Recent from talks
Nothing was collected or created yet.
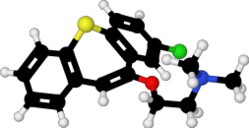
Zotepine
View on Wikipedia
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Zoleptil |
| AHFS/Drugs.com | International Drug Names |
| Routes of administration | Oral |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 7–13% (oral)[2] |
| Metabolism | N-desmethylation to norzotepine (30-40%)[2] |
| Elimination half-life | 13.7–15.9 hours, 12 hours (Norzotepine)[2] |
| Excretion | 17% (Urine)[2] |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| PDB ligand | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.189.143 |
| Chemical and physical data | |
| Formula | C18H18ClNOS |
| Molar mass | 331.86 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| | |
Zotepine is an atypical antipsychotic drug indicated for acute and chronic schizophrenia. It has been used in Germany since 1990 (although it has been discontinued in Germany) and Japan since 1982.
Zotepine is not approved for use in the United States, United Kingdom, Australia, Canada or New Zealand.[3]
Medical uses
[edit]Zotepine's primary use is as a treatment for schizophrenia[4] although clinical trials have been conducted (with positive results) into its efficacy as an antimanic agent in patients with acute bipolar mania.[5][6][7] In a 2013 study in a comparison of 15 antipsychotic drugs in effectivity in treating schizophrenic symptoms, zotepine demonstrated medium-strong effectivity. Less effective than clozapine, slightly less effective than olanzapine and risperidone, approximately as effective as paliperidone, and slightly more effective than haloperidol, quetiapine, and aripiprazole.[8]
Side effects
[edit]- Tachycardia
- Hypotension
- Orthostatic hypotension
- Palpitations
- Hyperprolactinaemia
- Weight gain (produces a similar degree of weight gain to that seen with clozapine and olanzapine treatment)[9]
- Somnolence (2nd highest effect size for causing sedation out of fifteen antipsychotics compared in a recent meta-analysis)[9]
- Extrapyramidal side effects [EPSE] (2nd largest odds ratio for causing EPSE out of fifteen antipsychotics compared in a recent meta-analysis, second only to haloperidol)[9]
- Constipation
- Xerostomia (dry mouth)
- Blurred vision
- Hypersalivation (drooling)
- Mydriasis
- Anxiety
- Agitation
- Rhinitis
- Sexual dysfunction
- Dyspnoea
- Diarrhoea
- Influenza-like symptoms
- Cough
- Vertigo
- Confusion
- Dyspepsia
- Flushing dry skin
- Arthralgia
- Myalgia
- Acne
- Conjunctivitis
- Thrombocythaemia
- QT interval prolongation
- Hyperthermia
- Hypothermia
- Increased serum creatinine
- Hyperglycaemia
- Hypoglycaemia
- Hyperlipidaemia
- Thirst
- Urinary incontinence
- Angle-closure glaucoma
- Agranulocytosis
- Neutropaenia
- Eosinophilia
- Leukocytopenia
- Hypoesthesia
- Anaemia
- Myoclonus
- Myasthenia
- Alopecia
- Thrombocytopaenia
- Bradycardia
- Epistaxis
- Abdominal enlargement
- Deep vein thrombosis
- Paralytic ileus
- Leukopenia
- Tardive dyskinesia
- Neuroleptic malignant syndrome
- Laryngeal edema
- Urinary retention
- Depression
- Ataxia
- Amnesia
- Seizure (dose-dependent risk)[3]
- Metabolic syndrome
- Diabetes mellitus type II
- Cholestasis
- Increased liver enzymes
- Photosensitivity
- Exanthema
- Pruritus
- Hypouricemia
- Oedema
Pharmacology
[edit]Pharmacodynamics
[edit]The antipsychotic effect of zotepine is thought to be mediated through antagonist activity at dopamine and serotonin receptors. Zotepine has a high affinity for the D1 and D2 receptors. It also affects the 5-HT2A, 5-HT2C, 5-HT6, and 5-HT7 receptors.[10] In addition, its active metabolite, norzotepine, serves as a potent norepinephrine reuptake inhibitor.[11]
| Macromolecule (Receptor or transporter protein) | Ki [nM][10] |
|---|---|
| SERT | 151 |
| NET | 530 |
| DAT | 3621 |
| 5-HT1A | 470.5 |
| 5-HT1B | 59.5 |
| 5-HT1D | 119 |
| 5-HT1E | 700 |
| 5-HT2A | 2.7 |
| 5-HT2C | 2.6 |
| 5-HT3 | 472 |
| 5-HT5A | 29 |
| 5-HT6 | 6 |
| 5-HT7 | 12 |
| α1A | 7 |
| α1B | 5 |
| α2A | 180 |
| α2B | 5.35 |
| α2C | 106 |
| M1 | 18 |
| M2 | 140 |
| M3 | 73 |
| M4 | 77 |
| M5 | 260 |
| D1 | 71 |
| D2 | 25 |
| D2S | 5.4 |
| D2L | 11 |
| D3 | 6.4 |
| D4 | 18 |
| D5 | 248 |
| H1 | 3.21 |
| H2 | 500 |
| H4 | 1977 |
Synthesis
[edit]The reaction of 2-chloroacetophenone with 4-chlorothiophenol gives a thioether. This is treated with morpholine and sulfur in a Willgerodt–Kindler reaction to give a phenylacetic acid derivative after acid hydrolysis of the amide intermediate. Cyclization of this compound in the presence of polyphosphoric acid forms the dibenzothiepin ring system of the drug. The enol ether, zotepine, is produced when this is treated with the chloroethyl amine and potassium carbonate in methyl isobutyl ketone as solvent. Under these conditions, the undesired product of C-alkylation is minimised.[12][13][14]
Society and culture
[edit]Brand names
[edit]Brand names include Losizopilon (JP), Lodopin (ID, JP), Nipolept (DE†), Setous (JP), Zoleptil (CZ, PT, TR, UK†), Zotewin (IN); where † indicates a formulation that has been discontinued.
See also
[edit]- Carbinoxamine, diphenhydramine, doxylamine, orphenadrine — the termination chain is the same
- Clotiapine - the base is similar
- Noxiptyline - the termination chain is similar
- Toll-like receptor 4 — investigating probable antagonistic (antiinflammatory) property of several TCA-based molecules
References
[edit]- ^ Anvisa (2023-03-31). "RDC Nº 784 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 784 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 2023-04-04). Archived from the original on 2023-08-03. Retrieved 2023-08-16.
- ^ a b c d e f g Truven Health Analytics, Inc. DRUGDEX® System (Internet) [cited 2013 Jun 25]. Greenwood Village, CO: Thomsen Healthcare; 2013.
- ^ a b "Zotepine". Martindale: The Complete Drug Reference. Royal Pharmaceutical Society of Great Britain. 16 August 2013. Retrieved 2 November 2013.
- ^ a b c d British National Formulary 58. British Medical Association and Royal Pharmaceutical Society of Great Britain; 2009.
- ^ Chan HY, Jou SH, Juang YY, Chang CJ, Chen JJ, Chen CH, et al. (April 2010). "A single-blind, comparative study of zotepine versus haloperidol in combination with a mood stabilizer for patients with moderate-to-severe mania". Psychiatry and Clinical Neurosciences. 64 (2): 162–9. doi:10.1111/j.1440-1819.2010.02066.x. PMID 20447012. S2CID 27657241.
- ^ Harada T, Otsuki S (1986). "Antimanic effect of zotepine". Clinical Therapeutics. 8 (4): 406–14. PMID 3089626.
- ^ Amann B, Sterr A, Mergl R, Dittmann S, Seemüller F, Dobmeier M, et al. (October 2005). "Zotepine loading in acute and severely manic patients: a pilot study". Bipolar Disorders. 7 (5): 471–6. doi:10.1111/j.1399-5618.2005.00241.x. PMID 16176441.
- ^ Leucht S, Cipriani A, Spineli L, Mavridis D, Orey D, Richter F, et al. (September 2013). "Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis". Lancet. 382 (9896): 951–62. doi:10.1016/S0140-6736(13)60733-3. PMID 23810019. S2CID 32085212.
- ^ a b c Leucht S, Cipriani A, Spineli L, Mavridis D, Orey D, Richter F, et al. (September 2013). "Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis". Lancet. 382 (9896): 951–62. doi:10.1016/S0140-6736(13)60733-3. PMID 23810019. S2CID 32085212.
- ^ a b National Institute of Mental Health (12 January 2011). "PDSD Ki Database". Chapel Hill (NC): University of North Carolina. Archived from the original on November 8, 2013. Retrieved 2 November 2013.
- ^ Shobo M, Kondo Y, Yamada H, Mihara T, Yamamoto N, Katsuoka M, et al. (June 2010). "Norzotepine, a major metabolite of zotepine, exerts atypical antipsychotic-like and antidepressant-like actions through its potent inhibition of norepinephrine reuptake". The Journal of Pharmacology and Experimental Therapeutics. 333 (3): 772–81. doi:10.1124/jpet.110.166264. PMID 20223878. S2CID 185592.
- ^ Ueda I, Sato Y, Maeno S, Umio S (October 1975). "The synthesis of 10-(4-methylpiperazino)dibenzo (b,f)thiepin and related compounds. Neurotropic and psychotropic agents". Chemical & Pharmaceutical Bulletin. 23 (10): 2223–2231. doi:10.1248/cpb.23.2223. PMID 1212752.
- ^ Ueda I, Sato Y, Maeno S, Umio S (October 1978). "Synthesis and pharmacological properties of 8-chloro-10-(2-dimethylaminoethoxy)dibenzo[b,f]thiepin and related compounds. Neurotropic and psychotropic agents. III". Chemical & Pharmaceutical Bulletin. 26 (10): 3058–3070. doi:10.1248/cpb.26.3058. PMID 31984.
- ^ "Zotepine". Pharmaceutical Substances. Thieme. Archived from the original on 2024-07-10. Retrieved 2024-07-10.
Further reading
[edit]- Green B. "Focus On Zotepine". Psychiatry On-Line.
- "Zotepine" (PDF). New Drug Evaluation. 36. October 1999. Archived from the original (PDF) on 2004-06-19.


