Recent from talks
Nothing was collected or created yet.
Low back pain
View on Wikipedia
| Low back pain | |
|---|---|
| Other names | Lower back pain, lumbago |
 | |
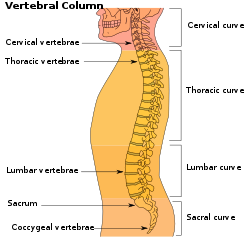
| Location of the lumbar region (pink) in relation to the human skeleton | |
| Pronunciation |
|
| Specialty | Orthopedics, rheumatology, rehabilitation medicine |
| Usual onset | 20 to 40 years of age[1] |
| Duration | ~65% get better in 6 weeks[2] |
| Types | Acute (less than 6 weeks), sub-chronic (6 to 12 weeks), chronic (more than 12 weeks)[3] |
| Causes | Usually non-specific, occasionally significant underlying cause[1][4] |
| Diagnostic method | Medical imaging (if red flags)[5] |
| Treatment | Continued normal activity, non-medication based treatments, NSAIDs[2][6] |
| Frequency | ~25% in any given month[7][8] |
Low back pain or lumbago is a common disorder involving the muscles, nerves, and bones of the back, in between the lower edge of the ribs and the lower fold of the buttocks. Pain can vary from a dull constant ache to a sudden sharp feeling.[4] Low back pain may be classified by duration as acute (pain lasting less than 6 weeks), sub-chronic (6 to 12 weeks), or chronic (more than 12 weeks).[3] The condition may be further classified by the underlying cause as either mechanical, non-mechanical, or referred pain.[5] The symptoms of low back pain usually improve within a few weeks from the time they start, with 40–90% of people recovered by six weeks.[2]
In most episodes of low back pain a specific underlying cause is not identified or even looked for, with the pain believed to be due to mechanical problems such as muscle or joint strain.[1][4] If the pain does not go away with conservative treatment or if it is accompanied by "red flags" such as unexplained weight loss, fever, or significant problems with feeling or movement, further testing may be needed to look for a serious underlying problem.[5] In most cases, imaging tools such as X-ray computed tomography are not useful or recommended for low back pain that lasts less than 6 weeks (with no red flags) and carry their own risks.[9] Despite this, the use of imaging in low back pain has increased.[10] Some low back pain is caused by damaged intervertebral discs, and the straight leg raise test is useful to identify this cause.[5] In those with chronic pain, the pain processing system may malfunction, causing large amounts of pain in response to non-serious events.[11] Chronic non-specific low back pain (CNSLBP) is a highly prevalent musculoskeletal condition that not only affects the body, but also a person's social and economic status. It would be greatly beneficial for people with CNSLBP to be screened for genetic issues, unhealthy lifestyles and habits, and psychosocial factors on top of musculoskeletal issues.[12] Chronic lower back pain is defined as back pain that lasts more than three months.[13]
The symptoms of low back pain usually improve within a few weeks from the time they start, with 40–90% of people recovered by six weeks.[2] Normal activity should be continued as much as the pain allows.[2] Initial management with non-medication based treatments is recommended.[6] Non–medication based treatments include superficial heat, massage, acupuncture, or spinal manipulation.[6] If these are not sufficiently effective, NSAIDs are recommended.[6][14] A number of other options are available for those who do not improve with usual treatment. Opioids may be useful if simple pain medications are not enough, but they are not generally recommended due to side effects,[15] including high rates of addiction, accidental overdose and death.[16] Surgery may be beneficial for those with disc-related chronic pain and disability or spinal stenosis.[17][18] No clear benefit of surgery has been found for other cases of non-specific low back pain.[17] Low back pain often affects mood, which may be improved by counseling or antidepressants.[19][20] Additionally, there are many alternative medicine therapies, but there is not enough evidence to recommend them confidently.[21] The evidence for chiropractic care[22] and spinal manipulation is mixed.[21][23][24][25]
Approximately 9–12% of people (632 million) have low back pain at any given point in time,[26] and nearly 25% report having it at some point over any one-month period.[7][8] About 40% of people have low back pain at some point in their lives,[7] with estimates as high as 80% among people in the developed world.[27] Low back pain is the greatest contributor to lost productivity, absenteeism, disability and early retirement worldwide.[26] Difficulty with low back pain most often begins between 20 and 40 years of age.[1] Women and older people have higher estimated rates of lower back pain and also higher disability estimates.[13] Low back pain is more common among people aged between 40 and 80 years, with the overall number of individuals affected expected to increase as the population ages.[7] According to the World Health Organization in 2023, lower back pain is the top medical condition world-wide from which the most number of people world-wide can benefit from improved rehabilitation.[13]
Signs and symptoms
[edit]In the common presentation of acute low back pain, pain develops after movements that involve lifting, twisting, or forward-bending. The symptoms may start soon after the movements or upon waking up the following morning. The description of the symptoms may range from tenderness at a particular point, to diffuse pain. It may or may not worsen with certain movements, such as raising a leg, or positions, such as sitting or standing. Pain radiating down the legs (known as sciatica) may be present. The first experience of acute low back pain is typically between the ages of 20 and 40. This is often a person's first reason to see a medical professional as an adult.[1] Recurrent episodes occur in more than half of people[28] with the repeated episodes being generally more painful than the first.[1]
Other problems may occur along with low back pain. Chronic low back pain is associated with sleep problems, including a greater amount of time needed to fall asleep, disturbances during sleep, a shorter duration of sleep, and less satisfaction with sleep.[29] In addition, a majority of those with chronic low back pain[need quotation to verify] show symptoms of depression[19] or anxiety.[21]
Causes
[edit]
Low back pain is not a specific disease but rather a complaint that may be caused by a large number of underlying problems of varying levels of seriousness.[30] The majority of low back pain does not have a clear cause[1] but is believed to be the result of non-serious muscle or skeletal issues such as sprains or strains.[31] Obesity, smoking, weight gain during pregnancy, stress, poor physical condition, and poor sleeping position may also contribute to low back pain.[31] There is no consensus as to whether spinal posture or certain physical activities are causal factors.[32] A full list of possible causes includes many less common conditions.[5] Physical causes may include osteoarthritis, degeneration of the discs between the vertebrae or a spinal disc herniation, broken vertebra(e) (such as from osteoporosis) or, rarely, an infection or tumor of the spine.[33]
Women may have acute low back pain from medical conditions affecting the female reproductive system, including endometriosis, ovarian cysts, ovarian cancer, or uterine fibroids.[34] Nearly half of all pregnant women report pain in the low back during pregnancy, which is attributed to changes in posture and the relocation of the center of gravity, leading to strain on the musculoskeletal system, including muscles, ligaments, and joints.[35]
Low back pain can be broadly classified into four main categories:
- Musculoskeletal – mechanical (including muscle strain, muscle spasm, or osteoarthritis); herniated nucleus pulposus, herniated disc; spinal stenosis; or compression fracture
- Inflammatory – HLA-B27 associated arthritis including ankylosing spondylitis, reactive arthritis, psoriatic arthritis, inflammation within the reproductive system, and inflammatory bowel disease
- Malignancy – bone metastasis from lung, breast, prostate, thyroid, among others
- Infectious – osteomyelitis, abscess, urinary tract infection.[36]
Pathophysiology
[edit]Back structures
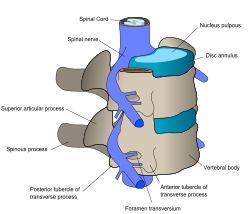
[edit]The lumbar (or lower back) region is the area between the lower ribs and gluteal fold which includes five lumbar vertebrae (L1–L5) and the sacrum. In between these vertebrae are fibrocartilaginous discs, which act as cushions, preventing the vertebrae from rubbing together while at the same time protecting the spinal cord. Nerves come from and go to the spinal cord through specific openings between the vertebrae, receiving sensory input and sending messages to muscles. Stability of the spine is provided by the ligaments and muscles of the back and abdomen. Small joints called facet joints limit and direct the motion of the spine.[37]
The multifidus muscles run up and down along the back of the spine, and are important for keeping the spine straight and stable during many common movements such as sitting, walking and lifting.[11] A problem with these muscles is often found in someone with chronic low back pain, because the back pain causes the person to use the back muscles improperly in trying to avoid the pain.[38] The problem with the multifidus muscles continues even after the pain goes away, and is probably an important reason why the pain comes back.[38] Teaching people with chronic low back pain how to use these muscles is recommended as part of a recovery program.[38]
An intervertebral disc has a gelatinous core surrounded by a fibrous ring.[39] When in its normal, uninjured state, most of the disc is not served by either the circulatory or nervous systems – blood and nerves only run to the outside of the disc.[39] Specialized cells that can survive without direct blood supply are in the inside of the disc.[39] Over time, the discs lose flexibility and the ability to absorb physical forces.[30] This decreased ability to handle physical forces increases stresses on other parts of the spine, causing the ligaments of the spine to thicken and bony growths to develop on the vertebrae.[30] As a result, there is less space through which the spinal cord and nerve roots may pass.[30] When a disc degenerates as a result of injury or disease, the makeup of a disc changes: blood vessels and nerves may grow into its interior and/or herniated disc material can push directly on a nerve root.[39] Any of these changes may result in back pain.[39]
Pain sensation
[edit]Pain erupts in response to a stimulus that either damages or can potentially damage the body's tissues. There are four main stages: transduction, transmission, perception, and modulation.[11] The nerve cells that detect pain have cell bodies located in the dorsal root ganglia and fibers that transmit these signals to the spinal cord.[40] The process of pain sensation starts when the pain-causing event triggers the endings of appropriate sensory nerve cells. This type of cell converts the event into an electrical signal by transduction. Several different types of nerve fibers carry out the transmission of the electrical signal from the transducing cell to the posterior horn of spinal cord, from there to the brain stem, and then from the brain stem to the various parts of the brain such as the thalamus and the limbic system. In the brain, the pain signals are processed and given context in the process of pain perception. Through modulation, the brain can modify the sending of further nerve impulses by decreasing or increasing the release of neurotransmitters.[11]
Parts of the pain sensation and processing system may not function properly; creating the feeling of pain when no outside cause exists, signaling too much pain from a particular cause, or signaling pain from a normally non-painful event. Additionally, the pain modulation mechanisms may not function properly. These phenomena are involved in chronic pain.[11]
Diagnosis
[edit]As the structure of the low back is complex, the reporting of pain is subjective, and is affected by social factors, the diagnosis of low back pain is not straightforward.[5] While most low back pain is caused by muscle and joint problems, this cause must be separated from neurological problems, spinal tumors, fracture of the spine, and infections, among others.[3][1] The ICD 10 code for low back pain is M54.5.
Classification
[edit]There are a number of ways to classify low back pain with no consensus that any one method is best.[5] There are three general types of low back pain by cause: mechanical back pain (including nonspecific musculoskeletal strains, herniated discs, compressed nerve roots, degenerative discs or joint disease, and broken vertebra), non-mechanical back pain (tumors, inflammatory conditions such as spondyloarthritis, and infections), and referred pain from internal organs (gallbladder disease, kidney stones, kidney infections, and aortic aneurysm, among others).[5] Mechanical or musculoskeletal problems underlie most cases (around 90% or more),[5][41] and of those, most (around 75%) do not have a specific cause identified, but are thought to be due to muscle strain or injury to ligaments.[5][41] Rarely, complaints of low back pain result from systemic or psychological problems, such as fibromyalgia and somatoform disorders.[41]
Low back pain may be classified based on the signs and symptoms. Diffuse pain that does not change in response to particular movements, and is localized to the lower back without radiating beyond the buttocks, is classified as nonspecific, the most common classification.[5] Pain that radiates down the leg below the knee, is located on one side (in the case of disc herniation), or is on both sides (in spinal stenosis), and changes in severity in response to certain positions or maneuvers is radicular, making up 7% of cases.[5] Pain that is accompanied by red flags such as trauma, fever, a history of cancer or significant muscle weakness may indicate a more serious underlying problem and is classified as needing urgent or specialized attention.[5]
The symptoms can also be classified by duration as acute, sub-chronic (also known as sub-acute), or chronic. The specific duration required to meet each of these is not universally agreed upon, but generally pain lasting less than six weeks is classified as acute, pain lasting six to twelve weeks is sub-chronic, and more than twelve weeks is chronic.[3] Management and prognosis may change based on the duration of symptoms.
Red flags
[edit]| Red flag[42] | Possible cause[1] |
|---|---|
| Previous history of cancer | Cancer |
| Unintentional weight loss | |
| Loss of bladder or bowel control | Cauda equina syndrome |
| Significant motor weakness or sensory problems | |
| Loss of sensation in the buttocks (saddle anesthesia) | |
| Significant trauma related to age | Fracture |
| Chronic corticosteroid use | |
| Osteoporosis | |
| Severe pain after lumbar surgery in past year |
Infection |
| Fever | |
| Urinary tract infection | |
| Immunosuppression | |
| Intravenous drug use |
The presence of certain signs, termed red flags, indicate the need for further testing to look for more serious underlying problems, which may require immediate or specific treatment.[5][43] The presence of a red flag does not mean that there is a significant problem. It is only suggestive,[44][45] and most people with red flags have no serious underlying problem.[3][1] If no red flags are present, performing diagnostic imaging or laboratory testing in the first four weeks after the start of the symptoms has not been shown to be useful.[5]
The usefulness of many red flags is poorly supported by evidence.[46][44] The most useful for detecting a fracture are: older age, corticosteroid use, and significant trauma especially if it results in skin markings.[46] The best determinant of the presence of cancer is a history of the same.[46]
With other causes ruled out, people with non-specific low back pain are typically treated symptomatically, without exact determination of the cause.[3][1] Efforts to uncover factors that might complicate the diagnosis, such as depression, substance abuse, or an agenda concerning insurance payments may be helpful.[5]
Tests
[edit]Imaging is indicated when there are red flags, ongoing neurological symptoms that do not resolve, or ongoing or worsening pain.[5] In particular, early use of imaging (either MRI or CT) is recommended for suspected cancer, infection, or cauda equina syndrome.[5] MRI is slightly better than CT for identifying disc disease; the two technologies are equally useful for diagnosing spinal stenosis.[5] Only a few physical diagnostic tests are helpful.[5] The straight leg raise test is almost always positive in those with disc herniation,[5] and lumbar provocative discography may be useful to identify a specific disc causing pain in those with chronic high levels of low back pain.[47] Therapeutic procedures such as nerve blocks can also be used to determine a specific source of pain.[5] Some evidence supports the use of facet joint injections, transforminal epidural injections and sacroiliac injections as diagnostic tests.[5] Most other physical tests, such as evaluating for scoliosis, muscle weakness or wasting, and impaired reflexes, are of little use.[5]
Complaints of low back pain are one of the most common reasons people visit doctors.[48][49] For pain that has lasted only a few weeks, the pain is likely to subside on its own.[50] Thus, if a person's medical history and physical examination do not suggest a specific disease as the cause, medical societies advise against imaging tests such as X-rays, CT scans, and MRIs.[49] Individuals may want such tests but, unless red flags are present,[51][52] they are unnecessary health care.[48][50] Routine imaging increases costs, is associated with higher rates of surgery with no overall benefit,[53][54] and the radiation used may be harmful to one's health.[53] Fewer than 1% of imaging tests identify the cause of the problem.[48] Imaging may also detect harmless abnormalities, encouraging people to request further unnecessary testing or to worry.[48] Even so, MRI scans of the lumbar region increased by more than 300% among United States Medicare beneficiaries from 1994 to 2006.[10]
Prevention
[edit]Exercise is recommended when experiencing non-specific lower back pain (LBP). The most effective way to decrease pain intensity is by focusing on trunk, pelvic, and leg stretching. Relaxation and postural exercise are not effective in reducing the pain intensity.[55]
Exercise alone, or along with education, appears to be useful for preventing low back pain.[56][57] Exercise is also probably effective in preventing recurrences in those with pain that has lasted more than six weeks.[58] Assessing chronic low back pain, a 2007 review concluded that a firm mattress is less likely to alleviate pain compared to a medium-firm mattress,[59] while a 2020 review stated that studies have been inadequate to comment on mattress firmness.[60] There is little to no evidence that back belts are any more helpful in preventing low back pain than education about proper lifting techniques.[56][57] Shoe insoles do not help prevent low back pain.[56][61][57]
Studies have proven that interventions aimed to reduce pain and functional disability need to be accompanied by psychological interventions to improve a patient's motivation and attitude toward their recovery. Education about an injury and how it can effect a person's mental health is just as important as the physical rehabilitation. However, all of these interventions should occur in partnership with a structured therapeutic exercise program and assistance from a trained physical therapist.[12]
Management
[edit]Most people with acute or subacute low back pain improve over time no matter the treatment.[6] There is often improvement within the first month.[6] Although fear in those suffering from low back pain often leads to avoiding activity, this is found to lead to greater disability.[57] The recommendations include remaining active, avoiding activity that worsen the pain, and understanding self-care of the symptoms.[6] Management of low back pain depends on which of the three general categories is the cause: mechanical problems, non-mechanical problems, or referred pain.[62] For acute pain that is causing only mild to moderate problems, the goals are to restore normal function, return the individual to work, and minimize pain. The condition is normally not serious, resolves without much being done, and recovery is helped by attempting to return to normal activities as soon as possible within the limits of pain.[3] Providing individuals with coping skills through reassurance of these facts is useful in speeding recovery.[1]
For those with sub-chronic or chronic low back pain, multidisciplinary treatment programs may help.[63] For chronic lower back pain, initial management with non–medication based treatments is recommended[6] Non–medication based treatments include exercise, multidisciplinary rehabilitation, acupuncture, mindfulness-based stress reduction, tai chi, yoga, motor control exercise, and progressive relaxation.[6] If these are not sufficiently effective, NSAIDs are recommended.[6] Acetaminophen and systemic steroids are not recommended as both medications are not effective at improving pain outcomes in acute or subacute low back pain.[6]
Physical therapy stabilization exercises for lumbar spine and manual therapy have shown decrease in pain symptoms in patients. Manual therapy and stabilization effects have similar effects on low back pain which overweighs the effects of general exercises.[64] The most effective types of exercise to improve low back pain symptoms are core strengthening and mixed exercise types. An appropriate type of exercise recommended is an aerobic exercise program for 12 hours of exercise over a duration of 8 weeks.[65]
Distress due to low back pain contributes significantly to overall pain and disability experienced. Therefore, treatment strategies that aim to change beliefs and behaviours, such as cognitive-behavioural therapy can be of use.[57]
Access to care as recommended in medical guidelines varies considerably from the care that most people with low back pain receive globally. This is due to factors such as availability, access and payment models (e.g. insurance, health-care systems).[66]
Physical management
[edit]Management of acute low back pain
[edit]Increasing general physical activity has been recommended, but no clear relationship to pain, disability or returning to work occurred when used for treating an acute episode of pain.[58][67][68] For acute pain, low- to moderate-quality evidence supports walking.[69] Aerobic exercise, such as progressive walking, appears useful for subacute and acute low back pain, is strongly recommended for chronic low back pain, and is recommended after surgery.[60] Directional exercises, which try to limit low back pain, are recommended in sub-acute, chronic and radicular low back pain. These exercises only work if they are limiting low back pain.[60] Exercise programs that incorporate stretching only are not recommended for acute low back pain. Stretching, especially with limited range of motion, can impede future progression of treatment from strength exercises.[60] Yoga and Tai chi are not recommended for acute or subacute low back pain, but are recommended for chronic back pain.[60] A 2023 review of low-quality studies concluded that exercise therapy of six weeks or less for low back pain had no clinical benefit.[70]
Treatment according to the McKenzie method is somewhat effective for recurrent acute low back pain, but its benefit in the short term does not appear significant.[1] There is tentative evidence to support the use of heat therapy for acute and sub-chronic low back pain,[71] but little evidence for the use of either heat or cold therapy in chronic pain.[72] Weak evidence suggests that back belts might decrease the number of missed workdays, but there is nothing to suggest that they help with the pain.[73] Ultrasound and shock wave therapies do not appear effective and therefore are not recommended.[74][75] Lumbar traction lacks effectiveness as an intervention for radicular low back pain.[76] It is also unclear whether lumbar supports are an effective treatment intervention.[77]
Management of chronic low back pain
[edit]Physical therapy is effective in decreasing pain and improving physical function, trunk muscle strength, and the mental health for those with chronic low back pain.[78] It also improves long-term function[72] and appears to reduce recurrence rates for as long as six months after the completion of the program.[79] The observed treatment effect for exercise when compared to no treatment, usual care or placebo, improved pain (low‐certainty evidence), but improvements were small for functional limitations (moderate‐certainty evidence).[78] There is no evidence that one particular type of exercise therapy is more effective than another,[80][81] so the form of exercise used can be based on preference, availability and cost.
The Alexander technique appears useful for chronic back pain,[82] and there is some evidence to support small benefits from the use of yoga.[83][84] Motor control exercise, which involves guided movement and use of normal muscles during simple tasks building to more complex tasks, improves pain and function up to 20 weeks, but there was little difference compared to manual therapy and other forms of exercise.[85] Motor control exercise accompanied by manual therapy also produces similar reductions in pain intensity when compared to general strength and condition exercise training, yet only the latter improved muscle endurance and strength, while concurrently decreasing self-reported disability.[86] Aquatic therapy is recommended as an option in those with other preexisting conditions like extreme obesity, degenerative joint disease, or other conditions that limit progressive walking. Aquatic therapy is not recommended for people with no preexisting condition that limits their progressive walking.[60] There is low-to-moderate quality evidence that supports pilates in low back pain for the reduction of pain and disability,[60][87] although there is no conclusive evidence that pilates is better than any other form of exercise for low back pain.[87]
People with chronic low back pain receiving multidisciplinary biopsychosocial rehabilitation programs may have less pain and disability than those receiving typical care or physiotherapy.[88]
Peripheral nerve stimulation, a minimally-invasive procedure, may be useful in cases of chronic low back pain that do not respond to other measures, although the evidence supporting it is not conclusive, and it is not effective for pain that radiates into the leg.[89] Evidence for the use of shoe insoles as a treatment is inconclusive.[61] Transcutaneous electrical nerve stimulation has not been found to be effective in chronic low back pain.[90] There has been little research that supports the use of lumbar extension machines and thus they are not recommended.[60]
Medications
[edit]If initial management with non–medication based treatments is insufficient, medication may be recommended.[6] As pain medications are only somewhat effective, expectations regarding their benefit may differ from reality, and this can lead to decreased satisfaction.[19]
The medication typically prescribed first are acetaminophen (paracetamol), NSAIDs (though not aspirin), or skeletal muscle relaxants and these are enough for most people.[91][19][6][92] Benefits with NSAIDs is thought to be small,[93][94] but is more effective than Acetaminophen (paracetamol), which may be no more effective than placebo at improving pain, quality of life, or function.[95][96] For adults with both acute and chronic lower back pain, NSAIDs can also reduce disability.[91] NSAIDs however, carry a greater risk of side effects, including kidney failure, stomach ulcers and possibly heart problems, so it is used at the lowest effective dosage for the shortest possible time.[57] NSAIDs are available in several different classes; there is no evidence to support the use of COX-2 inhibitors over any other class of NSAIDs with respect to benefits.[93][19][97] With respect to safety naproxen may be best.[98] Muscle relaxants may be minimally beneficial.[19] Muscle relaxants and benzodiazepines are shown to have small benefits compared to placebo for pain relief for acute lower back pain, and a higher chance of improving physical function. However they also come with an increased risk of adverse events. For chronic back pain, there may be a benefit in regards to use of benzodiazepines, with muscle relaxants in this context showing low-certainty evidence for no adverse reaction compared to placebo.[91]
Systemic corticosteriods are sometimes suggested for low back pain and may have a small benefit in the short-term for radicular low back pain, however, the benefit for non-radicular back pain and the optimal dose and length of treatment is unclear.[99]
As of 2022, the CDC has released a guideline for prescribed opioid use in the management of chronic pain.[15] It states that opioid use is not the preferred treatment when managing chronic pain due to the excessive risks involved, including high risks of addiction, accidental overdose and death.[16]
In chronic back pain, there's high-certainty evidence that tapentadol offers a small reduction in pain compared to placebo, and moderate-certainty evidence for a small benefit from strong opioids in reducing both pain and disability. Tramadol also shows low to moderate-certainty evidence for small reductions in pain and disability, while buprenorphine has very low to low-certainty evidence for similar small benefits. Overall, opioid use is associated with a low-certainty increased risk of adverse events like nausea, headaches, constipation, and dizziness.[91] Specialist groups advise against general long-term use of opioids for chronic low back pain.[19][100] If the pain is not managed adequately, short-term use of opioids such as morphine may be suggested,[101][19] although low back pain outcomes are poorer in the long-term.[57] If prescribed, a person and their clinician should have a realistic plan to discontinue its use in the event that the risks outweigh the benefit.[102] These medications carry a risk of addiction, may have negative interactions with other drugs, and have a greater risk of side effects, including dizziness, nausea, and constipation.[19] Opioid treatment for chronic low back pain increases the risk for lifetime illicit drug use[103] and the effect of long-term use of opioids for lower back pain is unknown.[104] For older people with chronic pain, opioids may be used in those for whom NSAIDs present too great a risk, including those with diabetes, stomach or heart problems. They may also be useful for a select group of people with neuropathic pain.[105]
SNRI antidepressants may have small effects on chronic low back pain, but are associated with adverse effects. Evidence is lacking for the use of SSRIs and tricyclic antidepressants.[106][91] Although the antiseizure drugs gabapentin, pregabalin, and topiramate are sometimes used for chronic low back pain evidence does not support a benefit.[107] Systemic oral steroids have not been shown to be useful in low back pain.[1][19] Facet joint injections and steroid injections into the discs have not been found to be effective in those with persistent, non-radiating pain; however, they may be considered for those with persistent sciatic pain.[108] Epidural corticosteroid injections provide a slight and questionable short-term improvement in those with sciatica but are of no long-term benefit.[109] There are also concerns of potential side effects.[110]
Surgery
[edit]Surgery may be useful in those with a herniated disc that is causing significant pain radiating into the leg, significant leg weakness, bladder problems, or loss of bowel control.[17] It may also be useful in those with spinal stenosis.[18] In the absence of these issues, there is no clear evidence of a benefit from surgery.[17]
Discectomy (the partial removal of a disc that is causing leg pain) can provide pain relief sooner than nonsurgical treatments.[17] Discectomy has better outcomes at one year but not at four to ten years.[17] The less invasive microdiscectomy has not been shown to result in a different outcome than regular discectomy.[17] For most other conditions, there is not enough evidence to provide recommendations for surgical options.[17] The long-term effect surgery has on degenerative disc disease is not clear.[17] Less invasive surgical options have improved recovery times, but evidence regarding effectiveness is insufficient.[17]
For those with pain localized to the lower back due to disc degeneration, fair evidence supports spinal fusion as equal to intensive physical therapy and slightly better than low-intensity nonsurgical measures.[18] Fusion may be considered for those with low back pain from acquired displaced vertebra that does not improve with conservative treatment,[17] although only a few of those who have spinal fusion experience good results,[18] and there may be no clinically important difference between disk replacement and fusion surgery.[111] There are a number of different surgical procedures to achieve fusion, with no clear evidence of one being better than the others.[112] Adding spinal implant devices during fusion increases the risk but provides no added improvement in pain or function.[10] Spinal cord stimulation using implanted electrodes is not supported by evidence due to the potential risks and costs.[113]
Alternative medicine
[edit]It is unclear if alternative treatments are useful for non-chronic back pain.[114] Chiropractic care or spinal manipulation therapy (SMT) appear similarly effective to other recommended treatments.[115][116][24] National guidelines differ, with some not recommending SMT, some describing manipulation as optional, and others recommending a short course for those who do not improve with other treatments.[3] A 2017 review recommended SMT based on low-quality evidence.[6] There is insufficient evidence to recommend manipulation under anaesthesia, or medically assisted manipulation.[117] SMT does not provide significant benefits compared to motor control exercises.[118]
The evidence supporting acupuncture treatment for providing clinically beneficial acute and chronic pain relief is very weak.[119] When compared to a 'sham' treatment, no differences in pain relief or improvements in a person's quality of life were found.[119] There is very weak evidence that acupuncture may be better than no treatment at all for immediate relief.[119] A 2012 systematic review reported the findings that for people with chronic pain, acupuncture may improve pain a little more than no treatment and about the same as medications, but it does not help with disability.[120] This pain benefit is only present right after treatment and not at follow-up.[120] Acupuncture may be an option for those with chronic pain that does not respond to other treatments like conservative care and medications,[1][121] however this depends on patient preference, the cost, and on how accessible acupuncture is for the person.[119]
Massage therapy does not appear to provide much benefit for acute low back pain.[1] Massage therapy has been found to be more effective for acute low back pain than no treatment; the benefits were found to be limited to the short term[122] and there was no effect for improving function.[122] For chronic low back pain, massage therapy was better than no treatment for both pain and function, though only in the short-term.[122] The overall quality of the evidence was low and the authors had no confidence that massage therapy is an effective treatment for low back pain.[122] Massage therapy is recommended for selected people with subacute and chronic low back pain, but it should be paired with another form of treatment like aerobic or strength exercises. For acute or chronic radicular pain syndromes massage therapy is recommended only if low back pain is considered a symptom. Mechanical massage tools are not recommended for the treatment of any form of low back pain.[60]
Prolotherapy – the practice of injecting solutions into joints (or other areas) to cause inflammation and thereby stimulate the body's healing response – has not been found to be effective by itself, although it may be helpful when added to another therapy.[21]
Herbal medicines, as a whole, are poorly supported by evidence.[123] The herbal treatments Devil's claw and white willow may reduce the number of individuals reporting high levels of pain; however, for those taking pain relievers, this difference is not significant.[21] Capsicum, in the form of either a gel or a plaster cast, has been found to reduce pain and increase function.[21]
Behavioral therapy may be useful for chronic pain.[20] There are several types available, including operant conditioning, which uses reinforcement to reduce undesirable behaviors and increase desirable behaviors; cognitive behavioral therapy, which helps people identify and correct negative thinking and behavior; and respondent conditioning, which can modify an individual's physiological response to pain.[21] The benefit however is small.[124] Medical providers may develop an integrated program of behavioral therapies.[21] The evidence is inconclusive as to whether mindfulness-based stress reduction reduces chronic back pain intensity or associated disability, although it suggests that it may be useful in improving the acceptance of existing pain.[125][126]
Tentative evidence supports neuroreflexotherapy (NRT), in which small pieces of metal are placed just under the skin of the ear and back, for non-specific low back pain.[127][128][21] Multidisciplinary biopsychosocial rehabilitation (MBR), targeting physical and psychological aspects, may improve back pain but evidence is limited.[129] There is a lack of good quality evidence to support the use of radiofrequency denervation for pain relief.[130]
KT Tape has been found to be no different for management of chronic non-specific low back pain than other established pain management strategies.[131]
Education
[edit]There is strong evidence that education may improve low back pain, with a 2.5 hour educational session more effective than usual care for helping people return to work in the short- and long-term. This was more effective for people with acute rather than chronic back pain.[132] The benefit of training for preventing back pain in people who work manually with materials is not clear, however moderate quality evidence does not show a role in preventing back pain.[133]
Prognosis
[edit]Overall, the outcome for acute low back pain is positive. Pain and disability usually improve a great deal in the first six weeks, with complete recovery reported by 40 to 90%.[2] In those who still have symptoms after six weeks, improvement is generally slower with only small gains up to one year. At one year, pain and disability levels are low to minimal in most people. Distress, previous low back pain, and job satisfaction are predictors of long-term outcome after an episode of acute pain.[2] Certain psychological problems such as depression, or unhappiness due to loss of employment may prolong the episode of low back pain.[19] Following a first episode of back pain, recurrences occur in more than half of people.[28]
For persistent low back pain, the short-term outcome is also positive, with improvement in the first six weeks but very little improvement after that. At one year, those with chronic low back pain usually continue to have moderate pain and disability.[2] People at higher risk of long-term disability include those with poor coping skills or with fear of activity (2.5 times more likely to have poor outcomes at one year),[134] those with a poor ability to cope with pain, functional impairments, poor general health, or a significant psychiatric or psychological component to the pain (Waddell's signs).[134]
Prognosis may be influenced by expectations, with those having positive expectations of recovery related to higher likelihood of returning to work and better recovery outcomes.[135]
Epidemiology
[edit]Low back pain that lasts at least one day and limits activity is a common complaint.[7] Globally, about 40% of people have low back pain at some point in their lives,[7] with estimates as high as 80% of people in the developed world.[27] Approximately 9 to 12% of people (632 million) have low back pain at any given point in time, which was calculated to 7460 per 100,000 globally in 2020.[26] Nearly one quarter (23.2%) report having it at some point over any one-month period.[7][8] Difficulty most often begins between 20 and 40 years of age.[1] However, low back pain becomes increasingly common with age, and is most common in the age group of 85.[26] Older adults more greatly affected by low back pain; they are more likely to lose mobility and independence and less likely to continue to participate in social and family activities.[26]
Women have higher rates of low back pain than men within all age groups, and this difference becomes more marked in older age groups (above 75 years).[26] In a 2012 review which found a higher rate in females than males, the reviewers thought this may be attributable to greater rates of pains due to osteoporosis, menstruation, and pregnancy among women, or possibly because women were more willing to report pain than men.[7] An estimated 70% of women experience back pain during pregnancy with the rate being higher the further along in pregnancy.[136]
Although the majority of low back pain has no specific underlying cause, workplace ergonomics, smoking and obesity are associated with low back pain in approximately 30% of cases.[26] Low levels of activity is also associated with low back pain.[57] Workplace ergonomics associated with low back pain include lifting, bending, vibration and physically demanding work, as well as prolonged sitting, standing and awkward postures.[26] Current smokers – and especially those who are adolescents – are more likely to have low back pain than former smokers, and former smokers are more likely to have low back pain than those who have never smoked.[137]
The overall number of individuals affected expected to increase with population growth and as the population ages,[26] with the largest increases expected in low- and middle-income countries.[57]
History
[edit]
Humans have suffered low-back pain since at least the Bronze Age. The oldest-known surgical treatise – the Edwin Smith Papyrus from ancient Egypt, dating to about 1500 BCE – describes a diagnostic test and treatment for a vertebral sprain. Hippocrates (c. 460 BCE – c. 370 BCE) was the first to use a term for sciatic pain and low-back pain; Galen (active mid to late second century CE) described the concept in some detail. Physicians through the end of the first millennium recommended watchful waiting. Through the Medieval period, folk-medicine practitioners provided treatments for back pain based on the belief that it was caused by spirits.[138] English-speakers adopted the Latin term lumbago (as "lumbaga", defined as "a Pain in the Muscles of the Loins") from as early as 1684.[139]
At the start of the 20th century, physicians thought that low-back pain was caused by inflammation of or damage to the nerves,[138] with neuralgia and neuritis frequently mentioned by them in the medical literature of the time.[140] The popularity of such proposed explanations decreased during the 20th century.[140] In the early-20th century, American neurosurgeon Harvey Williams Cushing (1869-1939) increased the acceptance of surgical treatments for low-back pain.[17] In the 1920s and 1930s, new theories of the cause arose, with physicians proposing a combination of nervous-system and psychological disorders such as nerve weakness (neurasthenia) and female hysteria.[138] Muscular rheumatism (now called fibromyalgia) was also cited with increasing frequency.[140]
Emerging technologies such as X-rays gave physicians new diagnostic tools, revealing the intervertebral disc as a source for back pain in some cases. In 1938, orthopedic surgeon Joseph S. Barr reported on cases of disc-related sciatica improved or cured with back surgery.[140] As a result of this work, in the 1940s, the vertebral-disc model of low-back pain took over,[138] dominating the literature through the 1980s, aided further by the rise of new imaging-technologies such as CT and MRI.[140] The discussion subsided as research showed disc problems to be a relatively uncommon cause of the pain. Since then, physicians have come to realize that it is unlikely that a specific cause for low-back pain can be identified in many cases, and question the need to find one at all — as most of the time symptoms resolve within 6 to 12 weeks regardless of treatment.[138] Modern treatment may devolve on physiotherapists.[141]
Society and culture
[edit]Low back pain results in large economic costs. In the United States, it is the most common type of pain in adults, responsible for a large number of missed work days, and is the most common musculoskeletal complaint seen in the emergency department.[30] In 1998, it was estimated to be responsible for $90 billion in annual health care costs, with 5% of individuals incurring most (75%) of the costs.[30] Between 1990 and 2001 there was a more than twofold increase in spinal fusion surgeries in the US, despite the fact that there were no changes to the indications for surgery or new evidence of greater usefulness.[10] Further costs occur in the form of lost income and productivity, with low back pain responsible for 40% of all missed work days in the United States.[142] Low back pain causes disability in a larger percentage of the workforce in Canada, Great Britain, the Netherlands and Sweden than in the US or Germany.[142] In the United States, low back pain is highest of Years Lived With Disability (YLDs) rank, rate, and percentage change[failed verification] for the 25 leading causes of disability and injury, between 1990 and 2016.[143]
Workers who experience acute low back pain as a result of a work injury may be asked by their employers to have x-rays.[144] As in other cases, testing is not indicated unless red flags are present.[144] An employer's concern about legal liability is not a medical indication and should not be used to justify medical testing when it is not indicated.[144] There should be no legal reason for encouraging people to have tests which a health care provider determines are not indicated.[144]
Research
[edit]Total disc replacement is an experimental option,[39] but no significant evidence supports its use over lumbar fusion.[17] Researchers are investigating the possibility of growing new intervertebral structures through the use of injected human growth factors, implanted substances, cell therapy, and tissue engineering.[39]
References
[edit]- ^ a b c d e f g h i j k l m n o p q Casazza BA (February 2012). "Diagnosis and treatment of acute low back pain". American Family Physician. 85 (4): 343–350. PMID 22335313.
- ^ a b c d e f g h da C Menezes Costa L, Maher CG, Hancock MJ, McAuley JH, Herbert RD, Costa LO (August 2012). "The prognosis of acute and persistent low-back pain: a meta-analysis". CMAJ. 184 (11): E613 – E624. doi:10.1503/cmaj.111271. PMC 3414626. PMID 22586331.
- ^ a b c d e f g h Koes BW, van Tulder M, Lin CW, Macedo LG, McAuley J, Maher C (December 2010). "An updated overview of clinical guidelines for the management of non-specific low back pain in primary care". European Spine Journal. 19 (12): 2075–2094. doi:10.1007/s00586-010-1502-y. PMC 2997201. PMID 20602122.
- ^ a b c "Low Back Pain Fact Sheet". National Institute of Neurological Disorders and Stroke. 3 November 2015. Archived from the original on 4 March 2016. Retrieved 5 March 2016.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x Manusov EG (September 2012). "Evaluation and diagnosis of low back pain". Primary Care. 39 (3): 471–479. doi:10.1016/j.pop.2012.06.003. PMID 22958556.
- ^ a b c d e f g h i j k l m n Qaseem A, Wilt TJ, McLean RM, Forciea MA, Denberg TD, Barry MJ, et al. (April 2017). "Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline From the American College of Physicians". Annals of Internal Medicine. 166 (7): 514–530. doi:10.7326/M16-2367. PMID 28192789.
- ^ a b c d e f g h Hoy D, Bain C, Williams G, March L, Brooks P, Blyth F, et al. (June 2012). "A systematic review of the global prevalence of low back pain". Arthritis and Rheumatism. 64 (6): 2028–2037. doi:10.1002/art.34347. PMID 22231424.
- ^ a b c Vos T, Flaxman AD, Naghavi M, Lozano R, Michaud C, Ezzati M, et al. (December 2012). "Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010". Lancet. 380 (9859): 2163–2196. doi:10.1016/S0140-6736(12)61729-2. PMC 6350784. PMID 23245607.
- ^ American Academy of Family Physicians, Choosing Wisely (2023). "Imaging for Low Back Pain". aafp.org. Retrieved 21 July 2023.
- ^ a b c d Deyo RA, Mirza SK, Turner JA, Martin BI (2009). "Overtreating chronic back pain: time to back off?". Journal of the American Board of Family Medicine. 22 (1): 62–68. doi:10.3122/jabfm.2009.01.080102. PMC 2729142. PMID 19124635.
- ^ a b c d e Salzberg L (September 2012). "The physiology of low back pain". Primary Care. 39 (3): 487–498. doi:10.1016/j.pop.2012.06.014. PMID 22958558.
- ^ a b Herrero P, Val P, Lapuente-Hernández D, Cuenca-Zaldívar JN, Calvo S, Gómez-Trullén EM (20 February 2024). "Effects of Lifestyle Interventions on the Improvement of Chronic Non-Specific Low Back Pain: A Systematic Review and Network Meta-Analysis". Healthcare. 12 (5): 505. doi:10.3390/healthcare12050505. ISSN 2227-9032. PMC 10931043. PMID 38470617.
- ^ a b c WHO guideline for non-surgical management of chronic primary low back pain in adults in primary and community care settings. World Health Organization. 2023. ISBN 978-92-4-008178-9.
- ^ Cashin AG, Wand BM, O'Connell NE, Lee H, Rizzo RR, Bagg MK, O'Hagan E, Maher CG, Furlan AD, van Tulder MW, McAuley JH (4 April 2023). "Pharmacological treatments for low back pain in adults: an overview of Cochrane Reviews". The Cochrane Database of Systematic Reviews. 2023 (4) CD013815. doi:10.1002/14651858.CD013815.pub2. ISSN 1469-493X. PMC 10072849. PMID 37014979.
- ^ a b Dowell D, Ragan KR, Jones CM, Baldwin GT, Chou R (November 2022). "CDC Clinical Practice Guideline for Prescribing Opioids for Pain – United States, 2022". MMWR. Recommendations and Reports. 71 (3): 1–95. doi:10.15585/mmwr.rr7103a1. PMC 9639433. PMID 36327391.
- ^ a b Deyo RA, Von Korff M, Duhrkoop D (January 2015). "Opioids for low back pain". BMJ. 350 (jan05 10) g6380. doi:10.1136/bmj.g6380. PMC 6882374. PMID 25561513.
- ^ a b c d e f g h i j k l m Manusov EG (September 2012). "Surgical treatment of low back pain". Primary Care. 39 (3): 525–531. doi:10.1016/j.pop.2012.06.010. PMID 22958562.
- ^ a b c d Chou R, Baisden J, Carragee EJ, Resnick DK, Shaffer WO, Loeser JD (May 2009). "Surgery for low back pain: a review of the evidence for an American Pain Society Clinical Practice Guideline". Spine. 34 (10): 1094–1109. doi:10.1097/BRS.0b013e3181a105fc. PMID 19363455. S2CID 1504909.
- ^ a b c d e f g h i j k Miller SM (September 2012). "Low back pain: pharmacologic management". Primary Care. 39 (3): 499–510. doi:10.1016/j.pop.2012.06.005. PMID 22958559.
- ^ a b Henschke N, Ostelo RW, van Tulder MW, Vlaeyen JW, Morley S, Assendelft WJ, Main CJ (July 2010). "Behavioural treatment for chronic low-back pain". The Cochrane Database of Systematic Reviews. 2011 (7) CD002014. doi:10.1002/14651858.CD002014.pub3. PMC 7065591. PMID 20614428.
- ^ a b c d e f g h i Marlowe D (September 2012). "Complementary and alternative medicine treatments for low back pain". Primary Care. 39 (3): 533–546. doi:10.1016/j.pop.2012.06.008. PMID 22958563.
- ^ Walker BF, French SD, Grant W, Green S (February 2011). "A Cochrane review of combined chiropractic interventions for low-back pain". Spine. 36 (3): 230–242. doi:10.1097/BRS.0b013e318202ac73. PMID 21248591. S2CID 26310171.
- ^ Dagenais S, Gay RE, Tricco AC, Freeman MD, Mayer JM (October 2010). "NASS Contemporary Concepts in Spine Care: spinal manipulation therapy for acute low back pain". The Spine Journal. 10 (10): 918–940. doi:10.1016/j.spinee.2010.07.389. PMID 20869008.
- ^ a b Rubinstein SM, van Middelkoop M, Assendelft WJ, de Boer MR, van Tulder MW (February 2011). Rubinstein SM (ed.). "Spinal manipulative therapy for chronic low-back pain". The Cochrane Database of Systematic Reviews. 2013 (2) CD008112. doi:10.1002/14651858.CD008112.pub2. hdl:1887/117578. PMC 12009663. PMID 21328304.
- ^ Rubinstein SM, Terwee CB, Assendelft WJ, de Boer MR, van Tulder MW (September 2012). "Spinal manipulative therapy for acute low-back pain". The Cochrane Database of Systematic Reviews. 9 (9) CD008880. doi:10.1002/14651858.CD008880.pub2. hdl:1871/48563. PMC 6885055. PMID 22972127.
- ^ a b c d e f g h i Ferreira ML, de Luca K, Haile LM, Steinmetz JD, Culbreth GT, Cross M, et al. (GBD 2021 Low Back Pain Collaborators) (June 2023). "Global, regional, and national burden of low back pain, 1990-2020, its attributable risk factors, and projections to 2050: a systematic analysis of the Global Burden of Disease Study 2021". The Lancet. Rheumatology. 5 (6): e316 – e329. doi:10.1016/S2665-9913(23)00098-X. PMC 10234592. PMID 37273833.
- ^ a b Vinod Malhotra, Yao, Fun-Sun F., Fontes, Manuel da Costa (2011). Yao and Artusio's Anesthesiology: Problem-Oriented Patient Management. Hagerstwon, MD: Lippincott Williams & Wilkins. pp. Chapter 49. ISBN 978-1-4511-0265-9. Archived from the original on 8 September 2017.
- ^ a b Stanton TR, Latimer J, Maher CG, Hancock MJ (April 2010). "How do we define the condition 'recurrent low back pain'? A systematic review". European Spine Journal. 19 (4): 533–539. doi:10.1007/s00586-009-1214-3. PMC 2899839. PMID 19921522.
- ^ Kelly GA, Blake C, Power CK, O'keeffe D, Fullen BM (February 2011). "The association between chronic low back pain and sleep: a systematic review". The Clinical Journal of Pain. 27 (2): 169–181. doi:10.1097/AJP.0b013e3181f3bdd5. PMID 20842008. S2CID 19569862.
- ^ a b c d e f Borczuk P (July 2013). "An evidence-based approach to the evaluation and treatment of low back pain in the emergency department". Emergency Medicine Practice. 15 (7): 1–23, Quiz 23–24. PMID 24044786. Archived from the original on 14 August 2013.
- ^ a b "Low Back Pain Fact Sheet". National Institute of Neurological Disorders and Stroke. National Institute of Health. Archived from the original on 19 July 2013. Retrieved 12 July 2013.
- ^ Swain CT, Pan F, Owen PJ, Schmidt H, Belavy DL (March 2020). "No consensus on causality of spine postures or physical exposure and low back pain: A systematic review of systematic reviews". Journal of Biomechanics. 102: 109312. doi:10.1016/j.jbiomech.2019.08.006. PMID 31451200. S2CID 201756091.
- ^ "Fast Facts About Back Pain". National Institute of Arthritis and Musculoskeletal and Skin Diseases. National Institute of Health. September 2009. Archived from the original on 5 June 2013. Retrieved 10 June 2013.
- ^ "Low back pain – acute". U.S. Department of Health and Human Services – National Institutes of Health. Archived from the original on 1 April 2013. Retrieved 1 April 2013.
- ^ Majchrzycki M, Mrozikiewicz PM, Kocur P, Bartkowiak-Wieczorek J, Hoffmann M, Stryła W, et al. (November 2010). "[Low back pain in pregnant women]". Ginekologia Polska (in Polish). 81 (11): 851–855. PMID 21365902.
- ^ Lane DR, Takhar SS (August 2011). "Diagnosis and management of urinary tract infection and pyelonephritis". Emergency Medicine Clinics of North America. 29 (3): 539–552. doi:10.1016/j.emc.2011.04.001. PMID 21782073.
- ^ Floyd, R., & Thompson, Clem. (2008). Manual of structural kinesiology. New York: McGraw-Hill Humanities/Social Sciences/Languages. [ISBN missing][page needed]
- ^ a b c Freeman MD, Woodham MA, Woodham AW (February 2010). "The role of the lumbar multifidus in chronic low back pain: a review". PM & R. 2 (2): 142–6, quiz 1 p following 167. doi:10.1016/j.pmrj.2009.11.006. PMID 20193941. S2CID 22246810.
- ^ a b c d e f g Hughes SP, Freemont AJ, Hukins DW, McGregor AH, Roberts S (October 2012). "The pathogenesis of degeneration of the intervertebral disc and emerging therapies in the management of back pain" (PDF). The Journal of Bone and Joint Surgery. British Volume. 94 (10): 1298–1304. doi:10.1302/0301-620X.94B10.28986. PMID 23015552. Archived from the original (PDF) on 4 October 2013. Retrieved 25 June 2013.
- ^ Patel NB (2010). "Chapter 3: Physiology of Pain". In Kopf A, Patel NB (eds.). Guide to Pain Management in Low-Resource Settings. Archived from the original on 5 October 2013. Retrieved 26 May 2017.
- ^ a b c Cohen SP, Argoff CE, Carragee EJ (December 2008). "Management of low back pain". BMJ. 337 a2718. doi:10.1136/bmj.a2718. PMID 19103627. S2CID 78716905.
- ^ Davis PC, Wippold II FJ, Cornelius RS, et al. (2011). American College of Radiology ACR Appropriateness Criteria – Low Back Pain (PDF) (Report). Archived from the original (PDF) on 22 December 2012.
- ^ North American Spine Society (February 2013), "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, North American Spine Society, retrieved 25 March 2013, which cites
- Chou R, Qaseem A, Snow V, Casey D, Cross JT, Shekelle P, Owens DK, et al. (Clinical Efficacy Assessment Subcommittee of the American College of Physicians, American College of Physicians, American Pain Society Low Back Pain Guidelines Panel) (October 2007). "Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society". Annals of Internal Medicine. 147 (7): 478–491. doi:10.7326/0003-4819-147-7-200710020-00006. PMID 17909209.
- Forseen SE, Corey AS (October 2012). "Clinical decision support and acute low back pain: evidence-based order sets". Journal of the American College of Radiology. 9 (10): 704–712.e4. doi:10.1016/j.jacr.2012.02.014. PMID 23025864.
- ^ a b Williams CM, Henschke N, Maher CG, van Tulder MW, Koes BW, Macaskill P, Irwig L (28 November 2023). "Red flags to screen for vertebral fracture in patients presenting with low-back pain". The Cochrane Database of Systematic Reviews. 11 (11) CD008643. doi:10.1002/14651858.CD008643.pub3. ISSN 1469-493X. PMC 10683370. PMID 38014846.
- ^ Henschke N, Maher CG, Ostelo RW, de Vet HC, Macaskill P, Irwig L (February 2013). "Red flags to screen for malignancy in patients with low-back pain". The Cochrane Database of Systematic Reviews. 2013 (2) CD008686. doi:10.1002/14651858.CD008686.pub2. PMC 10631455. PMID 23450586.
- ^ a b c Downie A, Williams CM, Henschke N, Hancock MJ, Ostelo RW, de Vet HC, et al. (December 2013). "Red flags to screen for malignancy and fracture in patients with low back pain: systematic review". BMJ. 347 (dec11 1) f7095. doi:10.1136/bmj.f7095. PMC 3898572. PMID 24335669.
- ^ Manchikanti L, Glaser SE, Wolfer L, Derby R, Cohen SP (2009). "Systematic review of lumbar discography as a diagnostic test for chronic low back pain". Pain Physician. 12 (3): 541–559. doi:10.36076/ppj.2009/12/541. PMID 19461822.
- ^ a b c d "Use of imaging studies for low back pain: percentage of members with a primary diagnosis of low back pain who did not have an imaging study (plain x-ray, MRI, CT scan) within 28 days of the diagnosis". 2013. Archived from the original on 4 October 2013. Retrieved 11 June 2013.
- ^ a b American Academy of Family Physicians, "Ten Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American Academy of Family Physicians, archived from the original on 10 February 2013, retrieved 5 September 2012
- ^ a b American College of Physicians, "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American College of Physicians, archived from the original on 1 September 2013, retrieved 5 September 2013
- ^ Chou R, Fu R, Carrino JA, Deyo RA (February 2009). "Imaging strategies for low-back pain: systematic review and meta-analysis". Lancet. 373 (9662): 463–472. doi:10.1016/S0140-6736(09)60172-0. PMID 19200918. S2CID 31602395.
- ^ Crownover BK, Bepko JL (April 2013). "Appropriate and safe use of diagnostic imaging". American Family Physician. 87 (7): 494–501. PMID 23547591.
- ^ a b Chou R, Qaseem A, Owens DK, Shekelle P, et al. (Clinical Guidelines Committee of the American College of Physicians) (February 2011). "Diagnostic imaging for low back pain: advice for high-value health care from the American College of Physicians". Annals of Internal Medicine. 154 (3): 181–189. doi:10.7326/0003-4819-154-3-201102010-00008. PMID 21282698. S2CID 1326352.
- ^ Flynn TW, Smith B, Chou R (November 2011). "Appropriate use of diagnostic imaging in low back pain: a reminder that unnecessary imaging may do as much harm as good". The Journal of Orthopaedic and Sports Physical Therapy. 41 (11): 838–846. doi:10.2519/jospt.2011.3618. PMID 21642763. S2CID 207399397.
- ^ Quentin C, Bagheri R, Ugbolue UC, Coudeyre E, Pélissier C, Descatha A, Menini T, Bouillon-Minois JB, Dutheil F (10 August 2021). "Effect of Home Exercise Training in Patients with Nonspecific Low-Back Pain: A Systematic Review and Meta-Analysis". International Journal of Environmental Research and Public Health. 18 (16): 8430. doi:10.3390/ijerph18168430. ISSN 1660-4601. PMC 8391468. PMID 34444189.
- ^ a b c Steffens D, Maher CG, Pereira LS, Stevens ML, Oliveira VC, Chapple M, et al. (February 2016). "Prevention of Low Back Pain: A Systematic Review and Meta-analysis". JAMA Internal Medicine. 176 (2): 199–208. doi:10.1001/jamainternmed.2015.7431. PMID 26752509.
- ^ a b c d e f g h i Hartvigsen J, Hancock MJ, Kongsted A, Louw Q, Ferreira ML, Genevay S, Hoy D, Karppinen J, Pransky G, Sieper J, Smeets RJ, Underwood M, Buchbinder R, Hartvigsen J, Cherkin D (June 2018). "What low back pain is and why we need to pay attention". The Lancet. 391 (10137): 2356–2367. doi:10.1016/s0140-6736(18)30480-x. hdl:1871.1/79cd95b7-4b74-4c5a-bf1f-adf61bcc71f5. ISSN 0140-6736. PMID 29573870. S2CID 4354991.
- ^ a b Choi BK, Verbeek JH, Tam WW, Jiang JY (January 2010). Choi BK (ed.). "Exercises for prevention of recurrences of low-back pain". The Cochrane Database of Systematic Reviews. 2010 (1) CD006555. doi:10.1002/14651858.CD006555.pub2. PMC 8078403. PMID 20091596.
- ^ Chou R, Qaseem A, Snow V, Casey D, Cross JT, Shekelle P, Owens DK, et al. (Clinical Efficacy Assessment Subcommittee of the American College of Physicians, American College of Physicians, American Pain Society Low Back Pain Guidelines Panel) (October 2007). "Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society". Annals of Internal Medicine. 147 (7): 478–491. doi:10.7326/0003-4819-147-7-200710020-00006. PMID 17909209.
- ^ a b c d e f g h i Hegmann KT, Travis R, Andersson GB, et al. (March 2020). "Non-Invasive and Minimally Invasive Management of Low Back Disorders". Journal of Occupational and Environmental Medicine. 62 (3): e111 – e138. doi:10.1097/JOM.0000000000001812. PMID 31977923.
- ^ a b Sahar T, Cohen MJ, Uval-Ne'eman V, Kandel L, Odebiyi DO, Lev I, et al. (April 2009). "Insoles for prevention and treatment of back pain: a systematic review within the framework of the Cochrane Collaboration Back Review Group". Spine. 34 (9): 924–933. doi:10.1097/BRS.0b013e31819f29be. PMID 19359999. S2CID 22162952.
- ^ Sprouse R (September 2012). "Treatment: current treatment recommendations for acute and chronic undifferentiated low back pain". Primary Care. 39 (3): 481–486. doi:10.1016/j.pop.2012.06.004. PMID 22958557.
- ^ Momsen AM, Rasmussen JO, Nielsen CV, Iversen MD, Lund H (November 2012). "Multidisciplinary team care in rehabilitation: an overview of reviews". Journal of Rehabilitation Medicine. 44 (11): 901–912. doi:10.2340/16501977-1040. PMID 23026978.
- ^ Gomes-Neto M, Lopes JM, Conceição CS, Araujo A, Brasileiro A, Sousa C, et al. (January 2017). "Stabilization exercise compared to general exercises or manual therapy for the management of low back pain: A systematic review and meta-analysis". Physical Therapy in Sport. 23: 136–142. doi:10.1016/j.ptsp.2016.08.004. PMID 27707631.
- ^ Hayden JA, Ellis J, Ogilvie R, Malmivaara A, van Tulder MW (28 September 2021). Cochrane Back and Neck Group (ed.). "Exercise therapy for chronic low back pain". Cochrane Database of Systematic Reviews. 2021 (10) CD009790. doi:10.1002/14651858.CD009790.pub2. PMC 8477273. PMID 34580864.
- ^ Foster NE, Anema JR, Cherkin D, Chou R, Cohen SP, Gross DP, Ferreira PH, Fritz JM, Koes BW, Peul W, Turner JA, Maher CG, Buchbinder R, Hartvigsen J, Cherkin D (2018). "Prevention and treatment of low back pain: evidence, challenges, and promising directions". The Lancet. 391 (10137): 2368–2383. doi:10.1016/s0140-6736(18)30489-6. ISSN 0140-6736. PMID 29573872. S2CID 205989057.
- ^ Hendrick P, Milosavljevic S, Hale L, Hurley DA, McDonough S, Ryan B, Baxter GD (March 2011). "The relationship between physical activity and low back pain outcomes: a systematic review of observational studies". European Spine Journal. 20 (3): 464–474. doi:10.1007/s00586-010-1616-2. PMC 3048226. PMID 21053026.
- ^ Schaafsma FG, Whelan K, van der Beek AJ, van der Es-Lambeek LC, Ojajärvi A, Verbeek JH (August 2013). "Physical conditioning as part of a return to work strategy to reduce sickness absence for workers with back pain". The Cochrane Database of Systematic Reviews. 2013 (8) CD001822. doi:10.1002/14651858.CD001822.pub3. PMC 7074637. PMID 23990391.
- ^ Hendrick P, Te Wake AM, Tikkisetty AS, Wulff L, Yap C, Milosavljevic S (October 2010). "The effectiveness of walking as an intervention for low back pain: a systematic review". European Spine Journal. 19 (10): 1613–1620. doi:10.1007/s00586-010-1412-z. PMC 2989236. PMID 20414688.
- ^ IJzelenberg W, Oosterhuis T, Hayden JA, Koes BW, van Tulder MW, Rubinstein SM, de Zoete A (30 August 2023). Cochrane Back and Neck Group (ed.). "Exercise therapy for treatment of acute non-specific low back pain". Cochrane Database of Systematic Reviews. 2023 (8). doi:10.1002/14651858.CD009365.pub2. PMC 10467021. PMID 37646368.
- ^ French SD, Cameron M, Walker BF, Reggars JW, Esterman AJ (January 2006). "Superficial heat or cold for low back pain". The Cochrane Database of Systematic Reviews. 2011 (1) CD004750. doi:10.1002/14651858.CD004750.pub2. PMC 8846312. PMID 16437495.
- ^ a b van Middelkoop M, Rubinstein SM, Kuijpers T, Verhagen AP, Ostelo R, Koes BW, van Tulder MW (January 2011). "A systematic review on the effectiveness of physical and rehabilitation interventions for chronic non-specific low back pain". European Spine Journal. 20 (1): 19–39. doi:10.1007/s00586-010-1518-3. PMC 3036018. PMID 20640863.
- ^ Guild DG (September 2012). "Mechanical therapy for low back pain". Primary Care. 39 (3): 511–516. doi:10.1016/j.pop.2012.06.006. PMID 22958560.
- ^ Ebadi S, Henschke N, Forogh B, Nakhostin Ansari N, van Tulder MW, Babaei-Ghazani A, Fallah E (July 2020). "Therapeutic ultrasound for chronic low back pain". The Cochrane Database of Systematic Reviews. 2020 (7) CD009169. doi:10.1002/14651858.CD009169.pub3. PMC 7390505. PMID 32623724.
- ^ National Institute for Health and Care Excellence (2016). Low back pain and sciatica in over 16s: assessment and management. Manchester: National Institute for Health and Care Excellence (NICE). ISBN 978-1-4731-2186-7. OCLC 1198756858.
- ^ Chou R, Deyo R, Friedly J, Skelly A, Hashimoto R, Weimer M, et al. (2016). Noninvasive Treatments for Low Back Pain. AHRQ Comparative Effectiveness Reviews. Rockville (MD): Agency for Healthcare Research and Quality (US). PMID 26985522.
- ^ van Duijvenbode IC, Jellema P, van Poppel MN, van Tulder MW (April 2008). "Lumbar supports for prevention and treatment of low back pain". The Cochrane Database of Systematic Reviews. 2008 (2) CD001823. doi:10.1002/14651858.cd001823.pub3. PMC 7046130. PMID 18425875.
- ^ a b Hayden JA, Ellis J, Ogilvie R, Malmivaara A, van Tulder MW (September 2021). "Exercise therapy for chronic low back pain". The Cochrane Database of Systematic Reviews. 9 (10) CD009790. doi:10.1002/14651858.cd009790.pub2. PMC 8477273. PMID 34580864.
- ^ Smith C, Grimmer-Somers K (June 2010). "The treatment effect of exercise programmes for chronic low back pain". Journal of Evaluation in Clinical Practice. 16 (3): 484–491. doi:10.1111/j.1365-2753.2009.01174.x. PMID 20438611.
- ^ van Middelkoop M, Rubinstein SM, Verhagen AP, Ostelo RW, Koes BW, van Tulder MW (April 2010). "Exercise therapy for chronic nonspecific low-back pain". Best Practice & Research. Clinical Rheumatology. 24 (2): 193–204. doi:10.1016/j.berh.2010.01.002. PMID 20227641.
- ^ Wewege MA, Booth J, Parmenter BJ (25 October 2018). "Aerobic vs. resistance exercise for chronic non-specific low back pain: A systematic review and meta-analysis". Journal of Back and Musculoskeletal Rehabilitation. 31 (5): 889–899. doi:10.3233/BMR-170920. PMID 29889056. S2CID 47013227.
- ^ Woodman JP, Moore NR (January 2012). "Evidence for the effectiveness of Alexander Technique lessons in medical and health-related conditions: a systematic review". International Journal of Clinical Practice. 66 (1): 98–112. doi:10.1111/j.1742-1241.2011.02817.x. PMID 22171910. S2CID 7579458.
- ^ Posadzki P, Ernst E (September 2011). "Yoga for low back pain: a systematic review of randomized clinical trials". Clinical Rheumatology. 30 (9): 1257–1262. doi:10.1007/s10067-011-1764-8. PMID 21590293. S2CID 17095187.
- ^ Wieland LS, Skoetz N, Pilkington K, Harbin S, Vempati R, Berman BM (November 2022). "Yoga for chronic non-specific low back pain". The Cochrane Database of Systematic Reviews. 2022 (11) CD010671. doi:10.1002/14651858.CD010671.pub3. PMC 9673466. PMID 36398843. S2CID 253627174.
- ^ Saragiotto BT, Maher CG, Yamato TP, Costa LO, Menezes Costa LC, Ostelo RW, Macedo LG (January 2016). "Motor control exercise for chronic non-specific low-back pain". The Cochrane Database of Systematic Reviews. 2016 (1) CD012004. doi:10.1002/14651858.cd012004. PMC 8761501. PMID 26742533.
- ^ Tagliaferri SD, Miller CT, Ford JJ, Hahne AJ, Main LC, Rantalainen T, et al. (June 2020). "Randomized Trial of General Strength and Conditioning Versus Motor Control and Manual Therapy for Chronic Low Back Pain on Physical and Self-Report Outcomes". Journal of Clinical Medicine. 9 (6): 1726. doi:10.3390/jcm9061726. PMC 7355598. PMID 32503243.
- ^ a b Yamato TP, Maher CG, Saragiotto BT, Hancock MJ, Ostelo RW, Cabral CM, et al. (Cochrane Back and Neck Group) (July 2015). "Pilates for low back pain". The Cochrane Database of Systematic Reviews. 2015 (7) CD010265. doi:10.1002/14651858.CD010265.pub2. PMC 8078578. PMID 26133923.
- ^ Kamper SJ, Apeldoorn AT, Chiarotto A, Smeets RJ, Ostelo RW, Guzman J, van Tulder MW (September 2014). "Multidisciplinary biopsychosocial rehabilitation for chronic low back pain". The Cochrane Database of Systematic Reviews. 2014 (9) CD000963. doi:10.1002/14651858.cd000963.pub3. PMC 10945502. PMID 25180773.
- ^ Nizard J, Raoul S, Nguyen JP, Lefaucheur JP (October 2012). "Invasive stimulation therapies for the treatment of refractory pain". Discovery Medicine. 14 (77): 237–246. PMID 23114579.
- ^ Dubinsky RM, Miyasaki J (January 2010). "Assessment: efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review): report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology". Neurology. 74 (2): 173–176. doi:10.1212/WNL.0b013e3181c918fc. PMID 20042705.
- ^ a b c d e Cashin AG, Wand BM, O'Connell N, Lee H, Rizzi RR, Bagga MK, O'Hagan E, Maher CG, Furlan AD, Tulder MW, McAuley JH (April 2023). "Pharmacological treatments for low back pain in adults: an overview of Cochrane Reviews". The Cochrane Database of Systematic Reviews. 4 (4): CD013815. doi:10.1002/14651858.CD012230. PMC 6353046. PMID 37014979.
- ^ "Acute low back pain without radiculopathy". English.prescrire.org. October 2019. Retrieved 15 November 2019.
- ^ a b Machado GC, Maher CG, Ferreira PH, Day RO, Pinheiro MB, Ferreira ML (July 2017). "Non-steroidal anti-inflammatory drugs for spinal pain: a systematic review and meta-analysis". Annals of the Rheumatic Diseases. 76 (7): 1269–1278. doi:10.1136/annrheumdis-2016-210597. PMID 28153830. S2CID 22850331.
- ^ van der Gaag WH, Roelofs PD, Enthoven WT, van Tulder MW, Koes BW (April 2020). "Non-steroidal anti-inflammatory drugs for acute low back pain". The Cochrane Database of Systematic Reviews. 2020 (4) CD013581. doi:10.1002/14651858.CD013581. PMC 7161726. PMID 32297973.
- ^ Saragiotto BT, Machado GC, Ferreira ML, Pinheiro MB, Abdel Shaheed C, Maher CG (June 2016). "Paracetamol for low back pain". The Cochrane Database of Systematic Reviews. 2019 (6) CD012230. doi:10.1002/14651858.CD012230. PMC 6353046. PMID 27271789.
- ^ Machado GC, Maher CG, Ferreira PH, Pinheiro MB, Lin CW, Day RO, et al. (March 2015). "Efficacy and safety of paracetamol for spinal pain and osteoarthritis: systematic review and meta-analysis of randomised placebo controlled trials". BMJ. 350 h1225. doi:10.1136/bmj.h1225. PMC 4381278. PMID 25828856.
- ^ Enthoven WT, Roelofs PD, Deyo RA, van Tulder MW, Koes BW (February 2016). "Non-steroidal anti-inflammatory drugs for chronic low back pain". The Cochrane Database of Systematic Reviews. 2 (8) CD012087. doi:10.1002/14651858.CD012087. PMC 7104791. PMID 26863524.
- ^ Bhala N, Emberson J, Merhi A, Abramson S, Arber N, Baron JA, et al. (Coxib and traditional NSAID Trialists' (CNT) Collaboration)) (August 2013). "Vascular and upper gastrointestinal effects of non-steroidal anti-inflammatory drugs: meta-analyses of individual participant data from randomised trials". Lancet. 382 (9894): 769–779. doi:10.1016/S0140-6736(13)60900-9. PMC 3778977. PMID 23726390.
- ^ Chou R, Pinto RZ, Fu R, Lowe RA, Henschke N, McAuley JH, Dana T (October 2022). "Systemic corticosteroids for radicular and non-radicular low back pain". The Cochrane Database of Systematic Reviews. 2022 (10) CD012450. doi:10.1002/14651858.CD012450.pub2. PMC 9585990. PMID 36269125.
- ^ Franklin GM (September 2014). "Opioids for chronic noncancer pain: a position paper of the American Academy of Neurology". Neurology. 83 (14): 1277–1284. doi:10.1212/WNL.0000000000000839. PMID 25267983.
- ^ Chaparro LE, Furlan AD, Deshpande A, Mailis-Gagnon A, Atlas S, Turk DC (April 2014). "Opioids compared with placebo or other treatments for chronic low back pain: an update of the Cochrane Review". Spine. 39 (7): 556–563. doi:10.1097/BRS.0000000000000249. PMID 24480962. S2CID 25356400.
- ^ Dowell D, Haegerich TM, Chou R (March 2016). "CDC Guideline for Prescribing Opioids for Chronic Pain – United States, 2016". MMWR. Recommendations and Reports. 65 (1): 1–49. doi:10.15585/mmwr.rr6501e1. PMC 6390846. PMID 26987082.
- ^ Shmagel A, Krebs E, Ensrud K, Foley R (September 2016). "Illicit Substance Use in US Adults With Chronic Low Back Pain". Spine. 41 (17): 1372–1377. doi:10.1097/brs.0000000000001702. PMC 5002230. PMID 27438382.
- ^ Abdel Shaheed C, Maher CG, Williams KA, Day R, McLachlan AJ (July 2016). "Efficacy, Tolerability, and Dose-Dependent Effects of Opioid Analgesics for Low Back Pain: A Systematic Review and Meta-analysis". JAMA Internal Medicine. 176 (7): 958–968. doi:10.1001/jamainternmed.2016.1251. PMID 27213267. S2CID 29903177.
- ^ de Leon-Casasola OA (March 2013). "Opioids for chronic pain: new evidence, new strategies, safe prescribing". The American Journal of Medicine. 126 (3 Suppl 1): S3-11. doi:10.1016/j.amjmed.2012.11.011. PMID 23414718.
- ^ Ferraro MC, Urquhart DM, Ferreira GE, Wewege MA, Shaheed CA, Traeger AC, Hoving JL, Visser EJ, McAuley JH, Cashin AG (March 2025). "Antidepressants for low back pain and spine-related leg pain". The Cochrane Database of Systematic Reviews. 2025 (3) CD001703. doi:10.1002/14651858.CD001703.pub4. PMC 11890917. PMID 40058767.
- ^ Enke O, New HA, New CH, Mathieson S, McLachlan AJ, Latimer J, et al. (July 2018). "Anticonvulsants in the treatment of low back pain and lumbar radicular pain: a systematic review and meta-analysis". CMAJ. 190 (26): E786 – E793. doi:10.1503/cmaj.171333. PMC 6028270. PMID 29970367.
- ^ Chou R, Loeser JD, Owens DK, Rosenquist RW, Atlas SJ, Baisden J, et al. (American Pain Society Low Back Pain Guideline Pane) (May 2009). "Interventional therapies, surgery, and interdisciplinary rehabilitation for low back pain: an evidence-based clinical practice guideline from the American Pain Society". Spine. 34 (10): 1066–1077. doi:10.1097/BRS.0b013e3181a1390d. PMID 19363457. S2CID 10658374.
- ^ Pinto RZ, Maher CG, Ferreira ML, Hancock M, Oliveira VC, McLachlan AJ, et al. (December 2012). "Epidural corticosteroid injections in the management of sciatica: a systematic review and meta-analysis". Annals of Internal Medicine. 157 (12): 865–877. doi:10.7326/0003-4819-157-12-201212180-00564. PMID 23362516. S2CID 21203011.
- ^ "Epidural Corticosteroid Injection: Drug Safety Communication – Risk of Rare But Serious Neurologic Problems". FDA. 23 April 2014. Archived from the original on 24 April 2014. Retrieved 24 April 2014.
- ^ Jacobs W, Van der Gaag NA, Tuschel A, de Kleuver M, Peul W, Verbout AJ, Oner FC (September 2012). "Total disc replacement for chronic back pain in the presence of disc degeneration". The Cochrane Database of Systematic Reviews (9) CD008326. doi:10.1002/14651858.CD008326.pub2. hdl:1871/48560. PMID 22972118.
- ^ Lee CS, Hwang CJ, Lee DH, Kim YT, Lee HS (March 2011). "Fusion rates of instrumented lumbar spinal arthrodesis according to surgical approach: a systematic review of randomized trials". Clinics in Orthopedic Surgery. 3 (1): 39–47. doi:10.4055/cios.2011.3.1.39. PMC 3042168. PMID 21369477.
- ^ Traeger AC, Gilbert SE, Harris IA, Maher CG (7 March 2023). Cochrane Back and Neck Group (ed.). "Spinal cord stimulation for low back pain". Cochrane Database of Systematic Reviews. 2023 (8) CD014789. doi:10.1002/14651858.CD014789.pub2. PMC 9990744. PMID 36878313.
- ^ Rothberg S, Friedman BW (January 2017). "Complementary therapies in addition to medication for patients with nonchronic, nonradicular low back pain: a systematic review". The American Journal of Emergency Medicine. 35 (1): 55–61. doi:10.1016/j.ajem.2016.10.001. PMID 27751598. S2CID 34520820.
- ^ Rubinstein SM, de Zoete A, van Middelkoop M, Assendelft WJ, de Boer MR, van Tulder MW (March 2019). "Benefits and harms of spinal manipulative therapy for the treatment of chronic low back pain: systematic review and meta-analysis of randomised controlled trials". BMJ. 364: l689. doi:10.1136/bmj.l689. PMC 6396088. PMID 30867144.
- ^ Rubinstein SM, Terwee CB, Assendelft WJ, de Boer MR, van Tulder MW, et al. (Cochrane Back and Neck Group) (September 2012). "Spinal manipulative therapy for acute low-back pain". The Cochrane Database of Systematic Reviews. 2012 (9) CD008880. doi:10.1002/14651858.CD008880.pub2. PMC 6885055. PMID 22972127.
- ^ Dagenais S, Mayer J, Wooley JR, Haldeman S (2008). "Evidence-informed management of chronic low back pain with medicine-assisted manipulation". The Spine Journal. 8 (1): 142–149. doi:10.1016/j.spinee.2007.09.010. PMID 18164462.
- ^ Macedo LG, Saragiotto BT, Yamato TP, Costa LO, Menezes Costa LC, Ostelo RW, Maher CG (February 2016). "Motor control exercise for acute non-specific low back pain". The Cochrane Database of Systematic Reviews. 2016 (2) CD012085. doi:10.1002/14651858.cd012085. PMC 8734597. PMID 26863390.
- ^ a b c d Mu J, Furlan AD, Lam WY, Hsu MY, Ning Z, Lao L (December 2020). "Acupuncture for chronic nonspecific low back pain". The Cochrane Database of Systematic Reviews. 2020 (12) CD013814. doi:10.1002/14651858.CD013814. PMC 8095030. PMID 33306198.
- ^ a b Furlan AD, Yazdi F, Tsertsvadze A, Gross A, Van Tulder M, Santaguida L, et al. (2012). "A systematic review and meta-analysis of efficacy, cost-effectiveness, and safety of selected complementary and alternative medicine for neck and low-back pain". Evidence-Based Complementary and Alternative Medicine. 2012 953139. doi:10.1155/2012/953139. PMC 3236015. PMID 22203884.
- ^ Lin CW, Haas M, Maher CG, Machado LA, van Tulder MW (July 2011). "Cost-effectiveness of guideline-endorsed treatments for low back pain: a systematic review". European Spine Journal. 20 (7): 1024–1038. doi:10.1007/s00586-010-1676-3. PMC 3176706. PMID 21229367.
- ^ a b c d Furlan AD, Giraldo M, Baskwill A, Irvin E, Imamura M (September 2015). "Massage for low-back pain". The Cochrane Database of Systematic Reviews. 2015 (9) CD001929. doi:10.1002/14651858.CD001929.pub3. PMC 8734598. PMID 26329399.
- ^ Gagnier JJ, Oltean H, van Tulder MW, Berman BM, Bombardier C, Robbins CB (January 2016). "Herbal Medicine for Low Back Pain: A Cochrane Review". Spine. 41 (2): 116–133. doi:10.1097/brs.0000000000001310. PMID 26630428. S2CID 42119774.
- ^ Cherkin DC, Herman PM (April 2018). "Cognitive and Mind-Body Therapies for Chronic Low Back Pain and Neck Pain: Effectiveness and Value". JAMA Internal Medicine. 178 (4): 556–557. doi:10.1001/jamainternmed.2018.0113. PMID 29507946. S2CID 3680364.
- ^ Cramer H, Haller H, Lauche R, Dobos G (September 2012). "Mindfulness-based stress reduction for low back pain. A systematic review". BMC Complementary and Alternative Medicine. 12: 162. doi:10.1186/1472-6882-12-162. PMC 3520871. PMID 23009599.
- ^ Anheyer D, Haller H, Barth J, Lauche R, Dobos G, Cramer H (June 2017). "Mindfulness-Based Stress Reduction for Treating Low Back Pain: A Systematic Review and Meta-analysis". Annals of Internal Medicine. 166 (11): 799–807. doi:10.7326/M16-1997. PMID 28437793. S2CID 1157568.
- ^ Urrútia G, Burton AK, Morral A, Bonfill X, Zanoli G (19 April 2004). "Neuroreflexotherapy for non-specific low-back pain". The Cochrane Database of Systematic Reviews. 2011 (2) CD003009. doi:10.1002/14651858.cd003009.pub2. PMC 8992702. PMID 15106186.
- ^ Urrútia G, Burton K, Morral A, Bonfill X, Zanoli G (March 2005). "Neuroreflexotherapy for nonspecific low back pain: a systematic review". Spine. 30 (6): E148 – E153. doi:10.1097/01.brs.0000155575.85223.14. PMID 15770167. S2CID 31140257.
- ^ Marin TJ, Van Eerd D, Irvin E, Couban R, Koes BW, Malmivaara A, et al. (June 2017). "Multidisciplinary biopsychosocial rehabilitation for subacute low back pain". The Cochrane Database of Systematic Reviews. 2017 (6) CD002193. doi:10.1002/14651858.cd002193.pub2. PMC 6481490. PMID 28656659.
- ^ Maas ET, Ostelo RW, Niemisto L, Jousimaa J, Hurri H, Malmivaara A, van Tulder MW (October 2015). "Radiofrequency denervation for chronic low back pain". The Cochrane Database of Systematic Reviews. 2015 (10) CD008572. doi:10.1002/14651858.cd008572.pub2. PMC 8782593. PMID 26495910.
- ^ Luz Júnior MA, Almeida MO, Santos RS, Civile VT, Costa LO (January 2019). "Effectiveness of Kinesio Taping in Patients With Chronic Nonspecific Low Back Pain: A Systematic Review With Meta-analysis". Spine. 44 (1): 68–78. doi:10.1097/BRS.0000000000002756. PMID 29952880. S2CID 49486200.
- ^ Engers A, Jellema P, Wensing M, van der Windt DA, Grol R, van Tulder MW (January 2008). "Individual patient education for low back pain". The Cochrane Database of Systematic Reviews. 2008 (1) CD004057. doi:10.1002/14651858.cd004057.pub3. hdl:2066/69744. PMC 6999124. PMID 18254037.
- ^ Verbeek JH, Martimo KP, Karppinen J, Kuijer PP, Viikari-Juntura E, Takala EP (June 2011). "Manual material handling advice and assistive devices for preventing and treating back pain in workers". The Cochrane Database of Systematic Reviews (6) CD005958. doi:10.1002/14651858.CD005958.pub3. PMID 21678349.
- ^ a b Chou R, Shekelle P (April 2010). "Will this patient develop persistent disabling low back pain?". JAMA. 303 (13): 1295–1302. doi:10.1001/jama.2010.344. PMID 20371789.
- ^ Hayden JA, Wilson MN, Riley RD, Iles R, Pincus T, Ogilvie R (November 2019). "Individual recovery expectations and prognosis of outcomes in non-specific low back pain: prognostic factor review". The Cochrane Database of Systematic Reviews. 2019 (11). doi:10.1002/14651858.cd011284.pub2. PMC 6877336. PMID 31765487.
- ^ Cunningham F (2009). Williams Obstetrics (23 ed.). McGraw Hill Professional. p. 210. ISBN 978-0-07-170285-0. Archived from the original on 8 September 2017.
- ^ Shiri R, Karppinen J, Leino-Arjas P, Solovieva S, Viikari-Juntura E (January 2010). "The association between smoking and low back pain: a meta-analysis". The American Journal of Medicine. 123 (1): 87.e7–87.35. doi:10.1016/j.amjmed.2009.05.028. PMID 20102998.
- ^ a b c d e Maharty DC (September 2012). "The history of lower back pain: a look "back" through the centuries". Primary Care. 39 (3): 463–470. doi:10.1016/j.pop.2012.06.002. PMID 22958555.
- ^ "lumbago". Oxford English Dictionary (Online ed.). Oxford University Press. (Subscription or participating institution membership required.)
- ^ a b c d e Lutz GK, Butzlaff M, Schultz-Venrath U (August 2003). "Looking back on back pain: trial and error of diagnoses in the 20th century". Spine. 28 (16): 1899–1905. doi:10.1097/01.BRS.0000083365.41261.CF. PMID 12923482. S2CID 25083375.
- ^ https://books.google.com/books?id=tROeDwAAQBAJ&pg=PA171
- ^ a b Manchikanti L, Singh V, Datta S, Cohen SP, Hirsch JA (2009). "Comprehensive review of epidemiology, scope, and impact of spinal pain". Pain Physician. 12 (4): E35 – E70. doi:10.36076/ppj.2009/12/E35. PMID 19668291.
- ^ Mokdad AH, Ballestros K, Echko M, Glenn S, Olsen HE, Mullany E, et al. (April 2018). "The State of US Health, 1990-2016: Burden of Diseases, Injuries, and Risk Factors Among US States". JAMA. 319 (14): 1444–1472. doi:10.1001/jama.2018.0158. PMC 5933332. PMID 29634829.
- ^ a b c d American College of Occupational and Environmental Medicine (February 2014), "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American College of Occupational and Environmental Medicine, archived from the original on 11 September 2014, retrieved 24 February 2014, which cites
- Talmage J, Belcourt R, Galper J, et al. (2011). "Low back disorders". In Hegmann KT (ed.). Occupational medicine practice guidelines: evaluation and management of common health problems and functional recovery in workers (3rd ed.). Elk Grove Village, IL: American College of Occupational and Environmental Medicine. pp. 336, 373, 376–77. ISBN 978-0-615-45227-2.
External links
[edit]Low back pain
View on GrokipediaClinical Presentation
Signs and symptoms
Low back pain commonly manifests as discomfort in the lumbar region, ranging from a dull, aching sensation to sharp, stabbing, or burning pain that may intensify with movement. Pain that dissipates with a simple position change strongly suggests a positional etiology and is likely responsive to conservative care like physical therapy.[10][11] Stiffness in the lower back and muscle spasms are frequent accompanying features, often resulting in reduced flexibility and difficulty maintaining certain postures.[8][12][13] The pain can be localized to the back or radiate along the path of the sciatic nerve into the buttocks, thighs, or calves, a condition referred to as sciatica, which may present as shooting or electric-like discomfort.[8] In cases involving nerve irritation, patients may experience associated symptoms such as numbness, tingling, or weakness in the legs.[13] Severe presentations can include bowel or bladder dysfunction, signaling potential urgency. Pain duration helps classify low back pain as acute (less than 6 weeks), subacute (6 to 12 weeks), or chronic (more than 12 weeks), with acute episodes often resolving more readily than persistent ones.[14][4] Symptoms typically interfere with daily activities, exacerbating during bending, lifting, prolonged sitting, or standing, thereby limiting mobility and productivity.[15][16] Low back pain can be categorized by dominant pain mechanisms: nociceptive (mechanical), featuring localized aching and stiffness aggravated by physical exertion or tissue damage; neuropathic, involving radiating, burning sensations due to nerve damage or compression, accompanied by sensory disturbances like paresthesia; and nociplastic, characterized by central sensitization without evident nociceptive or neuropathic sources, often seen in chronic non-specific cases with features such as widespread pain, fatigue, sleep disturbances, and emotional distress.[17][18]Classification
Low back pain is commonly classified based on its duration to distinguish acute episodes from more persistent conditions, aiding in prognosis and management planning. Acute low back pain is defined as lasting less than 6 weeks, subacute as 6 to 12 weeks, and chronic as exceeding 12 weeks.[14] This temporal framework helps clinicians anticipate recovery patterns, with acute cases often resolving spontaneously while chronic pain requires multidisciplinary approaches.[4] Etiological classification divides low back pain into non-specific and specific categories, reflecting the presence or absence of an identifiable structural or pathological cause. Non-specific low back pain accounts for approximately 90% of cases, where no precise anatomical source can be determined despite thorough evaluation.[19] In contrast, specific low back pain arises from identifiable etiologies such as herniated intervertebral disc or spinal stenosis, which may involve nerve compression or degenerative changes.[20] Further subtypes differentiate pain based on its distribution and underlying mechanisms. Radicular low back pain involves radiating discomfort into the lower extremities due to nerve root irritation or compression, often presenting as shooting or burning sensations along a dermatomal pattern.[21] Non-radicular pain, by comparison, is confined to the back without such radiation, typically stemming from musculoskeletal sources like strain or facet joint issues.[20] Severity assessment employs validated scales to quantify pain intensity and functional impairment, informing treatment escalation. The Numeric Pain Rating Scale (NPRS) measures pain on a 0-10 continuum, where 0 indicates no pain and 10 the worst imaginable, providing a simple, reliable metric for tracking changes over time.[22] The Oswestry Disability Index (ODI) evaluates functional limitations through a 10-item questionnaire, yielding a percentage score that reflects disability in daily activities such as personal care and mobility, with higher scores indicating greater impact.[23] The World Health Organization's 2023 guidelines specifically address chronic primary low back pain in primary care, defining it as persistent pain lasting more than 12 weeks without evidence of serious underlying pathology or identifiable specific causes, emphasizing a non-specific presentation in community settings.[24] This classification prioritizes holistic care for the majority of chronic cases encountered in routine practice.Pathophysiology
Anatomy of the back
The lumbar spine, or lower back, comprises five vertebrae designated L1 through L5, which are the largest and strongest in the vertebral column to accommodate substantial mechanical loads from the upper body.[25] Each lumbar vertebra features a robust body, a vertebral arch forming the posterior elements, and transverse processes that serve as attachment sites for muscles and ligaments; the L5 vertebra uniquely articulates with the sacrum at the lumbosacral junction, contributing to the transition between mobile lumbar segments and the rigid pelvis.[26] Intervertebral discs separate the lumbar vertebrae, providing cushioning and flexibility; each disc consists of a central gel-like nucleus pulposus surrounded by a fibrous annulus fibrosus, which resists compressive forces while permitting limited motion.[27] Facet joints, or zygapophyseal joints, connect adjacent vertebrae posteriorly, with superior and inferior articular processes that guide gliding motions and limit excessive rotation in the lumbar region.[26] Key ligaments stabilize the lumbar spine, including the anterior longitudinal ligament spanning the ventral surfaces of the vertebral bodies to resist hyperextension, and the posterior longitudinal ligament lining the posterior vertebral canal to prevent hyperflexion.[26] Additional stabilizers encompass the ligamentum flavum between laminae for elasticity during flexion, interspinous and supraspinous ligaments connecting spinous processes to resist forward bending, and the iliolumbar ligaments anchoring L5 to the ilium for pelvic stability.[28] Muscles of the lumbar back include the erector spinae group—comprising the iliocostalis, longissimus, and spinalis—which run longitudinally along the spine to extend and laterally bend the trunk, and the multifidus muscles, deep transversospinalis fibers that provide segmental stability and proprioceptive feedback.[29] Other contributors, such as the quadratus lumborum and psoas major, assist in lateral flexion and hip movement, respectively, while the thoracolumbar fascia envelops these structures to unify force transmission.[29] The spinal cord terminates at the L1-L2 level, giving way to the cauda equina—a bundle of lumbar and sacral nerve roots suspended in cerebrospinal fluid within the lumbar cistern—that exits via intervertebral foramina to innervate the lower limbs.[30] The sciatic nerve originates from the L4-S3 roots, forming the largest peripheral nerve and supplying the posterior thigh, leg, and foot.[30] Innervation of lumbar structures derives primarily from dorsal rami of spinal nerves for paraspinal muscles and posterior elements, with ventral rami contributing to anterior abdominal and pelvic musculature; sensory input arises from sinuvertebral nerves innervating discs and ligaments.[28] Blood supply to the lumbar spine arises from segmental arteries, including lumbar arteries branching from the aorta to nourish vertebral bodies and paraspinal tissues via anterior and posterior spinal arteries, with venous drainage through a rich plexus around the vertebrae.[28] Biomechanically, the lumbar spine bears up to 80% of body weight during upright posture, distributing compressive loads through vertebral bodies and discs while facet joints and ligaments ensure stability against shear and torsional forces; this configuration allows approximately 50-60 degrees of flexion-extension and limited lateral bending, essential for bipedal locomotion and daily activities.[31] With aging, lumbar discs undergo degeneration characterized by progressive dehydration and loss of proteoglycan content in the nucleus pulposus, leading to reduced disc height and increased stiffness by age 40-50 in many individuals.[32] Osteoporosis diminishes vertebral bone mineral density, particularly in trabecular bone, heightening fracture risk and altering load distribution; facet joints develop osteoarthritis with cartilage thinning and osteophyte formation, while muscles like the multifidus exhibit fatty infiltration and atrophy, compromising stability.[31] These changes can disrupt normal biomechanics, potentially contributing to pain signals from irritated structures.[31]Mechanisms of pain
Low back pain arises from the activation of nociceptors, specialized sensory receptors in peripheral tissues that detect potentially harmful stimuli such as mechanical pressure, thermal changes, or chemical irritants. These nociceptors, primarily free nerve endings in structures like muscles, ligaments, and intervertebral discs, transduce noxious inputs into electrical signals that initiate the pain response. In low back pain, mechanical deformation from injury or strain commonly triggers this nociceptive process, leading to localized hypersensitivity at the site of tissue damage.[33] Once activated, nociceptive signals are transmitted via primary afferent neurons to the dorsal horn of the spinal cord, where second-order neurons integrate and process the input. From the dorsal horn, these signals ascend primarily through the spinothalamic tract, a key anterolateral pathway that carries pain and temperature information to the thalamus and subsequently to cortical areas for perception and localization. This pathway enables the conscious experience of pain but can become altered in low back pain, contributing to referred sensations or diffuse discomfort.[34] In chronic low back pain, central sensitization emerges as a critical mechanism, involving neuroplastic changes in the central nervous system that amplify pain signals beyond the initial injury. This process enhances neuronal excitability and synaptic efficacy in nociceptive pathways, resulting in hyperalgesia (increased pain to noxious stimuli) and allodynia (pain from non-noxious stimuli) through mechanisms like long-term potentiation and reduced inhibition. Such adaptations persist even after peripheral damage resolves, perpetuating pain via altered membrane properties and circuit remodeling in the spinal cord and brain.[35] Tissue damage in low back pain also triggers the release of inflammatory mediators that sensitize nociceptors and sustain pain signaling. Pro-inflammatory cytokines such as interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α) promote the recruitment of immune cells and enhance nociceptor responsiveness, while prostaglandins, synthesized via cyclooxygenase enzymes, lower activation thresholds for pain receptors. These mediators create a feedback loop that prolongs inflammation and contributes to the transition from acute to chronic pain states.[36][37] The biopsychosocial model integrates these biological processes with psychological factors, highlighting how stress and emotions modulate central nervous system pain pathways. Chronic stress activates descending pathways involving the hypothalamic-pituitary-adrenal axis, releasing glucocorticoids that can exacerbate neuroinflammation and reduce endogenous pain inhibition, while negative emotions like anxiety amplify pain perception through limbic system interactions. This interplay underscores the role of cognitive-emotional states in sustaining low back pain beyond purely peripheral mechanisms.[38][39]Etiology
Mechanical causes
Mechanical low back pain refers to pain originating from structural or biomechanical issues within the spine, intervertebral discs, or surrounding soft tissues, without involvement of systemic diseases.[40] These causes typically result from wear and tear, injury, or improper loading on the lumbar region, leading to localized discomfort that may radiate but does not involve neurological deficits unless compression occurs. Approximately 90% of low back pain cases are classified as non-specific mechanical in nature, particularly in acute presentations.[41] Disc-related pathologies represent a primary subset of mechanical causes, encompassing herniation, degeneration, and annular tears. Lumbar disc herniation occurs when the inner nucleus pulposus protrudes through the outer annulus fibrosus, often due to age-related weakening or acute trauma, compressing nearby structures and eliciting pain.[42] Degenerative disc disease involves progressive loss of disc hydration and height, leading to instability and inflammation that contributes to chronic axial pain.[43] Annular tears, or disruptions in the disc's outer layer, can cause localized pain through chemical irritation of nociceptors, even without herniation.[44] Discogenic pain from these issues accounts for approximately 39% of chronic low back pain cases, making it the most common identifiable mechanical etiology.[45] Joint-related problems, such as facet joint arthritis, spondylolisthesis, spinal stenosis, and sacroiliac joint dysfunction, also contribute significantly to mechanical low back pain. Facet joint arthritis, or osteoarthritis of the zygapophyseal joints, results from cartilage breakdown and synovial inflammation, often exacerbated by extension or rotation, and is implicated in 15% to 45% of low back pain episodes.[46] This degeneration leads to hypertrophy, stiffness, and referred pain patterns. Spondylolisthesis involves anterior slippage of one vertebra over another, commonly degenerative in adults over 50, causing instability and load redistribution that provokes pain during movement.[47] Spinal stenosis, the narrowing of the spinal canal due to degenerative changes like ligamentum flavum hypertrophy or osteophyte formation, compresses neural elements and is a common cause of low back pain with leg symptoms in older adults.[48] Sacroiliac joint dysfunction, involving dysfunction or inflammation of the sacroiliac joint, accounts for 15-30% of chronic low back pain cases and often presents with unilateral pain in the lower back or buttocks, worsened by prolonged standing or stair climbing.[49] These joint disorders often coexist with disc changes, amplifying mechanical stress on the lumbar spine. Muscle and ligament strains constitute another frequent mechanical cause, arising from acute trauma, sudden twisting, or chronic overuse. Lumbar sprains involve stretching or tearing of ligaments stabilizing the spine, while strains affect muscles like the erector spinae or quadratus lumborum, resulting in sharp pain and reduced mobility.[50] These injuries are self-limiting in most cases but can recur if healing is incomplete, contributing to recurrent episodes. Biomechanical imbalances, including poor posture and repetitive lifting, promote uneven spinal loading and fatigue of supporting structures. Conditions such as lower crossed syndrome, characterized by weak core muscles (e.g., abdominals and gluteals) and tight hip flexors, perpetuate chronic low back pain by inducing anterior pelvic tilt, excessive lumbar lordosis, and sustained tissue stress on the spine.[51] Prolonged forward flexion or asymmetric postures alters lumbar lordosis, increasing intradiscal pressure and facet loading, which over time leads to tissue microtrauma.[52] Repetitive heavy lifting, common in occupational settings, induces cumulative shear forces on the lumbosacral junction, heightening strain risk. These factors often underlie acute flares in otherwise asymptomatic individuals. Many mechanical causes can present unilaterally on the right side, including muscle strains or sprains from injury or overuse, herniated discs with right-sided nerve root compression leading to sciatica, sacroiliac joint dysfunction, spinal stenosis with asymmetric symptoms, or facet joint arthritis.[53] Overall, mechanical causes predominate in acute low back pain among working-age adults (18-65 years), accounting for the majority of episodes. Most cases are mechanical and improve with rest and conservative management, resolving spontaneously in 80-90% within six weeks without specific intervention, but persistent or severe pain requires medical evaluation to rule out serious conditions.[54][53]Non-mechanical causes
Non-mechanical causes of low back pain encompass systemic conditions that originate outside the primary musculoskeletal structures of the spine, often involving inflammation, infection, malignancy, visceral organs, or metabolic bone disorders. These etiologies account for a minority of cases but are critical to identify due to their potential severity and need for prompt intervention. Unlike mechanical pain, which typically relates to local tissue strain, non-mechanical pain may present with systemic symptoms or atypical patterns, such as night pain or unremitting discomfort.[20] Inflammatory arthropathies represent a key category of non-mechanical causes. Ankylosing spondylitis, a seronegative spondyloarthropathy, primarily affects young adults and manifests as chronic inflammatory back pain with morning stiffness lasting over 30 minutes, often improving with exercise but worsening with rest; it involves sacroiliac joint inflammation that progresses to spinal fusion.[55] Rheumatoid arthritis, an autoimmune disease, less commonly targets the lumbar spine but can cause low back pain through pannus formation and synovial inflammation in facet joints or atlantoaxial subluxation extending to the lower segments, particularly in longstanding cases.[56] Infectious processes, such as vertebral osteomyelitis and discitis, arise from hematogenous spread or direct inoculation, leading to localized vertebral destruction and severe, progressive back pain often accompanied by fever and elevated erythrocyte sedimentation rates. Staphylococcus aureus is the most frequent pathogen, accounting for up to 50% of cases, with risk factors including intravenous drug use, diabetes, and immunosuppression; symptoms may include neurological deficits if abscess formation compresses the spinal cord.[57] Neoplastic conditions contribute to low back pain through direct spinal involvement or metastatic spread. Metastases from primary cancers like breast or prostate are common, with up to 70% of advanced breast cancer patients and nearly all with metastatic prostate cancer developing bone lesions, presenting as insidious, unrelenting pain exacerbated at night due to periosteal stretching and pathologic fractures. Primary malignancies, such as multiple myeloma, cause lytic lesions in the vertebrae, resulting in acute or chronic pain from structural compromise.[58] Visceral disorders can refer pain to the low back via shared neural pathways. Abdominal aortic aneurysm often produces deep, constant back pain from pressure on surrounding tissues, particularly if expanding, and may radiate to the flanks in symptomatic cases greater than 5 cm in diameter.[59] Renal colic, due to ureteral obstruction by kidney stones, causes intense, colicky flank pain radiating to the lower back and groin, typically lasting minutes to hours and associated with hematuria.[60] Endometriosis, affecting 10-15% of reproductive-age women, leads to cyclic low back pain from ectopic endometrial tissue irritating pelvic nerves, often worsening during menses and coexisting with dysmenorrhea.[61] Right-sided low back pain may particularly arise from referred pain due to right kidney conditions (e.g., stones or infection), appendicitis, or gynecological issues in women (e.g., endometriosis); less common but serious causes include abdominal aortic aneurysm or tumors.[53] Other non-mechanical causes include metabolic bone diseases and compressive neuropathies. Osteoporotic vertebral compression fractures, prevalent in postmenopausal women and those with low bone density, present with acute, band-like back pain following minimal trauma, potentially leading to height loss and kyphosis.[62] Paget's disease of bone involves disordered remodeling, affecting the spine in up to 50% of multifocal cases and causing chronic low back pain from vertebral enlargement, sclerosis, or fractures.[63] Cauda equina syndrome, a rare emergency from central disc herniation or tumor compression, features saddle anesthesia, bowel/bladder dysfunction, and low back pain with bilateral leg weakness.[64] These conditions often signal red flags like unexplained weight loss, fever, or progressive neurology, warranting urgent evaluation to differentiate from benign mechanical pain.[65]Risk factors
Risk factors for low back pain can be categorized as non-modifiable or modifiable, with additional influences from occupational and psychosocial domains. Non-modifiable factors include advancing age, particularly beyond 40 years, which is associated with increased prevalence due to degenerative changes in the spine.[66] Female sex also elevates susceptibility, with women experiencing higher lifetime prevalence rates compared to men, potentially linked to hormonal and biomechanical differences.[67] Genetic predisposition, such as familial tendencies toward intervertebral disc disease, further contributes, as evidenced by twin studies showing heritability in lumbar disc degeneration.[68] Modifiable risk factors encompass lifestyle elements like obesity, defined by a body mass index (BMI) greater than 30, which heightens mechanical stress on the spine and is linked to a 1.3- to 2-fold increased risk of low back pain.[69] Smoking impairs intervertebral disc nutrition by reducing blood flow and oxygen supply, accelerating degeneration and elevating pain risk.[70] A sedentary lifestyle similarly promotes vulnerability, with prolonged inactivity associated with a moderate elevation in low back pain incidence across adults.[71] Dietary patterns represent an additional modifiable factor. A high-carbohydrate diet rich in refined carbohydrates and low in fiber can promote systemic inflammation, as evidenced by elevated levels of C-reactive protein (CRP) and interleukin-6 (IL-6), which is associated with increased risk, severity, and pain sensitivity in chronic low back pain. Energy-dense diets high in refined grains and added sugars show a positive association with chronic low back pain, including an odds ratio of 1.13 (95% CI 1.01–1.32) for higher adherence to such patterns and 49% increased odds of chronic spinal pain with higher added sugar intake. In contrast, high-fiber carbohydrates may mitigate inflammation and potentially offer protective effects.[9][72] Occupational exposures play a significant role, including heavy lifting, which imposes excessive axial loads on the lumbar spine and is a well-established predictor of acute and chronic episodes.[52] Prolonged sitting, common in desk-based jobs, contributes through sustained static postures that strain paraspinal muscles and discs.[73] Vibration exposure, such as that experienced by truck drivers from whole-body vibration, further compounds risk by transmitting mechanical stress to the spine.[74] Psychosocial factors, integrated within the biopsychosocial model, include chronic stress, depression, and job dissatisfaction, which amplify pain perception and disability through central sensitization and behavioral pathways.[75] These elements often interact with physical risks, heightening overall susceptibility. Recent epidemiological data indicate that low physical activity levels increase the risk of chronic low back pain by approximately 20-30%, underscoring the protective role of regular moderate exercise.[76]Diagnosis
Medical history and examination
The medical history for low back pain begins with a detailed assessment of the pain's onset, which may be sudden or gradual, and its duration, distinguishing acute (less than 6 weeks), subacute (6-12 weeks), or chronic (more than 12 weeks) presentations.[] Clinicians inquire about aggravating and relieving factors, such as mechanical movements that worsen pain or rest that alleviates it, as well as prior episodes to identify patterns of recurrence. Occupational history is essential, evaluating work-related activities like heavy lifting or prolonged sitting that may contribute to symptoms.[] This focused history helps classify the pain as nonspecific, radicular, or indicative of other categories, while screening for potential red flags.[] The physical examination starts with inspection of posture and gait to detect abnormalities like scoliosis or antalgic walking patterns. Palpation assesses for paraspinal tenderness or muscle spasms along the lumbar spine. Range of motion is evaluated through forward flexion, extension, and lateral bending, noting limitations or pain provocation. Neurological tests include the straight-leg raise to identify radiculopathy, along with assessment of reflexes (e.g., patellar and Achilles), muscle strength, and sensation in the lower extremities to rule out nerve root involvement.[] [] Functional assessment quantifies the impact of low back pain on daily activities using validated tools such as the Roland-Morris Disability Questionnaire, a 24-item self-report measure that evaluates disability in tasks like bending or walking.[] This helps gauge severity and guide management planning. Biopsychosocial screening identifies yellow flags—psychosocial factors like fear-avoidance beliefs, negative pain attitudes, or low mood—that may predict chronicity and disability. Tools such as the Örebro Musculoskeletal Pain Screening Questionnaire are recommended for early detection during history-taking.[] Recent guidelines, including those from 2022 and 2023, emphasize a comprehensive history and examination as the initial step in evaluation, recommending against routine imaging unless specific concerns arise from these assessments.[] []Red flag conditions
Red flags in low back pain refer to clinical indicators that suggest potentially serious underlying conditions, such as malignancy, infection, fracture, or cauda equina syndrome, necessitating urgent evaluation, imaging, or specialist referral.[] These signs are present in approximately 1% to 5% of low back pain cases in primary care settings but require prompt action to avoid complications.[] Systemic red flags include unexplained weight loss, persistent fever or chills, recent infection, intravenous drug use, night pain unrelieved by rest, severe or unrelenting pain not improving with rest, age over 50 or under 18 with new onset, long-term steroid use, immunosuppression, and a personal history of cancer, which may indicate metastatic disease or systemic illness.[] These symptoms warrant immediate assessment, as they raise suspicion for non-mechanical causes like tumors or infections. Neurological red flags encompass progressive motor weakness or numbness in the lower extremities or legs, saddle anesthesia (numbness in the perineal area), and urinary or bowel retention or incontinence, which are hallmarks of cauda equina syndrome requiring emergency intervention.[] Such findings suggest spinal cord or nerve root compression and demand rapid referral to prevent permanent neurological damage.[] Patients with these symptoms should seek emergency care. These symptoms, particularly when accompanying low back pain or stiffness in older adults, require immediate medical attention. Traumatic red flags are indicated by recent significant trauma, such as a fall or accident—even minor in older adults or those with osteoporosis—pointing to possible vertebral fracture, which may present as pain or stiffness.[] In these cases, pain or stiffness following injury should prompt evaluation for structural damage, even if no deformity is evident. Inflammatory red flags feature morning stiffness lasting more than 1 hour that improves with physical activity, often suggesting spondyloarthropathies like ankylosing spondylitis.[] This pattern, combined with bilateral sacroiliac joint involvement, differentiates inflammatory from mechanical pain and supports referral for rheumatologic assessment.[] Visceral referred pain — When low back pain is right-sided or unilateral, particularly when accompanied by abdominal symptoms, fever, urinary changes, gastrointestinal disturbances, or other systemic signs, clinicians should consider referred pain from visceral sources as a potential serious non-mechanical cause. Examples include appendicitis, right kidney pathology (e.g., kidney stones or infection), gynecological issues in women (e.g., endometriosis), and abdominal aortic aneurysm. These conditions may require urgent evaluation, as they can represent life-threatening or time-sensitive pathology that demands prompt medical assessment to rule out serious complications.[20][53] Clinicians should obtain imaging or refer patients with red flags indicating severe or progressive neurological deficits or serious underlying conditions, while routine imaging is not recommended for nonspecific low back pain. These criteria emphasize targeted screening to identify the rare but critical subset of cases needing escalation, with no major updates as of 2025.Diagnostic tests
Diagnostic tests for low back pain primarily involve imaging and laboratory evaluations to identify specific underlying causes such as fractures, infections, tumors, or nerve compression, rather than for routine use in nonspecific cases. These tests are guided by clinical suspicion and are not recommended initially for most patients with acute, uncomplicated pain.[] Imaging modalities are selected based on the suspected pathology and presence of red flags. Plain X-rays are useful for assessing bony alignment, fractures, or degenerative changes in the spine, serving as an initial low-cost option when structural abnormalities are suspected.[] Magnetic resonance imaging (MRI) is the gold standard for evaluating soft tissue structures, including intervertebral discs, spinal cord, and nerve roots, particularly in cases of suspected radiculopathy, herniation, or inflammatory conditions like discitis.[] Computed tomography (CT) provides superior detail for bony structures, such as in spinal stenosis or complex fractures, though it involves ionizing radiation exposure.[] Laboratory tests help rule out systemic causes like infection or inflammation. Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) are elevated in inflammatory or infectious processes, such as epidural abscess or osteomyelitis, and are recommended when these are suspected based on history or fever.[] A complete blood count (CBC) can detect leukocytosis indicative of infection.[] For suspected malignancy, tumor markers like prostate-specific antigen (PSA) may be ordered if cancer is a concern, though these are not routine.[] Additional specialized tests include electromyography (EMG) and nerve conduction studies (NCS) to assess for radiculopathy or peripheral neuropathy by measuring electrical activity in muscles and nerves.[] Bone scintigraphy (bone scan) is sensitive for detecting metastases or occult fractures in the spine when cancer history or unexplained pain raises suspicion.[] Current guidelines, including the 2024 World Federation of Neurosurgical Societies (WFNS) recommendations, advise against routine imaging for nonspecific acute low back pain lasting less than 4-6 weeks without red flags, as it does not improve outcomes and may lead to unnecessary interventions.[] Imaging is reserved for cases with red flags (e.g., progressive neurologic deficits, unexplained weight loss) or persistent symptoms beyond 6 weeks.[] Limitations of these tests include the risk of overdiagnosis due to incidental findings, which are common in asymptomatic individuals (e.g., disc abnormalities on MRI in up to 30% of healthy adults), and radiation risks from X-rays and CT scans.[]Prevention
Lifestyle modifications
Lifestyle modifications play a crucial role in preventing and managing low back pain by addressing modifiable risk factors through daily habit changes. Maintaining a healthy body weight is essential, as excess weight increases mechanical stress on the spine. Individuals with a BMI greater than 25 kg/m² experience higher rates of chronic low back pain compared to those with normal weight. Some low-quality evidence suggests that weight loss programs may decrease low back pain intensity and disability in overweight or obese adults.[77][78] Observational studies indicate that dietary patterns influence chronic low back pain through effects on systemic inflammation. Diets high in refined carbohydrates, added sugars, and energy-dense foods are associated with increased odds of chronic spinal or low back pain, potentially mediated by elevated inflammatory markers such as C-reactive protein (CRP) and interleukin-6 (IL-6). For instance, higher added sugar intake has been linked to up to 49% increased odds of chronic spinal pain, while adherence to energy-dense dietary patterns shows a positive association with chronic low back pain. In contrast, higher consumption of whole grains and fiber-rich foods is associated with a lower likelihood of chronic pain. Reducing intake of refined carbohydrates and added sugars while increasing fiber-rich carbohydrates (such as whole grains, fruits, and vegetables) may therefore help mitigate systemic inflammation and potentially reduce the risk or severity of chronic low back pain.[79][9][72] Smoking cessation is another key modification, as tobacco use impairs blood flow to spinal discs, leading to reduced oxygenation and accelerated degeneration. Quitting smoking enhances disc nutrition and overall spinal health, with evidence from systematic reviews demonstrating improved pain levels in individuals with degenerative spinal conditions following cessation.[80] This benefit arises from restored vascular function, which supports tissue repair and reduces inflammation around the spine.[81] Incorporating activity pacing into daily routines helps mitigate the risks associated with prolonged sedentary behavior. Alternating between sitting and standing positions, along with taking regular breaks during desk-based work, prevents excessive strain on the lower back. Interventions promoting reduced sedentary time, such as using sit-stand desks and activity prompts, have been effective in lowering chronic low back pain incidence.[82] Similarly, optimizing sleep hygiene supports spinal recovery; using a supportive mattress that maintains neutral spinal alignment and adopting recommended sleeping positions can help reduce morning pain. These include sleeping on the back with a pillow under the knees to maintain the natural curve of the lower back and relax muscles, and sleeping on the side in the fetal position with a pillow or knee pillow between the knees to support the top leg, prevent it from dropping forward, maintain alignment of the pelvis and spine, and thereby reduce potential twisting that aggravates pain. Sleeping on the stomach should be avoided, as it strains the back and neck by flattening the natural spinal curve and increasing pressure. These positions preserve the natural curve of the lower back, minimizing pressure on discs and muscles.[83][84] Recent evidence underscores the protective effects of regular physical activity within lifestyle changes. A 2025 prospective study found that walking more than 100 minutes per day was associated with a 23% lower risk of developing chronic low back pain compared to less than 78 minutes daily, highlighting the value of incorporating moderate daily movement to bolster spinal resilience.[85]Ergonomic interventions
Ergonomic interventions focus on modifying the physical environment and work practices to minimize mechanical stress on the lower back, thereby reducing the risk of low back pain in occupational and daily settings. These adjustments aim to promote a neutral spine posture, where the natural S-curve of the spine is maintained, distributing loads evenly across the musculoskeletal system.[86] In workstation setups, adjustable chairs with lumbar support are essential to support the lower back's natural curve, with the seat height set so feet rest flat on the floor and thighs are parallel to it, preventing forward leaning that strains the spine. Monitors should be positioned with the top at or slightly below eye level, approximately an arm's length away, to avoid slouching or excessive neck flexion that contributes to back tension. Keyboard positioning should allow elbows to bend at about 90 degrees, with forearms parallel to the floor and wrists straight, enabling a relaxed shoulder and back posture during prolonged sitting. These configurations, recommended by OSHA, help maintain neutral spine alignment and have been shown to decrease reports of musculoskeletal discomfort, including low back pain, among office workers.[87][88][89][90] Proper lifting techniques are critical for manual material handling tasks, where bending at the knees and hips—rather than the waist—while keeping the load close to the body reduces torque on the lumbar spine. Team lifts are advised for objects over 50 pounds to distribute weight and avoid awkward postures, and using mechanical aids like carts or hoists further minimizes risk. NIOSH guidelines emphasize these methods, including the Revised NIOSH Lifting Equation to assess task risks, as they lower the physical demands that lead to low back injuries in high-risk occupations such as warehousing and construction.[91][92] For vehicle adaptations, particularly relevant for drivers in transportation roles, lumbar supports in seats promote spinal lordosis and reduce static loading on the lower back during extended periods. Studies indicate that prominent lumbar support in automobile seats is associated with decreased low back pain reports among drivers. Anti-vibration seats or cushions attenuate whole-body vibration exposure, a known risk factor for low back pain; randomized trials in truck drivers show that active suspension systems reducing vibration lead to improved low back pain outcomes compared to standard seats.[93][94] Home ergonomics involve arranging furniture to facilitate safe movements, such as placing frequently used items at waist height to avoid excessive bending or reaching, which can strain the back. When carrying loads, techniques similar to workplace lifting—bending at the knees and keeping objects close to the torso—prevent undue stress, and using supportive bags or carts for groceries aids in maintaining balance. These practices, aligned with general ergonomic principles, help mitigate cumulative back strain from household activities.[95][92][96] OSHA and NIOSH provide comprehensive guidelines for implementing these interventions, recommending risk assessments and worker training to tailor adjustments to specific job demands. Meta-analyses of ergonomic programs in occupational settings demonstrate significant reductions in work-related musculoskeletal pain, including low back pain, with odds ratios indicating lower prevalence among intervened groups in high-risk jobs. These measures integrate with broader lifestyle modifications to enhance overall prevention of mechanical low back causes.[97][91][98]Management
Non-pharmacological approaches
Non-pharmacological approaches form the cornerstone of management for low back pain across all durations, as recommended by major clinical guidelines that emphasize their use as first-line interventions to promote recovery and prevent chronicity. The World Health Organization's 2023 guideline for non-surgical management of chronic primary low back pain prioritizes holistic, person-centered care incorporating education, exercise, and physical therapies, while the American College of Physicians' guidelines endorse these for acute and subacute cases to reduce pain and disability without medications. Approximately 70% of acute low back pain cases resolve within six months with such conservative strategies, highlighting their effectiveness in facilitating natural recovery. For chronic low back pain (lasting more than 12 weeks), management prioritizes non-pharmacological approaches. Patients are encouraged to stay active and avoid prolonged bed rest, as inactivity can worsen stiffness and deconditioning. Engagement in physical therapy, strengthening and stretching exercises (e.g., yoga, pilates, walking, swimming), and low-impact aerobics is recommended. Self-care measures include application of heat or ice packs, maintaining good posture, and weight management to reduce mechanical stress on the spine.[99][100][101] For nonspecific chronic low back pain persisting after extensive diagnostic workup and potentially involving central nervous system sensitization, treatments emphasize multidisciplinary approaches, including physical therapy, cognitive behavioral therapy, medications targeting nerve pain, and interventional procedures where appropriate.[102] Exercise therapy is a key component, tailored to the pain's duration and individual needs to enhance strength, flexibility, and endurance. For acute low back pain, low-intensity aerobic activities such as walking or swimming are preferred to maintain mobility without exacerbating symptoms, while strengthening exercises targeting core muscles—like bird-dog, plank variations, planks, or bridges—are introduced gradually to support spinal stability and reduce compensatory tightness in paraspinal muscles. In chronic cases, a more structured program combining core strengthening, stretching (e.g., hamstring and hip flexor stretches), and aerobic exercise yields moderate-certainty evidence of reduced pain and improved function compared to no intervention, as shown in a 2021 Cochrane systematic review. These interventions should be supervised initially to ensure proper form and progression, with benefits accruing over 8-12 weeks of consistent participation. Specific lower back stretches commonly recommended for pain relief include:- Knee-to-chest stretch: Lie on your back, pull one knee to your chest, hold for 20-30 seconds, repeat with the other leg and then both.
- Cat-Cow stretch: On all fours, alternate arching and rounding your back.
- Child's pose: Kneel, sit back on heels, reach arms forward, hold.
- Pelvic tilt: Lie on back, tighten abdominals to flatten back against floor.
- Piriformis stretch: Cross one ankle over opposite knee, pull thigh toward chest.
- Knee-to-Chest Stretch: Lie on your back, pull one knee toward your chest while keeping the other foot flat. Hold 5-30 seconds, repeat 2-3 times per leg. Helps relieve lower back tension.
- Cat-Cow Stretch: On hands and knees, alternate arching (cat) and dipping (cow) your back. Repeat 10-20 times. Improves spinal flexibility and reduces stiffness.
- Pelvic Tilt: Lie on your back with knees bent, tighten abs to flatten your lower back against the floor, hold 5-10 seconds. Repeat 10-30 times. Strengthens core and stabilizes the spine.
- Bridge Exercise: Lie on your back, lift hips to form a straight line from knees to shoulders. Hold briefly, repeat 5-30 times. Strengthens glutes and lower back.
- Hamstring Stretch: Lie on your back, raise one leg and gently straighten it. Hold 5-30 seconds per side. Addresses tightness that contributes to back strain from bending.
- Manual therapy: Soft tissue mobilization, myofascial release, and massage to reduce paraspinal tightness and trigger points.
- Stretching exercises: Gentle stretches such as knee-to-chest, cat-cow pose, child's pose, and piriformis stretch to lengthen paraspinal and surrounding muscles.
- Strengthening exercises: Core stabilization (e.g., bird-dog, plank variations) and back extensor strengthening to support the spine and reduce compensatory tightness.
- Heat therapy: Application of moist heat to relax muscles before stretching or exercise.
- Postural education and ergonomic training: To prevent ongoing strain.
- Modalities: Ultrasound or electrical stimulation in some cases for pain relief.[99]