Recent from talks
Nothing was collected or created yet.
Anatomical terminology
View on WikipediaThis article needs additional citations for verification. (April 2025) |
 |
| This article is part of a series on |
| Anatomical terminology |
|---|
Anatomical terminology is a specialized system of terms used by anatomists, zoologists, and health professionals, such as doctors, surgeons, and pharmacists, to describe the structures and functions of the body.[1]
This terminology incorporates a range of unique terms, prefixes, and suffixes derived primarily from Ancient Greek and Latin. While these terms can be challenging for those unfamiliar with them, they provide a level of precision that reduces ambiguity and minimizes the risk of errors. Because anatomical terminology is not commonly used in everyday language, its meanings are less likely to evolve or be misinterpreted.
For example, everyday language can lead to confusion in descriptions: the phrase "a scar above the wrist" could refer to a location several inches away from the hand, possibly on the forearm, or it could be at the base of the hand, either on the palm or dorsal (back) side. By using precise anatomical terms, such as "proximal," "distal," "palmar," or "dorsal," this ambiguity is eliminated, ensuring clear communication.[2]
To standardize this system of terminology, Terminologia Anatomica was established as an international reference for anatomical terms.[3]
Word formation
[edit]Anatomical terminology follows a regular morphology, with consistent prefixes and suffixes used to modify different roots. The root of a term often refers to an organ or tissue. For example, the Latin name musculus biceps brachii can be broken down: musculus meaning muscle, biceps meaning "two-headed", and brachii referring to the arm (brachial region). The first term identifies the structure, the second indicates the type or instance of the structure, and the third specifies its location.[4]
Anatomical structures are often described in relation to landmarks, such as the umbilicus, sternum, or anatomical lines like the midclavicular line (from the center of the clavicle). The term cephalon or cephalic region refers to the head, which is further divided into the cranium (skull), facies (face), frons (forehead), oculus (eye area), auris (ear), bucca (cheek), nasus (nose), os (mouth), and mentum (chin). The neck is known as the cervix or cervical region. Examples of structures named for these areas include the frontalis muscle, submental lymph nodes, buccal membrane and orbicularis oculi muscle.
To reduce confusion, some terms are used specifically for certain body regions. For instance, in the skull rostral refers to proximity to the front of the nose and is primarily used when describing the skull's position, especially in comparison to other animals.[5]: 4 Similarly, in the arms, different terms help clarify the "front", "back", "inner" and "outer" surfaces. For example:
- Radial referring to the radius bone, seen laterally in the standard anatomical position.
- Ulnar referring to the ulna bone, medially positioned when in the standard anatomical position.
Additional terminology is used to describe the movement and actions of the hands and feet, and other structures such as the eyes.
History
[edit]International morphological terminology is used by the colleges of medicine and dentistry and other areas of the health sciences. It facilitates communication and exchanges between scientists from different countries of the world and it is used daily in the fields of research, teaching and medical care. The international morphological terminology refers to morphological sciences as a biological sciences' branch. In this field, the form and structure are examined as well as the changes or developments in the organism. It is descriptive and functional. Basically, it covers the gross anatomy and the microscopic (histology and cytology) of living beings. It involves both development anatomy (embryology) and the anatomy of the adult. It also includes comparative anatomy between different species. The vocabulary is extensive, varied and complex, and requires a systematic presentation.
Within the international field, a group of experts reviews, analyzes and discusses the morphological terms of the structures of the human body, forming today's Terminology Committee (FICAT) from the International Federation of Associations of Anatomists (IFAA).[6][7] It deals with the anatomical, histological and embryologic terminology. In the Latin American field, there are meetings called Iberian Latin American Symposium Terminology (SILAT), where a group of experts of the Pan American Association of Anatomy (PAA)[8] that speak Spanish and Portuguese, disseminates and studies the international morphological terminology.
The current international standard for human anatomical terminology is based on the Terminologia Anatomica (TA). It was developed by the Federative Committee on Anatomical Terminology (FCAT) and the International Federation of Associations of Anatomists (IFAA) and was released in 1998.[9] It supersedes the previous standard, Nomina Anatomica.[10] Terminologia Anatomica contains terminology for about 7500 human gross (macroscopic) anatomical structures.[11] For microanatomy, known as histology, a similar standard exists in Terminologia Histologica, and for embryology, the study of development, a standard exists in Terminologia Embryologica. These standards specify generally accepted names that can be used to refer to histological and embryological structures in journal articles, textbooks, and other areas. As of September 2016, two sections of the Terminologia Anatomica, including central nervous system and peripheral nervous system, were merged to form the Terminologia Neuroanatomica.[12]
The Terminologia Anatomica has been perceived with considerable criticism regarding its content including coverage, grammar and spelling mistakes, inconsistencies, and errors.[13]
Location
[edit]Anatomical terminology is often chosen to highlight the relative location of body structures. For instance, an anatomist might describe one band of tissue as "inferior to" another or a physician might describe a tumor as "superficial to" a deeper body structure.[4]
Anatomical position
[edit]
Anatomical terms used to describe location are based on a body positioned in what is called the standard anatomical position. This position is one in which a person is standing, feet apace, with palms forward and thumbs facing outwards.[14] Just as maps are normally oriented with north at the top, the standard body "map", or anatomical position, is that of the body standing upright, with the feet at shoulder width and parallel, toes forward. The upper limbs are held out to each side, and the palms of the hands face forward.[4]
Using the standard anatomical position reduces confusion. It means that regardless of the position of a body, the position of structures within it can be described without ambiguity.[4]
Regions
[edit]
In terms of anatomy, anatomical lines are theoretical lines used to divide the body into regions, such as the nine regions of the abdomen. Axillary lines provide reference points for the underarm region
In the front, the trunk is referred to as the "thorax" and "abdomen". The back as a general area is the dorsum or dorsal area, and the lower back is the lumbus or lumbar region. The shoulder blades are the scapular area and the breastbone is the sternal region. The abdominal region is the area between the chest and the pelvis. The breast is also called the mammary region, the armpit as the axilla and axillary, and the navel as the umbilicus and umbilical. The pelvis is the lower torso, between the abdomen and the thighs. The groin, where the thigh joins the trunk, are the inguen and inguinal area.
The entire arm is referred to as the brachium and brachial, the front of the elbow as the antecubitis and antecubital, the back of the elbow as the olecranon or olecranal, the forearm as the antebrachium and antebrachial, the wrist as the carpus and carpal area, the hand as the manus and manual, the palm as the palma and palmar, the thumb as the pollex, and the fingers as the digits, phalanges, and phalangeal. The buttocks are the gluteus or gluteal region and the pubic area is the pubis.
Anatomists divide the lower limb into the thigh (the part of the limb between the hip and the knee) and the leg (which refers only to the area of the limb between the knee and the ankle).[14] The thigh is the femur and the femoral region. The kneecap is the patella and patellar while the back of the knee is the popliteus and popliteal area. The leg (between the knee and the ankle) is the crus and crural area, the lateral aspect of the leg is the peroneal area, and the calf is the sura and sural region. The ankle is the tarsus and tarsal, and the heel is the calcaneus or calcaneal. The foot is the pes and pedal region, and the sole of the foot is the planta and plantar. As with the fingers, the toes are also called the digits, phalanges, and phalangeal area. The big toe is referred to as the hallux.
Abdomen
[edit]
To promote clear communication, for instance about the location of a patient's abdominal pain or a suspicious mass, the abdominal cavity can be divided into either nine regions or four quadrants.[4]
Abdominal quadrants
[edit]The abdomen may be divided into four quadrants, more commonly used in medicine, subdivides the cavity with one horizontal and one vertical line that intersect at the patient's umbilicus (navel).[4] The right upper quadrant (RUQ) includes the lower right ribs, right side of the liver, and right side of the transverse colon. The left upper quadrant (LUQ) includes the lower left ribs, stomach, spleen, and upper left area of the transverse colon. The right lower quadrant (RLQ) includes the right half of the small intestines, ascending colon, right pelvic bone and upper right area of the bladder. The left lower quadrant (LLQ) contains the left half of the small intestine and left pelvic bone.[14]
Abdominal regions
[edit]The more detailed regional approach subdivides the cavity into nine regions, with two vertical and two horizontal anatomical lines drawn according to landmark structures. The vertical; or midclavicular lines, are drawn as if dropped from the midpoint of each clavicle. The superior horizontal line is the subcostal line, drawn immediately inferior to the ribs.[4] The inferior horizontal line is called the intertubercular line, and is to cross the iliac tubercles, found at the superior aspect of the pelvis.
The upper right square is the right hypochondriac region and contains the base of the right ribs. The upper left square is the left hypochondriac region and contains the base of the left ribs. The epigastric region is the upper central square and contains the bottom edge of the liver as well as the upper areas of the stomach. The diaphragm curves like an upside down U over these three regions.
The central right region is called the right lumbar region and contains the ascending colon and the right edge of the small intestines. The umbilical region is central square and contains the transverse colon and the upper regions of the small intestines. The left lumbar region contains the left edge of the transverse colon and the left edge of the small intestine.
The lower right square is the right iliac region and contains the right pelvic bones and the ascending colon. The lower left square is the left iliac region and contains the left pelvic bone and the lower left regions of the small intestine. The hypogastric region is the lower central square and contains the bottom of the pubic bones, upper regions of the bladder and the lower region of the small intestine.[14]
Standard terms
[edit]When anatomists refer to the right and left of the body, it is in reference to the right and left of the subject, not the right and left of the observer. When observing a body in the anatomical position, the left of the body is on the observer's right, and vice versa. These standardized terms avoid confusion. Examples of terms include:[5]: 4
- Anterior and posterior, which describe structures at the front (anterior) and back (posterior) of the body. For example, the toes are anterior to the heel, and the popliteus is posterior to the patella.[15]
- Superior and inferior, which describe a position above (superior) or below (inferior) another part of the body. For example, the orbits are superior to the oris, and the pelvis is inferior to the abdomen.[15]
- Proximal and distal, which describe a position that is closer to (proximal) or farther from (distal) the trunk of the body.[15] For example, the shoulder is proximal to the arm, and the foot is distal to the knee.
- Superficial and deep, which describe structures that are closer to (superficial) or farther from (deep) the surface of the body. For example, the skin is superficial to the bones, and the brain is deep to the skull.[15] Sometimes profound is used synonymously with deep.
- Medial and lateral, which describe a position that is closer to (medial) or farther from (lateral) the midline of the body. For example, the shoulders are lateral to the heart, and the umbilicus is medial to the hips. The medial side of the left knee is the side toward the opposite knee.
- Radial and ulnar, which describe only structures at or distal to the elbow and may be used interchangeably with medial and lateral in that particular area because they are less confusing. Examples: The thumb is on the radial side of the hand (the same as saying the lateral side); the ulnar side of the wrist is the side toward the little finger (medial side).
- Dorsal and ventral, which describe structures derived from the back (dorsal) or front (ventral) such as in the embryo, before limb rotation.
- Rostral and caudal, which describe structures close to (rostral) or farther from (caudal) the nose. For example, the eyes are rostral to the back of the skull, and the tailbone is caudal to the chest.
- Cranial and caudal, which describe structures close to the top of the skull (cranial), and towards the bottom of the body (caudal).
- Occasionally, sinister for left, and dexter for right are used.
- Paired, referring to a structure that is present on both sides of the body. For example, the hands are paired structures.
Axes
[edit]Each locational term above can define the direction of a vector, and pairs of them can define axes, that is, lines of orientation. For example, blood can be said to flow in a proximal or distal direction, and anteroposterior, mediolateral, and inferosuperior axes are lines along which the body extends, like the X, Y, and Z axes of a Cartesian coordinate system. An axis can be projected to a corresponding plane.
Planes
[edit]
Anatomy is often described in planes, referring to two-dimensional sections of the body. A section is a two-dimensional surface of a three-dimensional structure that has been cut. A plane is an imaginary two-dimensional surface that passes through the body. Three planes are commonly referred to in anatomy and medicine:[4][5]: 4
- The sagittal plane is the plane that divides the body or an organ vertically into right and left sides. If this vertical plane runs directly down the middle of the body, it is called the midsagittal or median plane. If it divides the body into unequal right and left sides, it is called a parasagittal plane, or less commonly a longitudinal section.[4]
- The frontal plane is the plane that divides the body or an organ into an anterior (front) portion and a posterior (rear) portion. The frontal plane is often referred to as a coronal plane, following Latin corona, which means "crown".[4]
- The transverse plane is the plane that divides the body or organ horizontally into upper and lower portions. Transverse planes produce images referred to as cross sections.[4]
Functional state
[edit]Anatomical terms may be used to describe the functional state of an organ: [citation needed]
- Anastomoses refers to the connection between two structures previously branched out, such as blood vessels or leaf veins.
- Patent, meaning a structure such as an artery or vein that abnormally remains open, such as a patent ductus arteriosus, referring to the ductus arteriosus which normally becomes ligamentum arteriosum within three weeks of birth. Something that is patent may also refer to a channel such as a blood vessel, section of bowel, collecting system or duct that is not occluded and remains open to free flow. Such obstructions may include a calculus (i.e. a kidney stone or gallstone), plaque (like that encountered in vital arteries such as coronary arteries and cerebral arteries), or another unspecified obstruction, such as a mass or bowel obstruction.
- A plexus refers to a net-like arrangement of a nerve.
Anatomical variation
[edit]The term anatomical variation is used to refer to a difference in anatomical structures that is not regarded as a disorder. Many structures vary slightly between people, for example muscles that attach in slightly different places. For example, the presence or absence of the palmaris longus tendon. Anatomical variation is unlike congenital anomalies, which are considered a disorder.[16]
Movement
[edit]

Joints, especially synovial joints allow the body a tremendous range of movements. Each movement at a synovial joint results from the contraction or relaxation of the muscles that are attached to the bones on either side of the articulation. The type of movement that can be produced at a synovial joint is determined by its structural type.
Movement types are generally paired, with one being the opposite of the other. Body movements are always described in relation to the anatomical position of the body: upright stance, with upper limbs to the side of body and palms facing forward.[14]
General motion
[edit]Terms describing motion in general include:
- Flexion and extension, which refer to a movement that decreases (flexion) or increases (extension) the angle between body parts. For example, when standing up, the knees are extended.
- Abduction and adduction refers to a motion that pulls a structure away from (abduction) or towards (adduction) the midline of the body or limb. For example, a star jump requires the legs to be abducted.
- Internal rotation (or medial rotation) and external rotation (or lateral rotation) refers to rotation towards (internal) or away from (external) the center of the body. For example, the lotus position posture in yoga requires the legs to be externally rotated.
- Elevation and depression refer to movement in a superior (elevation) or inferior (depression) direction. Primarily refers to movements involving the scapula and mandible.[17]
Special motions of the hands and feet
[edit]These terms refer to movements that are regarded as unique to the hands and feet:[18]: 590–7
- Dorsiflexion and plantarflexion refers to flexion (dorsiflexion) or extension (plantarflexion) of the foot at the ankle. For example, plantarflexion occurs when pressing the brake pedal of a car.
- Palmarflexion and dorsiflexion refer to movement of the flexion (palmarflexion) or extension (dorsiflexion) of the hand at the wrist. For example, prayer is often conducted with the hands dorsiflexed.
- Pronation and supination refer to rotation of the forearm or foot so that in the anatomical position the palm or sole is facing anteriorly (supination) or posteriorly (pronation). For example, if a person is holding a bowl of soup in one hand, the hand is "supinated" and the thumb will point away from the body midline and the palm will be superior; if the hands are typing on a computer keyboard, they will be "pronated" with the thumbs toward the body midline and the palms inferior.
- Eversion and inversion refer to movements that tilt the sole of the foot away from (eversion) or towards (inversion) the midline of the body.
Muscles
[edit]
Muscle action that moves the axial skeleton work over a joint with an origin and insertion of the muscle on respective side. The insertion is on the bone deemed to move towards the origin during muscle contraction. Muscles are often present that engage in several actions of the joint; able to perform for example both flexion and extension of the forearm as in the biceps and triceps respectively.[14] This is not only to be able to revert actions of muscles, but also brings on stability of the actions though muscle coactivation.[19]
Agonist and antagonist muscles
[edit]The muscle performing an action is the agonist, while the muscle which contraction brings about an opposite action is the antagonist. For example, an extension of the lower arm is performed by the triceps as the agonist and the biceps as the antagonist (which contraction will perform flexion over the same joint). Muscles that work together to perform the same action are called synergists. In the above example synergists to the biceps can be the brachioradialis and the brachialis muscle.[14]
Skeletal and smooth muscle
[edit]
The gross anatomy of a muscle is the most important indicator of its role in the body. One particularly important aspect of gross anatomy of muscles is pennation or lack thereof. In most muscles, all the fibers are oriented in the same direction, running in a line from the origin to the insertion. In pennate muscles, the individual fibers are oriented at an angle relative to the line of action, attaching to the origin and insertion tendons at each end. Because the contracting fibers are pulling at an angle to the overall action of the muscle, the change in length is smaller, but this same orientation allows for more fibers (thus more force) in a muscle of a given size. Pennate muscles are usually found where their length change is less important than maximum force, such as the rectus femoris.[20]
Skeletal muscle is arranged in discrete muscles, an example of which is the biceps brachii. The tough, fibrous epimysium of skeletal muscle is both connected to and continuous with the tendons. In turn, the tendons connect to the periosteum layer surrounding the bones, permitting the transfer of force from the muscles to the skeleton. Together, these fibrous layers, along with tendons and ligaments, constitute the deep fascia of the body.[20]
Joints
[edit]Movement is not limited to only synovial joints, although they allow for most freedom. Muscles also run over symphysis, which allow for movement in for example the vertebral column by compression of the intervertebral discs. Additionally, synovial joints can be divided into different types, depending on their axis of movement.[21]
Body cavities
[edit]The body maintains its internal organization by means of membranes, sheaths, and other structures that separate compartments, called body cavities. The ventral cavity includes the thoracic and abdominopelvic cavities and their subdivisions. The dorsal cavity includes the cranial and spinal cavities.[14]
Membranes
[edit]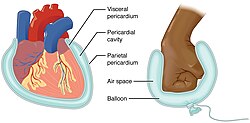
A serous membrane (also referred to as a serosa) is a thin membrane that covers the walls of organs in the thoracic and abdominal cavities. The serous membranes have two layers; parietal and visceral, surrounding a fluid filled space.[4] The visceral layer of the membrane covers the organ (the viscera), and the parietal layer lines the walls of the body cavity (pariet- refers to a cavity wall). Between the parietal and visceral layers is a very thin, fluid-filled serous space, or cavity.[4] For example, the pericardium is the serous cavity which surrounds the heart.[4]
Additional images
[edit]-
Older set of terminology shown in Parts of the Human Body: Posterior and Anterior View from the 1933 edition of Sir Henry Morris' Human Anatomy. See also List of human anatomical regions § Deprecated or older regions.
-
Labels of human body features displayed on images of actual human bodies, from which body hair and male facial hair have been removed
See also
[edit]References
[edit]- ^ BarCharts, Inc (2011). Anatomy Terminology. Boca Raton: BarCharts, Inc. ISBN 978-1-4232-1632-2.
{{cite book}}:|first=has generic name (help) - ^ Whitmore, Ian; Federative Committee on Anatomical Terminology, eds. (1998). Terminologia anatomica: = International anatomical terminology. Stuttgart: Thieme. ISBN 978-3-13-115251-0.
- ^ BarCharts, Inc (2011). Anatomy Terminology. Boca Raton: BarCharts, Inc. ISBN 978-1-4232-1632-2.
{{cite book}}:|first=has generic name (help) - ^ a b c d e f g h i j k l m n
 This article incorporates text available under the CC BY 4.0 license. Betts, J Gordon; Desaix, Peter; Johnson, Eddie; Johnson, Jody E; Korol, Oksana; Kruse, Dean; Poe, Brandon; Wise, James; Womble, Mark D; Young, Kelly A (February 26, 2016). Anatomy & Physiology. Houston: OpenStax CNX. 1.6. Anatomical Terminology. ISBN 978-1-93-816813-0. ID: 14fb4ad7-39a1-4eee-ab6e-3ef2482e3e22@8.24. Archived from the original on March 16, 2018. Retrieved March 15, 2018.
This article incorporates text available under the CC BY 4.0 license. Betts, J Gordon; Desaix, Peter; Johnson, Eddie; Johnson, Jody E; Korol, Oksana; Kruse, Dean; Poe, Brandon; Wise, James; Womble, Mark D; Young, Kelly A (February 26, 2016). Anatomy & Physiology. Houston: OpenStax CNX. 1.6. Anatomical Terminology. ISBN 978-1-93-816813-0. ID: 14fb4ad7-39a1-4eee-ab6e-3ef2482e3e22@8.24. Archived from the original on March 16, 2018. Retrieved March 15, 2018.
- ^ a b c Drake, Richard L.; Vogl, Wayne; Tibbitts, Adam W.M. Mitchell (2005). Gray's anatomy for students. illustrations by Richard Richardson, Paul (Pbk. ed.). Philadelphia: Elsevier/Churchill Livingstone. ISBN 978-0-443-06612-2.
- ^ Federative Committee on Anatomical Terminology (2008). Terminologia Histologica – International Terms for Human Cytology and Histology. Cardiff: Lippincott Williams & Wilkins. ISBN 978-0-7817-6610-4. OCLC 63680504.
- ^ Federative Committee on Anatomical Terminology (1998). Terminologia Anatomica – International Anatomical Terminology. Stuttgart: Thieme. ISBN 978-3-13-115251-0. OCLC 43947698.
- ^ Losardo, Ricardo J. (2009). "Pan American Association of Anatomy: history and relevant regulations". Int J Morphol. 27 (4): 1345–52. ISSN 0717-9367.
- ^ "Terminologia Anatomica" at Dorland's Medical Dictionary[permanent dead link]
- ^ Terminologia Anatomica: International Anatomical Terminology. New York: Thieme Medical Publishers. 1998. ISBN 978-0-86577-808-5.
- ^ Engelbrecht, Rolf (2005). Connecting Medical Informatics And ... - Google Book Search. IOS Press. ISBN 9781586035495. Retrieved 2008-08-22.
- ^ Ten Donkelaar, Hans J.; Broman, Jonas; Neumann, Paul E.; Puelles, Luis; Riva, Alessandro; Tubbs, R. Shane; Kachlik, David (2017-03-01). "Towards a Terminologia Neuroanatomica". Clinical Anatomy. 30 (2): 145–155. doi:10.1002/ca.22809. ISSN 1098-2353. PMID 27910135. S2CID 32863255.
- ^ Strzelec, B.; Chmielewski, P. P.; Gworys, B. (2017). "The Terminologia Anatomica matters: examples from didactic, scientific, and clinical practice". Folia Morphologica. 76 (3): 340–347. doi:10.5603/FM.a2016.0078. ISSN 1644-3284. PMID 28026851. Archived from the original on 2018-02-14. Retrieved 2018-02-14.
- ^ a b c d e f g h Betts, J Gordon; Desaix, Peter; Johnson, Eddie; Johnson, Jody E; Korol, Oksana; Kruse, Dean; Poe, Brandon; Wise, James; Womble, Mark D; Young, Kelly A (October 3, 2013). Anatomy & Physiology. Houston: OpenStax CNX. 1.6. Anatomical Terminology. ISBN 978-1-93-816813-0. ID: 14fb4ad7-39a1-4eee-ab6e-3ef2482e3e22@6.11. Archived from the original on January 9, 2014. Retrieved November 16, 2013.
- ^ a b c d "1.4B: Directional Terms". Medicine LibreTexts. 18 July 2018. Retrieved 4 March 2025.
- ^ DeSilva, Malini; Munoz, Flor M.; Mcmillan, Mark; Kawai, Alison Tse; Marshall, Helen; Macartney, Kristine K.; Joshi, Jyoti; Oneko, Martina; Rose, Annette Elliott (2016-12-01). "Congenital anomalies: Case definition and guidelines for data collection, analysis, and presentation of immunization safety data". Vaccine. 34 (49): 6015–6026. doi:10.1016/j.vaccine.2016.03.047. ISSN 0264-410X. PMC 5139892. PMID 27435386.
- ^ "Types of movements in the human body". Kenhub. Archived from the original on 2019-09-03. Retrieved 2019-09-03.
- ^ Swartz, Mark H. (2010). Textbook of physical diagnosis : history and examination (6th ed.). Philadelphia, PA: Saunders/Elsevier. ISBN 978-1-4160-6203-5.
- ^ Castrogiovanni, Paola; Conway, Nerys; Imbesi, Rosa; Trovato, Francesca Maria (September 2016). "Morphological and Functional Aspects of Human Skeletal Muscle". Journal of Functional Morphology and Kinesiology. 1 (3): 289–302. doi:10.3390/jfmk1030289.
- ^ a b Moore, Keith L.; Dalley, Arthur F.; Agur, Anne M. R. (2010). Moore's Clinically Oriented Anatomy. Phildadelphia: Lippincott Williams & Wilkins. pp. 29–35. ISBN 978-1-60547-652-0.
- ^ "9.1 Classification of Joints – Anatomy and Physiology". opentextbc.ca. Archived from the original on 2019-03-29. Retrieved 2019-09-03.
Further reading
[edit]- Calais-Germain, Blandine (1993). Anatomy of Movement. Eastland Press. ISBN 978-0-939616-17-6.
- Drake, Richard; Vogl, Wayne; Mitchell, Adam (2004). Gray's Anatomy for Students. Churchill Livingstone. ISBN 978-0-443-06612-2.
- Martini, Frederic; Timmons, Michael; McKinnley, Michael (2000). Human Anatomy (3rd ed.). Prentice-Hall. ISBN 978-0-13-010011-5.
- Marieb, Elaine (2000). Essentials of Human Anatomy and Physiology (6th ed.). Addison Wesley Longman. ISBN 978-0-8053-4940-5.
- Muscolino, Joseph E. (2005). The Muscular System Manual: The Skeletal Muscles of the Human Body (2nd ed.). C.V. Mosby. ISBN 978-0-323-02523-2.
- Ngai, Steven (2006). Understanding Anatomical Latin (PDF) (3rd ed.). Archived from the original (PDF) on 2009-03-25. Retrieved 2015-11-15.
- Losardo, R. J.; Valverde Barbato De Prates, N. E.; Arteaga-Martinez, M.; García Peláez, M. I.; Cabral, R. H. (2017). "International Morphological Terminology (anatomy, histology and embryology): beyond scientific terms". Journal of Morphological Sciences. 34 (3): 130–133. doi:10.4322/jms.109916. ISSN 2177-0298.
Sources
[edit]![]() This article incorporates text from a free content work. Licensed under CC BY 4.0. Text taken from Anatomy and Physiology, J. Gordon Betts et al, Openstax.
This article incorporates text from a free content work. Licensed under CC BY 4.0. Text taken from Anatomy and Physiology, J. Gordon Betts et al, Openstax.
Anatomical terminology
View on GrokipediaEtymology and Word Formation
Linguistic origins
Anatomical terminology predominantly derives from ancient Greek and Latin, languages chosen for their precision and universality in scientific description. Approximately 86% of modern English anatomical terms originate from these classical sources, reflecting their enduring role in standardizing medical nomenclature.[5] Greek roots often pertain to clinical and functional aspects, such as "kardia," meaning heart, which forms the basis for terms like "cardiac" and "cardia," denoting structures related to the heart's position or function.[6] Latin contributions emphasize structural elements, exemplified by "os," which signifies both bone—as in "osseous"—and mouth—as in "oral."[7] During the Renaissance, anatomists like Andreas Vesalius reinforced the adoption of Greek and Latin for anatomical naming to achieve greater accuracy and avoid the ambiguities of vernacular languages. Vesalius, in his seminal work De humani corporis fabrica (1543), drew upon classical texts by Galen and Celsus to unify terminology, establishing a lexicon that prioritized descriptive clarity over regional variations.[8] This linguistic revival not only corrected medieval misconceptions but also laid the groundwork for a standardized international nomenclature that persists today.[9] Eponyms, terms honoring individuals, emerged alongside classical derivations but have increasingly been phased out in favor of descriptive language. For instance, the Fallopian tubes—named after 16th-century anatomist Gabriele Falloppio—are now often referred to as uterine tubes to emphasize their anatomical location and function rather than personal attribution.[10] This shift, driven by efforts from organizations like the Federative International Programme on Anatomical Terminologies, promotes inclusivity and universality by reducing historical biases embedded in eponymous naming.[11] Medieval Arabic scholarship significantly influenced anatomical terminology by serving as a conduit for Greek knowledge into Latin Europe. Through centers like the Toledo School of Translators, scholars such as Avicenna (Ibn Sina) preserved and expanded upon Hellenistic texts, introducing or refining terms that bridged ancient and modern usage—such as adaptations of Greek "tashreeh" for dissection.[12] These contributions, documented in works like Avicenna's Canon of Medicine, enriched the linguistic foundation before the Renaissance resurgence of classical languages.[13]Prefixes, roots, and suffixes
Anatomical terminology relies on modular components—prefixes, roots, and suffixes—primarily derived from Greek and Latin to create precise, descriptive terms for body structures and processes.[14] Prefixes precede the root to specify location, direction, quantity, or quality, allowing terms to convey relational or modificational details. Common examples include "hypo-," meaning below or deficient, as in hypodermic (under the skin).[15] Another is "hyper-," denoting above or excessive, seen in hyperglycemia (excess blood sugar).[15] Other frequently used prefixes are "endo-" (within or inner), as in endocrine (secreting within), and "peri-" (around), as in pericardium (around the heart).[16] Roots provide the foundational meaning, typically referring to specific organs, tissues, or body parts, and can be combined to form compound terms. For body parts, "nephr-" (Greek for kidney) appears in nephritis (kidney inflammation), while "hepat-" (Greek for liver) is used in hepatocyte (liver cell).[17] Additional roots include "cardi-" (Greek for heart), as in cardiac (pertaining to the heart), and "derm-" (Greek for skin), forming dermatology (study of the skin).[16] These roots often pair with others, such as "gastr-" (Greek for stomach) in gastroenteritis (stomach and intestine inflammation).[17] Suffixes follow the root to indicate conditions, procedures, or functions, adding specificity to the term's implication. The suffix "-itis" signifies inflammation, exemplified by appendicitis (appendix inflammation).[16] "-ectomy" denotes surgical excision, as in hysterectomy (uterus removal).[17] Other common suffixes are "-ology" (study of), in histology (tissue study), and "-pathy" (disease of), as in nephropathy (kidney disease).[16] To form compound words accurately, rules govern the integration of these elements, preventing ambiguity and ensuring euphonic pronunciation. A combining vowel, usually "o," is added to the root when joining it to another root or a suffix starting with a consonant; for example, "gastr-" adjusts to "gastro-" in gastroscopy (stomach examination).[18] No such vowel is used if the suffix begins with a vowel, as in nephritic (pertaining to the kidney) from "nephr-."[18] Prefixes connect directly to roots without a vowel, like "hyper-" to "thyroid" in hyperthyroidism.[18] These conventions, rooted in classical languages, maintain terminological precision across medical fields.[16]Historical Development
Early anatomical nomenclature
The foundations of anatomical nomenclature trace back to ancient Egypt, where systematic descriptions of the body emerged from medical practices and embalming rituals. Key sources include the Edwin Smith Surgical Papyrus (c. 1600 BCE), the oldest known surgical treatise, which details 48 cases of injuries with precise observations of anatomy, such as the vascular and nervous systems, using terms like "mtw" for vessels that carried fluids throughout the body.[19] Similarly, the Ebers Papyrus (c. 1550 BCE) employs terminology for organs and channels, reflecting an understanding of the heart's central role in circulation, though intertwined with metaphysical concepts like the "wekhedu" as a source of disease.[19] This nomenclature, derived from hieroglyphic observations rather than dissection, emphasized functional descriptions over abstract naming, influencing later Mediterranean traditions.[19] In ancient Greece, anatomical terminology evolved through philosophical and empirical inquiry, but it was Claudius Galen's work in the Roman Empire (c. 129–216 CE) that established a dominant framework. Galen, drawing on Hippocratic and Aristotelian precedents, introduced terms like "ureter" for the tube connecting the kidney to the bladder and classified cranial nerves into seven pairs, using colloquial Greek words for practical descriptions in treatises such as On the Anatomy of Veins and Arteries.[20] His nomenclature, limited to about 100 terms, focused on functionality—such as heart valves and muscle attachments—based largely on animal dissections, which introduced errors like the rete mirabile in humans that persisted for centuries.[21] Galen's texts became the cornerstone of Roman anatomical knowledge, blending observation with humoral theory and exerting unchallenged authority across the empire.[20] During the medieval period, Arabic scholars preserved and expanded Galenic nomenclature through translations and original contributions, bridging ancient and European traditions. Avicenna (Ibn Sina, 980–1037 CE), in his Canon of Medicine, synthesized Greek sources while introducing precise terms for structures like the six extraocular eye muscles and the trigeminal nerve, distinguishing nerves from tendons to aid surgical precision.[22] His work, translated into Latin by figures like Gerard of Cremona in the 12th century, standardized terminology such as brain divisions into frontal, middle, and rear lobes, influencing Islamic and Byzantine medicine.[22] In Europe, monastic centers like the School of Salerno (c. 850–1250 CE) maintained anatomical records through manuscripts compiling Galen's texts, such as the Articella collection, which used Latin adaptations of Greek terms for physiology and pathology in monastic libraries.[23] These efforts, including rare 13th-century dissections in Western Europe, preserved nomenclature amid limited human autopsies, often highlighting vascular systems with preservatives like mercury sulfide.[24] The Renaissance marked a pivotal reform with Andreas Vesalius's De Humani Corporis Fabrica (1543), which challenged Galenic inconsistencies through human dissections and standardized Latin-based terminology. Vesalius corrected errors like the non-existent human rete mirabile, introducing ordinal systems for muscles and bones (e.g., numbering ribs and vertebrae) and detailed illustrations that clarified terms for organs and vessels.[25] His work reduced reliance on animal-derived nomenclature, promoting empirical descriptions that influenced subsequent anatomists like Fabricius ab Aquapendente.[21] This shift emphasized precision over tradition, laying groundwork for modern anatomical language rooted in Greco-Latin etymology.[25] By the 19th century, anatomical nomenclature faced proliferation and fragmentation, with eponyms—names honoring discoverers—multiplying to over 700 for common structures, exacerbating regional variations. Terms like the "circle of Willis" or "Achilles tendon" emerged alongside synonyms (e.g., the ileocecal valve known as Bauhin's, Tulp's, or Morgagni's valve), stemming from nationalistic naming in German, French, and British schools.[26] This inconsistency, with up to 50,000 terms for 5,000 structures by mid-century, hindered international communication and education, as possessive forms (e.g., Falloppio's tube) varied by language and tradition.[27] Such challenges underscored the need for unification, though eponyms persisted due to cultural reverence for pioneers like Harvey and Sylvius.[26]Modern standardization efforts
The modern era of anatomical terminology standardization began in 1895 with the establishment of the Basle Nomina Anatomica (BNA), the first internationally agreed-upon Latin nomenclature, developed by the German Anatomical Society during its meeting in Basel and based primarily on Carl Gegenbaur's influential textbook.[28] This initiative addressed the proliferation of inconsistent regional terms that had emerged since the Renaissance, aiming to create a unified lexicon of approximately 4,500 terms for gross anatomy. Subsequent revisions refined the BNA, with the Paris Nomina Anatomica (PNA) approved in 1955 by the International Anatomical Nomenclature Committee (IANC) at the Sixth International Congress of Anatomists, incorporating updates to reflect evolving anatomical knowledge while maintaining Latin as the primary language.[29] The push for global coordination intensified through the formation of dedicated international bodies. The Federative Committee on Anatomical Terminology (FCAT), established under the International Federation of Associations of Anatomists (IFAA) in 1989, evolved into the Federative International Committee on Anatomical Terminology (FICAT) by 1999, tasked with revising and expanding nomenclature to ensure consistency across disciplines.[30] In 2009, FICAT transitioned to the Federative International Programme for Anatomical Terminology (FIPAT), which continues to oversee the development, maintenance, and promotion of standardized terms, emphasizing their utility in education, research, and clinical practice.[31] A landmark achievement was the publication of Terminologia Anatomica (TA) in 1998, approved by the IFAA General Assembly in São Paulo, which superseded prior nominas as the official international standard for human gross anatomy, featuring bilingual Latin-English terms organized hierarchically and indexed for accessibility.[32] Building on this, FIPAT released Terminologia Histologica (TH) in 2008, providing standardized terms for cytology and histology to bridge microscopic anatomy with gross structures.[33] Further updates have incorporated terms relevant to medical imaging, such as those for radiological anatomy in the second edition of TA (TA2) published in 2019, facilitating precise communication in diagnostic contexts like CT and MRI interpretations. Despite these advances, ongoing challenges persist in achieving universal adoption and completeness. Multilingual implementation remains uneven, as TA's Latin-English framework requires translation into other languages for broader clinical use, particularly in non-English-speaking regions.[34] Digital integration efforts, including tools like the TA2 online viewer, aim to enhance accessibility but face hurdles in linking terminology to electronic health records and AI-driven analysis.[35] Additionally, FIPAT reports from the 2020s highlight incomplete coverage of neuroanatomy, with gaps in standardized terms for complex neural structures prompting calls for targeted revisions to support neuroscience advancements.[36]Fundamental Positioning and Directions
Anatomical position
The anatomical position serves as the foundational reference orientation for describing the human body in anatomical studies and medical practice. In this standard posture, the body stands erect with the feet together and parallel, pointing forward; the arms hang relaxed at the sides with the palms facing anteriorly (supinated); the head is aligned straight ahead with the eyes gazing forward and the mouth closed. This configuration ensures a neutral, reproducible stance that eliminates ambiguity in spatial descriptions.[37][38][39] The origins of this position trace back to the Renaissance era, where anatomists like Andreas Vesalius began depicting the human body in consistent, upright illustrations to facilitate accurate dissection and illustration in works such as De humani corporis fabrica (1543), laying the groundwork for standardized views. Over centuries, this evolved into a formalized reference during the 19th and 20th centuries through international nomenclature efforts, culminating in its explicit definition within modern anatomical standards to provide an unambiguous baseline for all body descriptions. The Federative International Programme on Anatomical Terminology (FIPAT), under the International Federation of Associations of Anatomists (IFAA), endorses this position as part of its global terminological framework.[40][1] Variations of the anatomical position accommodate horizontal or non-human orientations while preserving core alignments. The supine position extends it by having the body lie flat on the back with the face upward and palms still facing anteriorly, commonly used in clinical examinations and imaging. Conversely, the prone position involves lying face down, with the posterior surface against the support, adjusting the reference for ventral-dorsal relations. In veterinary anatomy for quadrupeds, the position adapts to a stance on all four limbs with the head extended forward, enabling analogous descriptions in animal studies. Radiological imaging often references the upright anatomical position theoretically but applies supine adjustments for patient comfort and scan acquisition.[41][42][43][37] This reference posture is crucial for maintaining consistency in anatomical communication, serving as the basis from which all structural relations are defined, thereby minimizing errors in medical education, surgical planning, and diagnostic imaging. By standardizing descriptions, it prevents misinterpretations during procedures like dissections or operations, where precise localization of organs and tissues is essential for safety and efficacy. In clinical settings, adherence to this position enhances interdisciplinary collaboration among surgeons, radiologists, and anatomists.[38][41][44]Directional and positional terms
Directional and positional terms in anatomy describe the relative locations and orientations of body structures, providing a standardized language for precise communication among healthcare professionals and researchers. These terms are defined relative to the anatomical position, where the body stands upright with arms at the sides, palms facing forward, and feet together.[45] The term superior (Latin: superior) refers to a position above or closer to the head, while inferior (Latin: inferior) indicates a position below or toward the feet; synonyms include cranial or cephalic for superior and caudal for inferior, particularly in describing the trunk.[2][45] For example, the heart is superior to the diaphragm.[45] Anterior (Latin: anterior or anticus) denotes the front of the body, synonymous with ventral (Latin: ventralis) in human anatomy, whereas posterior (Latin: posterior or posticus) means the back, equivalent to dorsal (Latin: dorsalis).[2][45] The nose is anterior to the ears, and the spine is posterior to the sternum.[45] Medial (Latin: medialis) describes a position toward the midline of the body, and lateral (Latin: lateralis) indicates away from the midline or toward the side.[2][45] The big toe is medial to the other toes, while the ears are lateral to the nose.[45] For extremities, proximal (Latin: proximalis) means closer to the point of origin or attachment, and distal (Latin: distalis) means farther from it.[2][45] The elbow is proximal to the wrist on the arm.[45] Superficial (Latin: superficialis or sublimis) refers to nearer the body surface, and deep (Latin: profundus) to farther from it.[2][45] The skin is superficial to the muscles.[45] Ipsilateral (Latin: ipsilateralis) denotes the same side of the body, and contralateral (Latin: contralateralis) the opposite side, often used in neurology.[2][45] In clinical contexts, these terms facilitate accurate descriptions in reports and procedures; for instance, in radiology, "medial" specifies a lesion toward the body's midline, aiding diagnosis and treatment planning.[45] They are essential for unambiguous communication in surgery, imaging, and patient assessments.[45] While primarily standardized for humans, these terms adapt in veterinary anatomy for quadrupeds, where rostral (Latin: rostralis) describes positions toward the nose in the head, and ventral/dorsal replaces anterior/posterior to account for the horizontal body orientation.[2][43][46]Spatial Organization
Body planes
Body planes are imaginary flat surfaces that divide the human body into sections to facilitate the description of anatomical structures, locations, and movements relative to the anatomical position. Standardized in the Terminologia Anatomica (TA2), these planes provide a consistent framework for anatomical communication across medical and scientific disciplines. The principal planes are oriented vertically or horizontally with respect to the body's long axis in the standard upright posture.[47] The sagittal plane (plana sagittalia) is a vertical plane that divides the body into unequal left and right portions. A specific type, the midsagittal plane (planum medianum), passes through the midline to create symmetrical halves, while parasagittal planes (plana paramediana) are parallel to the midsagittal plane but positioned off-center, allowing for descriptions of lateral structures. The coronal plane (plana coronalia, also known as the frontal plane) is another vertical plane, oriented perpendicular to the sagittal plane, that separates the body into anterior (front) and posterior (back) sections. The transverse plane (plana transversa, or horizontal plane) runs perpendicular to the body's long axis, dividing it into superior (upper) and inferior (lower) parts. These three principal planes intersect at right angles and form the basis for most anatomical orientations.[47] Oblique planes are non-perpendicular divisions that cut across the body at an angle to the principal planes, providing views of structures not aligned with standard axes, such as diagonal muscle fibers or irregular organs. In clinical applications, body planes are essential for medical imaging: computed tomography (CT) and magnetic resonance imaging (MRI) scans are typically acquired in transverse (axial) slices and reconstructed in sagittal or coronal views to assess pathology in specific orientations. In embryology, these planes guide the sectioning of embryos to study developmental processes, such as the formation of germ layers and organ primordia during early gestation.[47][48]| Plane | Latin Term | Orientation | Division Created |
|---|---|---|---|
| Sagittal | Plana sagittalia | Vertical, parallel to midline | Left and right portions |
| Midsagittal | Planum medianum | Vertical, through midline | Equal left and right halves |
| Parasagittal | Plana paramediana | Vertical, parallel to midsagittal | Unequal left and right portions |
| Coronal | Plana coronalia | Vertical, perpendicular to sagittal | Anterior and posterior sections |
| Transverse | Plana transversa | Horizontal, perpendicular to long axis | Superior and inferior parts |
| Oblique | Angled to principal planes | Diagonal sections of structures |
Body axes
Body axes in anatomical terminology refer to the imaginary lines around which the body or its segments rotate during movement, providing a framework for analyzing spatial orientation and motion in three dimensions. These axes are perpendicular to the body's cardinal planes and serve as references for describing rotations. The three primary axes are the sagittal axis, frontal (or coronal) axis, and vertical (longitudinal) axis, each aligned with specific anatomical directions.[49] The sagittal axis, also known as the anteroposterior axis, extends from the front (anterior) to the back (posterior) of the body. Rotations around this axis occur in the frontal plane, facilitating movements that deviate laterally from the midline, such as abduction and adduction of limbs.[49] The frontal axis, or mediolateral axis, runs from the midline (medial) to the side (lateral). It supports rotations in the sagittal plane, enabling forward and backward motions like flexion and extension at joints.[49] The vertical axis, referred to as the longitudinal or superoinferior axis, aligns from the top (superior) to the bottom (inferior) of the body. Rotations about this axis take place in the transverse plane, allowing twisting actions such as medial and lateral rotation.[49] In biomechanics, body axes are essential for joint motion analysis, where they define the orientation of local coordinate systems to quantify angular displacements and velocities. For instance, aligning axes with anatomical landmarks (e.g., superior-inferior, anterior-posterior, and medial-lateral directions) enables precise evaluation of joint kinematics, such as range of motion in the knee or shoulder during dynamic activities.[50] This approach is widely used in gait analysis and sports science to assess functional performance and identify deviations from normal patterns.[50] Body axes also underpin coordinate systems in 3D modeling for anatomy software, where they standardize representations of human structure across imaging modalities like MRI. In these systems, the sagittal axis corresponds to the Y-direction (anterior-posterior), the frontal axis to the X-direction (left-right), and the vertical axis to the Z-direction (inferior-superior), facilitating data registration and visualization in tools such as the Allen Brain Atlas. This alignment ensures interoperability in computational anatomy, supporting applications from surgical planning to virtual simulations.Regional divisions
The human body is divided into standardized regions to facilitate precise description and location of structures in anatomical and clinical contexts. These regional divisions are defined in the Terminologia Anatomica (TA), the international standard for human anatomical nomenclature established by the Federative International Programme for Anatomical Terminology (FIPAT).[2] The terms emphasize surface topography and are derived from Latin roots, allowing for consistent communication across medical disciplines without reliance on eponyms or vernacular language.[51] In the head and neck, the primary regions include the regio cranialis (cranial region, encompassing the skull and scalp), regio facialis (facial region, covering the face from forehead to chin), and regio cervicalis (cervical region, denoting the neck from mandible to clavicle).[2] These divisions are bounded by natural landmarks such as the superciliary arches superiorly for the face and the jugular notch inferiorly for the neck, enabling targeted descriptions in neurology and otolaryngology.[52] The trunk is segmented into the regio thoracica (thoracic region, from clavicles to diaphragm), regio abdominalis (abdominal region, from diaphragm to iliac crests), regio pelvica (pelvic region, from iliac crests to thighs), and regio glutea (gluteal region, the buttocks posterior to the pelvis).[2] These areas are delineated by skeletal features like the costal margin for the thorax and the pubic symphysis for the pelvis, supporting systematic examination in thoracic and abdominal assessments. For the limbs, the upper limb comprises the regio brachialis (brachial region, the arm from shoulder to elbow), regio antebrachialis (antebrachial region, the forearm to wrist), and regio manualis (manual region, the hand).[2] The lower limb includes the regio femoralis (femoral region, the thigh from hip to knee), regio cruralis (crural region, the leg to ankle), and regio pedalis (pedal region, the foot).[2] Boundaries are set by joints, such as the glenohumeral joint for the brachial region and the tibiofibular joint for the crural region, aiding in orthopedic evaluations.[53][54] Specific subregions enhance precision, such as the regio axillaris (axillary region, the armpit bounded by pectoralis major, latissimus dorsi, and humerus) and regio inguinalis (inguinal region, the groin area between abdominal wall and thigh).[2] These are defined by muscular and fascial planes, like the axillary fascia and inguinal ligament, and are crucial for identifying lymph node distributions. Standardized regional divisions are clinically essential for surgery, imaging, and diagnostics, as they ensure unambiguous localization— for instance, specifying an inguinal hernia versus a femoral one reduces errors in procedural planning.[51] This nomenclature, rooted in TA, promotes interoperability in global healthcare by integrating with directional terms like medial and lateral for relational descriptions.[2]Movement and Motion
General types of movement
In anatomical terminology, general types of movement describe the fundamental motions of body segments at synovial joints, standardized to ensure precise communication in medical and scientific contexts. These terms are defined relative to the anatomical position and are categorized based on the axes and planes of motion, as established by the Federative International Programme for Anatomical Terminology (FIPAT).[55] Movements occur around specific axes—such as the sagittal, frontal, or transverse—and within corresponding planes, allowing for systematic description of joint kinematics.[42] Flexion refers to the bending movement that decreases the angle between two body parts or segments at a joint, typically occurring in the sagittal plane around a transverse axis. For example, flexion at the elbow brings the forearm closer to the upper arm. Extension is the opposite, straightening the joint to increase the angle between segments, also in the sagittal plane; for instance, extending the knee aligns the thigh and lower leg. These paired movements are fundamental to hinge-like synovial joints, enabling angular displacement.[42][38] Abduction involves moving a body part away from the midline or median plane of the body, occurring in the frontal (coronal) plane around an anteroposterior axis; raising the arm laterally at the shoulder exemplifies this. Adduction, conversely, moves the part toward the midline in the same plane, such as lowering the arm back to the side. These terms apply primarily to appendicular structures like limbs and are essential for describing lateral deviations at joints like the hip.[42][38] Rotation describes the twisting motion of a body part around its longitudinal axis, which may be medial (internal, toward the midline) or lateral (external, away from the midline); for example, turning the head side to side at the atlantoaxial joint. This movement occurs in the transverse plane and is characteristic of pivot joints. Circumduction combines flexion, extension, abduction, and adduction to produce a conical or circular path at a joint, without rotation around the distal segment; it is best demonstrated at multiaxial ball-and-socket joints like the shoulder, where the arm traces a circle.[42][38] Basic kinematics of synovial joints are classified by degrees of freedom, which indicate the number of independent directions in which motion can occur, determining the range and type of general movements permitted. Uniaxial joints allow one degree of freedom, such as flexion/extension in hinge joints or rotation in pivot joints. Biaxial joints permit two degrees, enabling combinations like flexion/extension and abduction/adduction in condyloid or saddle joints. Multiaxial joints offer three degrees of freedom, supporting circumduction and rotations in ball-and-socket or plane joints, thus providing the greatest versatility for general motions.[56]/8:_Joints/8.4:_Synovial_Joints/8.4E:_Synovial_Joint_Movements)Specialized motions
Specialized motions refer to distinct types of movement primarily associated with the distal appendages, the hands and feet, which build upon foundational terms like flexion and extension to describe precise actions essential for manipulation and locomotion. These terms arise from the unique synovial joint configurations in these regions, enabling greater versatility compared to proximal body movements.[57] In the hand, opposition denotes the movement where the thumb pad touches the pads of the other fingers, allowing for precision grasping and a key feature of human manual dexterity. Abduction of the fingers spreads them away from the midline of the hand, while adduction brings them together, occurring at the metacarpophalangeal joints to facilitate spreading or closing of the digits. Circumduction at the carpals involves a circular motion of the hand at the wrist, combining sequential flexion, adduction, extension, and abduction for fluid rotational maneuvers.[57] For the foot, inversion turns the sole medially toward the midline, while eversion turns it laterally away from the midline; these occur at the intertarsal joints among the tarsal bones and involve combined adduction with plantar flexion for inversion or abduction with dorsiflexion for eversion. Dorsiflexion elevates the anterior aspect of the foot toward the shin, and plantar flexion depresses it to point the toes downward, both at the ankle's hinge joint to support gait and balance.[57][58] These specialized motions reflect evolutionary adaptations, particularly in the hand, where enhanced thumb opposition and finger mobility evolved around 2 million years ago in early Homo species to improve dexterity for tool use and object grasping, distinguishing humans from earlier hominins like Australopithecus with less efficient torque at the trapeziometacarpal joint. In the foot, such motions support bipedal stability on varied terrains, though the emphasis on hand adaptations underscores primate progression toward manipulative precision.[59] Clinically, terms like pes planus describe flatfoot deformity characterized by loss of the medial longitudinal arch, often linked to excessive pronation or eversion during weight-bearing, which alters foot mechanics and may increase injury risk through overpronation.[60]Muscular and Functional Terms
Muscle naming and classification
Muscle names in anatomical terminology are derived from Latin and Greek roots that describe specific characteristics of the muscle, such as its position, form, attachments, or actions, facilitating precise identification and understanding in medical and scientific contexts.[61] This systematic nomenclature aids in studying the musculoskeletal system by encoding descriptive information directly into the name.[62] One primary criterion for naming muscles is their location within the body, often referencing nearby bones, regions, or landmarks. For instance, the pectoralis major is named for its position on the chest (pectus meaning "chest" in Latin), while the temporalis muscle derives its name from the temporal region of the skull.[61] Similarly, the tibialis anterior indicates its anterior attachment to the tibia bone.[62] Muscles are also named based on their shape or size, providing visual cues about their morphology. The deltoid muscle, for example, is triangular in shape (from the Greek delta, Δ), and the quadriceps femoris refers to its four distinct heads (quadri- meaning "four").[61] Size indicators include terms like maximus for the largest, as in gluteus maximus, or minimus for the smallest, as in gluteus minimus.[62] Other shape-based names include trapezius, resembling a trapezoid, and orbicularis, denoting a circular form.[61] Names frequently reflect the muscle's origin and insertion points, with the origin typically named first followed by the insertion. The sternocleidomastoid muscle exemplifies this, originating from the sternum (sterno-) and clavicle (cleido-) and inserting on the mastoid process (-mastoid).[61] This convention highlights the muscle's anatomical attachments, such as in the brachioradialis, which spans from the humerus (brachi-) to the radius (-radialis).[62] Functional aspects of muscle action also influence naming, particularly for skeletal muscles involved in specific movements. Flexor muscles, like the flexor carpi radialis, decrease joint angles, while extensors, such as the extensor digitorum, increase them.[61] Adductors pull structures toward the midline, as in the adductor magnus, and abductors move them away, exemplified by the abductor pollicis brevis.[62] Beyond naming conventions, muscles are classified into three main types based on structure, function, and control: skeletal, smooth, and cardiac, each with distinct histological features. Skeletal muscle is voluntary, striated, and multinucleated, with long cylindrical fibers organized into sarcomeres containing actin and myosin filaments, enabling precise, forceful contractions attached to bones via tendons.[63] Smooth muscle is involuntary and non-striated, featuring fusiform, spindle-shaped cells with a single central nucleus and no sarcomeres, found in walls of hollow organs like blood vessels and the digestive tract for sustained, rhythmic contractions.[63] Cardiac muscle, also involuntary and striated, consists of branched fibers with intercalated discs for synchronized contractions, located exclusively in the heart walls, with one or occasionally two centrally located nuclei and abundant mitochondria for continuous pumping action.[63] These histological distinctions—such as the presence of striations and specific cellular arrangements—underlie their specialized roles in the body.[63]Functional muscle roles
In anatomical terminology, functional muscle roles describe the dynamic interactions among skeletal muscles during movement, emphasizing how groups of muscles coordinate to produce efficient and controlled actions at joints. These roles are essential for understanding biomechanics, where muscles do not act in isolation but in coordinated patterns to enable precise motion while maintaining stability. The primary roles include agonists, antagonists, synergists, and fixators, each contributing to the overall mechanics of locomotion and posture.[64] The agonist, also known as the prime mover, is the muscle primarily responsible for initiating and executing a specific movement by contracting to generate force. For example, the biceps brachii serves as the agonist during elbow flexion, pulling the forearm toward the shoulder.[64] This role highlights the muscle's dominant contribution to the intended action, often relying on neural activation to achieve the desired joint motion.[65] In opposition, the antagonist is the muscle that resists or reverses the action of the agonist, relaxing to allow smooth movement while providing control to prevent excessive speed or range. The triceps brachii acts as the antagonist to the biceps brachii during elbow flexion, lengthening to counteract the pull and ensure deceleration.[64] Antagonists maintain joint stability and are crucial for reciprocal actions, such as extending the elbow after flexion.[66] Synergists are muscles that assist the agonist by contributing additional force or modifying the direction of pull to enhance efficiency and reduce unwanted movements. For instance, the brachialis synergizes with the biceps brachii in elbow flexion by providing supplementary flexion power without rotating the forearm.[64] A specific type of synergist, the fixator, stabilizes the origin of the agonist or fixes the bone against which the prime mover acts, preventing displacement during contraction. The rhomboids function as fixators for the biceps brachii by anchoring the scapula during arm flexion.[67] Biomechanical concepts further elucidate these roles through mechanisms like reciprocal inhibition, a neural reflex where activation of the agonist inhibits the antagonist via spinal interneurons, promoting relaxation and efficient opposition. This process, first described by Charles Sherrington in his foundational work on nervous system integration, ensures smooth transitions between muscle contractions and prevents simultaneous opposition that could cause rigidity.[68] Muscle coordination integrates these roles via proprioceptive feedback from muscle spindles and Golgi tendon organs, allowing hierarchical recruitment of motor units to modulate force and adapt to varying loads during activities like walking or lifting.[68] In pathological contexts, alterations in muscle size impact these functional roles; atrophy refers to the reduction in muscle mass and cross-sectional area due to disuse or denervation, diminishing the agonist's force generation and synergists' supportive capacity, which can lead to compensatory overuse of antagonists and joint instability.[69] Conversely, hypertrophy involves an increase in muscle fiber size through protein synthesis in response to resistance training, enhancing the prime mover's power output and overall coordination but potentially altering antagonist balance if uneven.[69] These changes underscore the functional implications of muscle adaptation in maintaining biomechanical equilibrium.[70]Structural and Containment Terms
Joint terminology
Joints, or articulations, are the points of connection between bones in the skeletal system, enabling stability and movement. Anatomical terminology for joints encompasses both structural and functional classifications to describe their composition and range of motion. Structurally, joints are categorized based on the type of connective tissue binding the bones: fibrous, cartilaginous, or synovial.[71] Functionally, they are divided into synarthroses (immovable), amphiarthroses (slightly movable), and diarthroses (freely movable), with fibrous joints typically corresponding to synarthroses, cartilaginous to amphiarthroses, and synovial to diarthroses.[72] This dual classification provides a comprehensive framework for understanding joint anatomy and pathology.[73] Fibrous joints (synarthroses) consist of bones united by dense fibrous connective tissue without a joint cavity, providing rigid stability. Subtypes include sutures, which are interlocking fibrous connections found in the skull (e.g., coronal suture between the frontal and parietal bones); gomphoses, peg-in-socket joints securing teeth to the alveolar sockets via the periodontal ligament; and syndesmoses, which allow slight movement and connect bones with a ligamentous sheet, such as the distal tibiofibular syndesmosis.[71] These joints are essential for protecting vital structures like the brain while permitting minimal flexibility in certain areas.[72] Cartilaginous joints (amphiarthroses) feature bones connected by cartilage, offering more resilience than fibrous joints but limited mobility. They are divided into synchondroses, joined by hyaline cartilage, which can be temporary (e.g., epiphyseal plates in growing long bones) or permanent (e.g., the first sternocostal joint between the rib and sternum); and symphyses, united by fibrocartilage for slight compressibility, as seen in the pubic symphysis or intervertebral discs between vertebrae.[73] This type supports weight-bearing with shock absorption, crucial in the axial skeleton.[71] Synovial joints (diarthroses) are the most common and mobile, characterized by a fluid-filled joint cavity enclosed by a fibrous capsule and lined with a synovial membrane that secretes lubricating synovial fluid.[72] They are further classified by shape and axis of movement: hinge joints (uniaxial, e.g., elbow allowing flexion and extension); pivot joints (uniaxial rotation, e.g., proximal radioulnar joint for forearm pronation/supination); condyloid joints (biaxial, e.g., wrist permitting flexion/extension and abduction/adduction); saddle joints (biaxial opposition, e.g., carpometacarpal joint of the thumb); plane joints (multiaxial gliding, e.g., intercarpal joints); and ball-and-socket joints (multiaxial, e.g., glenohumeral shoulder joint enabling circumduction).[73] These variations allow diverse motions essential for locomotion and manipulation.[71] Joint naming conventions derive from the bones involved, their shape, or functional characteristics. Many are eponymous or descriptive based on articulating bones, such as the glenohumeral joint (scapula and humerus) or temporomandibular joint (temporal bone and mandible).[71] Shape-based terms include "hinge" for uniaxial synovial joints or "saddle" for biaxial ones, while functional descriptors like "pivot" emphasize motion type.[73] This nomenclature facilitates precise communication in clinical and educational contexts.[72] Accessory structures enhance joint function and stability. Ligaments are dense bands of fibrous connective tissue that connect bones across the joint, reinforcing the capsule and limiting excessive motion (e.g., the anterior cruciate ligament in the knee).[71] Bursae are small, fluid-filled sacs lined with synovium that cushion and reduce friction between tendons, bones, and skin, such as the subacromial bursa in the shoulder.[73] These elements are integral to synovial joint integrity.[72] Clinical terminology addresses joint disorders and interventions. Subluxation refers to partial dislocation where the articular surfaces are misaligned but maintain some contact, often due to ligament laxity (e.g., in the shoulder).[71] Ankylosis denotes the abnormal fusion of a joint into a single bony mass, either through pathology (e.g., rheumatoid arthritis) or surgically induced synostosis, resulting in immobility.[72] In modern contexts, terms like arthroplasty describe prosthetic joint replacement, where artificial components (e.g., metal alloys or polymers) mimic natural articulations in procedures such as total hip arthroplasty.[71] These terms reflect advancements in orthopedics for restoring function.[73]| Structural Type | Functional Type | Key Features | Examples |
|---|---|---|---|
| Fibrous | Synarthrosis | Dense fibrous tissue, no cavity | Skull sutures, tooth sockets |
| Cartilaginous | Amphiarthrosis | Cartilage union (hyaline or fibrocartilage) | Pubic symphysis, epiphyseal plates |
| Synovial | Diarthrosis | Joint cavity with synovial fluid | Knee (hinge), hip (ball-and-socket) |



