effects. These efforts build on recent approvals, such as Ryeqo (relugolix 40 mg, estradiol 1 mg, norethisterone acetate 0.5 mg) for treatment of endometriosis symptoms in reproductive-age women.[135] A key phase 3b extension of the SPIRIT trials is evaluating the long-term impact of Ryeqo on bone mineral density in women with uterine fibroids and endometriosis, monitoring changes over up to 2 years to assess reversibility of any losses upon discontinuation. This multinational study highlights norethisterone's role in mitigating estrogen suppression effects.[136] Another active investigation, NCT07173127, is a prospective cohort study assessing Ryeqo's effects on hemostasis parameters, such as coagulation factors and fibrinolysis markers, in premenopausal women with endometriosis or fibroids to quantify venous thromboembolism risk. Initiated in 2024 with an estimated completion in 2026, it enrolls 100 participants and measures outcomes like D-dimer levels and prothrombin time at baseline and after 6 months of therapy. Early findings suggest minimal prothrombotic shifts compared to GnRH agonists alone.[137] Emerging work also explores norethisterone monotherapy for breakthrough bleeding in long-acting reversible contraception users. A 2025 randomized trial demonstrated that 10 mg/day dosing effectively resolved prolonged bleeding in etonogestrel implant recipients, with low adverse event rates, prompting follow-up studies on optimal regimens for implant-related dysfunctional uterine bleeding. Ongoing extensions aim to evaluate recurrence rates over 12 months.[138]Potential New Applications
Research into norethisterone enanthate (NETE), a long-acting ester of norethisterone, has explored its role in male hormonal contraception when combined with testosterone undecanoate. In a phase IIb multicenter efficacy trial involving 320 healthy men aged 18-50, intramuscular injections of 200 mg NETE and 1000 mg testosterone undecanoate every 8 weeks suppressed spermatogenesis to ≤1 million sperm/mL in 96% of participants by week 26, demonstrating high contraceptive potential during the suppression phase.[139] However, the study was terminated early in 2016 following an external safety review that identified unfavorable lung function changes and mood alterations in some participants, raising concerns about the risk-benefit profile.[140] Despite this setback, ongoing reviews highlight NETE's ability to effectively suppress gonadotropins and provide androgenic support, positioning it as a candidate for future injectable regimens if safety issues are addressed through dose optimization or alternative formulations.[141] Norethisterone acetate has shown promise in gender-affirming care for menstrual suppression among transgender and gender-diverse adolescents and young adults assigned female at birth. A 2023 prospective cohort study found that norethindrone acetate (5 mg daily) achieved amenorrhea or spotting-only in 96% of users after 6 months, with high satisfaction rates and minimal side effects like weight gain or mood changes.[30] Similarly, a 2022 survey of 74 transgender and gender-diverse youth indicated that oral norethindrone was the most frequently selected method for bleeding management, preferred for its ease of use and reversibility compared to intrauterine devices.[142] These findings support its integration into protocols for alleviating gender dysphoria related to menstruation, though long-term data on bone health and cardiovascular risks remain limited.[143] Emerging evidence also suggests norethisterone's utility in managing heavy menstrual bleeding during cancer treatment to prevent anemia and improve quality of life. The 2021 American College of Obstetricians and Gynecologists guidelines recommend progestins like norethisterone (10 mg daily) as a first-line option for menstrual suppression in adolescents undergoing chemotherapy or radiation, citing rapid onset and oral administration advantages over GnRH agonists.[144] A 2024 systematic review of hematologic cancer patients reinforced this, reporting that hormone therapy achieved resolution of bleeding in 97% of cases without significant interference with oncologic therapies.[145] Further prospective trials are needed to evaluate its efficacy in diverse cancer subtypes and combination with other supportive care.References
- https://www.sciencedirect.com/topics/[neuroscience](/page/Neuroscience)/norethisterone




