Recent from talks
Nothing was collected or created yet.
Brucellosis
View on Wikipedia
This article needs additional citations for verification. (March 2025) |
| Brucellosis | |
|---|---|
| Other names | undulant fever, undulating fever, Mediterranean fever, Malta fever, Cyprus fever, rock fever (Micrococcus melitensis)[1] |
| Specialty | Infectious disease |
| Symptoms | fever, chills, loss of appetite, sweats, weakness, fatigue, joint pain, muscle pain, back pain, headache.[2] |
| Complications | central nervous system infections (meningitis, encephalitis), inflammation and infection of the spleen and liver, infection and inflammation of the epididymus and testicles (epididymo-orchitis), arthritis, inflammation of the inner lining of the heart chambers (endocarditis).[2] |
| Causes | Ingestion of bacteria within the genus Brucella |
| Diagnostic method | x-rays, computerized tomography (CT) scan or magnetic resonance imaging (MRI), cerebrospinal fluid culture, echocardiography.[3] |
| Prevention | avoid unpasteurized dairy foods, cook meat thoroughly, wear gloves, take safety precautions in high-risk workplaces, vaccinate domestic animals.[2] |
| Treatment | antibiotics |
| Medication | doxycycline, rifampicin, aminoglycosides [specify] |
Brucellosis[4] is a zoonosis spread primarily via ingestion of unpasteurized milk from infected animals.[5] It is also known as undulant fever, Malta fever, and Mediterranean fever.[6]
The bacteria causing this disease, Brucella, are small, Gram-negative, nonmotile, nonspore-forming, rod-shaped (coccobacilli) bacteria. They function as facultative intracellular parasites, causing chronic disease, which usually persists for life. Four species infect humans: B. abortus, B. canis, B. melitensis, and B. suis. B. abortus is less virulent than B. melitensis and is primarily a disease of cattle. B. canis affects dogs. B. melitensis is the most virulent and invasive species; it usually infects goats and occasionally sheep. B. suis is of intermediate virulence and chiefly infects pigs. Symptoms include profuse sweating and joint and muscle pain. Brucellosis has been recognized in animals and humans since the early 20th century.[7][8]
Signs and symptoms
[edit]
The symptoms are like those associated with many other febrile diseases, but with emphasis on muscular pain and night sweats. The duration of the disease can vary from a few weeks to many months or even years.
In the first stage of the disease, bacteremia occurs and leads to the classic triad of undulant fevers, sweating (often with a characteristic foul, moldy smell sometimes likened to wet hay), and migratory arthralgia and myalgia (joint and muscle pain).[10] Blood tests characteristically reveal a low number of white blood cells and red blood cells, show some elevation of liver enzymes such as aspartate aminotransferase and alanine aminotransferase, and demonstrate positive Bengal rose and Huddleston reactions. Gastrointestinal symptoms occur in 70% of cases and include nausea, vomiting, decreased appetite, unintentional weight loss, abdominal pain, constipation, diarrhea, an enlarged liver, liver inflammation, liver abscess, and an enlarged spleen.[11]
This complex is, at least in Portugal, Israel, Syria, Iran, and Jordan, known as Malta fever. During episodes of Malta fever, melitococcemia (presence of brucellae in the blood) can usually be demonstrated using blood culture in tryptose medium or Albini medium. If untreated, the disease can give rise to focalizations[clarification needed] or become chronic. The focalizations of brucellosis usually occur in bones and joints, and osteomyelitis or spondylodiscitis of the lumbar spine, accompanied by sacroiliitis, is very characteristic of this disease. Orchitis is also common in men.
The consequences of Brucella infection are highly variable and may include arthritis, spondylitis, thrombocytopenia, meningitis, uveitis, optic neuritis, endocarditis, and various neurological disorders collectively known as neurobrucellosis.
Cause
[edit]
Brucellosis in humans is usually associated with consumption of unpasteurized milk and soft cheeses made from the milk of infected animals—often goats—infected with B. melitensis, and with occupational exposure of laboratory workers, veterinarians, and slaughterhouse workers. These infected animals may be healthy and asymptomatic.[12] Some vaccines used in livestock, most notably B. abortus strain 19, also cause disease in humans if accidentally injected. Brucellosis induces inconstant fevers, miscarriage, sweating, weakness, anemia, headaches, depression, and muscular and bodily pain. The other strains, B. suis and B. canis, cause infection in pigs and dogs, respectively.[13]
Overall findings support that brucellosis poses an occupational risk to goat farmers with specific areas of concern including weak awareness of disease transmission to humans and lack of knowledge on specific safe farm practices such as quarantine practices.[14]
Wildlife reservoirs and zoonotic transmission
[edit]Brucellosis affects both domestic and wildlife species, with the latter serving as significant reservoirs that contribute to disease persistence and transmission. Notably, bison, elk, wild boars, and deer have been identified as carriers, particularly in North America and Europe[15] Humans can contract the disease through direct handling of infected animals, aerosol exposure, or consumption of undercooked game meat.[16] Additionally, the wildlife trade has been implicated in the geographical spread of brucellosis, as the movement and sale of infected animals, particularly in unregulated markets, introduce the bacteria into new ecosystems, increasing disease risks for both humans and animals.[17] Reports from Central Asia and sub-Saharan Africa highlight cases where wildlife trafficking has facilitated brucellosis outbreaks in non-endemic regions.[18]
Transmission through hunting and game meat consumption
[edit]Hunters and individuals who consume wild game face an elevated risk of brucellosis exposure due to direct contact with infected animals and inadequate meat preparation. Transmission can occur during field-dressing or handling of infected carcasses, as Brucella bacteria can enter the body through skin abrasions, mucous membranes, or inhalation of aerosolized pathogens.[19] Additionally, the consumption of undercooked or improperly handled wild game meat remains a significant risk factor, particularly in regions where game animals constitute a primary food source. Implementing protective measures, such as the use of personal protective equipment (PPE) during handling and ensuring thorough cooking of game meat, is essential to mitigating the risk of brucellosis transmission within hunting communities.
Diagnosis
[edit]
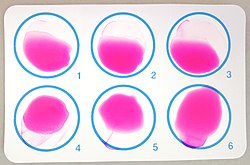
The diagnosis of brucellosis relies on:[20]
- Demonstration of the agent: blood cultures in tryptose broth, bone marrow cultures. The growth of brucellae is extremely slow (they can take up to two months to grow), and the culture poses a risk to laboratory personnel due to the high infectivity of brucellae.
- Demonstration of antibodies against the agent, either with the classic Huddleson, Wright, and/or Bengal Rose reactions, either with ELISA or the 2-mercaptoethanol assay for IgM antibodies associated with chronic disease
- Histologic evidence of granulomatous hepatitis on hepatic biopsy
- Radiologic alterations in infected vertebrae: the Pedro Pons sign (preferential erosion of the anterosuperior corner of lumbar vertebrae) and marked osteophytosis are suspicious of brucellic spondylitis.
Definite diagnosis of brucellosis requires the isolation of the organism from the blood, body fluids, or tissues, but serological methods may be the only tests available in many settings. Positive blood culture yield ranges between 40 and 70% and is less commonly positive for B. abortus than B. melitensis or B. suis. Identification of specific antibodies against bacterial lipopolysaccharide and other antigens can be detected by the standard agglutination test (SAT), rose Bengal, 2-mercaptoethanol (2-ME), antihuman globulin (Coombs') and indirect enzyme-linked immunosorbent assay (ELISA). SAT is the most commonly used serology in endemic areas.[21][22] An agglutination titre greater than 1:160 is considered significant in nonendemic areas and greater than 1:320 in endemic areas.[citation needed]
Due to the similarity of the O polysaccharide of Brucella to that of various other Gram-negative bacteria (e.g. Francisella tularensis, Escherichia coli, Salmonella urbana, Yersinia enterocolitica, Vibrio cholerae, and Stenotrophomonas maltophilia), the appearance of cross-reactions of class M immunoglobulins may occur. The inability to diagnose B. canis by SAT due to lack of cross-reaction is another drawback. False-negative SAT may be caused by the presence of blocking antibodies (the prozone phenomenon) in the α2-globulin (IgA) and in the α-globulin (IgG) fractions.[citation needed]
Dipstick assays are new and promising, based on the binding of Brucella IgM antibodies, and are simple, accurate, and rapid. ELISA typically uses cytoplasmic proteins as antigens. It measures IgM, IgG, and IgA with better sensitivity and specificity than the SAT in most recent comparative studies.[23] The commercial Brucellacapt test, a single-step immunocapture assay for the detection of total anti-Brucella antibodies, is an increasingly used adjunctive test when resources permit. PCR is fast and should be specific. Many varieties of PCR have been developed (e.g., nested PCR, real-time PCR, and PCR-ELISA) and found to have superior specificity and sensitivity in detecting both primary infection and relapse after treatment.[24] Unfortunately, these are not standardized for routine use, and some centres have reported persistent PCR positivity after clinically successful treatment, fuelling the controversy about the existence of prolonged chronic brucellosis.[citation needed]
Other laboratory findings include normal peripheral white cell count, and occasional leucopenia with relative lymphocytosis. The serum biochemical profiles are commonly normal.[25]
Prevention
[edit]Livestock vaccination and disease surveillance
[edit]Vaccination is the most effective method for controlling brucellosis in livestock. In cattle, the most common vaccines are Brucella abortus strain 19 and RB51,[26] while for goats and sheep, B. melitensis Rev-1 is used. Other methods include regular serological screening, and the culling of infected animals helps prevent the spread of disease. In many countries, mandatory vaccination programs[27] and test-and-slaughter policies have been shown to significantly reduce brucellosis incidence in livestock populations.[28][29]
Food safety and pasteurization
[edit]Brucellosis is commonly transmitted to humans through the consumption of unpasteurized dairy products, particularly raw milk and cheese. Pasteurization is one of the most effective methods to eliminate Brucella with many countries implementing it while hosting public educational campaigns to discourage the consumption of raw dairy.[30]
Wildlife reservoirs and disease control
[edit]Wild animals, including bison, elk, wild boars, and deer, serve as natural reservoirs for Brucella. Spillover infections from wildlife to livestock pose ongoing challenges, particularly in regions with dairy farms.[31] Control measures include restricted feeding areas, selective culling, and experimental wildlife vaccination programs. Hunters and individuals handling game meat are advised to wear protective gloves and cook meat thoroughly to prevent infection.[32]
Occupational safety and laboratory precautions
[edit]Brucellosis poses an occupational hazard for veterinarians, farmers, slaughterhouse workers, and laboratory personnel who handle infected animals or biological specimens. Common preventive measures include the use of personal protective equipment (PPE), proper ventilation in slaughterhouses, and adherence to laboratory biosafety protocols.[33] Accidental exposure in laboratory settings can occur through aerosolized bacteria or direct contact with infected samples, necessitating post-exposure antibiotic prophylaxis.[34]
Public health education and community awareness
[edit]Educational initiatives are essential to reducing brucellosis transmission, particularly in rural communities where unpasteurized dairy products remain widely consumed. Public health campaigns emphasize the importance of basic knowledge of brucellosis disease and transmission, safe food handling, and vaccination compliance.[35]
International disease control efforts and One Health integration
[edit]Brucellosis control relies on a One Health approach integrating human, animal, and environmental health. Global organizations, including the World Health Organization (WHO), Food and Agriculture Organization (FAO), World Organisation for Animal Health (WOAH), and United Nations Environment Programme (UNEP),[36] advocate for integrated strategies to manage health threats across humans, animals, plants, and the environment, to prevent prevent future pandemics. Collaborative efforts to identify risk factors enhances outbreak surveillance, livestock vaccination programs, and food safety regulations such as mandatory pasteurization, ensuring a sustainable and comprehensive approach disease management.[37]
Treatment
[edit]Antibiotics such as tetracyclines, rifampicin, and the aminoglycosides streptomycin and gentamicin are effective against Brucella bacteria. However, the use of more than one antibiotic is needed for several weeks, because the bacteria incubate within cells.[citation needed]
The gold standard treatment for adults is daily intramuscular injections of streptomycin 1 g for 14 days and oral doxycycline 100 mg twice daily for 45 days (concurrently). Gentamicin 5 mg/kg by intramuscular injection once daily for 7 days is an acceptable substitute when streptomycin is not available or contraindicated.[38] Another widely used regimen is doxycycline plus rifampicin twice daily for at least 6 weeks. This regimen has the advantage of oral administration. A triple therapy of doxycycline, with rifampicin and co-trimoxazole, has been used successfully to treat neurobrucellosis.[39] Doxycycline plus streptomycin regimen (for 2 to 3 weeks) is more effective than doxycycline plus rifampicin regimen (for 6 weeks).[40]
Doxycycline can cross the blood–brain barrier, but requires the addition of two other drugs to prevent relapse. Ciprofloxacin and co-trimoxazole therapy are associated with an unacceptably high rate of relapse. In brucellic endocarditis, surgery is required for an optimal outcome. Even with optimal antibrucellic therapy, relapses still occur in 5 to 10% of patients with Malta fever.[citation needed]
Prognosis
[edit]The mortality of the disease in 1909, as recorded in the British Army and Navy stationed in Malta, was 2%. The most frequent cause of death was endocarditis. Recent advances in antibiotics and surgery have been successful in preventing death due to endocarditis. Prevention of human brucellosis can be achieved by eradication of the disease in animals by vaccination and other veterinary control methods, such as testing herds/flocks and slaughtering animals when infection is present. Currently, no effective vaccine is available for humans. Boiling milk before consumption, or before using it to produce other dairy products, is protective against transmission via ingestion. Changing the traditional food habits of eating raw meat, liver, or bone marrow is necessary, but difficult to implement.[citation needed] Patients who have had brucellosis should probably be excluded indefinitely from donating blood or organs. [citation needed] Exposure of diagnostic laboratory personnel to Brucella organisms remains a problem in both endemic settings and when brucellosis is unknowingly imported by a patient.[41] After appropriate risk assessment, staff with significant exposure should be offered postexposure prophylaxis and followed up serologically for 6 months.[42]
Epidemiology
[edit]Argentina
[edit]According to a study published in 2002, an estimated 10–13% of farm animals were infected with Brucella species.[43] Annual losses from the disease were calculated at around US$60 million. Since 1932, government agencies have undertaken efforts to contain the disease. As of 2022[update], all cattle aged 3–8 months must receive the Brucella abortus strain 19 vaccine.[44]
Australia
[edit]Australia is free of cattle brucellosis, although it occurred in the past. Brucellosis of sheep or goats has never been reported. Brucellosis of pigs does occur. Feral pigs are the typical source of human infections.[45][46]
Canada
[edit]On 19 September 1985, the Canadian government declared its cattle population brucellosis-free. Brucellosis ring testing of milk and cream, and testing of cattle to be slaughtered, ended on 1 April 1999. Monitoring continues through testing at auction markets, through standard disease-reporting procedures, and testing of cattle being qualified for export to countries other than the United States.[47]
China
[edit]An outbreak infecting humans took place in Lanzhou in 2019 after the Lanzhou Biopharmaceutical Plant, which was involved in vaccine production, accidentally pumped out the bacteria into the atmosphere in exhaust air due to use of expired disinfectant.[48][49]
According to Georgios Pappas, an infectious-disease specialist and author of a report published in the journal Clinical Infectious Diseases,[50] the result was "possibly the largest laboratory accident in the history of infectious diseases." According to Pappas, out of nearly 70,000 people tested, more than 10,000 were seropositive, citing figures compiled by the provincial health authorities in Lanzhou's Gansu province. Pappas also states that Chinese documents show that more than 3,000 people living near the plant applied for compensation, an indication of at least a mild illness.[51]
Europe
[edit]
Malta
[edit]Until the early 20th century, the disease was endemic in Malta to the point of it being referred to as "Maltese fever". Since 2005, due to a strict regimen of certification of milk animals and widespread use of pasteurization, the illness has been eradicated from Malta.[52]
Republic of Ireland
[edit]Ireland was declared free of brucellosis on 1 July 2009. It had troubled the country's farmers and veterinarians for several decades.[53][54] The Irish government submitted an application to the European Commission, which verified that Ireland had been liberated.[54] Brendan Smith, Ireland's then Minister for Agriculture, Food and the Marine, said the elimination of brucellosis was "a landmark in the history of disease eradication in Ireland".[53][54] Ireland's Department of Agriculture, Food and the Marine intends to reduce its brucellosis eradication programme now that eradication has been confirmed.[53][54]
UK
[edit]Mainland Britain has been free of brucellosis since 1979, although there have been episodic reintroductions since.[55] The last outbreak of brucellosis in Great Britain was in cattle in Cornwall in 2004.[55][56] Northern Ireland was declared officially brucellosis-free in 2015.[55]
New Zealand
[edit]Brucellosis in New Zealand is limited to sheep (B. ovis). The country is free of all other species of Brucella.[57]
United States
[edit]Dairy herds in the U.S. are tested at least once a year to be certified brucellosis-free[58] with the Brucella milk ring test.[59] Cows confirmed to be infected are often killed. In the United States, veterinarians are required [citation needed] to vaccinate all young stock, to further reduce the chance of zoonotic transmission. This vaccination is usually referred to as a "calfhood" vaccination. Most cattle receive a tattoo in one of their ears, serving as proof of their vaccination status. This tattoo also includes the last digit of the year they were born.[60]
The first state–federal cooperative efforts towards eradication of brucellosis caused by B. abortus in the U.S. began in 1934.[citation needed]
Brucellosis was originally imported to North America with non-native domestic cattle (Bos taurus), which transmitted the disease to wild bison (Bison bison) and elk (Cervus canadensis). No records exist of brucellosis in ungulates native to America until the early 19th century.[61]
History
[edit]

Brucellosis first came to the attention of British medical officers in the 1850s in Malta during the Crimean War, and was referred to as Malta Fever. Jeffery Allen Marston (1831–1911) described his case of the disease in 1861. The causal relationship between organism and disease was first established in 1887 by David Bruce.[62][63] Bruce considered the agent spherical and classified it as a coccus.[citation needed]
In 1897, Danish veterinarian Bernhard Bang isolated a bacillus as the agent of heightened spontaneous abortion in cows, and the name "Bang's disease" was assigned to this condition. Bang considered the organism rod-shaped and classified it as a bacillus. At the time, no one knew that this bacillus had anything to do with the causative agent of Malta fever.[64]
Maltese scientist and archaeologist Themistocles Zammit identified unpasteurized goat milk as the major etiologic factor of undulant fever in June 1905.[65]
In the late 1910s, American bacteriologist Alice C. Evans was studying the Bang bacillus and gradually realized that it was virtually indistinguishable from the Bruce coccus.[66] The short-rod versus oblong-round morphologic borderline explained the leveling of the erstwhile bacillus/coccus distinction (that is, these "two" pathogens were not a coccus versus a bacillus but rather were one coccobacillus).[66] The Bang bacillus was already known to be enzootic in American dairy cattle, which showed itself in the regularity with which herds experienced contagious abortion.[66] Having made the discovery that the bacteria were certainly nearly identical and perhaps totally so, Evans then wondered why Malta fever was not widely diagnosed or reported in the United States.[66] She began to wonder whether many cases of vaguely defined febrile illnesses were in fact caused by the drinking of raw (unpasteurized) milk.[66] During the 1920s, this hypothesis was vindicated. Such illnesses ranged from undiagnosed and untreated gastrointestinal upset to misdiagnosed[66] febrile and painful versions, some even fatal. This advance in bacteriological science sparked extensive changes in the American dairy industry to improve food safety. The changes included making pasteurization standard and greatly tightening the standards of cleanliness in milkhouses on dairy farms. The expense prompted delay and skepticism in the industry,[66] but the new hygiene rules eventually became the norm. Although these measures have sometimes struck people as overdone in the decades since, being unhygienic at milking time or in the milkhouse, or drinking raw milk, is not a safe alternative.[citation needed]
In the decades after Evans's work, this genus, which received the name Brucella in honor of Bruce, was found to contain several species with varying virulence. The name "brucellosis" gradually replaced the 19th-century names Mediterranean fever and Malta fever.[67]
Neurobrucellosis, a neurological involvement in brucellosis, was first described in 1879. In the late 19th century, its symptoms were described in more detail by M. Louis Hughes, a Surgeon-Captain of the Royal Army Medical Corps stationed in Malta who isolated brucella organisms from a patient with meningo-encephalitis.[68] In 1989, neurologists in Saudi Arabia made significant contributions to the medical literature involving neurobrucellosis.[69][70]
These obsolete names have previously been applied to brucellosis:[67][71]
- Crimean fever
- Cyprus fever
- Gibraltar fever
- Goat fever
- Italian fever
- Neapolitan fever
Biological warfare
[edit]Brucella species had been weaponized by several advanced countries by the mid-20th century. In 1954, B. suis became the first agent weaponized by the United States at its Pine Bluff Arsenal near Pine Bluff, Arkansas. Brucella species survive well in aerosols and resist drying. Brucella and all other remaining biological weapons in the U.S. arsenal were destroyed in 1971–72 when the American offensive biological warfare program was discontinued by order of President Richard Nixon.[72]
The experimental American bacteriological warfare program focused on three agents of the Brucella group:[citation needed]
- Porcine brucellosis (agent US)
- Bovine brucellosis (agent AA)
- Caprine brucellosis (agent AM)
Agent US was in advanced development by the end of World War II. When the United States Air Force (USAF) wanted a biological warfare capability, the Chemical Corps offered Agent US in the M114 bomblet, based on the four-pound bursting bomblet developed for spreading anthrax during World War II. Though the capability was developed, operational testing indicated the weapon was less than desirable, and the USAF designed it as an interim capability until it could eventually be replaced by a more effective biological weapon.[citation needed]
The main drawback of using the M114 with Agent US was that it acted mainly as an incapacitating agent, whereas the USAF administration wanted deadly weapons. The stability of M114 in storage was too low to allow for storing it at forward air bases, and the logistical requirements to neutralize a target were far higher than originally planned. Ultimately, this would have required too much logistical support to be practical in the field.[citation needed]
Agents US and AA had a median infective dose of 500 organisms/person, and for Agent AM, it was 300 organisms/person. The incubation time was believed to be about 2 weeks, with a duration of infection of several months. The lethality estimate was, based on epidemiological information, 1 to 2 per cent. Agent AM was believed to be a somewhat more virulent disease, with a fatality rate of 3 per cent being expected.[citation needed]
Other animals
[edit]Species infecting domestic livestock are B. abortus (cattle, bison, and elk), B. canis (dogs), B. melitensis (goats and sheep), B. ovis (sheep), and B. suis (caribou and pigs). Brucella species have also been isolated from several marine mammal species (cetaceans and pinnipeds).[citation needed]
Cattle
[edit]B. abortus is the principal cause of brucellosis in cattle. The bacteria are shed from an infected animal at or around the time of calving or abortion. Once exposed, the likelihood of an animal becoming infected is variable, depending on age, pregnancy status, and other intrinsic factors of the animal, as well as the number of bacteria to which the animal was exposed.[73] The most common clinical signs of cattle infected with B. abortus are high incidences of abortions, arthritic joints, and retained placenta.[citation needed]
The two main causes for spontaneous abortion in animals are erythritol, which can promote infections in the fetus and placenta,[clarification needed], and the lack of anti-Brucella activity in the amniotic fluid. Males can also harbor the bacteria in their reproductive tracts, namely seminal vesicles, ampullae, testicles, and epididymises.[citation needed]
Dogs
[edit]The causative agent of brucellosis in dogs, B. canis, is transmitted to other dogs through breeding and contact with aborted fetuses. Brucellosis can occur in humans who come in contact with infected aborted tissue or semen. The bacteria in dogs normally infect the genitals and lymphatic system, but can also spread to the eyes, kidneys, and intervertebral discs. Brucellosis in the intervertebral disc is one possible cause of discospondylitis. Symptoms of brucellosis in dogs include abortion in female dogs and scrotal inflammation and orchitis in males. Fever is uncommon. Infection of the eye can cause uveitis, and infection of the intervertebral disc can cause pain or weakness. Blood testing of the dogs prior to breeding can prevent the spread of this disease. It is treated with antibiotics, as with humans, but it is difficult to cure.[74]
Aquatic wildlife
[edit]Brucellosis in cetaceans is caused by the bacterium B. ceti. First discovered in the aborted fetus of a bottlenose dolphin, the structure of B. ceti is similar to Brucella in land animals. B. ceti is commonly detected in two suborders of cetaceans, the Mysticeti and Odontoceti. The Mysticeti include four families of baleen whales, filter-feeders, and the Odontoceti include two families of toothed cetaceans ranging from dolphins to sperm whales. B. ceti is believed to transfer from animal to animal through sexual intercourse, maternal feeding, aborted fetuses, placental issues, from mother to fetus, or through fish reservoirs. Brucellosis is a reproductive disease, so it has an extreme negative impact on the population dynamics of a species. This becomes a greater issue when the already low population numbers of cetaceans are taken into consideration. B. ceti has been identified in four of the 14 cetacean families, but the antibodies have been detected in seven of the families. This indicates that B. ceti is common amongst cetacean families and populations. Only a small percentage of exposed individuals become ill or die. However, particular species apparently are more likely to become infected by B. ceti. The harbor porpoise, striped dolphin, white-sided dolphin, bottlenose dolphin, and common dolphin have the highest frequency of infection amongst odontocetes. In the mysticetes families, the northern minke whale is by far the most infected species. Dolphins and porpoises are more likely to be infected than cetaceans such as whales. Concerning sex and age biases, the infections do not seem influenced by an individual's age or sex. Although fatal to cetaceans, B. ceti has a low infection rate for humans.[75]
Terrestrial wildlife
[edit]The disease in its various strains can infect multiple wildlife species, including elk (Cervus canadensis), bison (Bison bison), African buffalo (Syncerus caffer), European wild boar (Sus scrofa), caribou (Rangifer tarandus), moose (Alces alces), and marine mammals (see section on aquatic wildlife above).[76][77] While some regions use vaccines to prevent the spread of brucellosis between infected and uninfected wildlife populations, no suitable brucellosis vaccine for terrestrial wildlife has been developed.[78] This gap in medicinal knowledge creates more pressure for management practices that reduce spread of the disease.[78]
Wild bison and elk in the greater Yellowstone area are the last remaining reservoir of B. abortus in the US. The recent transmission of brucellosis from elk back to cattle in Idaho and Wyoming illustrates how the area, as the last remaining reservoir in the United States, may adversely affect the livestock industry. Eliminating brucellosis from this area is a challenge, as many viewpoints exist on how to manage diseased wildlife. However, the Wyoming Game and Fish Department has recently begun to protect scavengers (particularly coyotes and red fox) on elk feedgrounds, because they act as sustainable, no-cost, biological control agents by removing infected elk fetuses quickly.[79]
The National Elk Refuge in Jackson, Wyoming, asserts that the intensity of the winter feeding program affects the spread of brucellosis more than the population size of elk and bison.[76] Since concentrating animals around food plots accelerates spread of the disease, management strategies to reduce herd density and increase dispersion could limit its spread.[76]
See also
[edit]References
[edit]- ^ Wyatt HV (2014). "How did Sir David Bruce forget Zammit and his goats ?" (PDF). Journal of Maltese History. 4 (1). Malta: Department of History, University of Malta: 41. ISSN 2077-4338. Archived from the original (PDF) on 2016-07-21. Journal archive
- ^ a b c "Brucellosis". mayoclinic.org. Mayo Clinic. Retrieved June 5, 2022.
- ^ "Brucellosis". mayoclinic.org. Mayo Clinic. Retrieved June 5, 2022.
- ^ "Brucellosis". American Heritage Dictionary. Archived from the original on 2011-06-06.
- ^ "Diagnosis and Management of Acute Brucellosis in Primary Care" (PDF). Brucella Subgroup of the Northern Ireland Regional Zoonoses Group. August 2004. Archived from the original (PDF) on 2007-10-13.
- ^ Di Pierdomenico A, Borgia SM, Richardson D, Baqi M (July 2011). "Brucellosis in a returned traveller". CMAJ. 183 (10): E690-2. doi:10.1503/cmaj.091752. PMC 3134761. PMID 21398234.
- ^ Park. K., Park's textbook of preventive and social medicine, 23rd edition. Page 290-91
- ^ Roy R (2013), "Chapter-23 Biostatistics", Mahajan and Gupta Textbook of Preventive and Social Medicine, Jaypee Brothers Medical Publishers (P) Ltd, pp. 434–449, doi:10.5005/jp/books/12262_23 (inactive 1 July 2025), ISBN 978-93-5090-187-8
{{citation}}: CS1 maint: DOI inactive as of July 2025 (link) - ^ "Brucellosis: Resources: Surveillance". CDC. 2018-10-09.
- ^ Hayoun MA, Muco E, Shorman M (2023), "Brucellosis", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 28722861, retrieved 2023-11-08
- ^ "Access Anytime Anywhere". Cleveland Clinic. Retrieved 2025-06-07.
- ^ Wyatt HV (October 2005). "How Themistocles Zammit found Malta Fever (brucellosis) to be transmitted by the milk of goats". Journal of the Royal Society of Medicine. 98 (10). The Royal Society of Medicine Press: 451–4. doi:10.1177/014107680509801009. OCLC 680110952. PMC 1240100. PMID 16199812.
- ^ "Top-ranked Hospital in the Nation". Mayo Clinic. Retrieved 2025-06-07.
- ^ Peck ME, Jenpanich C, Amonsin A, Bunpapong N, Chanachai K, Somrongthong R, et al. (January 2019). "Knowledge, Attitudes and Practices Associated with Brucellosis among Small-Scale Goat Farmers in Thailand". Journal of Agromedicine. 24 (1): 56–63. doi:10.1080/1059924X.2018.1538916. PMID 30350754. S2CID 53034163.
- ^ Godfroid J, Al Dahouk S, Pappas G, Roth F, Matope G, Muma J, Marcotty T, Pfeiffer D, Skjerve E (2013-05-01). "A "One Health" surveillance and control of brucellosis in developing countries: Moving away from improvisation". Comparative Immunology, Microbiology and Infectious Diseases. Special issue: One Health. 36 (3): 241–248. doi:10.1016/j.cimid.2012.09.001. hdl:2263/21766. ISSN 0147-9571. PMID 23044181.
- ^ CDC (2024-06-04). "About Brucellosis". Brucellosis. Retrieved 2025-03-19.
- ^ Karesh WB, Cook RA, Bennett EL, Newcomb J (July 2005). "Wildlife Trade and Global Disease Emergence". Emerging Infectious Diseases. 11 (7): 1000–1002. doi:10.3201/eid1107.050194. ISSN 1080-6040. PMC 3371803. PMID 16022772.
- ^ Qureshi KA, Parvez A, Fahmy NA, Abdel Hady BH, Kumar S, Ganguly A, Atiya A, Elhassan GO, Alfadly SO, Parkkila S, Aspatwar A (2023-12-12). "Brucellosis: epidemiology, pathogenesis, diagnosis and treatment–a comprehensive review". Annals of Medicine. 55 (2). doi:10.1080/07853890.2023.2295398. ISSN 0785-3890. PMC 10769134. PMID 38165919.
- ^ "Brucellosis". www.pa.gov. Retrieved 2025-03-19.
- ^ "Top-ranked Hospital in the Nation". Mayo Clinic. Retrieved 2025-06-07.
- ^ Franco MP, Mulder M, Gilman RH, Smits HL (December 2007). "Human brucellosis". The Lancet. Infectious Diseases. 7 (12): 775–86. doi:10.1016/S1473-3099(07)70286-4. PMID 18045560.
- ^ Al Dahouk S, Nöckler K (July 2011). "Implications of laboratory diagnosis on brucellosis therapy". Expert Review of Anti-Infective Therapy. 9 (7): 833–45. doi:10.1586/eri.11.55. PMID 21810055. S2CID 5068325.
- ^ Mantur B, Parande A, Amarnath S, Patil G, Walvekar R, Desai A, et al. (August 2010). "ELISA versus conventional methods of diagnosing endemic brucellosis". The American Journal of Tropical Medicine and Hygiene. 83 (2): 314–8. doi:10.4269/ajtmh.2010.09-0790. PMC 2911177. PMID 20682874.
- ^ Yu WL, Nielsen K (August 2010). "Review of detection of Brucella spp. by polymerase chain reaction". Croatian Medical Journal. 51 (4): 306–13. doi:10.3325/cmj.2010.51.306. PMC 2931435. PMID 20718083.
- ^ Vrioni G, Pappas G, Priavali E, Gartzonika C, Levidiotou S (June 2008). "An eternal microbe: Brucella DNA load persists for years after clinical cure". Clinical Infectious Diseases. 46 (12): e131-6. doi:10.1086/588482. PMID 18462106.
- ^ "Disease Alert: Bovine Brucellosis". www.aphis.usda.gov. Retrieved 2025-03-19.
- ^ Singh BB, Kostoulas P, Gill JP, Dhand NK (2018-05-10). Wunder E (ed.). "Cost-benefit analysis of intervention policies for prevention and control of brucellosis in India". PLOS Neglected Tropical Diseases. 12 (5) e0006488. doi:10.1371/journal.pntd.0006488. ISSN 1935-2735. PMC 5963803. PMID 29746469.
- ^ Zamri-Saad M, Kamarudin MI (2016-12-01). "Control of animal brucellosis: The Malaysian experience". Asian Pacific Journal of Tropical Medicine. 9 (12): 1136–1140. doi:10.1016/j.apjtm.2016.11.007. ISSN 1995-7645. PMID 27955740.
- ^ Bahmani N, Bahmani A (January 2022). "A review of brucellosis in the Middle East and control of animal brucellosis in an Iranian experience". Reviews in Medical Microbiology. 33 (1): e63 – e69. doi:10.1097/MRM.0000000000000266. ISSN 2770-3150.
- ^ Dadar M, Tiwari R, Sharun K, Dhama K (2021-01-01). "Importance of brucellosis control programs of livestock on the improvement of one health". Veterinary Quarterly. 41 (1): 137–151. doi:10.1080/01652176.2021.1894501. ISSN 0165-2176. PMC 7946044. PMID 33618618.
- ^ Bardenstein S, Grupel D, Blum SE, Motro Y, Moran-Gilad J (2023). "Public and animal health risks associated with spillover of Brucella melitensis into dairy farms". Microbial Genomics. 9 (4): 001014. doi:10.1099/mgen.0.001014. ISSN 2057-5858. PMC 10210956. PMID 37115199.
- ^ CDC (2024-06-04). "About Brucellosis". Brucellosis. Retrieved 2025-03-19.
- ^ Pereira CR, Cotrim de Almeida JV, Cardoso de Oliveira IR, Faria de Oliveira L, Pereira LJ, Zangerônimo MG, Lage AP, Dorneles EM (2020-05-11). Lin T (ed.). "Occupational exposure to Brucella spp.: A systematic review and meta-analysis". PLOS Neglected Tropical Diseases. 14 (5) e0008164. doi:10.1371/journal.pntd.0008164. ISSN 1935-2735. PMC 7252629. PMID 32392223.
- ^ CDC (2024-06-24). "Laboratory Risks for Brucellosis". Brucellosis. Retrieved 2025-03-19.
- ^ Ghugey SL, Setia MS, Deshmukh JS (August 2022). "The effects of health education intervention on promoting knowledge, beliefs and preventive behaviors on brucellosis among rural population in Nagpur district of Maharashtra state, India". Journal of Family Medicine and Primary Care. 11 (8): 4635–4643. doi:10.4103/jfmpc.jfmpc_1562_21. ISSN 2249-4863. PMC 9638594. PMID 36352929.
- ^ "Quadripartite Secretariat for One Health". www.who.int. Retrieved 2025-03-19.
- ^ FAO, UNEP, WHO, WOAH (2022). One Health Joint Plan of Action, 2022–2026. FAO ; UNEP ; WHO ; World Organisation for Animal Health (WOAH). ISBN 978-92-5-136957-9.
- ^ Hasanjani Roushan MR, Mohraz M, Hajiahmadi M, Ramzani A, Valayati AA (April 2006). "Efficacy of gentamicin plus doxycycline versus streptomycin plus doxycycline in the treatment of brucellosis in humans". Clinical Infectious Diseases. 42 (8): 1075–80. doi:10.1086/501359. PMID 16575723.
- ^ McLean DR, Russell N, Khan MY (October 1992). "Neurobrucellosis: clinical and therapeutic features". Clinical Infectious Diseases. 15 (4): 582–90. doi:10.1093/clind/15.4.582. PMID 1420670.
- ^ Yousefi-Nooraie R, Mortaz-Hejri S, Mehrani M, Sadeghipour P (October 2012). "Antibiotics for treating human brucellosis". The Cochrane Database of Systematic Reviews. 10 (10) CD007179. doi:10.1002/14651858.cd007179.pub2. PMC 6532606. PMID 23076931.
- ^ Yagupsky P, Baron EJ (August 2005). "Laboratory exposures to brucellae and implications for bioterrorism". Emerging Infectious Diseases. 11 (8): 1180–5. doi:10.3201/eid1108.041197. PMC 3320509. PMID 16102304.
- ^ Centers for Disease Control Prevention (CDC) (January 2008). "Laboratory-acquired brucellosis--Indiana and Minnesota, 2006". MMWR. Morbidity and Mortality Weekly Report. 57 (2): 39–42. PMID 18199967.
- ^ Samartino LE (December 2002). "Brucellosis in Argentina". Veterinary Microbiology. 90 (1–4): 71–80. doi:10.1016/s0378-1135(02)00247-x. PMID 12414136.
- ^ "Brucelosis Bovina". SENASA - Argentine Government. 2022. Archived from the original on 2016-02-16.
- ^ "Queensland Health: Brucellosis". State of Queensland (Queensland Health). 2010-11-24. Archived from the original on 2011-04-22. Retrieved 2011-06-06.
- ^ Lehane, Robert (1996) Beating the Odds in a Big Country: The eradication of bovine brucellosis and tuberculosis in Australia, CSIRO Publishing, ISBN 0-643-05814-1
- ^ "Reportable Diseases". Accredited Veterinarian's Manual. Canadian Food Inspection Agency. Archived from the original on 2007-02-08. Retrieved 2007-03-18.
- ^ China reports outbreak of brucellosis disease 'way larger' than originally thought 18 September 2020 www.news.com.au, accessed 18 September 2020
- ^ "兰州药厂泄漏事件布病患者:肿痛无药可吃,有人已转成慢性病_绿政公署_澎湃新闻-The Paper". www.thepaper.cn. Retrieved 2 June 2021.
- ^ Pappas G (15 November 2022). "The Lanzhou Brucella Leak: The Largest Laboratory Accident in the History of Infectious Diseases?". Clinical Infectious Diseases. 75 (10): 1845–1847. doi:10.1093/cid/ciac463. PMID 35675697.
- ^ Warwick J, Willman D (April 12, 2023). "China's struggles with lab safety carry danger of another pandemic". The Washington Post. Washington D.C.
- ^ Naudi JR (2005). Brucellosis, The Malta Experience. Malta: Publishers Enterprises group (PEG) Ltd. ISBN 978-99909-0-425-3.
- ^ a b c "Ireland free of brucellosis". RTÉ. 2009-07-01. Retrieved 2009-07-01.
- ^ a b c d "Ireland declared free of brucellosis". The Irish Times. 2009-07-01. Archived from the original on 2021-04-03. Retrieved 2009-07-01.
Michael F Sexton, president of Veterinary Ireland, which represents vets in practice, said: "Many vets and farmers in particular suffered significantly with brucellosis in past decades and it is greatly welcomed by the veterinary profession that this debilitating disease is no longer the hazard that it once was."
- ^ a b c Monitoring brucellosis in Great Britain 3 September 2020 veterinary-practice.com, accessed 18 September 2020
- ^ Guidance Brucellosis: how to spot and report the disease 18 October 2018 www.gov.uk, accessed 18 September 2020
- ^ "MAF Biosecurity New Zealand: Brucellosis". Ministry of Agriculture and Forestry of New Zealand. Archived from the original on 2012-03-20. Retrieved 2011-06-06.
- ^ Brucellosis Eradication APHIS 91–45–013. United States Department of Agriculture. October 2003. p. 14.
- ^ Hamilton AV, Hardy AV (March 1950). "The brucella ring test; its potential value in the control of brucellosis". American Journal of Public Health and the Nation's Health. 40 (3): 321–3. doi:10.2105/AJPH.40.3.321. PMC 1528431. PMID 15405523.
- ^ Vermont Beef Producers. "How important is calfhood vaccination?" (PDF). Archived from the original (PDF) on 2008-05-09.
- ^ Meagher M, Meyer ME (September 1994). "On the Origin of Brucellosis in Bison of Yellowstone National Park: A Review" (PDF). Conservation Biology. 8 (3): 645–653. Bibcode:1994ConBi...8..645M. doi:10.1046/j.1523-1739.1994.08030645.x. JSTOR 2386505. Archived from the original (PDF) on 2017-01-08. Retrieved 2017-01-07.
- ^ Wilkinson L (1993). "Brucellosis". In Kiple KF (ed.). The Cambridge World History of Human Disease. Cambridge University Press.
- ^ Brucellosis named after Major-General Sir David Bruce at Whonamedit?
- ^ Evans A (1963). Dr. Alice C. Evans Memoir. Archived from the original on May 10, 2020.
- ^ Wyatt HV (2015). "The Strange Case of Temi Zammit's missing experiments" (PDF). Journal of Maltese History. 4 (2). Malta: Department of History, University of Malta: 54–56. ISSN 2077-4338. Archived from the original (PDF) on 2016-07-21. Journal archive
- ^ a b c d e f g de Kruif P (1932). "Ch. 5 Evans: death in milk". Men Against Death. New York: Harcourt, Brace. OCLC 11210642.
- ^ a b Wyatt HV (31 July 2004). "Give A Disease A Bad Name". British Medical Journal. 329 (7460). BMJ Publishing Group Ltd.: 272–278. doi:10.1136/bmj.329.7460.272. ISSN 0959-535X. JSTOR 25468794. OCLC 198096808. PMC 498028.
- ^ Madkour MM (2014). Brucellosis. Elsevier Science. p. 160. ISBN 978-1-4831-9359-5.
- ^ Malhotra R (2004). "Saudi Arabia". Practical Neurology. 4 (3): 184–185. doi:10.1111/j.1474-7766.2004.03-225.x.
- ^ Al-Sous MW, Bohlega S, Al-Kawi MZ, Alwatban J, McLean DR (March 2004). "Neurobrucellosis: clinical and neuroimaging correlation". AJNR. American Journal of Neuroradiology. 25 (3): 395–401. PMC 8158553. PMID 15037461.
- ^ "Medicine: Goat Fever". Time. 1928-12-10. ISSN 0040-781X. Retrieved 2017-05-01.
- ^ Woods JB (April 2005). USAMRIID's Medical Management of Biological Casualties Handbook (PDF) (6th ed.). Fort Detrick, Maryland: U.S. Army Medical Institute of Infectious Diseases. p. 53. Archived from the original (PDF) on 2007-06-09.
- ^ Radostits, O.M., C.C. Gay, D.C. Blood, and K.W. Hinchcliff. (2000). Veterinary Medicine, A textbook of the Diseases of Cattle, Sheep, Pigs, Goats and Horses. Harcourt Publishers Limited, London, pp. 867–882. ISBN 0702027774.
- ^ Ettinger SJ, Feldman EC (1995). Textbook of Veterinary Internal Medicine (4th ed.). W.B. Saunders Company. ISBN 978-0-7216-4679-4.
- ^ Guzmán-Verri C, González-Barrientos R, Hernández-Mora G, Morales JA, Baquero-Calvo E, Chaves-Olarte E, Moreno E (2012). "Brucella ceti and brucellosis in cetaceans". Frontiers in Cellular and Infection Microbiology. 2: 3. doi:10.3389/fcimb.2012.00003. PMC 3417395. PMID 22919595.
- ^ a b c "Brucellosis". www.fws.gov. U.S. Fish &Wildlife Service. 2016. Archived from the original on 2016-10-09. Retrieved 2016-10-03.
- ^ Godfroid J (August 2002). "Brucellosis in wildlife" (PDF). Revue Scientifique et Technique. 21 (2): 277–86. doi:10.20506/rst.21.2.1333. PMID 11974615. Archived from the original (PDF) on 2015-06-06. Retrieved 2016-10-07.
- ^ a b Godfroid J, Garin-Bastuji B, Saegerman C, Blasco JM (April 2013). "Brucellosis in terrestrial wildlife" (PDF). Revue Scientifique et Technique. 32 (1): 27–42. CiteSeerX 10.1.1.1020.9652. doi:10.20506/rst.32.1.2180. PMID 23837363. Archived from the original (PDF) on 2015-06-06. Retrieved 2016-10-07.
- ^ Cross PC, Maichak EJ, Brennan A, Scurlock BM, Henningsen J, Luikart G (April 2013). "An ecological perspective on Brucella abortus in the western United States" (PDF). Revue Scientifique et Technique. 32 (1): 79–87. doi:10.20506/rst.32.1.2184. PMID 23837367. Archived from the original (PDF) on April 16, 2016.
Further reading
[edit]- WHO fact sheet on brucellosis
- Brucella genomes and related information at PATRIC, a Bioinformatics Resource Center funded by NIAID
- Prevention about Brucellosis from Centers for Disease Control
- Capasso L (August 2002). "Bacteria in two-millennia-old cheese, and related epizoonoses in Roman populations". The Journal of Infection. 45 (2): 122–7. doi:10.1053/jinf.2002.0996. PMID 12217720. – re high rate of brucellosis in humans in ancient Pompeii
- Brucellosis, factsheet from European Centre for Disease Prevention and Control
Brucellosis
View on GrokipediaPathophysiology
Causative Agents and Species
Brucellosis is an infectious disease caused by facultative intracellular, Gram-negative coccobacilli of the genus Brucella, which are non-motile, non-spore-forming, and capable of aerobic or microaerophilic growth.[2][8] These bacteria exhibit smooth lipopolysaccharide (S-LPS) in their outer membrane for most pathogenic species, conferring resistance to host defenses and contributing to chronic infection.[9] The genus comprises at least 12 recognized species, but human infections are predominantly attributable to four zoonotic species: Brucella melitensis, B. abortus, B. suis, and B. canis, with B. melitensis demonstrating the highest virulence and invasiveness in humans.[10][11] B. melitensis, biovars 1–3, primarily infects goats and sheep, causing the most severe human brucellosis cases, often through consumption of unpasteurized dairy products; it accounts for the majority of infections in endemic Mediterranean, Middle Eastern, and Central Asian regions.[1][10] B. abortus, biovars 1–6 and 9, is associated with cattle and typically results in milder human disease, though it remains a significant occupational hazard for veterinarians and farmers handling infected livestock.[3][8] B. suis biovars 1–5 affect swine and can cause more chronic, suppurative infections in humans, including localized abscesses, with biovar 2 also infecting reindeer and hares in Europe.[12] B. canis, linked to dogs, leads to infections that are harder to diagnose serologically due to cross-reactivity issues but generally cause acute febrile illness in exposed individuals, such as pet owners or laboratory workers.[10][8] Less commonly implicated species include B. ovis (sheep, primarily causing genital disease in rams with rare, mild human cases) and B. neotomae (desert wood rats, mainly experimental or opportunistic in humans), which lack the broad zoonotic potential of the primary pathogens due to lower invasiveness and host adaptation.[12][13] Emerging atypical Brucella, such as those from marine mammals (B. ceti, B. pinnipedialis), have been isolated in sporadic human cases, often linked to occupational exposure, but their role in routine brucellosis remains marginal.[11] All pathogenic species share genomic similarities, with over 90% sequence identity, enabling intracellular survival via mechanisms like type IV secretion systems, though species-specific virulence factors influence tissue tropism and clinical severity.[14]| Species | Primary Reservoir(s) | Human Virulence Characteristics | Common Biovars |
|---|---|---|---|
| B. melitensis | Goats, sheep | Most virulent; severe systemic disease | 1–3 |
| B. abortus | Cattle | Moderate; often milder febrile illness | 1–6, 9 |
| B. suis | Swine, reindeer | Chronic, suppurative; relapsing infections | 1–5 |
| B. canis | Dogs | Acute; diagnostic challenges due to serology | N/A |
| B. ovis | Sheep | Low; rare, mild cases | N/A |
| B. neotomae | Rodents | Minimal; opportunistic | N/A |
Transmission Routes and Reservoirs
Brucella species, the causative agents of brucellosis, are primarily maintained in animal reservoirs, with specific associations between bacterial species and host animals. Brucella melitensis, the most pathogenic to humans, is predominantly found in small ruminants such as goats and sheep.[15] Brucella abortus is chiefly associated with cattle, while Brucella suis infects pigs, feral swine, reindeer, and caribou; Brucella canis primarily affects dogs.[3] Wildlife species, including bison and elk, serve as reservoirs for B. abortus in regions like the Greater Yellowstone Ecosystem, complicating eradication efforts due to potential spillover to livestock.[16] Other animals, such as camels, moose, and marine mammals, can harbor Brucella but are less common reservoirs.[3] Transmission to humans is almost exclusively zoonotic, occurring through direct or indirect contact with infected animals or their products, rather than sustained human-to-human spread. The primary route involves ingestion of unpasteurized dairy products, such as milk and cheese from infected goats, sheep, or cattle, which contain high bacterial loads in mammary secretions.[10] Occupational exposure is common among veterinarians, farmers, slaughterhouse workers, and laboratory personnel, via cutaneous or mucosal contact with contaminated tissues, blood, placentas, aborted fetuses, or uterine fluids, where bacteria enter through breaks in the skin or conjunctiva.[17] Aerosol inhalation represents a less frequent but documented pathway, particularly in abattoirs or during laboratory manipulation of cultures, leading to pulmonary infection.[18] Human-to-human transmission is rare and typically limited to specific scenarios, including congenital infection via intrauterine exposure, vertical transmission through breastfeeding, or iatrogenic routes such as blood transfusions and organ transplants.[19] Sexual transmission has been reported anecdotally but lacks robust epidemiological support.[13] In animal populations, bacteria spread horizontally through ingestion of contaminated feed, water, or aborted materials, and vertically via semen during breeding or in utero to offspring, perpetuating reservoir status.[20] Eradication programs emphasize vaccination and culling in livestock to reduce environmental shedding, as Brucella survives in soil, water, and carcasses for weeks to months, facilitating indirect transmission.[17]Mechanisms of Infection and Persistence
Brucella species, facultative intracellular bacteria, primarily infect host cells via uptake by professional phagocytes such as macrophages and dendritic cells, often following entry through compromised mucosal surfaces or abraded skin.[21] Upon phagocytosis, the bacteria reside within an early phagosomal compartment and deploy virulence factors to inhibit maturation into a phagolysosome, thereby evading degradation by lysosomal enzymes and reactive oxygen species.[22] This inhibition involves lipopolysaccharide O-chain components and cyclic β-1,2-glucans, which disrupt endosomal trafficking regulators and prevent fusion with lysosomes.[23][24] Virulent strains like B. abortus further modulate the vacuole's membrane to acquire endoplasmic reticulum (ER)-derived markers, transitioning the phagosome into a replicative Brucella-containing vacuole (rBCV) within hours of entry.[25][21] Replication occurs predominantly in the rough ER, where Brucella exploits the host's nutrient-rich environment for binary fission, producing progeny that can egress via ER-derived vesicles or cell lysis, disseminating to distant sites like spleen, liver, and bone marrow.[21] The type IV secretion system (T4SS) plays a central role by injecting effector proteins into the host cytosol, altering signaling pathways to favor bacterial proliferation and suppress antimicrobial responses.[26] Proteins like Dps, a ferritin-like molecule, enhance survival by sequestering iron and mitigating oxidative stress within the rBCV.[27] Persistence arises from Brucella's stealth adaptations that dampen innate immunity, including blockade of neutrophil degranulation, natural killer cell activation, and excessive cytokine production, resulting in minimal acute inflammation despite systemic spread.[28][29] The pathogen manipulates host cell apoptosis—delaying it in macrophages to allow replication while inducing it in lymphocytes—and reprograms immunometabolism to sustain chronic intracellular niches, often forming granulomatous lesions in target organs.[30] Effectors from the T4SS further inhibit antigen presentation and T-cell priming, enabling indefinite residence without clearance, which underpins relapsing infections even post-antibiotics.[31][26] This evasion contrasts with attenuated strains, which fail to block phagolysosomal fusion and succumb to host defenses.[22]Clinical Manifestations
Acute Phase Symptoms
The acute phase of brucellosis typically follows an incubation period of 5 to 60 days, with a mean of about 2 weeks, though it can extend to several months depending on the bacterial dose and host factors.[2] [32] Onset may be abrupt, manifesting with chills, high fever, severe headache, and prostration, or insidious, beginning with low-grade fever, malaise, and fatigue that progressively worsen.[8] [2] Fever is the hallmark symptom, reported in 80-100% of cases, often exhibiting an undulating or intermittent pattern with spikes up to 40°C (104°F) followed by periods of remission, classically described as a "Mediterranean" or "Malta" fever lasting 1-2 weeks per cycle.[32] [2] Profuse night sweats, sometimes drenching, accompany the fever in 70-90% of patients and contribute to significant dehydration and weight loss.[32] [1] Generalized malaise, profound fatigue, asthenia, and anorexia are nearly universal, affecting over 90% of individuals and often leading to rapid weight loss of 10-20 kg in untreated cases.[2] [32] Musculoskeletal complaints predominate, with arthralgia (50-80%) and myalgia (20-50%) commonly migratory and involving large joints like the knees, hips, and sacroiliac area, as well as low back pain mimicking sciatica.[33] [2] Headache occurs in 50-70% of patients, ranging from mild to severe and occasionally associated with photophobia or meningism.[32] Gastrointestinal symptoms such as nausea, vomiting, constipation, or diarrhea affect 10-30%, while respiratory involvement like nonproductive cough is less frequent (10-20%).[2] Physical examination in the acute phase may reveal relative bradycardia disproportionate to the fever, mild hepatosplenomegaly in 20-30% of cases, and peripheral lymphadenopathy in 10-20%, though orchitis or epididymitis can occur in 2-40% of male patients as a focal manifestation.[32] [8] These symptoms overlap with influenza, typhoid, or other systemic infections, complicating early recognition without exposure history.[3] [1]Chronic Forms and Complications
Chronic brucellosis is defined as persistence of symptoms beyond one year following initial infection, often due to inadequate treatment or diagnostic delay, affecting 10-30% of cases despite early intervention.[34] Patients may present with either focal complications evidencing active infection or nonspecific persistent symptoms without detectable pathogens, complicating diagnosis and management.[35] Common nonspecific manifestations include chronic fatigue, arthralgia, low-grade fever, depression, and musculoskeletal pain, reported in 62-75% of chronic cases.[36] Osteoarticular involvement represents the predominant focal complication in chronic brucellosis, occurring in 20-60% of patients and manifesting as spondylitis, sacroiliitis, peripheral arthritis, or osteomyelitis.[32] Spondylitis, particularly affecting the lumbar spine, can lead to vertebral destruction and neurological deficits if untreated, with sacroiliitis being the most frequent initial site.[37] These lesions arise from bacterial persistence within bone marrow, causing granulomatous inflammation and erosion, often requiring prolonged antimicrobial therapy combined with surgical debridement in severe cases.[38] Neurobrucellosis, a rarer chronic sequela affecting 1-4% of cases, involves central or peripheral nervous system invasion, presenting as meningitis, encephalitis, radiculopathy, or peripheral neuritis with symptoms including headache, seizures, hearing loss, and paresis.[39] Cerebrospinal fluid analysis typically reveals lymphocytic pleocytosis and elevated protein, with Brucella DNA detectable via PCR in persistent infections.[40] Cardiovascular complications, though infrequent (1-2% incidence), pose the highest mortality risk in chronic brucellosis, primarily through endocarditis affecting native or prosthetic valves, leading to valvular destruction, heart failure, or embolization.[38] Brucella's intracellular tropism facilitates biofilm formation on endothelium, exacerbating vegetations and necessitating combined medical-surgical interventions.[41] Other focal sites include genitourinary (e.g., orchitis, epididymitis in 2-40% of males) and hepatic involvement, with abscesses or chronic hepatitis contributing to long-term organ dysfunction.[42] Relapse rates in chronic forms exceed 14%, often linked to incomplete eradication and focal persistence.[43]Diagnostic Methods
Clinical Assessment
Clinical assessment of brucellosis relies on recognizing nonspecific symptoms, epidemiological risk factors, and physical findings suggestive of systemic infection, often in the context of potential zoonotic exposure. Patients typically present with an incubation period of 5 to 60 days, though it can extend to several months, following contact with infected animals or consumption of contaminated products.[2] Suspicion arises in individuals with occupational exposure, such as veterinarians, farmers, slaughterhouse workers, or laboratory personnel handling Brucella species, or those in endemic regions consuming unpasteurized dairy from goats, sheep, cattle, or camels.[33] In nonendemic areas, it frequently manifests as fever of unknown origin (FUO), with chills reported in nearly 80% of cases.[32] The hallmark symptoms include undulant or cyclical fever, profuse night sweats, profound fatigue, malaise, and anorexia leading to weight loss.[2] Arthralgia and myalgia, often migratory and affecting the sacroiliac joints, spine, or large joints, occur in up to 70-90% of patients, while headache and back pain are common.[44] Gastrointestinal complaints such as nausea, vomiting, or abdominal pain may accompany hepatosplenomegaly, and neuropsychiatric features like depression or insomnia can emerge.[1] In men, orchitis or epididymitis affects about 2-40% of cases, and women may experience endometritis.[2] These flu-like symptoms are insidious and intermittent, mimicking influenza, typhoid fever, or malaria, which underscores the need for detailed travel and dietary history to guide suspicion.[35] Physical examination may reveal relative bradycardia, lymphadenopathy (cervical or inguinal), or organomegaly, though findings are often unremarkable in early stages.[32] Osteoarticular involvement, the most frequent complication assessed clinically, presents as spondylitis or arthritis, detectable via localized tenderness or limited range of motion.[44] In chronic cases, persistent low-grade fever, fatigue, and localized pain predominate, with up to 30% of untreated patients developing relapses or focal disease like endocarditis or neurobrucellosis, identified through auscultatory murmurs or neurological deficits.[2] Assessment emphasizes ruling out differentials like tuberculosis or rheumatologic disorders, with clinical scoring systems sometimes used to stratify probability pending laboratory confirmation.[45]Laboratory Confirmation
Laboratory confirmation of brucellosis requires microbiological, serological, or molecular evidence, with isolation of Brucella species from clinical specimens serving as the definitive diagnostic criterion.[33] Blood cultures yield the organism in 40-70% of acute cases, though positivity decreases in chronic infections; bone marrow cultures achieve higher sensitivity, up to 90%, due to intracellular persistence of the bacteria.[46] Specimens such as cerebrospinal fluid, synovial fluid, or tissues from affected organs may also be cultured on selective media like Farrell or Castaneda under 5-10% CO2 incubation for up to 21-42 days, as Brucella grows slowly and requires biosafety level 3 precautions to mitigate aerosol transmission risks.[47] [48] Serological tests detect anti-Brucella antibodies and are widely used for presumptive diagnosis, particularly in resource-limited settings, but must be interpreted cautiously due to potential cross-reactivity with pathogens like Yersinia enterocolitica or persistent titers post-treatment.[46] The standard tube agglutination test (SAT) or microagglutination test (MAT) with titers ≥1:160 supports presumptive evidence per CDC criteria, often confirmed by a fourfold rise between acute and convalescent sera collected 2-4 weeks apart.[49] Screening assays like the Rose Bengal plate test offer rapid results with high sensitivity (up to 99%) but lower specificity, necessitating confirmatory tests such as 2-mercaptoethanol (2-ME) to differentiate IgM from IgG or Coombs antiglobulin tests for prozone phenomena in high-titer cases.[50] [51] Enzyme-linked immunosorbent assay (ELISA) provides quantitative IgG/IgM detection with sensitivities exceeding 90% in acute brucellosis, though specificity varies (80-95%) and requires species-specific antigens for accuracy.[52] Molecular methods, including polymerase chain reaction (PCR), enable rapid detection of Brucella DNA in blood or tissues, bypassing culture delays and biosafety concerns, with real-time PCR assays achieving sensitivities of 80-100% in early infection when bacterial loads are highest.[53] Genus- or species-specific PCR targets like bcsp31 or IS711 genes confirm infection presumptively, as endorsed by CDC, outperforming culture in treated patients or focal complications; multiplex formats distinguish Brucella spp. but may detect non-viable DNA, necessitating correlation with clinical findings.[54] [55] Combined approaches—serology for screening, culture or PCR for confirmation—optimize diagnostic yield, as no single test exceeds 100% sensitivity across disease phases.[56]Treatment Approaches
Antibiotic Regimens
The treatment of brucellosis requires prolonged combination antibiotic therapy, typically lasting at least six weeks, to eradicate the intracellular persistence of Brucella species and minimize relapse rates, which can reach 5-15% even with optimal regimens.[2] [57] Monotherapy is ineffective due to the bacterium's ability to survive within host cells, necessitating drugs with good intracellular penetration such as tetracyclines and rifamycins.[6] Guidelines from the World Health Organization (WHO) and Centers for Disease Control and Prevention (CDC) emphasize dual therapy for uncomplicated cases in adults, with adjustments for children, pregnant individuals, or complications like neurobrucellosis.[1] [58] The standard oral regimen for adults and children over eight years consists of doxycycline at 100 mg twice daily combined with rifampin at 600-900 mg once daily, administered for six weeks; this WHO-recommended approach balances efficacy with tolerability, though rifampin monotherapy relapse rates exceed 20%.[1] [6] [59] An alternative, often considered the historical gold standard, pairs doxycycline (100 mg twice daily for six weeks) with streptomycin (1 g intramuscularly daily for the first two to three weeks), which achieves lower relapse rates in some osteoarticular cases but requires parenteral administration and monitoring for ototoxicity.[57] [2] Gentamicin (5 mg/kg daily for seven days) may substitute for streptomycin in outpatient settings, offering comparable efficacy with reduced nephrotoxicity risk.[60] [61] For special populations, trimethoprim-sulfamethoxazole (TMP-SMZ; 160/800 mg twice daily for six weeks) plus rifampin serves as an option in children under eight or pregnant women, avoiding tetracyclines' teratogenic effects, though evidence shows higher relapse rates compared to doxycycline-based regimens.[1] [58] Triple therapy, such as doxycycline plus streptomycin and rifampin, has demonstrated superior bacterial clearance and reduced relapses in meta-analyses of randomized trials (odds ratio for relapse 0.48 versus dual therapy), but it increases adverse events like gastrointestinal upset and hepatotoxicity without universal endorsement due to cost and complexity.[62] [63] [60] Consultation with infectious disease specialists is advised for tailoring therapy, particularly in endemic regions where resistance patterns—though rare—may influence choices.| Regimen Type | Primary Drugs and Doses | Duration | Indications and Considerations |
|---|---|---|---|
| Dual Oral (WHO/CDC Standard) | Doxycycline 100 mg BID + Rifampin 600-900 mg QD | 6 weeks | Uncomplicated adult cases; avoids injections but higher relapse in some studies.[1] [58] |
| Dual Parenteral-Assisted | Doxycycline 100 mg BID + Streptomycin 1 g IM QD (first 2-3 weeks) | 6 weeks total | Preferred for severe or osteoarticular disease; monitor for vestibular toxicity.[57] [6] |
| Alternative Dual | Doxycycline 100 mg BID + Gentamicin 5 mg/kg QD | Doxycycline 6 weeks; Gentamicin 7 days | Shorter aminoglycoside course; suitable for outpatient management.[60] |
| Pediatric/Pregnancy | TMP-SMZ 160/800 mg BID + Rifampin 15-20 mg/kg QD | 6 weeks | Tetracycline contraindicated; increased relapse risk observed.[1] |
| Triple (Investigational/Select Cases) | Doxycycline + Streptomycin + Rifampin | 6 weeks | Lower relapse in trials but more side effects; not first-line.[63] [62] |
Management of Relapses and Complications
Relapses in brucellosis occur in 5% to 15% of treated cases, attributable to factors such as inadequate antibiotic penetration into intracellular reservoirs, insufficient treatment duration, poor patient adherence, or initial use of monotherapy.[64][63] Management of relapse requires prompt reinitiation of combination antibiotic therapy, mirroring acute treatment protocols but often extended to 8 weeks or more, with regimens favoring doxycycline (100 mg twice daily) combined with rifampin (600-900 mg daily) and an aminoglycoside like streptomycin (15 mg/kg daily for the first 2-3 weeks) to enhance efficacy against persistent bacteria.[6][65] Clinical monitoring includes serial serologic testing and imaging if focal symptoms recur, with relapse defined by return of fever, positive blood cultures, or rising antibody titers post-treatment.[66] Complications such as osteoarticular involvement (e.g., spondylitis or sacroiliitis in up to 30% of cases), neurobrucellosis, or endocarditis necessitate tailored interventions beyond standard antimicrobials. For osteoarticular complications, antibiotics are prolonged (up to 3 months), supplemented by analgesics, nonsteroidal anti-inflammatory drugs, and immobilization or physical therapy to alleviate pain and prevent deformity, with surgical drainage reserved for abscesses unresponsive to medical therapy.[2] Neurobrucellosis, including meningitis, demands high-dose intravenous antibiotics like ceftriaxone or trimethoprim-sulfamethoxazole for 4-6 months, alongside corticosteroids for severe inflammation, achieving cure rates above 80% with early intervention.[67] Endocarditis, a rare but fatal complication (mortality up to 1-2% overall), typically requires surgical valve replacement combined with triple antibiotic therapy (e.g., doxycycline, rifampin, gentamicin) for at least 6 weeks postoperatively to address valvular destruction and embolic risks.[6][68] In refractory cases or chronic brucellosis with multiple relapses, triple therapy with rifampin, doxycycline, and streptomycin is preferred, yielding relapse rates under 5% in systematic reviews, though patient factors like immunosuppression or delayed diagnosis elevate risks.[69][70] Adjunctive measures include supportive care for symptoms (e.g., fever control with antipyretics) and exclusion of ongoing zoonotic exposure to prevent reinfection, as relapses mimic primary illness but may involve higher complication rates if untreated.[71] Overall, vigilant follow-up for 1-2 years post-treatment is essential, as late relapses can emerge due to bacterial latency.[72]Prognosis
Factors Influencing Outcomes
The prognosis of human brucellosis is generally excellent with prompt antibiotic therapy, yielding cure rates above 90% in uncomplicated acute cases, though relapse occurs in 5-15% of treated patients and chronic forms can persist without full resolution.[2] Delayed diagnosis, often exceeding 30 days from symptom onset, heightens the likelihood of progression to focal complications such as spondylitis or endocarditis, which correlate with treatment failure rates up to 20-30% higher than in non-focal disease.[73] [74] Host factors play a pivotal role; advanced age (≥45 years) independently predicts adverse outcomes, including prolonged hospitalization and higher complication rates, attributable to diminished immune competence and increased prevalence of comorbidities like diabetes or renal impairment.[75] [76] Comorbidities, particularly cardiovascular or pulmonary disorders, exacerbate disability risks, with elevated serum creatinine levels signaling renal involvement that worsens overall recovery.[2] [76] In pregnant individuals, infection elevates miscarriage risk by 20-30%, alongside preterm labor, due to placental tropism of Brucella species.[77] Disease-specific determinants include chronicity (symptoms >6 weeks), focal organ involvement (e.g., osteoarticular in 10-30% of cases), and hypoalbuminemia (<3.5 g/dL), all of which independently forecast treatment non-response and relapse, with multivariate analyses confirming odds ratios of 2-5 for failure in such scenarios.[74] [35] Virulence variations among species—B. melitensis causing more severe systemic illness than B. suis—further modulate severity, as do initial fever ≥38.3°C and arthralgia, which predict relapse in up to 25% of regimens under 6 weeks.[35] [78] Treatment adherence and regimen duration (minimum 6 weeks dual therapy) mitigate these risks, but incomplete courses double relapse incidence.[2]Long-Term Health Impacts
Chronic brucellosis, defined as persistent symptoms lasting more than one year following acute infection, affects a minority of patients and is characterized by recurrent fevers, fatigue, arthralgia, myalgia, depression, and malaise.[79] These symptoms can endure for years despite treatment, with Brucella DNA detectable in some cases, suggesting bacterial persistence as a contributing factor.[80] Relapse occurs in approximately 10% of cases, predominantly within the first year post-treatment, but reactivation has been documented up to 28 years later.[81] Osteoarticular complications represent the most prevalent long-term sequelae, occurring in 10% to 85% of chronic cases and including spondylodiscitis, peripheral arthritis, sacroiliitis, and osteomyelitis, which may lead to chronic pain, deformity, and impaired mobility.[82] These manifestations arise from granulomatous inflammation and bone erosion, often requiring prolonged antibiotic therapy and surgical intervention in refractory instances.[44] Cardiovascular involvement, particularly endocarditis, emerges as a severe long-term risk, constituting the primary cause of mortality in brucellosis with fatality rates up to 8% in followed cohorts; it manifests as valvular destruction and heart failure, necessitating valve replacement in advanced stages.[83] Neurobrucellosis and genitourinary sequelae, such as chronic epididymo-orchitis or prostatitis, contribute to persistent neurological deficits like peripheral neuritis or cognitive impairment, alongside reproductive dysfunction including infertility.[38] Hepatic and splenic abscesses may persist as chronic suppurative foci, exacerbating systemic inflammation.[84] Overall prognosis for long-term survival remains favorable, with mortality below 2%, though untreated or relapsed chronic disease impairs quality of life through enduring fatigue, emotional lability, and organ-specific morbidity.[33] Early diagnosis and extended antimicrobial regimens mitigate but do not eliminate risks of these sequelae.[36]Prevention and Control
Strategies in Animal Husbandry
Control of brucellosis in livestock relies on integrated strategies emphasizing vaccination, surveillance, and biosecurity to interrupt transmission cycles, as the bacterium persists in reproductive tissues and aborted materials of infected animals.[85] In cattle, the primary hosts, calfhood vaccination with Brucella abortus strain 19 (S19) reduces abortion rates and shedding by over 90% in vaccinated herds when administered between 4-12 months of age, though it does not confer complete immunity and requires serological monitoring to distinguish vaccinated from infected animals.[86] Strain RB51, a rough mutant, is used for adult cattle vaccination in the United States under permit, offering similar protective efficacy against clinical disease but with lower interference in diagnostic tests.[86] For small ruminants like sheep and goats, Rev-1 vaccine against B. melitensis has demonstrated sustained reductions in herd prevalence, with Greece reporting a drop in human cases following 15 years of mass vaccination.[87] Test-and-slaughter programs, involving serological screening (e.g., Rose Bengal or ELISA) followed by depopulation of reactors, have eradicated brucellosis from high-income countries with low initial prevalence, such as the European Union by 2009, but prove less effective and costlier in endemic settings without vaccination support.[85] Economic analyses indicate test-and-slaughter alone yields negative returns in regions like Armenia due to high surveillance costs and incomplete compliance, whereas combining it with vaccination enhances cost-effectiveness by limiting new infections.[88] Quarantine of infected herds and restrictions on animal movement, enforced via national identification systems, further prevent interstate or international spread, as seen in U.S. state-federal cooperative programs requiring negative tests for interstate transport.[89] Husbandry practices mitigate zoonotic risk through sanitation, such as prompt removal and incineration of aborted fetuses, placentas, and uterine fluids—primary sources of environmental contamination—and segregation of pregnant animals to dedicated calving areas.[90] Biosecurity protocols, including disinfection of equipment and avoidance of commingling at markets, reduce indirect transmission, particularly in extensive grazing systems where wildlife reservoirs like bison can reintroduce the pathogen.[89] No viable treatment exists for infected livestock due to persistent bacteremia, underscoring prevention over cure; integrated programs incorporating these elements have lowered bovine prevalence below 1% in vaccinated U.S. herds since the 1950s.[86][85]Human and Occupational Precautions
For the general population, primary precautions against brucellosis involve avoiding ingestion of unpasteurized milk, cheese, or other dairy products from potentially infected animals such as goats, sheep, cattle, or camels, as pasteurization effectively eliminates the bacteria.[3] [1] Consumption of undercooked meat from these species should also be avoided, with thorough cooking recommended to inactivate Brucella organisms.[3] Individuals in high-risk occupations, including livestock farmers, veterinarians, slaughterhouse and abattoir workers, and hunters, face elevated exposure risks through direct contact with infected animal tissues, blood, uterine secretions, aborted fetuses, or placentas.[91] [1] Essential protective measures include wearing personal protective equipment (PPE) such as rubber gloves, goggles or face shields, masks or respirators, impermeable aprons or gowns, and boots during handling of animals or their products to prevent percutaneous, mucosal, or inhalation exposure.[3] [91] Strict hygiene practices, including immediate handwashing with soap after contact, disinfection of equipment, and covering any skin breaks, further mitigate transmission risks.[1] [91] Laboratory personnel handling Brucella cultures or suspect specimens require biosafety level 3 (BSL-3) practices, including manipulation within certified biosafety cabinets to contain aerosols, alongside full PPE ensembles.[47] Following high-risk exposures—such as needlestick injuries, mucosal splashes, or inhalation without protection—workers should initiate post-exposure prophylaxis (PEP) promptly, typically with doxycycline (100 mg twice daily) plus rifampin (600 mg once daily) for at least 21 days, adjustable for strain-specific resistance like rifampin-resistant B. abortus RB51.[47] Exposed individuals undergo symptom monitoring, including daily temperature checks for 24 weeks and weekly clinical evaluations, with serological testing at baseline and intervals up to 24 weeks to detect seroconversion.[47] Occupational health programs emphasizing training on these protocols have demonstrated effectiveness in reducing incident rates among at-risk groups.[91]Vaccine Development Challenges
Development of a safe and effective human vaccine against brucellosis has proven elusive, with no licensed product available as of 2024, despite decades of research. Existing veterinary vaccines, such as the live attenuated strains S19 for cattle and Rev-1 for sheep and goats, induce protection in animals but pose significant risks to humans, including potential infection via aerosol or mucosal exposure during production or administration. These strains retain residual virulence, leading to cases of human brucellosis among veterinarians and laboratory workers, which underscores their unsuitability for human use.[92][93] A primary obstacle stems from Brucella's biology as a facultative intracellular pathogen that evades host defenses by surviving within macrophages and dendritic cells, necessitating vaccines that elicit robust cell-mediated immunity—particularly Th1 responses with interferon-gamma production—rather than solely humoral antibodies. Subunit vaccines targeting outer membrane proteins or lipoproteins often fail to generate sufficient T-cell activation, resulting in inadequate protection in preclinical models like mice, which imperfectly mimic human disease dynamics. Live attenuated candidates risk uncontrolled replication and persistence, mirroring the pathogen's natural tropism for lymphoid tissues, while inactivated or killed vaccines historically underperform due to poor induction of mucosal and cellular immunity at entry sites like the oropharynx or conjunctiva.[94][87][95] Safety-efficacy trade-offs further complicate progress, as attenuation strategies that reduce virulence in animals may not translate predictably to humans, potentially causing abortion in pregnant individuals or disease in the immunocompromised—a critical concern given brucellosis's zoonotic nature and occupational risks in endemic regions. Many candidates also interfere with serological diagnostics by inducing antibodies that confound surveillance, a persistent issue with smooth-lipopolysaccharide-containing strains like S19 and Rev-1. Novel approaches, including DNA vaccines, viral vectors, and multi-epitope constructs, face immunogenicity hurdles such as antigen instability, short half-lives, and the need for potent adjuvants, often requiring multiple doses without guaranteed long-term efficacy.[96][97][98] Regulatory and practical barriers exacerbate these biological challenges, including the absence of standardized correlates of protection, ethical constraints on human trials in high-prevalence areas, and limited funding incentives due to brucellosis's neglect in global health priorities. Animal models, while useful, overestimate protection against diverse Brucella species (B. melitensis, B. abortus, B. suis), and field trials demand large cohorts in resource-poor settings where compliance and monitoring are difficult. Efforts like the AgResults Brucellosis Vaccine Challenge Project aim to incentivize improved livestock vaccines with human applicability, but human-specific mucosal or prime-boost strategies remain preclinical, with no phase III data reported.[99][100][101]Epidemiology
Global Incidence and Trends
Brucellosis imposes a substantial global health burden, with recent modeling estimates indicating 1.6 to 2.1 million new human cases annually, a figure significantly higher than prior assumptions due to underreporting in endemic areas.[5] [35] This conservative projection derives from integrating human surveillance data with animal prevalence metrics, accounting for at-risk populations in livestock-dependent regions.[102] The disease affects all age groups and both sexes, transmitted primarily through unpasteurized dairy consumption or contact with infected animals, and remains reportable in most countries, though incomplete notifications—such as only 48.4% of required reports to the World Organisation for Animal Health by 2019—obscure true scale.[1] [103] Endemicity persists in the Mediterranean Basin, Middle East, sub-Saharan Africa, Central Asia, and parts of Latin America, where annual incidence can exceed 20 per 100,000 in pastoral communities, contrasting with near-elimination in high-income regions through pasteurization and vaccination.[1] [35] In the European Union and European Economic Area, the notification rate stood at 0.04 cases per 100,000 population in 2022, reflecting effective controls but underscoring zoonotic importation risks.[104] Globally, approximately 3.5 billion people face exposure risk, amplified by informal animal husbandry and trade.[105] Trends show no uniform decline; while veterinary interventions have curbed outbreaks in select areas, resource-limited settings report stable or rising cases amid diagnostic gaps and misattribution to similar febrile illnesses like malaria.[106] Surveillance deficiencies, including serological under-detection and variable reporting standards, hinder precise trend analysis, with evidence suggesting the true incidence may exceed modeled estimates in high-burden zones.[103] Recent data from 2020 onward indicate persistence rather than reduction, driven by livestock mobility and climate-influenced vector dynamics in endemic foci.[107]Regional and Country-Specific Patterns
Brucellosis remains highly endemic in the Middle East and Mediterranean Basin, where annual incidence rates often exceed 20 cases per 100,000 population in countries such as Syria, Iraq, and Turkey, driven by consumption of unpasteurized dairy products and close contact with infected livestock like goats and sheep.[108] In Syria, the disease reports some of the world's highest per capita incidences, attributed to ongoing conflict disrupting veterinary controls and pastoralist practices.[109] Neighboring regions in West Asia, including Iran and Saudi Arabia, show similar patterns, with Brucella melitensis predominating due to small ruminant husbandry.[110] In sub-Saharan Africa and North Africa, prevalence is widespread but underreported, with pooled livestock seroprevalence around 8-12% in affected areas, correlating to human cases from zoonotic transmission in nomadic herding communities.[111] Endemic hotspots include East Africa (e.g., Tanzania, Ethiopia) and the Sahel region, where annual human incidences can reach 5-10 per 100,000, exacerbated by limited diagnostic capacity and misdiagnosis as malaria.[35][5] Asia exhibits high burden in Central and West Asia, with countries like Tajikistan ranking among the top 25 globally for incidence; in one 2023 outbreak, rates hit 32.7 per 100,000 by mid-year in remote villages due to raw milk consumption.[112] China reports a national average of 3.0 cases per 100,000 annually from 2010-2019 data, with hotspots in northern pastoral provinces, though divergent trends show declines in some areas via vaccination but rises in others from wildlife interfaces.[35] India and Mongolia also sustain elevated rates linked to dairy farming.[113] Latin America shows variable endemicity, with Central America facing the highest risks (e.g., Mexico, Guatemala) from cattle and small ruminant reservoirs, followed by Andean countries like Peru and Bolivia where incidences surpass 10 per 100,000 in rural zones.[5] Southern cone nations such as Argentina and Brazil report sporadic outbreaks, often tied to imported strains or uncontrolled livestock movement.[108] In Europe, incidence is low (typically <0.1 per 100,000), largely confined to southern and eastern countries with outbreaks from imported cheeses or Balkan endemic foci; B. melitensis persists in pockets of Greece, Portugal, and the former Yugoslav states despite eradication programs.[5] Northern and Western Europe report mostly travel-related or laboratory-acquired cases. North America maintains near-elimination through rigorous animal surveillance, with rare U.S. incidents (<100 annually) often occupational among veterinarians or linked to Mexican imports.[10] Oceania remains brucellosis-free in humans due to stringent biosecurity.[108]| Region | Key Endemic Countries | Estimated Incidence (per 100,000) | Primary Drivers |
|---|---|---|---|
| Middle East/Mediterranean | Syria, Iraq, Turkey | >20 | Unpasteurized dairy, conflict |
| Africa | Ethiopia, Tanzania | 5-10 | Herding, underdiagnosis |
| Asia | Tajikistan, China | 3-30+ (localized) | Pastoralism, outbreaks |
| Latin America | Mexico, Peru | >10 (rural) | Livestock contact |
| Europe/North America | Southern Europe, U.S. (rare) | <0.1 | Imported/occupational |
